Introduction
The world is experiencing a demographic transition with a noticeable increase in the population aged 60 years or older. This phenomenon, which is particularly rapid in Latin American countries, is a great medical and social achievement. However, this brings social, cultural, economic and health challenges, given the high prevalence of chronic diseases, among which dementia and cognitive impairment are specially important (1).
The worldwide prevalence of dementia is estimated to be 35.6 million, and it is expected to rise to 150 million in 2050 (2). It is the third leading cause of death in Europe, accounting for 8.57% of the total number of deaths (2). Neurocognitive disorders can significantly affect the quality of life of elderly people and their families (3).
Therefore, it is important to detect interventions that make it possible to develop effective strategies to prevent and control risk factors for the onset of cognitive impairment (4), such as the appropriate use of medications (5). It has recently been suggested that the use of proton pump inhibitors (PPI) could favor the development of cognitive impairment (6). These drugs have shown a clear benefit in the pathologies for which they are indicated; but they are often prescribed inappropriately (7,8).
Some have suggested that this association is due to an alteration in vitamin B12 absorption, secondary to atrophy of the gastric mucosa, which in turn is produced by hypochlorhydria, acidification of the lysosomes of the microglia. In addition, it has been found that there may be an alteration in beta- and gamma-secretases, enzymes known to be involved in Alzheimer’s disease (9,10).
Limited data are available in Latin America on this subject. Therefore, the primary objective of this study is to describe the link between cognitive impairment and the use of PPIs in the older adult population of Bogotá, Colombia.
Material and methods
We analyzed data from the SABE (Spanish acronym for Health, Well-Being and Aging) study. This cross-sectional study was conducted in 2012 in Bogotá, and included 2,000 people aged 60 years or older (81.9% of the eligible people who finally agreed to participate in the study). We used a probabilistic sampling by conglomerates which is statistically representative of the city’s population of 779,539 subjects aged 60 years or older. This instrument was derived from the international tool SABE, previously applied in other studies, modified and adapted to the Colombian context (11,12,13).
The SABE Bogotá study included 11 main topics, ranging from sociodemographic aspects, living conditions, poverty and violence, to health status, including cognitive status, anthropometric measurements, functional assessment, disabilities and access to health services.
The teams of interviewers were trained by the lead investigators, thematic researchers, statistician and field coordinator. The results were collected on paper, and then two programmers in Excel for Windows transferred them to a separate database.
All the people signed an informed consent in order to participate in the study. This study was approved by the Ethics Committee of the Pontificia Universidad Javeriana, Bogotá, Colombia.
Variables
Dependent variable
The dependent variable
of interest was alteration in the cognitive tests, determined according to the score
obtained in the Modified Mini Mental State Examination (MMSE-M), an instrument validated
in Spanish and widely used in this study; this questionnaire has a minimum score
of 0 and a maximum of 19. The cutoff point is 13 (0-12 “deterioration” and 13-19
“without deterioration”) (14). It includes: Orientation (4 points), Registration
of 3 words (3 points), Attention and Calculation (5 points), Comprehension (3 points),
Recall (3 points), Drawing (1 point), with a sensitivity of 93,.8 and a specificity of 93.9 (15).
Independent variables
Older adults who scored more than or equal to 13 in the MMSE-M were asked verbally about PPI use and duration of use (months); otherwise, this information was requested from the proxi. To minimize memory bias, they were asked to show the box or the packaging of the medication they were using at the time. The PPIs were omeprazole, lanzoprazole, pantoprazole and esomeprazole.
In addition, sociodemographic variables were included for adjustment, such as age, sex, marital status (dichotomized in married and single), and years of schooling; comorbidities were also included, such as diabetes, chronic obstructive pulmonary disease, hypertension, cardiovascular disease, cerebrovascular accident, arthropathies and depression.
Statistical analysis
Univariate analysis was used to explore the extreme values and the normal distribution to adjust and categorize variables. The categorical variables are expressed as frequencies and percentages, while for the continuous variables the means and standard deviations were used. The association between the dependent variable and the independent variables was analyzed; chi-square tests were used for categorical variables and T-tests for continuous variables. Based on the ROC curve, better sensitivity and specificity figures were found, time of PPI use greater than or equal to 24 months was selected, and it was dichotomized again. We performed a multivariate logistic regression model, in which the outcome variable was cognitive impairment, and the independent variable was unadjusted PPI use, and then adjusted for sex, age, marital status and years of schooling, to obtain odds ratio (OR) with 95% confidence intervals. A variable of interaction was used between the age and the time of use of the drug, given that said variable (age) is affecting both the outcome and the independent variable of interest. The level of statistical significance was established at p < 0.05. The data was analyzed with Stata Version 14 for iOS.
Results
A total of 2,000 older adults were evaluated. The average age was 71.17 ± 8.05 years, 63.4% were women, 35.75% were married, the average number of years of schooling was 5.52 ± 4.58. The prevalence of PPI use was 20.7%, with an average duration of use of 74.8 ± 93.76 months. The MMSE-M was altered in 12.6% of the older adults (Table 1).
Table 1
Description of the sample and
bivariate analysis
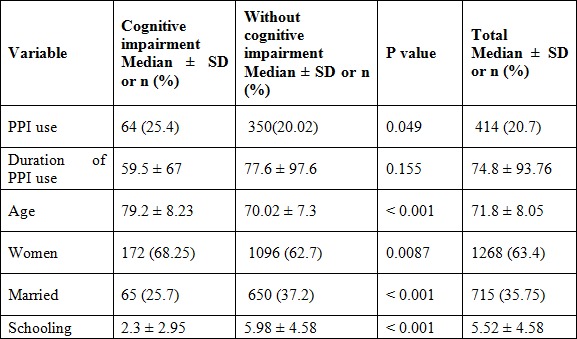
SD: standard deviation.
In the bivariate analysis, statistically significant associations were documented among older people with cognitive impairment and older age, female sex, being unmarried, a low schooling level and use of PPIs, all with p less than 0.05 (Table 1).
In the multivariate analysis, PPI use for 24 or more months, adjusting for the variables of age, sex, level of schooling and marital status, showed a 1.90 times increase in the risk of association (OR: 1.90; CI: 1.11-3.24; p = 0.018) (Table 2).
Table 2
Multivariate analysis
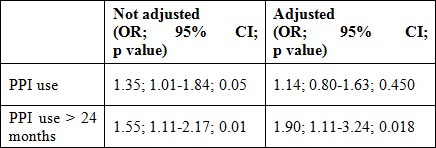
Adjusted for age, sex, marital status, schooling and comorbidities
CI: confidence interval.
Discussion
This study shows a significant association of increased risk between using PPIs for 24 or more months and developing cognitive impairment.
There is a high prevalence of cognitive impairments in Latin America (16,17). Therefore, it is very important that health systems focus on their prevention, with the control of risk factors as a pillar (18,19).
Studies have found the biological feasibility of the association between PPI use and cognitive impairment in murine models. This may have implications for human beings, as has been observed in developed countries where research has been conducted on PPIs and their positive association with cognitive impairment, as shown in this study in the Latin American context, where information on the subject is limited (6,9).
Initial evidence shows a significant increase in the occurrence of cognitive impairment in PPI users (6,20). However, in contrast to previous research, a recent longitudinal study conducted in the United States found no association between the use of PPI and cognitive impairment. This is probably due to methodological differences between the studies (21).
There are divergent and not entirely conclusive concepts on this hypothesis; in addition, there is a high degree of heterogeneity among these studies, due to the differences in their methodological designs.
This study has some limitations. First, as it was a cross-sectional study, it was not possible to determine the causality of the associations. Second, the dependent variable is self-reported, which can lead to memory bias, and because of the cross-sectional characteristics of the survey it was not possible to establish the previous MMS-E score, as well as the non-discrimination of the cognitive impairment severity, which was assessed by a scale and not by a specialized medical examination. On the other hand, this study has important strengths. It is noteworthy that it shows an association of a hypothesis with limited information in the subject area; another strength is that this is the first epidemiological study in older people in Bogotá that measures the association between PPI use and cognitive impairment.
This study demonstrated a positive association between cognitive impairment and PPI use. This leads to the formulation of new longitudinal studies to obtain more scientific information to establish causality and thus create public health policies to reduce the incidence of neurodegenerative disorders.
Funding
This project was
funded by the Administrative Department of Science, Technology and Innovation, Colciencias, code 120354531692, and by the Pontificia Universidad Javeriana.
References
1. Cesari M, Marzetti E, Thiem U, Perez-Zepeda MU, Abellan Van Kan G, Landi F, et al. The geriatric management of frailty as paradigm of “The end of the disease era”. Eur J Intern Med. 2016;31:11-4.
2. World Health Organization. The top 10 causes of death 2017 [internet]. Avalaible at: http://www.who.int/mediacentre/factsheets/fs310/en/
3. Beerens HC, Zwakhalen SM, Verbeek H, Ruwaard D, Hamers JP. Factors associated with quality of life of people with dementia in long-term care facilities: a systematic review. Int J Nurs Stud. 2013;50(9):1259-70. doi: https://doi.org/10.1016/j.ijnurstu.2013.02.005.
4. Livingston G, Sommerlad A, Orgeta V, Costafreda SG, Huntley J, Ames D, et al. Dementia prevention, intervention, and care. Lancet. 2017;390(10113):2673-2734. doi: https://doi.org/10.1016/S0140-6736(17)31363-6.
5. Delgado Silveira E, Montero Errasquín B, Muñoz García M, Vélez-Díaz-Pallares M, Lozano Montoya I, Sánchez-Castellano C, et al. [Improving drug prescribing in the elderly: a new edition of STOPP/START criteria]. Rev Esp Geriatr Gerontol. 2015;50(2):89-96.
6. Wijarnpreecha K, Thongprayoon C, Panjawatanan P, Ungprasert P. Proton pump inhibitors and risk of dementia. Ann Transl Med. 2016;4(12):240.
7. Mossner J. The indications, applications, and risks of proton pump inhibitors. Dtsch Arztebl Int. 2016;113(27-28):477-83. doi: https://doi.org/10.3238/arztebl.2016.0477.
8. Moriarty F, Bennett K, Cahir C, Fahey T. Characterizing potentially inappropriate prescribing of proton pump inhibitors in older people in primary care in ireland from 1997 to 2012. J Am Geriatr Soc. 2016;64(12):e291-e6.
9. Badiola N, Alcalde V, Pujol A, Munter LM, Multhaup G, Lleo A, et al. The proton-pump inhibitor lansoprazole enhances amyloid beta production. PloS one. 2013;8(3):e58837.
10. Majumdar A, Cruz D, Asamoah N, Buxbaum A, Sohar I, Lobel P, et al. Activation of microglia acidifies lysosomes and leads to degradation of Alzheimer amyloid fibrils. Mol Biol Cell. 2007;18(4):1490-6.
11. Peláez M, Palloni A, Albala C, Alfonso JC, Ham-Chande R, Hennis A, et al. SABE - Survey on Health, Well-Being, and Aging in Latin America and the Caribbean, 2000. Inter-university Consortium for Political and Social Research (ICPSR) [distributor]; 2005.
12. Cano-Gutiérrez C, Bordaz MG, Reyes-Ortiz C, Arciniegas AJ, Samper-Ternent R . Evaluación de factores asociados al estado funcional en ancianos de 60 años o más en Bogotá, Colombia. Biomédica. 2017;37(supl 1). doi: http://dx.doi.org/10.7705/biomedica.v37i1.3197.
13. Cano-Gutiérrez C, Samper-Ternent R, Cabrera J, Rosselli D. [Medication use among older adults in Bogota, Colombia]. Rev Peru Med Exp Salud Publica. 2016;33(3):419-24. doi: https://doi.org/10.17843/rpmesp.2016.333.2292.
14. Albala C, Lebrao ML, León Díaz EM, Ham-Chande R, Hennis AJ, Palloni A, et al. [The Health, Well-Being, and Aging ("SABE") survey: methodology applied and profile of the study population]. Rev Panam Salud Publica. 2005;17(5-6):307-22.
15. Icaza M, Albala C. Minimental State Examinations (MMSE) del estudio de demencia en Chile: Analisis Estadístico. Washington, D.C; 1999.
16. Rodríguez L, Juan de J. Demencia: prevalencia, factores de riesgo, impacto y prevención, el estudio 10/66. Inf Psiquiátr. 2015;219:9-20.
17. Gutiérrez-Robledo LM, Arrieta-Cruz I. [Dementia in Mexico: The need for a National Alzheimer s Plan]. Gaceta Médica de Mexico. 2015;151(5):667-73.
18. Baumgart M, Snyder HM, Carrillo MC, Fazio S, Kim H, Johns H. Summary of the evidence on modifiable risk factors for cognitive decline and dementia: A population-based perspective. Alzheimer's & Dementia. 2015;11(6):718-26.
19. Lovden M, Xu W, Wang HX. Lifestyle change and the prevention of cognitive decline and dementia: what is the evidence? Curr Opin Psychiatry. 2013;26(3):239-43. doi: https://doi.org/10.1097/YCO.0b013e32835f4135.
20. Gomm W, von Holt K, Thome F, Broich K, Maier W, Fink A, et al. Association of proton pump inhibitors with risk of dementia: a pharmacoepidemiological claims data analysis. JAMA Neurol. 2016;73(4):410-6.
21. Goldstein FC, Steenland K, Zhao L, Wharton W, Levey AI, Hajjar I. Proton pump inhibitors and risk of mild cognitive impairment and dementia. J Am Geriatr Soc. 2017;65(9):1969-74.
Author notes
a
Director of Internal Medicine and Geriatrics, Hospital Cardiovascular del Niño, Soacha, Cundinamarca,
Colombia
b
Geriatric
Epidemiology Research Department, National Institute of Geriatrics, Mexico City,
Mexico.
Faculty of Health Sciences, School of Medicine, Universidad Anáhuac del Norte, Mexico City, Mexico.
c
Geriatric
Epidemiology Research Department, National Institute of Geriatrics, Mexico City,
Mexico.
Faculty of Health Sciences, School of Medicine, Universidad Anáhuac del Norte, Mexico City, Mexico.
d
Geriatric
Epidemiology Research Department, National Institute of Geriatrics, Mexico City,
Mexico.
e
Director
of the Aging Institute, School of Medicine, Pontificia
Universidad Javeriana, Bogotá, Colombia.
ulises.perez@salud.gob.mx
Additional information
How to cite: Gómez C, Borda Borda MG, Pérez MU, Tella-Vega P, Cano-Gutiérrez CA. Association
between the Use of Proton Pump Inhibitors and Cognitive Impairment in Older Adults. Univ
Med. 2019;60(1). doi: http://dx.doi.org/10.11144/Javeriana.umed60-1.inhi