Introduction
According to The World Bank (1), as a result of globalization, political conflicts, climate change and, social and economic problems that afflict countries, international migration has increased around the world. In 2013, more than 247 million people were living in different countries from that in which they were born, and the flows of world remittances increased to US$583,000 million in 2014.
International migration (emigration, immigration, return, remittances) may affect the health of emigrants, indigenous population of the receiving countries, members of the household that stay in the countries of origin and performance of health systems. Available literature on the effect of international migration on health is abundant and it is mainly focused on the effects that it produces on the health of immigrants and on the impact that the drain of health professionals has on health systems. However, the interest for studying the impact of migration on health has increased in the countries of origin, since developing countries are those which produce most emigrants and the health of population, as well as the possibility that the former has to access to health services, constitute key elements to achieve economic development (2).
There is evidence that international migration may affect the health of all the members in the household that stay in the countries of origin. For instance, it can negatively affect the health of children since they receive less preventive health care (3) or it constitutes a stressful situation that affects psychological wellbeing (4,5,6). It could also present positive effects such as the increase of the expenditure and demand of health services as a result of the reception of remittances (7,8,9), the improvement of child nutrition indicators (10,11) and the decrease of child mortality (12).
International migration affects the health of adolescents and youngsters when enabling the acquisition of unhealthy habits such as smoking (13) and producing emotional stress (14). Mental health of women may also be affected (15,16,17), as well as the diet of older adults (18). On the other hand, emigrants and returned migrants, can also transfer values, norms and practices acquired abroad for the benefit of their communities that may affect health outcomes (19,20).
Several are the ways through which migration (emigration, return, remittances) affects health outcomes in the countries of origin, diverse are the health outcomes that may be affected and the effects can be positive, negative or appear in both directions. In spite of the fact that migration effects on people that stay in the countries of origin are multidimensional, studies generally focus on only one part of them, making it difficult to understand its true impact. For instance, when a study focuses on anthropometric measures, it can put to one side the psychological aspects that could simultaneously be affected.
The study of the effects of international migration on health outcomes of people and households in the countries of origin is a less-paid attention subject in comparison to the studies focused on the destination countries. Therefore, this systematic review pretends to contribute with a broad panorama of the different ways in which international migration may affect health outcomes in the countries of origin. This effect can take place due to: 1) families may receive remittances, or have a family member who has returned or is living abroad; and 2) the health of returned migrants may have been affected by the previous migratory experience.
In this sense, this systematic review is addressed by the following question: which are the effects that international migration, seen from remittances, return or emigration, produce on the health condition of people or households in the countries of origin?
Methods
The systematic review was carried out in two phases. In the first, which did not include the PubMed database and concluded on March 16th, 2016, published articles between January 1st, 2000 and January 1st, 2016 were searched. In the second phase, which concluded on August 21st, 2017, published articles between January 1st, 2000 and August 15th, 2017 were searched in the PubMed database and published articles between January 1st, 2016 and August 15th, 2017 were searched in the other databases.
The following descriptors in English and Spanish were used for the search: health (salud), mortality (mortalidad), morbidity (morbilidad), disease (enfermedad), mental health (salud mental), mental illness (enfermedad mental), nutrition (nutrición), child health (salud infantil), infant mortality (mortalidad infantil), health expenditure (gasto en salud), remittances (remesas), international migration (migración internacional), emigration (emigración) and return migration (migración de retorno). The last four descriptors were combined with each of the considered possible health outcomes. Each database was reviewed independently by two authors and results of the search were compiled using Mendeley. It is worth mentioning the fact that the search is limited to published articles only in Spanish or English may be a potential source of bias, since it excludes published articles in other languages.
Data from Ebsco, Jstor, Proquest, Pubmed, IDEAS RePec, Scielo and Google Schoolar were taken into account for the review of articles. The Boolean connector “and” was used in all cases. Keywords were combined with the conjunction “and” in the databases which do not have the option to choose the Boolean connector (IDEAS RePec, Scielo and Google Scholar).
Original articles, published in scientific journals and working papers that represented empirical, quantitative or qualitative works were included. Thesis, editorials, articles based on opinion or reflection, systematic reviews, book chapters or texts presented in academic events were established as exclusion criteria. The articles that marginally referred to the subject were also excluded; those that focused on internal migration or did not differentiate between internal or international migration and the articles that treat health condition as a determining factor of migration or focus on the effects on the countries of destination were also excluded.
The search strategy showed 471 academic articles and working papers: Ebsco (91), Jstor (27), Proquest (109), IDEAS RePec (59), Scielo (49), Google Schoolar (95) and Pubmed (41) (this figure includes duplicates). After the review process, 85 articles remained. Figure 1 describes in detail the process of the systematic review
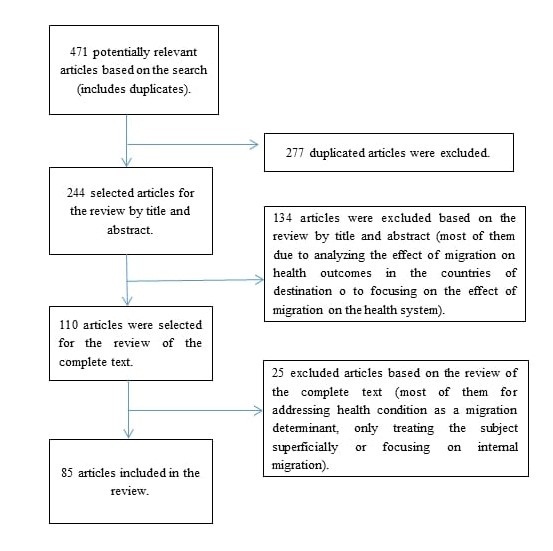 Figure 1.
Process of systematic review
Figure 1.
Process of systematic review
Source: own work
For purposes of analysis, the
information extracted from the studies was: author(s), year of publication, target
population, sample size, city and country, objective, type of study,
recollection technique and data analysis, main results and conclusions. These
data were systematized in a table of evidence that would allow its subsequent
categorization and analysis. From this systematization, three categories under
which the works could be classified were: 1) the effect of emigration or the
return of a family member on the health of the members of the households in the
country of origin (36 articles), 2) the effect of transfers, monetary and
non-monetary (ideas) on health or health expenditure of households in the
countries of origin (27 articles), 3) the effect of the migratory experience on
the health condition of those who returned (8 articles). Some articles analyzed
two of these categories at the same time (14 articles).
Results
The systematic review produced 85
articles, from which 73 were published in scientific journals that received
peer evaluation and the others were working papers on economics. No published
studies that complied with the inclusion criteria were found in 2000 and 2001.
81.2% of the studies were published between 2009 and 2017. Most articles (88.2%)
were published in English. The country in which the selected studies focused the
most was Mexico (38 articles). Table 1 shows the total of documents by country in
each region. Most of the studies found in Mexico can be due to its broad
migratory tradition and to limiting the search to two languages.
Table 1.
Number of
studies by region and country
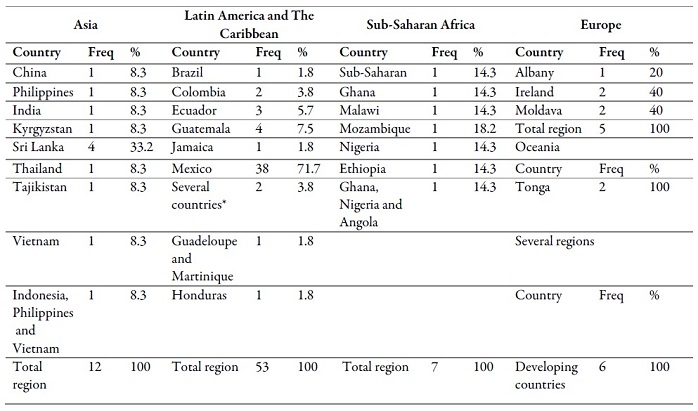
*
Bolivia, Ecuador, El Salvador, Guatemala, Haiti,
Honduras, Mexico, Nicaragua, Paraguay, Peru and Dominican Republic.
Source: own
work, based on reviewed literature
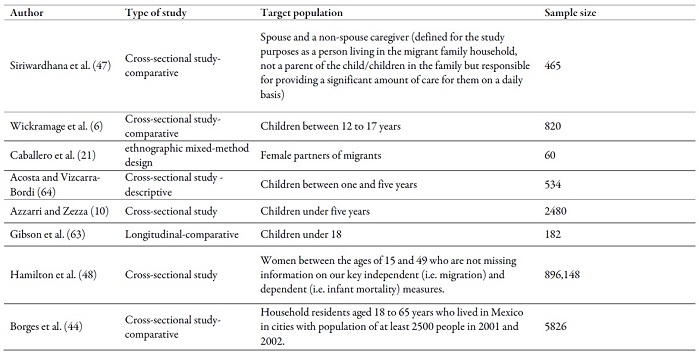
In general terms, the target populations of the reviewed articles were: 1) children, 2) adolescents, 3) women, 4) older adults and 5) households. Seventy-eight quantitative articles, 4 qualitative articles (21,22,23,24) and three mixed were found (4,25,26). Seventy three percent of the works reviewed corresponded to cross-sectional studies (sixty-two articles). Of these, thirty-six articles, were comparative, of which three were descriptive, and one related to cases and controls. 22% of the studies were longitudinal (nineteen articles), the majority of these being comparative (twelve articles). Of the work with a qualitative approach, ethnographic designs (four articles) and narrative (two articles) predominated. The type of study, target population and sample size of each of the reviewed studies are described in annex 1. Approximately, 43.5% of the studies reported the presence of selection bias due to un-observed variables and inverse causality, which can cause endogeneity problems, which, if untreated, may produce biased estimations of the impact of migration on health outcomes. This problem was more common in the studies that analyzed the effect of remittances on health expenditure or some health-related outcomes. The strategies most used to avoid biased estimations were the instrumental variables (12,27,28,29,30,31,32,33,34), estimation through the methods Propensity Score Matching and the models of difference in differences (35,36), as well as the use of estimators of fixed effects, in the case of the models with panel data (37,38,39).
Figure 2 shows the different health outcomes that, in the countries of origin are affected by international migration, according to the reviewed literature.
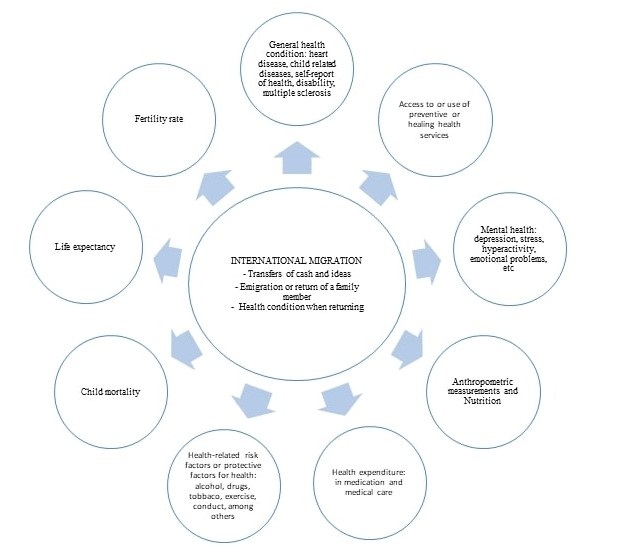 Figure
2.
Health
outcomes affected by international migration in the countries of origin
Figure
2.
Health
outcomes affected by international migration in the countries of origin
Source: own work, based on reviewed literature
Effect of emigraton or return of a family member on health
conditions of the household in the origin countries
The fact of having a migrant or a returnee brings about changes in the household that can have an influence on health outcomes . These changes have to do with the responsabilities taken on by the members of the household, gender-related roles, and the supply of care, support and supervision.
According to Banerjee et al. (40), women, for instance, can be forced to take on new responsibilities, with which the fertility rate can be affected and prenatal and postnatal care can decrease, having an influence on variables such as early death of their children in migrant households. Contrary to Lindstrom and Muñoz-Franco (41), women who have migrant relatives have a greater probability of receiving prenatal and postnatal care and assistance at birth, due to the decrease of financial and cultural barriers, by means of remittances and the diffusion of new ideas, attitudes and behaviors.
Jayatissa and Wickramage (42) support the idea that migration decreases childcare because of the time limitations of the father, and Schmeer (43) that it can explain the lack of support and supervision that children require, contributing to the generation of diseases or diarrhea. Naturally, if the mother, in the country of origin, has greater autonomy and resources, the effect can be positive. Likewise, the lack of supervision that migrants can carry out on their children, could be associated with the use and abuse of substances such as alcohol, marihuana and cocaine by the migrants’ relatives in Mexico (44).
Additionally, the support that migrant children cannot give to older parents can be associated with the fact that these suffer from a mental illness or have experienced a heart attack or a cardiovascular accident (45). Barrett and Mosca (46) found that especially older mothers of migrant children were depressed and felt lonely.
On the other hand, international migration can create stress among the family members who stay. According to Pottinger (5), migration of parents represents a potential trauma for the children that stay, placing them in a situation of higher risk regarding psychosocial problems. Smeekens et al. (14), obtained similar results when concluding that adolescents missed their parents very much and felt lonely and stressed, which affected their physical condition; and Ming-Hsuan (13), for whom children with migrant parents had less chances of being vaccinated and were more likely to smoke, can be associated with a deficient family relationship or a weak connection with their parents in their youth.
Rivera-Heredia et al. (25) studied the perception of daughters, mothers, wives or sisters of migrants on the stressful events associated with international migration (absence of partner, uncertainty and concern for the migrant, lack of money and children’s health). They found that women can experience loneliness, sadness and anger, as well as fatigue, insomnia and depression. To similar conclusions reached Siriwardhana (23) in a study for Sri Lanka about the migrants spouses.
Additionally, international migration affects the social networks of support with which the families of migrants rely on. However, according to Frank (17), even though women with migrant spouses dealt with greater stress and less support during pregnancy, the probability of low weight at birth did not increase and birth results were positive. This might be due to better conduct practices of women; naturally, excluding those whom are less willing to exclusively breastfeed their babies. In the same way, Azzarri and Zezza (10) suggest that migration has a negative impact on the duration of exclusive breastfeeding, if their job imposes additional restrictions of time to breastfeeding mothers, and these know and can access breast milk substitutes more easily.
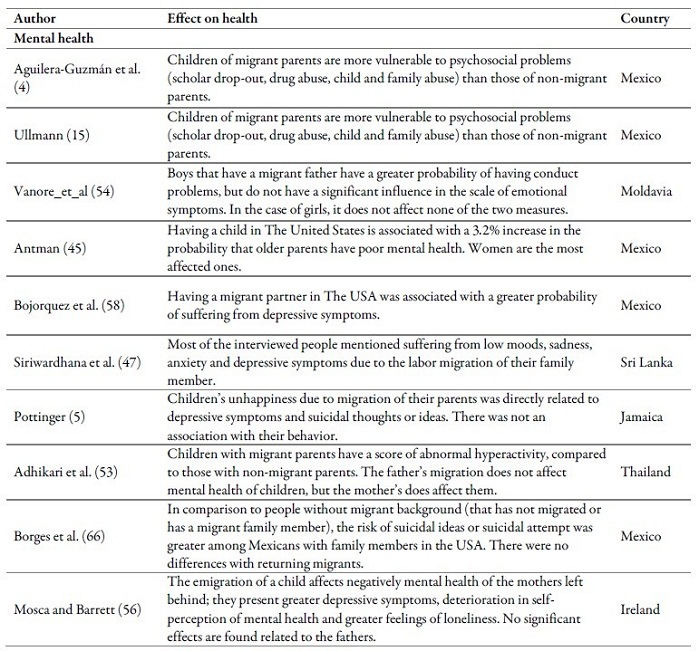
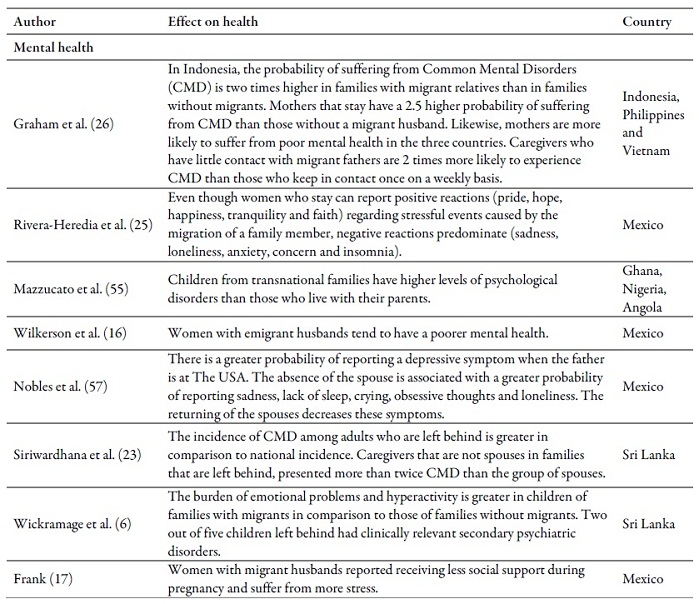
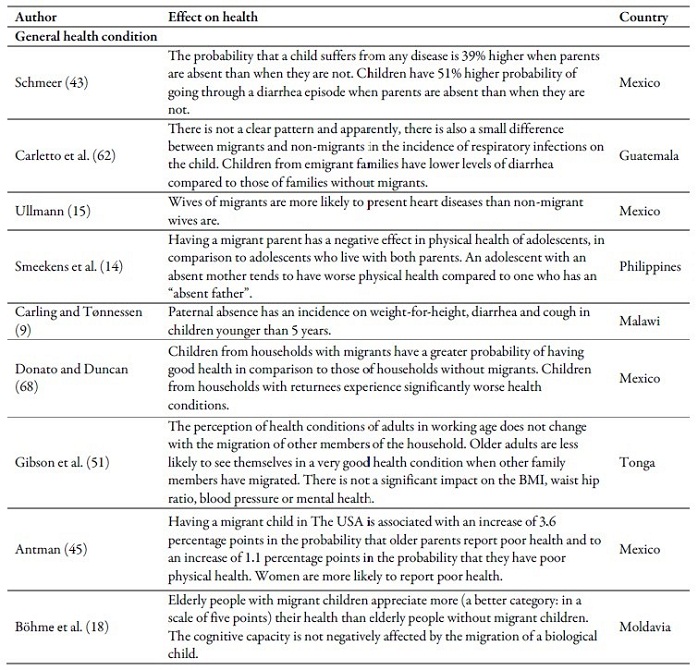
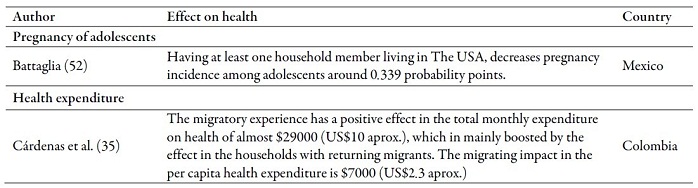
Table 2 summarizes the main results of the articles that deal with the effect of emigration or the return of a family member on health in the countries of origin. Some studies found positive effects; others, negative ones. With regard to child mortality, all the articles found positive effects (3,47,48,49). The opposite occurred with risk factors, the migration of a family member increases the probability that children and/or adolescents smoke (13), consume more alcohol or psychoactive substances (4) and exercise less (50). It also affects alcohol consumption of older adults (44,51). Child care practices decrease (42) and the contagion risk of HIV/ITS increases (22). On the other hand, the migration of a family member decreases the incidence of pregnancy in adolescents (52).
Negative effects were found in different indicators of mental health in children (5,53,54), adolescents (4,6,55), caregivers (26,23), older adults (45,56), wives of the migrants (15,16,25,57), spouses (23) and members of the household in general (58).
Migration also has positive effects on the access to private health services (59), healing (60), and of antenatal control (61), as well on the use of contraceptive methods (41). In contrast, the migration of a family member family can negatively affect vaccinations of children (3,13) and the search of medical care of grandparents (23).
With respect to the indicators that describe the general health conditon, results are ambiguous. While some studies found that the migration of the parents or a family member was associated with a better self-reported health condition (18) and the decrease of the Body Mass Index and blood pressure (51), other unfavorable results such as the increase of the probability that children younger than 5 years suffer from a disease due to the absence of their parents (9,43), the deterioration of physical health of adolescents (14), the decrease in the propensity to self-report good health (45,51), the increase of the report of heart diseases (15).
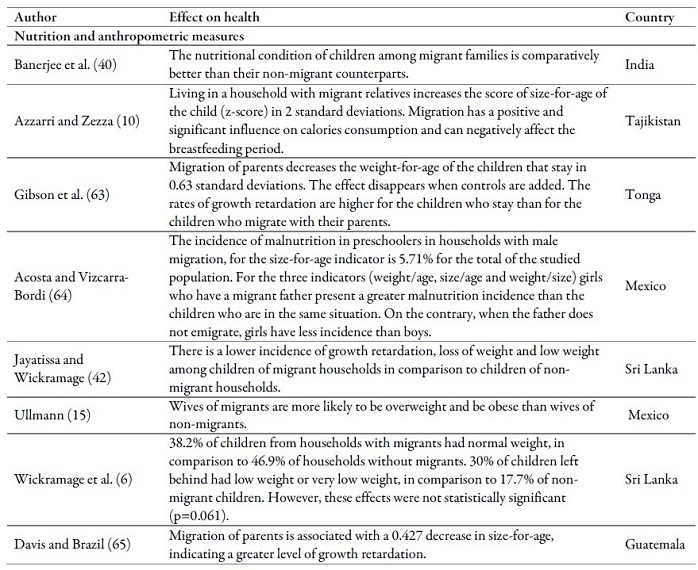
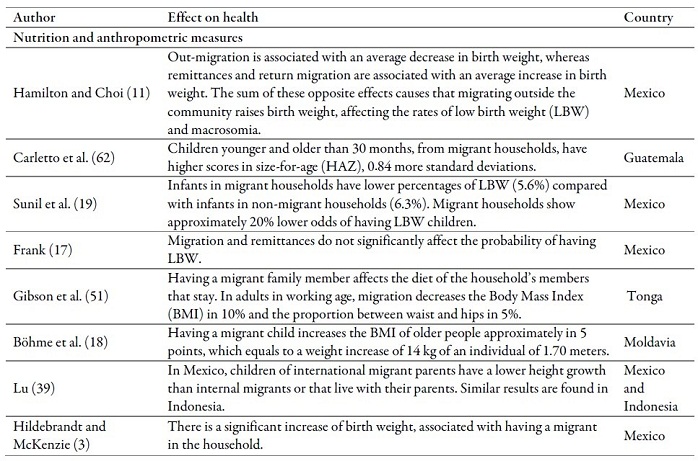
Results in terms of the effects on the anthropometric measures and nutritional condition are not convincing either. There is evidence of positive impacts on the children’s nutritional condition (10,40), the diet of older adults (18), the increase of weight at birth (3,19), the weight conditions of children younger than 15 years old (9) and the decrease in the prevelance of growth retardation (62,42). However, some studies reported negative effects such as the worsening of the diet of the household members (51,63), malnutrition among pre-schoolers (64), children younger than 18 years old would present growth retardation (63,65), the migrants’ wives (15), and children between 1 and 5 years old were overweight (64), a part from the abandonment of exclusive breastfeeding (10).
In the countries of origin, the health of families may be affected by the return of any of their members. In fact, according to Cárdenas et al. (35), in Colombia, the migratory experience has a positive influence on the total health expenditure per month; mainly due to the effect on households with returned migrants.
However, several studies carried out for Mexico reached to similar conclusions. Hamilton and Choi (11) found that return migration was associated to a lower risk of low birth weight and to a higher risk of macrosomy. To Flores et al. (49), in the Mexican states, an increase of 10% in the households with returned migrants may be associated to a decrease of 5.5% in child mortality rates; which may be related to the exposition to practices that produced better child health results in the United States (66,67,68).
Donato and Duncan (68) studied children’s health in three types of Mexican families: 1) those who lived in the United States, 2) those who had returned from the United States, and 3) those who lived in Mexico and had never had a migratory experience. They found that children’s health was better in the families who lived in the United States, and significantly worse when they lived in returned families. A possible explanation to this was the called ‘salmon effect’, according to which, the ones who returned were the least healthy and successful.
Finally, Hernández-Rosete et al. (22) found that indigenous women of the Mexican rural zone were in risk of contracting AIDS, since they felt they were forced into having un-protected sex when their husbands returned from the United States; despite the fear that they were infected with the virus, as a result of having being unfaithful. Additionally, men were seeking to get them pregnant and control them.
Other authors did not find evidence that migration or the return of a family member affected health-related outcomes, such as mental health of children (5,53) and older adults, (18), suicidal risk (66), the health perception of people (35), child mortality (67), the probability of low weight at birth (17), or malnutrition (64). Ullmann (15) does not find that having a migrant husband compared to not having one produces significant differences in hypertension, diabetes or having smoked once.
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
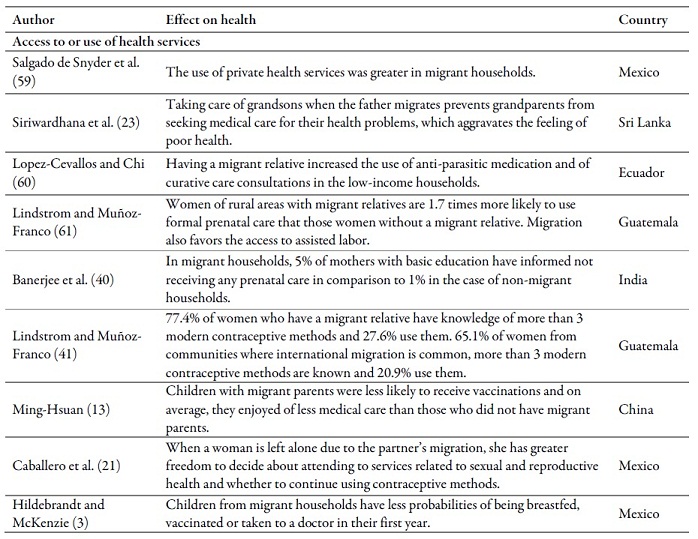
Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
Souce: own work, based on
reviewed literature
Table 2
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin

Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin

Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
Souce: own work, based on
reviewed literature
Table 2.
Main
effects of emigration or return of a family member on health outcomes in the
countries of origin
Souce: own work, based on
reviewed literature
Effect of transfers on health conditions of the household in
the origin countries
Family, financial and political connections are established among the countries of origin and destination, beyond their borders. Not only the emigrant modifies his cultural elements and those related to his identity, but he also helps reproducing the socio-cultural system of the place of origin. With migration, the cultural horizons of the communities of origin and destination broaden; lifestyles, ideas about family and the way to consume and behave also change. This exchange of knowledge and ways of living comprises the set of non-monetary transfers that complement remittances and produce effects on different aspects; including the health of the households in the countries of origin.
International migration can be considered as a determining factor in health of the countries of origin, due to its capacity to alter socio-economic and psichosocial circumstances of individuals and families. The migration effect on health is caused in part, by means of monetary transfers (remittances), or non-monetary transfers (cultural practices, norms and social arrangements) (17). It is clear that remittances can decrease during economic crisis, which affects health outcomes of the receiving families (number of visits to the hospital to take care of medical emergencies or amount of money destined to buy medications) (69). Remittances and repatriated savings alter the levels of income and wealth and the contact with health practices used in the countries of destination, increases knowledge about health and makes the use of financial resources more efficient (3).
According to Wilkerson et al. (16), migration of spouses can negatively affect mental health of women when they are forced to perform a different gender role than the one they are traditionally used to. On the contrary, according to Azzarri and Zezza (10), the impact on nutrition can be positive, considering remittances and the possibility than women can handle the budget, which increases the intake of kilocalories in the household and the growth patterns of children improve.
Remittances relieve income restrictions of households, enabling the purchase of medication, nutritional food and health services, which increases life expectation and decreases the child mortality rate (34). The effect on the percentage of health expenditure is also positive, especially for the households without an employment insurance (70,71). Likewise, Salinas (24) found that returning elder migrants could access to private health services and medications, due to remittances. On the contrary, Valero and Trevino (72) found that families with less resources can be far from starting to spend on health, in spite of the fact that their income increases marginally (remittances), since they consider that health is a need they can postpone in order to attend more important or imperative matters.
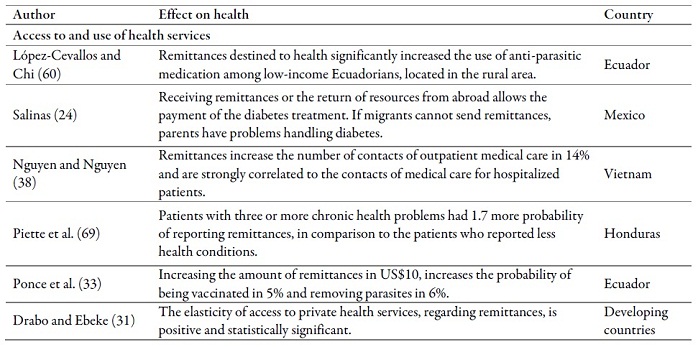
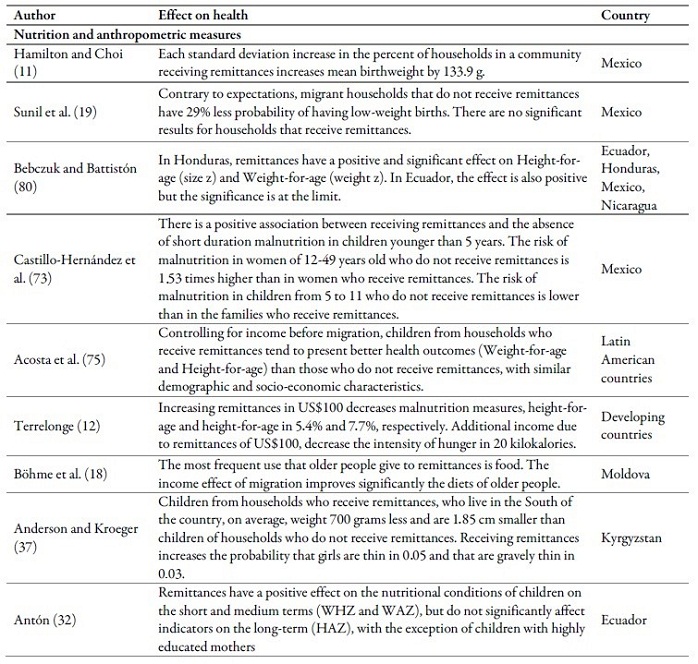
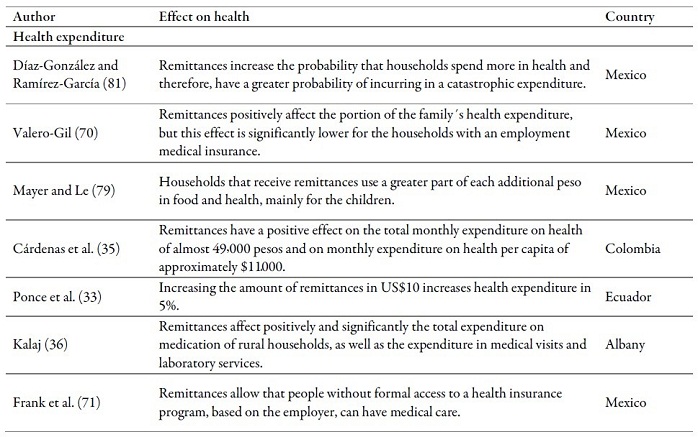
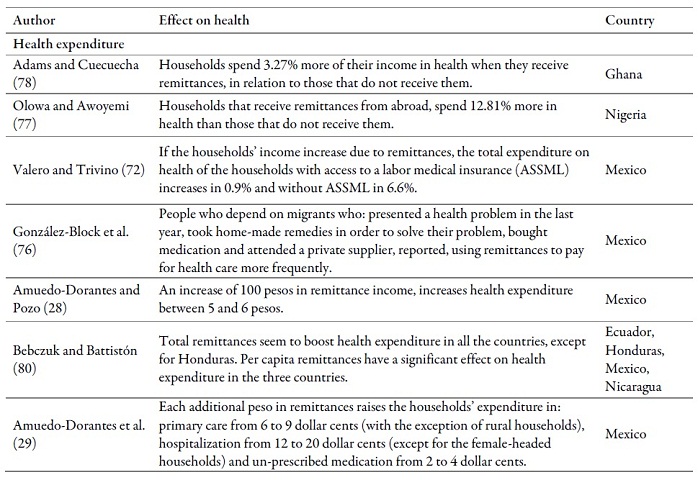
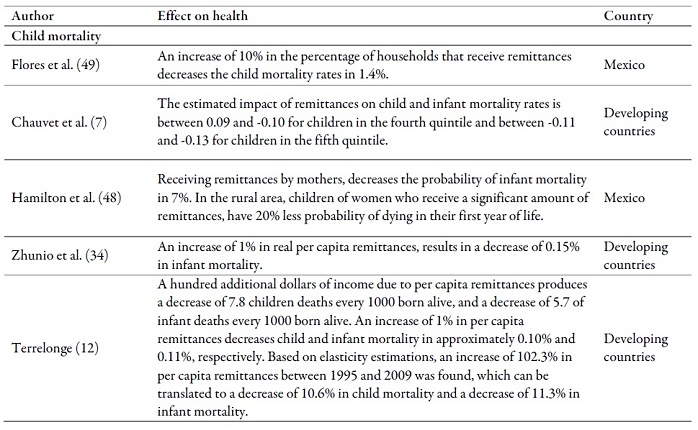
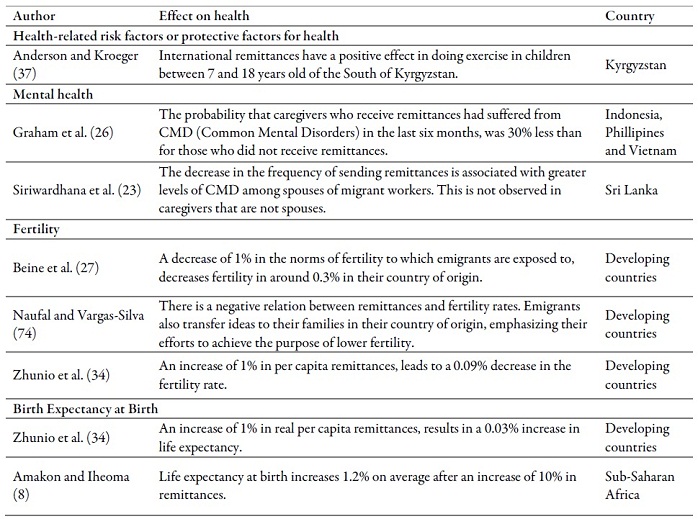
Table 3 relates the main impacts that, may produce transfers, of cash or ideas, on health outcomes in the countries of origin. In general, results tend to be positive regarding the access to and use of health services, nutrition, fertility, mortality, life expectancy at birth, health expenditure and general health condition.
Regarding the access to or use of health services, it can be highlighted that receiving remittances affects positively the use of antiparastitic (60) and diabetes (24) medication, the use of outpatient and non-outpatient health services by children (38) and the substitution of public health services for private ones (31). On the other hand, patients who report the decrease of remittances are less likely to visit a hospital and take less prescribed medication (69).
In regards to nutrition, receiving remittances is associated with improvements in the nutritional condition of children younger than 5 years (12,32,73). There is as well an asociation between receiving remittances and the decrease of fertility rates (27,34,74) and child mortality (7,12,34,49). Regarding the general health condition, receiving remittances decreases the probability of suffering from a chronic or sudden disease (36) and improves health outcomes, including the children’s (7,8,75).
In reference to health expenditure, receiving remittances increases medication expenditure (29,76), hospitalization (29), medical visits and laboratoy services (36), preventive health activities (33) and, in general, the total health expenditure of households (8,28,33,35,70,72,77,78,79,80,81).
On the other hand, regarding anthropometric measures, results are ambiguous. Some authors find that households that receive remittances present better anthropometric measures (11,32,75), while others find negative results about these indicators (19,37). Similar results are found in terms of risk factors or protectors. Some studies find a positive association between remittances and doing exercise (37) and others find negative effects (50).
Some studies did not find evidence that remittances affected health outcomes such as the proportion of children who attend school with malnutrition (73), consumption of health services (35), access to public health services (31), health expenditure of households (12), child mortality (65,67) and that measure the long-term health condition of children (growth retardation, low weight), the prevalence of respiratory diseases and of diarrhea (33).
Table 3.
Main effects of cash transfers and of ideas
on health outcomes in the countries of origin

Source: own work, based on reviewed literature
Table 3.
Main effects of cash transfers and of ideas
on health outcomes in the countries of origin
Source: own work, based on reviewed literature
Table 3.
Main effects of cash transfers and of ideas
on health outcomes in the countries of origin
Source: own work, based on reviewed literature
Table 3.
Main effects of cash transfers and of ideas
on health outcomes in the countries of origin
Source: own work, based on reviewed literature
Table 3.
Main effects of cash transfers and of ideas
on health outcomes in the countries of origin
Source: own work, based on reviewed literature
Table 3.
Main effects of cash transfers and of ideas
on health outcomes in the countries of origin
Source: own work, based on reviewed literature
Effects of migratory experience on the health condition of those
who returned
Health outcomes in the countries of origin can be affected by the return of nationals, since, when returning, they can be older, sick, disabled or having suffered a deportation, which would place them in vulnerable position. However, it is also possible that who return have the economic means to attend their needs regarding health services.
According to Wong and González-González (82), migrants can return to the country of origin being older adults and suffering from some degree of disability or poverty, when they have been subdued to intense physical work in the countries of destination. For Bojorquez et al. (83), this result can be worse in the case of forced returnees, among which greater predominance of common mental problems can be present
In fact, Habtamu et al. (84) found that Ethiopian migrants who returned from the Middle East and South Africa, experienced symptoms of common mental disorders (headaches, lack of appetite, fatigue, insomnia and feeling of unhappiness or nervousness). This psychological distress and even long-term mental illnesses could be related to adversities experienced by immigrants in the different migratory stages (not receiving their salary on time, not having contact with their families, lack of awareness on the type of work they must carry out and lack of necessary knowledge and abilities for the work, etc.).
For Fernández-Niño et al. (85), deported ones are more likely to perceive their own health as poor or very poor, which is an expression of the accumulation of vulnerabilities to which they have been exposed to, considering their undocumented condition. Barrett and Mosca (46) found that returned women had less problems with alcohol, inasmuch as, the benefits of the migratory experience (sense of independence and control) exceeded the costs (nostalgia). On the contrary, returned men had a greater dependence on alcohol, due to the stress caused by migration.
Cabre et al. (86) studied the probability that migration had an influence on the risk of developing multiple sclerosis in the French Antilles. They found that the appearance of this disease had a more environmental origin rather than a genetic one and could be due to the fact that migrants would have introduced the factors that precipitated it or to that in the Antilles, the environmental factors that protected the population from this disease would have disappeared.
Finally, the greater predominance of smoking and obesity among returned Mexicans after living in The United States can be by cause of their greater economic capacity to buy cigarettes, food and high calorie drinks. Their emotional and psychiatric disorders can be the result of anti-migrant legislation and hostile political climate that Mexican immigrants deal with in The United States (20).
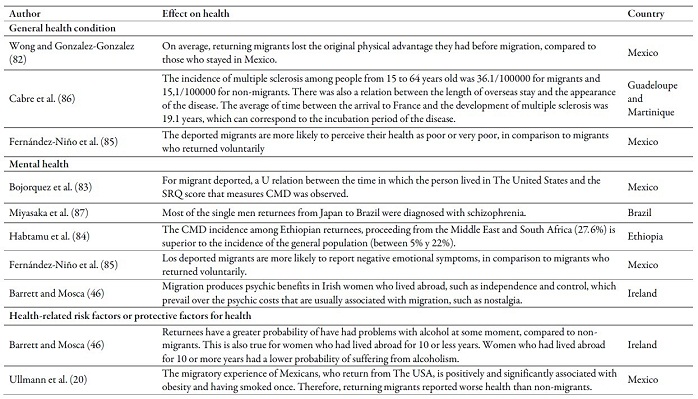
Table 4 shows that the migratory experience may produce positive or negative effects on mental health of migrants who return to their country of origin. The other health indicators analyzed in the studies are negatively affected. For instance, results in the French Antilles, show that the prevalance of multiple sclerosis was higher among those who returned than in those who had not migrated (86). In other cases, the migratory experience was positively associated with the presence of heart desease and obesity among those who returned (20) and with greater disability in older adults (82). Those who were deported were more likely to perceive poor health conditions (85), and have more risk factors, such as alcohol consumption (46) and smoking (20).
Regarding mental health, women report having the feeling of independence and control as a pyschic benefit, which prevails over psychic costs like nostalgia (46). Other authors found unfavorable results on mental health. For instance, Miyasaka et al. (87) could establish that migrants who returned from Japan to Brazil were mainly single men with a psychiatric history, to which schizophrenia was diagnosed, associated with the loneliness that they had experienced during their stay abroad. Ullmann et al. (20) positively related the migratory experience of returnees to Mexico to emotional or psychiatric disorders. Regarding the deported returnees, Fernández-Niño et al. (85) found them more likely to report negative emotional symptoms and Bojorquez et al. (83) associated a longer stay at The United States with a greater presence of common mental disorders (CMD) in Mexico. Similar results were found in Ethiopia in (84).
Finally, some authors did not find that the migratory experience affected certain health outcomes in the country of origin. For instance, Ullmann et al. (20) did not find an association between the migratory experience and the report of good health in adults and Borges et al. (66) did not find any differences in regards to suicidal risk among individuals without a personal mirgration history or migrant family members, and returned migrants.
Table 4.
Main effects of the migratory experience on the health
condition of the returnees
Source: own work, based on reviewed literature
Conclusions
The objective of this work is to carry out a literature review aimed at answering the following research question: which are the effects of international migration – seen as remittances, return or emigration – on the households’ health results or on people in the contries of origin.
The review of articles was carried out systematically, by means of an exhasutive and rigurous analysis of several data bases, according to previously established eligibility cirteria. Likewise, data extracted from every document was recorded in a table of evidence and the review methodology was clearly presented; through which any person can reproduce it.
Considering that the objective was providing a global view of the stage of the research in the topic, among the criteria for selecting articles, the methdological aspects were not taken into account, in order not to exclude those that contribute with the problem’s understanding. Indeed, great methodological heterogeneity among the articles reviewed was found. This impeded contrasting populations, sample sizes and types of studies in the way demanded by a systematic literature review to reach to strong conclusions that this type of review assures.
As expected, en general terms, results are not consistent. For the same health indicator, the effect of international migration may differ among countries and considering different groups of population, considering gender, ethnic group and age. This may also be due to the complexity of international migration and health depending on multiple factors. The migratory phenomenon in the countries of origin, apart from obbeying to multiple causes, comprises remittances, return and emigration. Health outcomes are due to genetic, environmental, socio-economic factors and life styles, some of which may be influenced by the migratory experience of the family member who emigrated or returned.
According to the documents reviewed, the fact that a family member of the household had emigrated or returned has different effects on health. It positively affects the general health condition, the anthropometric measures, nutrition and child mortality and, negatively, mental health and risk factors. With regard to access to health services, most studies reported positive effects.
In general terms, cash or non-cash transfers, have a positive influence on health of the countries of origin. On the other hand, many of the authors that studied the health condition of the returnees found that the migratory experience affected health in a negative way .
Several reasons can affect health as a consequence of international migration. Remittances, specifically, strengthen the household’s finances and decrease the need of child labor, producing an increase in the access to health services and expenditure in this area. Separation of parents and children can decrease the support and supervision provided to children, fostering the acquisition of harmful habits and harboring feelings of anger and sadness. This can also decrease the influence of pregnancy among adolescents.
Migrants and those who returned may transfer predominant behavioral rules in their countries of destination and contribute to modify ideas and cultural practices that have an influence on health, in the same way that migration of the spouse can modify the gender roles within the households and increase the responsibility of women, causing their mental health to be affected.
This review will be highly useful for those who study the subject. It will enable the advance in the research to be determined, the exisitng voids, the new questions that may arise, the most appropriate methodologies to answer them, as well as the less studied countries and populations. It would be interesting to establish, for instance, until what point, results on the health of the countries of origin when it is the mother who migrates, differ.
Therefore, in view of the considerable dimension that international migration has assumed, and the importance of health in terms of human development, there is a need for more studies to be put forward. These studies could take into consideration the construction of compound indicators that integrate several health outcomes, given that international migration can simultaneaoulsy affect different aspects of health. Also, qualitative research that enables the analysis of quantitative results in wider social and cultural contexts must be encouraged, as well as accessing people’s lives, their daily routines and their social relationships.
References
1. World Bank. Migration: Overview [Internet]. 2016 [access 2016 Nov. 22]. Available at: https://www.worldbank.org/en/topic/migrationremittancesdiasporaissues/overview
2. World Health Organization. Health and the Millennium Development Goals [Internet]. 2005 [access 2016 Jan. 12]. Available at: http://www.who.int/hdp/publications/mdg_en.pdf
3. Hildebrandt N, McKenzie DJ. The Effects of Migration on Child Health in Mexico. Economía. 2005;6(1):257-289.
4. Aguilera-Guzmán RM, Salgado-de-Snyder VN, Romero M, Medina-Mora ME. Paternal absence and international migration: stressors and compensators associated with the mental health of mexican teenagers of rural origin. Adolescence. 2004;39(156):711-723.
5. Pottinger AM. Children’s experience of loss by parental migration in inner-city Jamaica. Am J Orthopsychiatry. 2005;75(4):485-496.
6. Wickramage K, Siriwardhana C, Vidanapathirana P, Weerawarna S, Jayasekara B, Pannala G, et al. Risk of mental health and nutritional problems for left-behind children of international labor migrants. BMC Psychiatry. 2015;15(39):1-12.
7. Chauvet L, Gubert F, Mesple-Somps S. Aid, Remittances, Medical Brain Drain and Child Mortality: Evidence Using Inter and Intra-Country Data. J Dev Stud. 2013;49(6):801-818.
8. Amakom U, Iheoma CG. Impact of Migrant Remittances on Health and Education Outcomes in Sub-Saharan Africa. IOSR-IJHSS. 2014;9(8):33-44.
9. Carling J, Tønnessen M. Fathers’ whereabouts and children’s welfare in Malawi. Dev. South. Afr. 2013;30(6):724-742.
10. Azzarri C, Zezza A. International migration and nutritional outcomes in Tajikistan. Food Policy. 2011;36(1):54-70.
11. Hamilton ER, Choi KH. The mixed effects of migration: Community-level migration and birthweight in Mexico. Soc Sci Med. 2015;(132):278-286.
12. Terrelonge SC. For Health, Strength and Daily Food: The Dual Impact of Remittances and Public Health Expenditure on Household Health Spending and Child Health Outcomes. J Dev Stud. 2014;50(10):1397-1410.
13. Ming-Hsuan L. Migration and Children’s Welfare in China: The Schooling and Health of Children Left behind. J Develop Area. 2011;44(2):165-182.
14. Smeekens C, Stroebe MS, Abakoumkin G. The impact of migratory separation from parents on the health of adolescents in the Philippines. Soc Sci Med. 2012;75(12): 2250-2257.
15. Ullmann SH. The health impacts of international migration on Mexican women. Glob. Public Health. 2012;7(9):946-960.
16. Wilkerson JA, Yamawaki N, Downs SD. Effects of husbands’ migration on mental health and gender role ideology of rural Mexican women. Health Care Women Int. 2009;30(7):614-628.
17. Frank R. International Migration and Infant Health in Mexico. J. Immigr. Health. 2005;7(1):11-22.
18. Böhme MH, Persian R, Stöhr T. Alone but better off? Adult child migration and health of elderly parents in Moldova. J Health Econ. 2015;39:211-227.
19. Sunil TS, Flores M, Garcia GE. New evidence on the effects of international migration on the risk of low birthweight in Mexico. Matern Child Nutr. 2012;8(2):185-198.
20. Ullmann SH, Goldman N, Massey DS. Healthier before they migrate, less healthy when they return? The health of returned migrants in Mexico. Soc Sci Med. 2011;73(3):421-428.
21. Caballero M, Leyva-Flores R, Ochoa-Marín SC, Zarco Á, Guerrero C. Las mujeres que se quedan: Migración e implicación en los procesos de búsqueda de atención de servicios de salud. Salud Pública Méx. 2008;50(3):241-250.
22. Hernández-Rosete D, Maya García O, Bernal E, Castañeda X, Lemp G. Migración y ruralización del SIDA: relatos de vulnerabilidad en comunidades indígenas de México. Rev. Saúde Pública. 2008;42(1):131-138.
23. Siriwardhana C, Wickramage K, Jayaweera K, Adikari A, Weerawarna S, Van-Bortel T, et al. Impact of Economic Labour Migration: A Qualitative Exploration of Left-Behind Family Member Perspectives in Sri Lanka. J Immigr Minor Health. 2015;17(3):885-894.
24. Salinas JJ. Tapping Healthcare Resource by Older Mexicans with Diabetes: How Migration to the United States Facilitates Access. J Cross Cult Gerontol. 2008;23(3):301-312.
25. Rivera-Heredia ME, Obregón-Velasco N, Cervantes-Pacheco EI. Migración, sucesos estresantes y salud: perspectivas de las mujeres michoacanas de comunidades rurales con familiares migrantes. Acta Univ. 2013;23(1):49-59.
26. Graham E, Jordan LP, Yeoh BS. A. Parental migration and the mental health of those who stay behind to care for children in South-East Asia. Soc Sci Med. 2015;132:225-235.
27. Beine M, Docquier F, Schiff M. International Migration, Transfers of Norms and Home Country Fertility [Working Paper]. Geneva: The World Bank, Development Research Group, Trade Team; 2009; 44925.
28. Amuedo-Dorantes C, Pozo S. New Evidence on the Role of Remittances on Health Care Expenditures by Mexican Households [Discussion Paper]. Bonn, Germany: IZA; 2009; 4617.
29. Amuedo-Dorantes C, Sainz T, Pozo S. Remittances and Healthcare Expenditure Patterns of Populations in Origin Communities: Evidence from Mexico [Working paper]. Buenos Aires, Argentina: Inter-American Development Bank, Integration and Regional Programs Department; 2007; 25.
30. Medina C, Cardona L. The Effects of Remittances on Household Consumption, Education Attendance and Living Standards: the Case of Colombia. Lect Econ. 2010;(72):11-43.
31. Drabo A, Ebeke C. Remittances. Public Health Spending and Foreign Aid in the Access to Health Care Services in Developing Countries [Working paper]. Clermont Ferrand, France: Cerdi; 2010.
32. Antón JI. The Impact of Remittances on Nutritional Status of Children in Ecuador. International Migration Review. 2010;44(2):269-299.
33. Ponce J, Olivié I, Onofa M. The role of international remittances in health outcomes in Ecuador: Prevention and response to shocks. Int Migr Rev. 2011;45(3):727-745.
34. Zhunio MC, Vishwasrao S, Chiang EP. The influence of remittances on education and health outcomes: a cross country study. App. Econ. 2012;44(35):4605-4616.
35. Cárdenas M, Medina C, Trejos A. Measuring Economic and Social Impacts of Migration in Colombia: New evidence [Working paper]. Bogotá, Colombia: Banco de la República; 2010; 601.
36. Kalaj EH. A Micro-level Analysis of the Effect of Remittances on Health Expenditures: Evidence from Albania. Mediterr J Soc Sci. 2015;6(1):665-673.
37. Anderson K, Kroeger A. Remittances and Children`s Capabilities: New Evidence from Kyrgyzstan, 2005-2008 [Discussion paper]. Bonn, Germany: Forschungsinstitut zur Zukunft der Arbeit; 2012; 6293.
38. Nguyen C, Nguyen H. Do Internal and International Remittances Matter to Health, Education and Labor of Children? The Case of Vietnam [Working paper]. Munich, Germany: Personal RePec Archive, MPRA; 2013; 48672.
39. Lu Y. Internal migration, international migration, and physical growth of left-behind children: A study of two settings. Health Place. 2015;36:118-126. https://www.doi.org/10.1016/j.healthplace.2015.09.008
40. Banerjee SK, Jayachandran V, Roy TK. Has Emigration Influenced Kerala’s Living Standards? A Micro Level Investigation. Econ Polit Wkly. 2002;37(18):1755-1765.
41. Lindstrom DP, Muñoz-Franco E. Migration and the diffusion of modern contraceptive knowledge and use in rural Guatemala. Studies in Family Planning. 2005;36(4):277-288.
42. Jayatissa R, Wickramage K. What Effect Does International Migration Have on the Nutritional Status and Child Care Practices of Children Left Behind? Int. J. Environ. Res. Public Health. 2016;13(218):1-10.
43. Schmeer K. Father absence due to migration and child illness in rural Mexico. Soc Sci Med. 2009;69(8):1281-1286.
44. Borges G, Medina-Mora ME, Breslau J, Aguilar-Gaxiola S. The effect of migration to the United States on substance use disorders among returned Mexican migrants and families of migrants. Am J Public Health. 2007;97(10):1847-1851.
45. Antman FM. Adult Child Migration and the Health of Elderly Parents Left Behind in Mexico. Am. Econ. Rev. 2010;100(2):205-208.
46. Barrett A, Mosca I. The psychic costs of migration: Evidence from Irish return migrants. J. Popul. Econ. 2013;26(2):483-506.
47. Siriwardhana C, Wickramage K, Siribaddana S, Vidanapathirana P, Jayasekara B, Weerawarna S, et al. Common mental disorders among adult members of “left-behind” international migrant worker families in Sri Lanka. BMC Public Health. 2015;(15):1-9.
48. Hamilton ER, Villarreal A, Hummer RA. Mother’s, household, and community U.S. migration experience and infant mortality in rural and urban Mexico. Popul. Res. Policy Rev. 2009;28(2):123-142.
49. Flores M, Sunil T, Picazzo-Palencia E, Cortez-Hernandez DE. A Spatial Analysis of the Effects of International Migration on Infant Mortality in Mexico. Soc Dev Issues. 2012;34(2):1-15.
50. Palos-Lucio G, Flores M, Rivera-Pasquel M, Salgado-de-Snyder VN, Monterrubio E, Henao S, et al. Association between migration and physical activity of school-age children left behind in rural Mexico. Int J Med. Public Health. 2015;60(1):49-58. https://www.doi.org/10.1007/s00038-014-0630-2
51. Gibson J, McKenzie D, Stillman S. The Impacts of International Migration on Remaining Household Members Omnibus Results from a Migration Lottery Program [Working paper]. Washington, DC: The World Bank Development Research Group, Trade and Integration Team; 2009; 4956.
52. Battaglia M. Migration, health knowledge and teenage fertility: Evidence from Mexico. SERIEs. 2015;6(2):179-206.
53. Adhikari R, Jampaklay A, Chamratrithirong A, Richter K, Pattaravanich U, Vapattanawong P. The Impact of Parental Migration on the Mental Health of Children Left Behind. J. Immigr. Minor. Health. 2014;16(5):781-789. https://www.doi.org/10.1007/s10903-013-9809-5
54. Vanore M, Mazzucato V, Siegel M. “Left behind” but not left alone: Parental migration & the psychosocial health of children in Moldova. Soc Sci Med. 2015;132:252-260.
55. Mazzucato V, Cebotari V, Veale A, White A, Grassi M, Vivet J. International parental migration and the psychological well-being of children in Ghana, Nigeria, and Angola. Soc Sci Med. 2015;132:215-224.
56. Mosca I, Barrett A. The Impact of Adult Child Emigration on the Mental Health of Older Parents [Discussion paper]. Bonn, Germany: The Institute for the Study of Labor (IZA); 2014; 8037.
57. Nobles J, Rubalcava L, Teruel G. After spouses depart: Emotional wellbeing among nonmigrant Mexican mothers. Soc Sci Med. 2015;132:236-244.
58. Bojorquez I, Salgado-de-Snyder N, Casique I. International migration of partner, autonomy and depressive symptoms among women from a mexican rural area. Int. J. Soc. Psychiatry. 2009;55(4):306-321.
59. Salgado-De-Snyder VN, González-Vázquez T, Infante-Xibille C, Márquez-Serrano M, Pelcastre-Villafuerte B, Serván-Mori EE. Servicios de salud en la Mixteca: Utilización y condición de afiliación en hogares de migrantes y no-migrantes a EU. Salud Pública Méx. 2010;52(5):424-431.
60. López-Cevallos DF, Chi C. Health Care Utilization in Ecuador. Rev Panam Salud Públ. 2012;31(1):9-16.
61. Lindstrom DP, Muñoz-Franco E. Migration and maternal health services utilization in rural Guatemala. Soc Sci Med. 2006;63(3):706-721.
62. Carletto C, Covarrubias K, Maluccio JA. Migration and child growth in rural Guatemala. Food Policy. 2011;36(1):16-27.
63. Gibson J, McKenzie D, Stillman S. What happens to diet and child health when migration splits households? Evidence from a migration lottery program. Food Policy. 2011;36(1):7-15.
64. Acosta LD, Vizcarra-Bordi I. Desnutrición infantil en comunidades mazahuas con migración masculina internacional en México Central. Poblac. Salud Mesoam. 2009;6(2):118.
65. Davis J, Brazil N. Migration, Remittances and Nutrition Outcomes of Left-Behind Children: A National-Level Quantitative Assessment of Guatemala. PLOS ONE. 2016;11(3):1-17.
66. Borges G, Breslau J, Su M, Miller M, Medina-Mora ME, Aguilar-Gaxiola S. Immigration and suicidal behavior among Mexicans and Mexican Americans. Am J Public Health. 2009;99(4):728-733.
67. Yabiku ST, Agadjanian V, Cau B. Labor migration and child mortality in Mozambique. Soc Sci Med. 2012;75(12):2530-2538.
68. Donato KM, Duncan EM. Migration, Social Networks, and Child Health in Mexican Families. J. Marriage Fam.. 2011;73(4):713-728.
69. Piette JD, Mendoza-Avelares MO, Chess L, Milton EC, Reyes AM, Rodriguez-saldaña J. Report on Honduras: ripples in the pond-the financial crisis and remittances to chronically ill patients in Honduras. Int. J. Health Serv. 2012;42(2):197-212.
70. Valero-Gil J. Remittances and the Household’s Expenditures on Health. J Bus Strat. 2009;26(1):119-140.
71. Frank R, Palma-Coca O, Rauda-Esquivel J, Olaiz-Fernández G, Díaz-Olavarrieta C, Acevedo-García D. The relationship between remittances and health care provision in Mexico. Am. J. Public Health. 2009;99(7):1227-1231.
72. Valero JN, Trevino MDL. El gasto en salud de los hogares en México, y su relación con la disponibilidad de recursos, las remesas y la asignación intrafamiliar. Econo. Mex. (Nueva Época). 2010;19(2):311-342.
73. Castillo Hernández JL, Álvarez Ramírez MM, Romero Hernández EY, Cortés SC, Zenteno-Cuevas R, Berrún-Castañón LN. Asociación de las remesas con el estado nutricio y la adecuación de la dieta en habitantes de la localidad El Espinal, municipio de Naolinco, Veracruz, México. Rev. Avanc. Seg. Alim. y Nutr. 2009;1(1):77-87.
74. Naufal G, Vargas-Silva C. Changing Fertility Preferences One Migrant at a Time: The Impact of Remittances on the Fertility Rate [Discussion paper]. Bonn, Germany: The Institute for the Study of Labor (IZA); 2009; 4066.
75. Acosta P, Fajnzylber P, Lopez H. The Impact of Remittances on Poverty and Human Capital: Evidence from Latin American Household Surveys [Working paper]. Washington, DC: The World Bank; 2007; 4247.
76. González-Block MÁ, De-la-Sierra-de-la-Vega LA, Vargas-Bustamante A. Utilización de remesas de migrantes en California para atención a la salud de sus dependientes en México. Salud Pública Méx. 2013;55(4):459-468.
77. Olowa OW, Awoyemi TT. Remittances and Household Expenditure in Rural Nigeria. J Rural Econ Dev. 2009;20(1):30-43.
78. Adams RH, Cuecuecha A. The Impact of Remittances on Investment and Poverty in Ghana. World Dev. 2013;50:24-40.
79. Mayer D, Le Thi ML. El uso de las transferencias privadas inter-vivos por los hogares: el caso de México. Estud Demogr Urb. 2008;23(2):233-269.
80. Bebczuk R, Battistón D. Remittances and Life Cycle Deficits in Latin America [Working paper]. La Plata, Argentina: Universidad Nacional de la Plata; 2010; 94.
81. Díaz-González E, Ramírez-García JB. Gastos catastróficos en salud, transferencias gubernamentales y remesas en México. Pap Pobl. 2017;23(91):65-91.
82. Wong R, Gonzalez-Gonzalez C. Old-Age Disability and Wealth Among Return Mexican Migrants From the United States. J. Aging Health. 2010;22(7):932-354.
83. Bojorquez I, Aguilera RM, Ramírez J, Cerecero D, Mejía S. Common Mental Disorders at the Time of Deportation: A Survey at the Mexico–United States Border. J. Immigr. Health. 2015;17(6):1732-1738.
84. Habtamu K, Minaye A, Zeleke WA. Prevalence and associated factors of common mental disorders among Ethiopian migrant returnees from the Middle East and South Africa. BMC Psychiatry. 2017;17(1):1-12.
85. Fernández-Niño JA, Ramírez-Valdés DJ, Cerecero-Garcia D, Bojorquez-Chapela I. Deported Mexican migrants: Health status and access to care. Rev. Saúde Pública. 2014;48(3):478-485.
86. Cabre P, Signate A, Olindo S, Merle H, Caparros-Lefebvre D, Béra O, Smadja D. Role of return migration in the emergence of multiple sclerosis in the French West Indies. Brain. 2005;128(12): 2899-2910.
87. Miyasaka SL, Canasiro S, Abe Y, Otsuka K, Tsuji K, Hayashi T, et al. Migration and mental health: Japanese Brazilians in Japan and in Brazil. J. Bras. Psiquiatr. 2007;56(1):48-52.
Annex
Annex 1
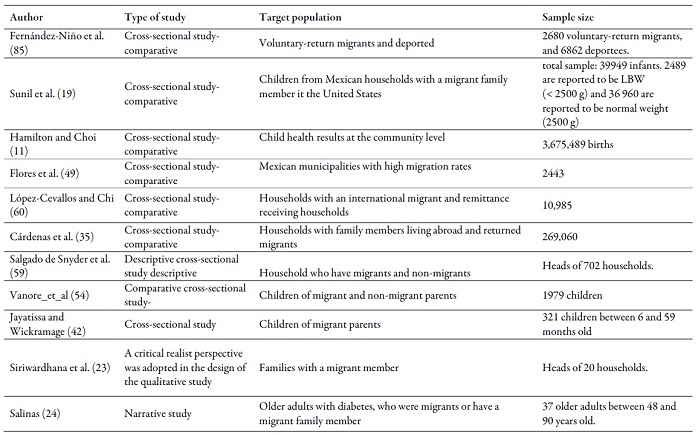
Type of study, target population and sample
size of the works reviewed
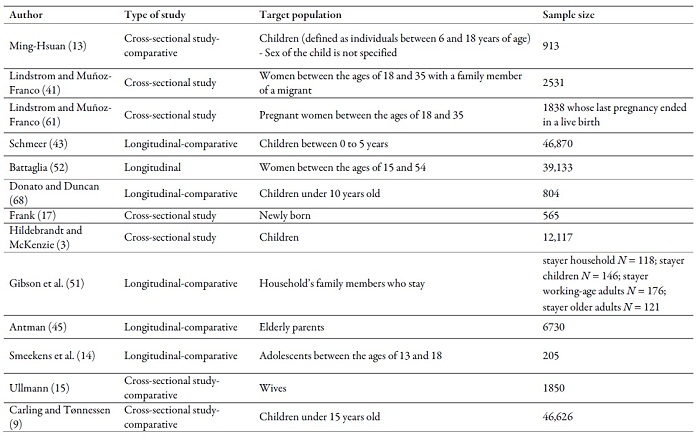
Source: own work, based on reviewed
literature
Annex 1.
Type of study, target population and sample
size of the works reviewed

Source: own work, based on reviewed
literature
Annex 1.
Type of study, target population and sample
size of the works reviewed

Source: own work, based on reviewed
literature
Annex 1.
Type of study, target population and sample
size of the works reviewed
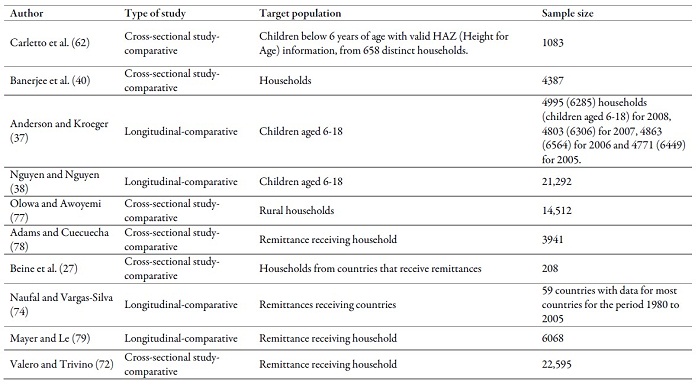
Source: own work, based on reviewed
literature
Annex 1
Type of study, target population and sample
size of the works reviewed
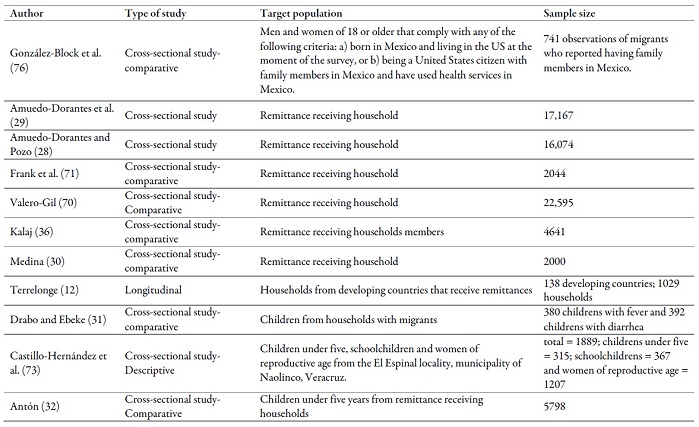
Source: own work, based on reviewed literature
Annex 1.
Type of study, target population and sample
size of the works reviewed
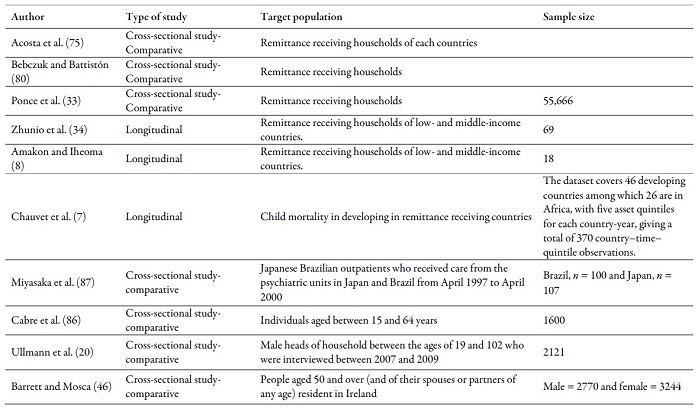
Source: own work, based on reviewed literature
Annex 1.
Type of study, target population and sample
size of the works reviewed
Source: own work, based on reviewed literature
Annex 1.
Type of study, target population and sample
size of the works reviewed
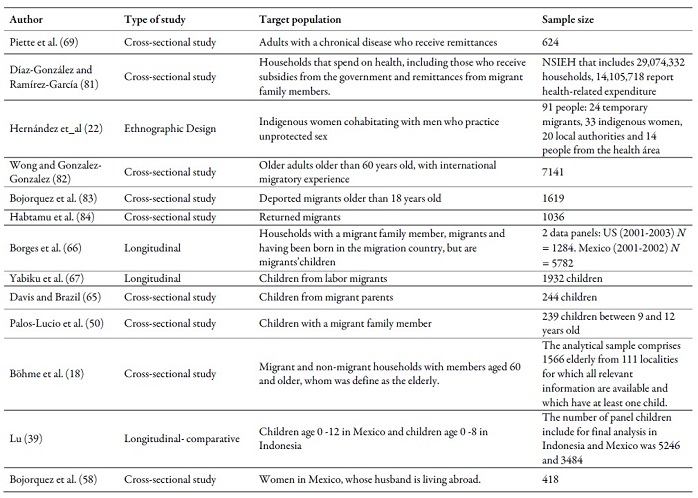
Source: own work, based on reviewed literature
Notes
*
Research article
Author notes
a Corresponding author. E-mail: luismtovar@gmail.com
Additional information
How
to cite this article:: Tovar-Cuevas LM, Victoria-Paredes MT, Zarama C, Arellano-Morales M. International migration and health in the countries of origin. The effect on households with migrants and/or recipients of remittances, and on returned migrants. A systematic review. Revista Gerencia y Políticas de Salud. 2019;18(37). https://doi.org/10.11144/Javeriana.rgps18-37.imhc