Introduction
Family health problems influence the individual health, since the latter is determined by healthy or pathogenic practices followed by the family group. A healthy family lifestyle promotes the health of its members, whereas an unhealthy family lifestyle can make the family members sick (1).
It is considered that the relationship between individual and family health is a two-way issue, that is, the influence is reciprocal. Individual health develops in the context of a family, with the formation of habits, lifestyles, value systems, norms, attitudes and behaviors towards health (1,2).
On the other hand, hypertension is a highly prevalent process in all countries, whether developed or not, and affects almost 40% of adults; it is also the main cause of death and disability worldwide through its cardiovascular complications. In the genesis of this high prevalence and incidence, multiple authors point to the change in lifestyle as a generator —at least partial— of this very negative evolution (3,4,5).
The scarce physical activity and sedentary behaviors are associated with dysfunctional aspects of family dynamics (6). The prevalence of a sedentary lifestyle is greater in women, increases as their age increases and has been related to the enlargement of the waist circumference; furthermore, it has been described that sedentary people have an increase in their heart rate that could be related as a sign of cardiovascular system involvement (7).
Individuals who live in family dysfunction develop bad eating habits (8), that is, a dysfunctional family environment and a single parent structure are risk factors for overweight and obesity (9).
The determination of anthropometric indices are tools for predicting hypertension, due to their strong association (10,11). The presence of conflict between parents is associated with a more deteriorated bond between parents and children and greater consumption of alcohol and other drugs (12).
In the province of Loja there is a high prevalence of risk factors for arterial hypertension, among which are overweight and obesity, with 63.9%; alcohol consumption, with 40.6%; tobacco consumption, with 42.3%; physical inactivity, with 55.8%, and prehypertension, with 34.8% (13). Hence, lifestyle not only influences the onset and development of arterial hypertension, but also its control (14,15).
Treating high blood pressure and its complications requires costly interventions that deplete governmental and individual budgets, so that lifestyle changes, through early detection and control of risk factors, generate both health and economic benefits (16,17,18,19,20).
Changes in lifestyles such as smoking cessation, reduction of excess weight, moderation of alcohol consumption, physical activity, reduction of salt intake, increase of fruit and vegetable intake, together with reduction of the consumption of saturated fats, can contribute to lower blood pressure rates (21).
The objective of this research was to determine the relationship between family functionality and modifiable risk factors for arterial hypertension in adults from 20 to 64 years of age from the city of Loja, Ecuador.
There are few studies on the influence of the family on health risk behaviors, so the relationship between family functionality and the modifiable risk factors for arterial hypertension is unknown.
Materials and Methods
Type of Study
A cross-sectional, correlational, analytical study was
conducted during November 2015 and October 2016, in a random sample of individuals
between 20 and 64 years of age.
Design of the Research
In the development of the present project, field research
was used, based on information from surveys and direct observation of the participants.
Calculation of the Sample
Size
The data from the Ecuador Population and Housing Census 2010 was taken as a basis, considering the age group between 20 and 64 years of the urban parishes of the city of Loja (97,223 adults). The number of surveys was determined applying the Pita Fernández formula with an expected proportion of 5%, a confidence level of 95% and an accuracy of 5%.
To determine the number of surveys that were to be carried out in each of the four urban parishes of the city of Loja, a classification performed in subgroups or strata with similar environmental (altitude and latitude) and demographic (population density in adults from 20 to 64 years of age) characteristics. The number of surveys in each parish was divided by the number of neighborhoods and the blocks in which the instrument was applied were randomly drawn using Excel®. The work was carried out with a minimum desired power of 80%, and its verification was carried out using the G*Power® software, with which a total number of 414 people was obtained.
The inclusion criteria were: men and women from 20 to 64 years of age who agreed to be part of this study. The exclusion criteria were: refusal to participate in the study, pregnant women, people with intellectual or physical disabilities that made it difficult to take anthropometric measurements, body mass index less than 18.5 kg/m2, patients diagnosed with or under treatment for arterial hypertension. Once the stratification and randomization was done, the roadmap was developed to apply the instrument in the field and collect the information.
Techniques Used to Collect the Information
The secondary information was collected with the help of documents and information
about the work context. The primary information was obtained by applying a survey
addressed to the participants who were asked to answer objectively and concretely
the items proposed.
Ethics
There was an informed consent, which let the participants know about the
purpose of the study, its importance, the procedures that were to be carried out,
as well as that their participation is voluntary and that they can change their
mind later and stop participating, although they had accepted before.
Procedure to Collect the Data
Family functionality. It was determined applying the Family Function Perception Test, which assesses the cohesion, harmony, communication, permeability, affectivity, roles and adaptability of the family. A pilot test was carried out on 30 individuals with similar characteristics and a Cronbach’s alpha of 0.768 was obtained, with an acceptable internal consistency.
Degree of tobacco consumption. It was determined according to the parameters and stratification of the World Health Organization (WHO). Likewise, a pilot test was applied on 30 individuals with similar characteristics and a Cronbach’s alpha of 0.803 was obtained, with a good internal consistency.
Degree of alcohol consumption. It was established according to the parameters of the Alcohol Use Disorder Identification Test (AUDIT). For the local validation of the AUDIT, a pilot test was carried out on 30 individuals with similar characteristics and a Cronbach’s alpha of 0.873 was obtained, with a good internal consistency.
Physical activity. It was determined through the International Physical Activity Questionnaire. This is a short, self-administered format of the last 7 days. After a pilot test on 30 individuals with similar characteristics, a Cronbach’s alpha of 0.727 was obtained, with an acceptable internal consistency.
Body Mass Index (BMI). It was established using a weight/height scale previously calibrated to meet the international standards and scales in kilograms and in linear meters. The nutritional status was classified based on the WHO stratification, according to the body mass index (Weight [kg]/height [m2]).
Blood pressure. It was determined by the auscultatory method with a calibrated and properly validated tensiometer. The patients remained seated and still in a chair for at least 5 minutes, with the feet on the floor and the arm at the height of the heart with an adequate size of bracelet (that surpasses at least 80% the arm). The systolic blood pressure was taken as the point at which the first of two or more sounds is heard (phase 1), and the diastolic blood pressure, as the point after which the sound disappears. The blood pressure indices were classified based on the parameters of the Spanish Society of Cardiology.
Method and Model of Analysis. Once the collection instrument was applied, the data was systematized and tabulated with the SPSS program (version 16.0). The relationship of variables was analyzed applying the Pearson’s chi-square statistical test. To measure the association between the variables studied, it was necessary to calculate the Cramer V coefficient. Regarding the odds ratio (OR), to determine protective or risk factors, we worked on dichotomous tables and confidence limits with an interval of 95%.
Results
The sample consisted of 414 participants (132 men and 282 women), with an average age of 38.41 years, of which 68.1% were female. The prevalence of family dysfunction was 52.17%; low level of physical activity, 74.88%; tobacco consumption, 26.09%; overweight-obesity, 73.91%; altered blood pressure (normal high), 21.01%, and risky alcohol consumption, 35.75% (see annexes).
Family dysfunction was a risk factor for: low level of physical activity, since a χ2
c value of 11.97 was found (p<0.05 [0.007]; OR: 1.61; 95% CI: 1.03-2.52); tobacco consumption, with a χ2
c of 10.53 (p<0.05 [0.015]; OR: 1.63; 95% CI: 1.04-2.55); overweight-obesity, with a χ2
c of 10.49 (p<0.05 [0.015]; OR: 1.77; 95% CI: 1.13-2.76); altered blood pressure, with a χ2
c of 21.37 (p<0.05 [0.000]; OR: 2.00; 95% CI: 1.22-3.28); risky alcohol consumption, with a χ2
c of 62.91 (p<0.05 [0.000]; OR: 5.69; 95% CI: 3.59-9.01).
Discussion
The results of the study show a statistically significant association between family functionality and risk factors for hypertension, such as low physical activity, tobacco consumption, overweight-obesity, normal high blood pressure and risky alcohol consumption; however, the magnitude of this association, determined by the Cramer’s V coefficient, ranges from 0.17 to 0.39, which establishes a low to moderate degree of association, and this relationship should, therefore, be investigated further.
In the nutritional diagnosis of the population studied, classified according to the BMI, overweight-obesity was prevalent, with 73.91%, similar to what occurred in the study by Freire et al. (13), where an overweight-obesity prevalence of 62.8% was observed.
Family dysfunction is a risk factor for the development of scarce physical activity. The correlation between family dysfunction and tobacco consumption contrasts with the results of the study by Santander et al. (22), where participants belonging to households perceived as dysfunctional had a significantly higher risk of tobacco use (OR: 1.46; 95% CI: 1.02-2.07; p<0.03).
Family dysfunction constituted a risk for the development of overweight-obesity, results similar to those obtained in the study by González-Rico et al. (23), in which there was an association between family dysfunction and obesity (OR: 1.63; 95% CI: 1.08-2.46; p<0.01).
Participants with family dysfunction presented altered blood pressure, results that could be compared with the study by González et al. (24), where it was shown that 84.13% of dysfunctional families showed lack of control of blood pressure levels (χ2: 54.6, p = 0.0000, Cramer V: 0.4223).
The association between family dysfunction and alcohol consumption determined in this study is comparable with the results of the study by Musitu et al. (25), which shows a positive and significant relationship between a negative family functionality and substance use (β = 0.15, p<0.01), among these alcohol.
Conclusions
There is a statistically significant relationship between family function and risk factors for arterial hypertension. The data support the hypothesis that family dysfunction constitutes a predisposing factor for the development of risk factors for arterial hypertension.
The analysis of this relationship contributes to the advancement of knowledge and is very useful as a basis for delineating family and community preventive strategies.
Conflicts
of interest
The authors declared no conflicts of
interest.
Acknowledgements
We thank the study participants for their collaboration in obtaining the data.
Sponsored by the Post-graduate Program in Family and Community Medicine of the National University of Loja, Ecuador, in collaboration with the Ministry of Public Health of Ecuador and financed by the International Development Bank. Reviewed by Dr. Angélica Gordillo. Specialist in Internal Medicine, treating doctor at the Isidro Ayora Hospital of Loja. Professor of the Human Health Area at the National University of Loja.
References
1. González I. Reflexiones acerca de la salud familiar. Rev Cubana Med Gen Integr. 2000;16(5):508-12.
2. Rodríguez J, López N, Tamayo O, Rodríguez S. La familia como célula fundamental de la sociedad en la atención primaria de salud. Rev Cubana Tecnol Salud. 2015;5(3):48-53.
3. Amicucci M, Gonçalves M, Guimarães L, Amaral L. Hipertensión arterial y estilo de vida en Sinop, Municipio de la Amazonía Legal. Arq Bras Cardiol. 2010;94(5):621-6.
4. Ordúñez P, Pérez E, Hospedales J. Más allá del ámbito clínico en el cuidado de la hipertensión arterial. Rev Panam Salud Pública. 2010;28(4):311-8.
5. Weschenfelder D, Gue Martini J. Hipertensión arterial: principales factores de riesgo modificables en la estrategia salud de la familia. Enferm Global. 2012;11(26):344-53.
6. Lavielle P, Pineda V, Jáuregui O, Castillo M. Actividad física y sedentarismo: determinantes sociodemográficos, familiares y su impacto en la salud del adolescente. Rev Panam Salud Pública. 2014;16(2):161-72.
7. Moreno J, Cruz H, Angarita A. Evaluación de razones de prevalencia para sedentarismo y factores de riesgo en un grupo de estudiantes universitarios. Chía-Colombia. Enferm Global. 2014;7(34):114-22.
8. Mejía G, Salazar F, Sanabria L, Polanía H, Lizcano P, Medina R. Caracterización sociodemográfica y familiar de obesos intervenidos a través de cirugía bariátrica en el Hospital Universitario de Neiva. Revista Facultad de Salud. 2014;6(1):59-66.
9. Flores J, Sánchez F. Estructura y funcionalidad familiar en el desarrollo de sobrepeso y obesidad en escolares Zacatecanos. Ibn Sina. 2011;1-15.
10. Afrifa E, Agyemang C, Ardey S, Ogedegbe G, Graft A. The association of physical activity, body mass index and The association of physical activity, body mass index and the blood pressure levels among urban poor youth in Accra Ghana. BMC Public Health. 2015;15(1):1-9. doi: http://doi.org/10.1186/s12889-015-1546-3.
11. Lee J, Lim N, Baek T, Park S, Park H. Anthropometric indices as predictors of hypertension among men and women aged 40-69 years in the Korean population: The Korean Genome and Epidemiology Study. BMC Public Health. 2015;15(1):140. doi: http://doi.org/10.1186/s12889-015-1471-5.
12. Fantin MB, García HD. Factores familiares, su influencia en el consumo de sustancias adictivas. Ajayu. 2011;9(2):193-214.
13. Freire W, Belmont P, Gómez L, Mendieta M, Monge R, Piñeiros P, et al. Tomo I: Encuesta Nacional de Salud y Nutrición de la población ecuatoriana de cero a 59 años. ENSANUT-ECU 2012. Quito: Ministerio de Salud Pública/Instituto Nacional de Estadísticas y Censos; 2014.
14. Córdoba R, Cabezas C, Camarelles F, Gómez J, Díaz D, López A, et al. Recomendaciones sobre el estilo de vida. Atención Primaria. 2012;44(1):16-22.
15. Roca A, Coll C. Medidas no farmacológicas en el tratamiento antihipertensivo. Atención Primaria. 2010;36(2):1-29. doi: http://doi.org/10.1016/S0212-6567(05)70581-3.
16. Fuentes L, Muñoz A. Efectos de una intervención integral en la reducción de factores de riesgo cardiovascular en mujeres con sobrepeso u obesidad de la Región de Los Ríos. Rev Med Chile. 2010;138:974-81.
17. Galán A, Cuixart C, Villar F, Navarro J, Lobos J, Ortega R, et al. Recomendaciones preventivas cardiovasculares. Atencion Primaria. 2014;44(1):3-15.
18. Giraldo A, Toro M, Macías A, Valencia C, Palacio S. La promoción de la salud como estrategia para el fomento de estilos de vida saludables. Hacia la Promoción de la Salud. 2010;15(1):128-43.
19. Organización Mundial de la Salud (OMS). Información general sobre la hipertensión en el mundo. Washington: OMS; 2013. p. 1-39.
20. Shafieyan Z, Qorbani M, Rastegari Mehr B, Mahboubi M, Rezapour A, Safari O, et al. Association between lifestyle and hypertension in patients referred to health care centers of Ilam City in 2014. Glob J Health. 2015;8(6):161-7.
21. Calvo C, Waisman G, Juncos L. Hipertensión arterial: objetivos y estrategias del tratamiento farmacológico. Atención Primaria. 2010;1-11.
22. Santander S, Zubarew T, Santelices L, Argollo P, Cerda J, Bórquez M. Influencia de la familia como factor protector de conductas de riesgo en escolares chilenos. Rev Med de Chile. 2008;136(3):317-24. doi: http://doi.org/10.4067/S0034-98872008000300006.
23. González-Rico J, Vásquez-Garibay E, Cabrera-Pivaral C, González-Pérez G, Troyo-Sanromán R. La disfunción familiar como factor de riesgo para obesidad en escolares mexicanos. Rev Med Inst Mex Seguro Soc. 2012;50(2):127-34.
24. González A, González N, Vásquez Y, González L, Gómez R. Importancia de la participación familiar en el control de la hipertension arterial. Medicentro [internet]. 2004;8(2):3-9. Available at: http://www.sld.cu/galerias/pdf/servicios/hta/importancia_de_lafamilia_en_el_control_de_la_hta_.pdf
25. Musitu G, Jiménez T, Murgui S. Funcionamiento familiar, autoestima y consumo de sustancias en adolescentes: un modelo de mediación. Salud Pública Méx. 2007;49(1):3-10. doi: http://doi.org/10.1590/S0036-36342007000100002.
Annex
Annex 1. Relationship between family dysfunction and
risk factors for arterial hypertension

Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex
2. Distribution of Adults by Age and Gender
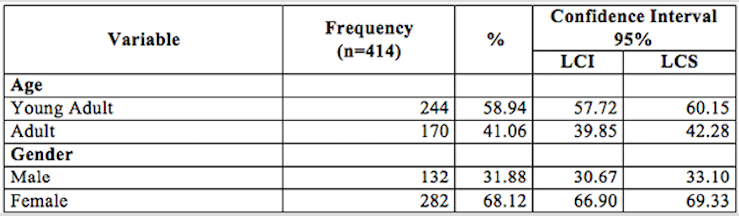
Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex 3. Prevalence of Family Dysfunction
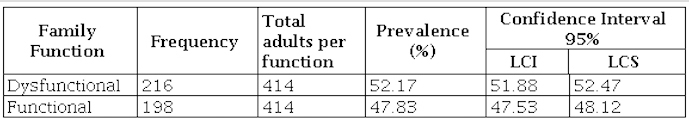
Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex 4. Prevalence of Scarce Physical Activity

Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex 5. Prevalence of Tobacco Consumption

Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex 6. Prevalence of Overweight-Obesity
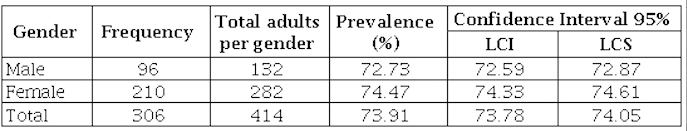
Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex 7. Prevalence of normal high blood pressure

Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Annex 8. Prevalence of Risky Alcohol Consumption

Source:
Direct research 2016. Database of the research project Family factors and their relationship with modifiable risk factors for hypertension
in adults from 20 to 64 years of age Loja 2016. UNL-ASH. Prepared by: MD Jorge Poma.
Author notes
a
Corresponding author. E-mail: jorgeluispomamingaok@gmail.com
Additional information
How to cite: Poma J, Carrillo L, González
J. Family functionality and modifiable
risk factors for arterial hypertension. Univ Med. 2018;59(1): xx-xx. doi: https://doi.org/10.11144/Javeriana.umed59-1.ffha