Introduction
Laparoscopic surgery has revolutionized the surgical management of patients with various pathologies. This has created the need for training in the area and a change in general surgery training programs (1,2) through technology, simulation equipment in organic, inorganic or virtual models (3,4). The American Board of Surgery and the Accreditation Council for Continuing Medical Education consider this training a priority. For this reason, they have developed the course Fundamentals of Laparoscopic Surgery as a requirement to approve the residency course. Although it is possible to evaluate the performance using simulators, training in laparoscopic surgery in a university hospital must be accompanied by quality control (5) in which the measurement and quantification of demographic and clinical outcomes data undergo descriptive evaluation so that ideas emerge on the best way to develop and teach these competences (6,7).
Laparoscopic appendectomy (LA) and laparoscopic cholecystectomy (LC) are the most performed general surgical procedures in the world (8,9), and are performed early in the surgery resident’s training. These procedures offer an opportunity to master necessary skills before performing more complex procedures (10,11).
The aim of this study is to describe the evolution in the surgical experience of a group of general surgery residents, and the LA and LC morbidity and mortality trend at the Hospital Universitario San Ignacio during the period between January 2008 and December 2014. We expect that these results guide the training process of general surgery residents at university hospitals.
Materials and methods
An observational analytical retrospective cohort study was conducted in which we reviewed medical records taken from the institutional database. 3146 LCs and 1045 LAs carried out between January 1, 2008 and December 31, 2014 were included. In the case of LCs, elective and emergency procedures were evaluated. A total of 52 residents were analyzed, 10 of whom were fully followed up on their learning curve throughout their training time, and 6 withdrew before finishing their training.
The following demographic variables were analyzed: age, American Society of Anesthesiologists (ASA) anesthetic risk classification, severity grading according to the 2013 Tokyo Guidelines (12), and pathology report. The recorded outcomes were: operative time (minutes), hospital stay (days), and intraoperative complications: hollow viscus injury, conversion to open surgery, bile duct injury (according to Strasberg classification) (13) and bleeding (greater than 500 cm3). The postoperative complications evaluated (at 30 days) were: unplanned reoperation, surgical site infection (SSI), bleeding and mortality.
We excluded records with incomplete data, surgeries in which an additional surgery was performed, and procedures performed by instructors. It is necessary to make it clear that all surgeries performed at the hospital are performed under in-person supervision in the operating room.
Surgical
technique and follow-up
The abdominal cavity was accessed by 10 mm umbilical incision using the Hasson technique, pneumoperitoneum insufflation and diagnostic laparoscopy. In LAs, 5 mm and 10 mm trocars were placed under direct vision in the suprapubic region and in the left iliac fossa. The mesentery and the appendicular artery were managed with different types of energy: LigaSure™ (ValleyLab, Inc., Boulder, Colorado), HARMONIC ACE®+ Shears (Ethicon Endo-Surgery, Cincinnati, OH) or monopolar electrocautery, according to the treating surgeon’s criteria and the degree of inflammation of the tissues. Once the base was fully identified, it was ligated with Hem-O-Lok® (Weck Closure Systems, Research Triangle Park, Durham, NC, USA). To retrieve the surgical piece, a bag was used when the appendix was in gangrenous phase or with peritonitis, and in the latter case, the cavity was irrigated with saline and dried exhaustively.
For LCs, a 10 mm trocar was placed in the epigastrium and two 5 mm trocars in the right upper quadrant. The structures of the hepatocystic triangle were dissected and Strasberg’s safety vision was obtained (14). The cystic artery and the cystic duct were clipped with metal clips and cut with scissors. In case of thick cystic duct, Hem-O-Lok was used. The gallbladder was dissected from the liver bed with monopolar electrocautery, in order to retrieve it through the epigastric port. Both for LAs and LCs, the patients were discharged after controlling the pain, when there was no systemic inflammatory response and the oral route was well tolerated.
Statistical
analysis
Quantitative variables were analyzed with central tendency and dispersion measures, and qualitative variables with relative frequencies (percentages) and proportions. The Microsoft Excel 2016TM program was used to organize the variables and calculate proportions and percentages. The Stata version 8.0 program (Statacorp, College Station, TX) was used for the univariate and multivariate analysis, and nonparametric hypothesis tests were performed to compare the independent groups (Mann-Whitney U and Kruskall-Wallis) with p values <0.05.
Ethical
aspects
This is an analytical observational study and therefore no intervention was carried out with the participants; it is rated as a “no risk” study, according to Resolution 008430 of 1993 of the Ministry of Health of Colombia. The criterion of respect for the autonomy and dignity of the subjects included in the study prevailed throughout the study, as well as that of protection of their rights, information and welfare.
Since this is a review of medical records of a university hospital, it was required that it be submitted to the research committee of the Surgery Department, and that it be approved by the Hospital Research Committee. In the approval it was recorded that there is no direct intervention on the patient, which is why informed consent is not required. In addition, this study was conducted under the ethical standards of the latest official version of the Declaration of Helsinki.
Results
Laparoscopic appendectomy
Patient demographic data are shown
in Table 1. The majority of patients were women, were classified
as ASA I, and the most common pathology was acute edematous/fibrinopurulent
appendicitis. The mean hospital stay was 1.66 days (SD: 1.91). There was a sustained
growth in the number of procedures, globally and per year of residency training;
the number of LAs increased from 12 in 2008 to 456 in 2014.
Table 1
Demographic and clinical data
of the analyzed population (n = 4191)
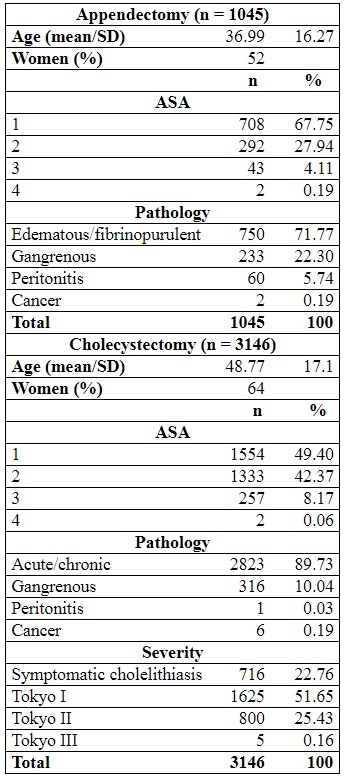
The mean operative time was 56.55 min with a SD of 25.63.
When evaluating the times per year of residency training, the
mean was 58.24 min (SD: 21.6) and a median of 55 for the first year; 61.1 minutes
(SD: 24.7) and a median of 55 for the second year; 53.84 minutes (SD: 26.2) and
a median of 50 for the third year, and 51.33 minutes (SD: 32.6) and a median of
45 for the fourth year. As shown in Figure 1, there was a decreasing trend
in the median and in the interquartile range in the data distribution, without being
statistically significant.
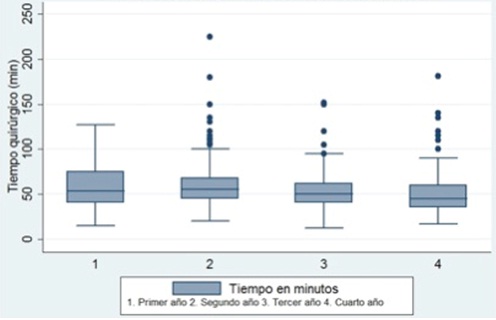 Figure 1
Surgical time for laparoscopic appendectomy
by residency level
Figure 1
Surgical time for laparoscopic appendectomy
by residency level
The mean operative
time according to the severity and the histopathological
report was 51.67, 66.77 and 76.80 min for edematous/fibrinopurulent
appendicitis, gangrenous appendicitis and peritonitis, respectively. When comparing
the operative times between edematous/fibrinopurulent
and gangrenous appendicitis, the difference was statistically significant, with
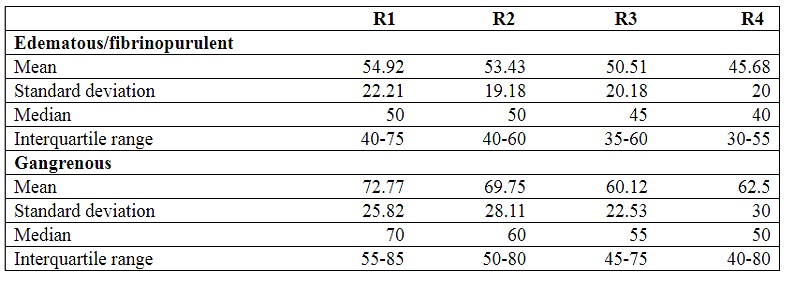
a p value > 0.05. An inverse relationship was documented
between the mean operative time according to the pathology and the year of residency
training, as shown in Table 2.
Table 2
Surgical time, in minutes, according to the pathology and year of residency training
Complications
There were 8 intraoperative complications (0.77%), 3 due to bleeding, and 5 related to hollow viscus injury, 4 (80%) of which were caused by third and fourth year residents. There were a total of 28 patients (2.68%) with conversion to open surgery. The main cause were technical difficulties in the management of the appendicular base (25 patients); 11 (44%) of these cases occurred with second year residents.
The most common postoperative complication was SSI, with 30 cases (2.87%), followed by adynamic ileus, with 25 cases (2.39%). Overall and within the course of time, the general behavior of intraoperative complications, conversions to open surgery, ileus, SSIs and readmissions decreased by year of residency training. A mortality of 0.57% was documented (n = 6).
Laparoscopic cholecystectom
Table 1 shows the demographic data. There was an increase in the annual number of LCs, with 370 in 2008 and 563 in 2014. This showed a greater exposure of residents to procedures in direct relation with time. This exposure was greater in the second year of residency training, with 1433 cholecystectomies performed, compared to 898 for third year residents, and 815 for fourth year residents. 77% of the LCs were performed in the context of acute cholecystitis, 67% of which were classified as Tokyo I. The mean hospital stay was 1.54 days (SD: 3.4).
The mean operative time was 69.87 min (SD: 30.78) with a median of 60 min, and 50-85 interquartile range. The surgical time decreased as the residency level advanced (Figure 2). When comparing the operating time per year of residency training, the mean times were 74.7, 66.9 and 64.5 min for second, third and fourth year residents, respectively. There was a statistically significant difference (p value <0.05) of the mean times in the Kruskall-Wallis test, and was higher in the LCs performed by second year residents.
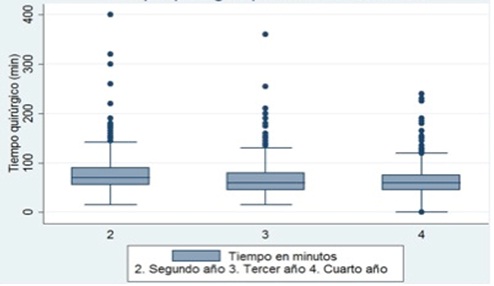 Figure 2
Surgical time for
laparoscopic cholecystectomy by level of residence
Figure 2
Surgical time for
laparoscopic cholecystectomy by level of residence
Likewise, when comparing between operative times of the second and third years, and between those of the third and fourth years, we found lower mean times as residents progressed in their residency training, with p values < 0.05.
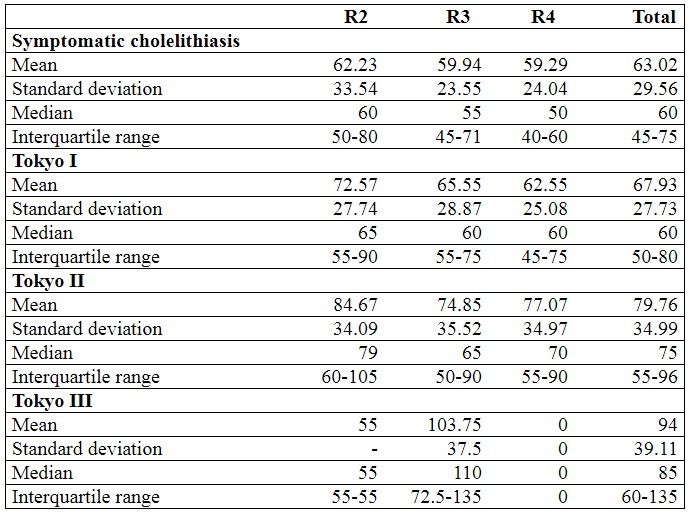
The evaluation of the mean operative time according to the clinical severity as per Tokyo classification showed that it increased as the severity increased (Table 3). In addition, when comparing the severity according to the histopathological report and the mean time, there was a statistically significant difference (p value < 0.05), with mean times in acute/chronic phase of 67.85 min (SD: 29.97), and 88.01 min (SD: 32.87) in gangrenous phase. These data show that, although the times were longer as the severity increased, they decreased when the surgeries were performed by more advanced year residents.
Table 3
Operative time, in minutes, according to the clinical
severity and level of residency training
Complications
There were a total of 61 (1.9%)
intraoperative complications, 30 of which (6.7%) corresponded to bleeding, 17 (3.8%)
to hollow viscus injury, and 14 (0.45%) to bile duct injury.
The majority were Strasberg type A (n = 8). There were a total
of 98 postoperative complications (3.1%), 29 of which (0.92%) corresponded
to reoperation, 13 (0.41%) to bleeding, 29 (0.92%) to SSI, and 43 (1.37%) to conversion
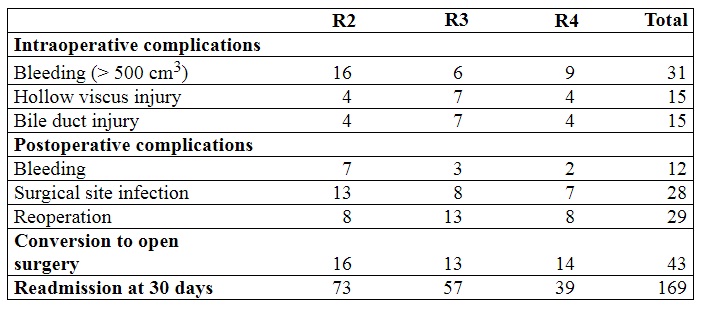
to open surgery. Table 4 shows the relationship between complications and the level
of residency training. The majority of complications occurred in patients operated
by second year residents.
Table 4
Complications of laparoscopic cholecystectomy per year of residency training
Eight deaths were documented (0.25%), 4 of which were related
to massive postoperative bleeding; 2 of these patients had a medical indication
for anticoagulation and received perioperative bridging therapy according to institutional
protocols.
Discussion
The results of this study show an overall increase in the number of LAs and LCs performed during the period studied, and that surgical times improve as residency training progresses. According to our hospital data, there was an increase in the proportion of LAs performed per year: from 0.72% in 2010, to 73% in 2014, and exposure to this procedure in earlier stages of residency training; as reported by like Carson et al. (15), where most of the procedures performed by general surgery residents between 1999 and 2008 were minimally invasive (3.7 to 11.2%, p = 0.00001). According to Chung and Ahmed (16), within 10 years the percentage of open surgeries will be reduced by 60%, except in cases of trauma. These data demonstrate the need for residency programs to provide adequate preparation in the laparoscopic approach, and possibly an increasingly early exposure to minimally invasive procedures (17,18).
In our study we can see that in the first years evaluated, there were few LCs and LAs, most of which were performed by third and fourth year residents, while in recent years there has been an increase in interventions performed by second year residents. In the case of LCs, this phenomenon was observed as of 2011, when approximately 50% of cholecystectomies were performed by second year residents. This indicates that in our department the learning curve takes place during this period. This increasingly early exposure within residency training had no statistically significant differences in morbidity and mortality outcomes; this may indicate that with adequate training and supervision, trainee surgeons can achieve a satisfactory level of competence in these procedures, without increasing the number of complications (19). Similarly, Jolley et al. (17) wrote about the participation of residents in basic laparoscopic procedures, LAs and LCs, which did not have significant differences in terms of mortality, morbidity or reoperation, although in both surgeries the presence of the resident was associated with longer operative times, which were 60 minutes or more for LAs (20). In our case, the mean time for LAs was 56 min, with differences between the levels of residency training, but without exceeding the mean time reported in the literature, and 69 min for LCs, which was shorter than the results reported in other international studies (6,8,10, 11,21,22,23).
There was a decreasing trend in the mean and median operative time, both for LA and LC, according to the year of residency training; this decrease was statistically significant, when compared according to the clinical severity and the histopathological report in LC. Kauvar et al. (24) obtained similar results, and reported a longer mean time in the first years of residency training and, like our data, show that the duration of LA and CL decreases during the 4 training years, as residents gradually advance in the learning curve (6,25,26). As raised by Garg et al. (27), our study showed a direct relationship between the severity of the clinical picture and the operative time, which was longer in the case of gangrenous appendicitis and Tokio III cholecystitis.
The context analyzed and the results show that a structured laparoscopic surgery training in basic procedures during residency in a university hospital improves the residents’ surgical skills (28,29). This through keeping a record of procedures performed, especially in academic programs, in which this process demonstrates that university hospitals meet the teaching objectives in the teaching of laparoscopic surgery, which is accompanied by a better control of the academic process quality.
A limitation of the present study is its retrospective nature, since there may be sub- or over-registration of the information. To document of the operative time, the anesthetic record was used, in which the time variable was recorded as an interval variable and not as a ratio interval. Furthermore, given the retrospective nature of the study, each resident was not taken into account individually, since the objective was to assess the training evolution according to the year of residency training, rather than the evolution of each individual resident, which would have required an analysis to control for confounding variables, such as previous laparoscopic training. However, we consider that, despite the descriptive nature of the study, the large number of cases allows identifying existing differences between each year of residency training.
Conclusion
We see that the number of laparoscopic procedures, specifically
LAs and LCs, has increased over time, which has involved greater efforts to teach
basic and complex laparoscopic skills in the general surgery residency program.
These should focus mainly on the first two training years, when there is a greater
exposure, with a decrease in the operative time that will occur progressively as
more experience is acquired during the first residency
years, and during the learning curve, in which the complexity of these procedures
will increase. All this process will require a system to record and provide feedback
on the processes carried out in a learning-healthcare context that allows keeping
morbidity and mortality within the expected margins for a given procedure, within
what is reported worldwide.
References
1. Nácul MP, Cavazzola LT, Melo MC De. Current status of residency training in laparoscopic. ABCD Arq Bras Cir Dig (São Paulo). 2015;28(1):81-5.
2. McCoy AC, Gasevic E, Szlabick RE, Sahmoun AE, Sticca RP. Are open abdominal procedures a thing of the past?: An analysis of graduating general surgery residents’ case logs from 2000 to 2011. J Surg Educ. 2013;70(6):683-9. https://dx.doi.org/10.1016/j.jsurg.2013.09.002
3. Shetty S, Zevin B, Grantcharov TP, Roberts KE, Duffy AJ. Perceptions, training experiences, and preferences of surgical residents toward laparoscopic simulation training: A resident survey. J Surg Educ. 2014;71(5):727-33. https://dx.doi.org/10.1016/j.jsurg.2014.01.006
4. Henao O, Escallón J, Green J, Farcas M, Sierra JM, Sánchez W, et al. Fundamentos de cirugía laparoscópica en Colombia empleando telesimulación: una herramienta adicional para la formació integral de cirujanos. Biomédica. 2013;33(1):1-24.
5. Priego JP, Lobo ME, Rodríguez VG, Cabañas MJ, Peromingo FR, Fresnada MV. ¿Es adecuada la formación del residente en cirugía laparóscopica? Rev Chil Cirugía. 2008;60:418-23.
6. Fahrner R, Turina M, Neuhaus V, Schöb O. Laparoscopic cholecystectomy as a teaching operation: Comparison of outcome between residents and attending surgeons in 1,747 patients. Langenbeck’s Arch Surg. 2012;397(1):103-10. https://doi.org/10.1007/s00423-011-0863-y
7. Lekawa M, Shapiro SJ, Gordon LA, Rothbart J, Hiatt JR. The laparoscopic learning curve. Surg Laparosc Endosc [Internet]. 1995 Dec [cited 2016 May 30];5(6):455-8. Available at: https://www.ncbi.nlm.nih.gov/pubmed/8611992
8. Shabtai M, Rosin D, Zmora O, Munz Y, Scarlat A, Shabtai EL, et al. The impact of a resident’s seniority on operative time and length of hospital stay for laparoscopic appendectomy: Outcomes used to measure the resident's laparcoscopic skills. Surg Endosc Other Interv Tech. 2004;18(9):1328-30.
9. Watanabe Y, Bilgic E, Lebedeva E, McKendy KM, Feldman LS, Fried GM, et al. A systematic review of performance assessment tools for laparoscopic cholecystectomy. Surg Endosc [Internet]. 2016;30(3):832-44. Available at: https://www.ncbi.nlm.nih.gov/pubmed/26092014
10. Harrison VL, Dolan JP, Pham TH, Diggs BS, Greenstein AJ, Sheppard BC, et al. Bile duct injury after laparoscopic cholecystectomy in hospitals with and without surgical residency programs: Is there a difference? Surg Endosc Other Interv Tech. 2011;25(6):1969-74.
11. Koulas SG, Tsimoyiannis J, Koutsourelakis I, Zikos N, Pappas-Gogos G, Siakas P, et al. Laparoscopic cholecystectomy performed by surgical trainees. JSLS [Internet]. 2006;10(4):484-7. Available at: https://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3015736&tool=pmcentrez&rendertype=abstract
12. Takada T, Strasberg SM, Solomkin JS, Pitt HA, Gomi H, Yoshida M, et al. TG13: Updated Tokyo GUIDELINES for the management of acute cholangitis and cholecystitis. J Hepatobiliary Pancreat Sci [Internet]. 2013 Jan [cited 2016 May 30];20(1):1-7. Available at: https://www.ncbi.nlm.nih.gov/pubmed/23307006
13. Mercado MA, Domínguez I. Classification and management of bile duct injuries. World J Gastrointest Surg [Internet]. 2011;3(4):43-8. Available at: https://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3083499&tool=pmcentrez&rendertype=abstract
14. Strasberg SM, Brunt LM. Rationale and use of the critical view of safety in laparoscopic cholecystectomy. J Am Coll Surg. 2010;211(1):132-8. https://dx.doi.org/10.1016/j.jamcollsurg.2010.02.053
15. Carson JS, Smith L, Are M, Edney J, Azarow K, Mercer DW, et al. National trends in minimally invasive and open operative experience of graduating general surgery residents: Implications for surgical skills curricula development? Am J Surg. 2011;202(6):720-6. https://dx.doi.org/10.1016/j.amjsurg.2011.06.045
16. Chung RS, Ahmed N. The impact of minimally invasive surgery on residents’ open operative experience: analysis of two decades of national data. Ann Surg [Internet]. 2010 Feb [citado 2016 May 8];251(2):205-12. Available at: https://www.ncbi.nlm.nih.gov/pubmed/19858698
17. Jolley J, Lomelin D, Simorov A, Tadaki C, Oleynikov D. Resident involvement in laparoscopic procedures does not worsen clinical outcomes but may increase operative times and length of hospital stay. Surg Endosc Other Interv Tech. 2015;1-9. https://dx.doi.org/10.1007/s00464-015-4674-z
18. Rattner DW, Apelgren KN, Eubanks WS. The need for training opportunities in advanced laparoscopic surgery. Surg Endosc [Internet]. 2001 Oct [citado 2016 May 31];15(10):1066-70. Available at: https://www.ncbi.nlm.nih.gov/pubmed/11727071
19. Pariani D, Fontana S, Zetti G, Cortese F. Laparoscopic cholecystectomy performed by residents: a retrospective study on 569 patients. Surg Res Pract [Internet]. 2014;2014:912143. Available at: https://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=4208583&tool=pmcentrez&rendertype=abstract
20. Lin YY, Shabbir A, So JBY. Laparoscopic appendectomy by residents: Evaluating outcomes and learning curve. Surg Endosc Other Interv Tech. 2010;24(1):125-30.
21. Advani V, Ahad S, Gonczy C, Markwell S, Hassan I. Does resident involvement effect surgical times and complication rates during laparoscopic appendectomy for uncomplicated appendicitis? An analysis of 16,849 cases from the ACS-NSQIP. Am J Surg. 2012;203(3):347-52. https://dx.doi.org/10.1016/j.amjsurg.2011.08.015
22. Gifford E, Kim DY, Nguyen A, Kaji AH, Nguyen V, Plurad DS, et al. The effect of residents as teaching assistants on operative time in laparoscopic cholecystectomy. Am J Surg. 2016;211(1):288-93. https://dx.doi.org/10.1016/j.amjsurg.2015.06.019
23. Schwartz SI, Yaghoubian AT, Andacheh ID, Green SH, Falor AE, Kaji AH, et al. Senior residents as teaching assistants during laparoscopic cholecystectomy in the 80-hour workweek era: Effect on biliary injury and overall complication rates. J Surg Educ. 2013;70(6):796-9. https://dx.doi.org/10.1016/j.jsurg.2013.09.011
24. Kauvar DS, Braswell A, Brown BD, Harnisch M. Influence of resident and attending surgeon seniority on operative performance in laparoscopic cholecystectomy. J Surg Res [Internet]. 2006 May 15 [citado 2016 May 31];132(2):159-63. Available at: https://www.ncbi.nlm.nih.gov/pubmed/16412471
25. Böckler D, Geoghegan J, Klein M, Weissmann Q, Turan M, Meyer L, et al. Implications of laparoscopic cholecystectomy for surgical residency training. JSLS [Internet]. Jan [citado 2016 May 31];3(1):19-22. Available at: https://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3015346&tool=pmcentrez&rendertype=abstract
26. Lim SH, Salleh I, Poh BK, Tay KH. Laparoscopic cholecystectomy: an audit of our training programme. ANZ J Surg [Internet]. 2005 May [citado 2016 May 31];75(4):231-3. Available at: https://www.ncbi.nlm.nih.gov/pubmed/15839972
27. Garg CP, Vaidya BB, Chengalath MM. Efficacy of laparoscopy in complicated appendicitis. Int J Surg [Internet]. 2009 Jul [citado 2016 May 31];7(3):250-2. Available at: https://europepmc.org/abstract/med/19393776
28. Lucena Olavarrieta JR, Coronel P. Formación del cirujano en técnicas quirúrgicas laparoscópicas. Rev la Fac Med [Internet]. [citado 2016 May 31];29(2):97-102. Available at: https://www.scielo.org.ve/scielo.php?script=sci_arttext&pid=S0798-04692006000200001&lng=es&nrm=iso&tlng=es
29. Long KL, Spears C, Kenady DE, Scott Roth J. Implementation of a low-cost laparoscopic skills curriculum in a third-world setting. J Surg Educ. 2014;71(6):860-4. https://dx.doi.org/10.1016/j.jsurg.2014.05.004
Author notes:
a Correspondence: cuevas-l@javeriana.edu.co
Additional information
How to cite: Cuevas López L, Cortés Murgueitio N Díaz Castrillón CE,
Pinzón F, Molina GR. Experience
and learning curve of laparoscopic appendectomy and cholecystectomy of general surgery
residents in a Latin American hospital. Univ Med. 2019;60(2). https://doi.org/10.11144/Javeriana.umed60-2.curv