Introduction
Perinatal asphyxia is one of the leading causes of mortality in children under the age of five years (1,2). It is estimated that for each patient who dies due to perinatal asphyxia there are 10 survivors with serious sequelae (3). In the Bogotá Capital District, for 2014, perinatal asphyxia represented 6.4% of early neonatal mortality (4). Hypoxic-ischemic encephalopathy (HIE) is the set of alterations in the central nervous system of the newborn, caused by oxygen deprivation and the subsequent ischemia. This clinical picture was originally described and classified by Sarnat and Sarnat (5,6).
Since 2010, the American Heart Association and the International Liaison Committee on Resuscitation have recommended that all newborns older than 36 weeks of gestational age with moderate-to-severe HIE should be offered the possibility of therapeutic hypothermia within the post-resucitation care. This recommendation was endorsed in the Clinical practice guide for newborns with perinatal asphyxia, published in April 2013 by the Ministry of Health and Social Protection of Colombia (7,8).
Current findings have shown that the use of therapeutic hypothermia within the first six hours after the asphyxia event reduces statistically and clinically the combined result of mortality or disability longer than 18 months, without increasing the risk of disability among survivors and with positive effects that remain until childhood (9,10).
The program of Selective Hypothermia with Cool-Cap (helmet) in the Neonatal Intensive Care Unit of Hospital Universitario San Ignacio offers this therapeutic option to newborns with HIE. The present article describes the experience of the treating team with a group of neonates treated at the hospital. This contributes to the knowledge of this area of newborn care, by presenting clinical outcomes of interest in the context of a tertiary hospital in Colombia.
In Colombia, a cohort of patients treated with total body therapeutic hypothermia during 2017 has already been described (11). The study aimed to describe the results obtained with the other method of selective hypothermia: blanket.
Methods
Observational, sequential cross-sectional study. Patients’ data include an observation from June 2015 to March 2017. The sample size was based on the census and included all patients referred to the program during the observation period with asphyxia criteria, defined by the American Academy of Pediatrics and the American College of Gynecology and Obstetrics as metabolic or mixed acidosis (pH < 7.0 in a sample of cord blood at birth), 5-minute Apgar score < 3, neurological involvement (seizures, coma and hypotonia) and involvement of multiple organs (heart, lung, liver, kidney and intestines) (6).
Selective cerebral hypothermia therapy with Cool-Cap is used to treat newborns with moderate to severe HIE, in order to selectively cool the head with moderate systemic hypothermia (34-35 ºC), reduce mortality and prevent or reduce the severity of neurologic injury associated with HIE. Patients remain in intensive care with continuous monitoring of vital signs and brain activity by means of an extended electroencephalogram. The therapy lasts 72 hours, and then reheating is carried out at 0.5 ºC per hour until reaching physiological temperatures (36.5-37.5 ºC).
The variables studied were defined according to what is reported in the literature (5,12) and to the care protocol of the newborn unit. The variables were collected directly from the patients’ medical records, tabulated in an Excel® 2010 spreadsheet, and exported to the Stata 14 software for analysis. The presence of encephalopathy at discharge and death were considered outcome variables. The graphs were generated with GraphPad 7.04.
Continuous variables were compared using the Student’s T test. Relative frequencies were analyzed and compared according to variants of clinical interest using chi square. The prevalence ratio and their 95% confidence intervals (95% CI) were also calculated for the encephalopathy and death outcomes according to the clinical variables of interest. An α = 0.05 (significant p <0.05) was considered for all the statistical data used. For categorical variables such as Apgar, 3 groups were established: 0-5, 6-7 and 8-10, and were compared using Kruskal-Wallis.
Variables were defined as follows: severe arrhythmia (different from sinus bradycardia or bigeminy), severe hypotension (when, despite volume administration, dopamine was required at more than 20 μg/kg/minute) and venous thrombosis (vessel thrombosis not related to venous access lines). For the other variables defined as postnatal complications we took a time of 7 days of life, and we considered:
-
Mild
hypotension: average blood pressure < 40 mm Hg.
-
Coagulopathy:
clinical bleeding or alteration of clotting times.
-
Renal failure:
urinary output < 0.5 ml/kg/hour for more than 24 hours or increase in creatinine higher than 009 mmol/L.
-
Hyponatremia: seric sodium < 135 mmol/L.
-
Hypokalemia: seric potassium < 3.5 mmol/L.
-
Thrombocytopenia:
platelets < 150,000 per uL.
-
Elevation of
liver enzymes: AST > 200 IU/L and ALT > 100 IU/L.
-
Metabolic
acidosis after starting the protocol: pH < 7.34 or base deficit ≥ 4 mmol/L.
-
Respiratory
difficulty: need for mechanical ventilation or continuous positive airway
pressure (CPAP).
-
Systemic
infection: positive cultures in blood, cerebrospinal fluid or urine taken after
starting therapy.
-
Hemoconcentration: increase in
hematocrit > 20%.
-
Hypoglycemia: glycemia < 47m/dL.
-
Hypocalcemia: calcium < 8
mmol/L.
-
Difficulty
maintaining the target temperature: less than 33.5 ºC or more than 37.5 ºC for
more than one hour.
Ethical aspects
All data is reported in an
aggregated and anonymous manner. The database is kept in the computers of the
researchers with unique usernames and passwords and under the security
parameters of the Pontificia Universidad Javeriana. The study protocol was reviewed and approved by
the School of Medicine and Hospital Universitario San
Ignacio Research Ethics Committee.
Results
41 patients were treated in the program during the observation period. The protocol admission
criteria were: newborns ≥ 36 weeks gestational age and body weight ≥ 1800 grams
who had moderate or severe encephalopathy defined by A
and B criteria, indicated as:
-
Criteria A: One
or more of the following findings: 10-minute Apgar score ≤5, continuous
resuscitation including endotracheal intubation or mask 10 minutes after birth,
umbilical cord blood pH < 7.0 in the first hour of life , excess base ≥ -16 in umbilical cord gases or in any blood sample in
the first 60 minutes of life.
-
Criteria B:
Altered state of consciousness (lethargy, stupor or coma), and at least one of
the following: hypotonia, abnormal reflexes or
pupillary abnormalities, weak or absent sucking reflex, clinical seizures.
If the patient met criteria
A and B, an amplitude electroencephalogram was performed. Patients with
imperforate anus and major congenital abnormalities were excluded. A patient
with panhypopituitarism undiagnosed at birth was
included.
Table 1 describes the
general characteristics of the subjects when entering the program. 14% of the
cases were between 36 and 37 weeks gestational age (GE), 82% of the cases were
between 38 and 40 weeks GE, there was only one case with 41 weeks. The most
frequent gestational age was 39 weeks (41.5%). The most frequent type of
delivery was natural birth (51.2%). Regarding the electroencephalographic (EEG)
activity before the intervention, 61% of the cases suffered from abnormal
activity of moderate type and 17% had abnormal EEG activity of severe type.
Table 1
General characteristics of the patients served by the
program
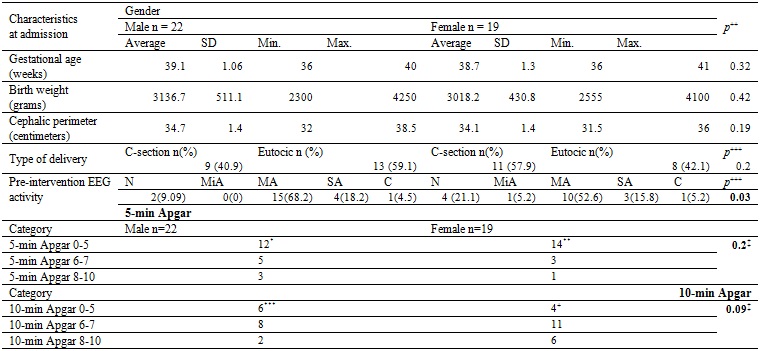
The main characteristics
defining the delivery are presented discriminated by sex. No significant
differences were found in the proportion of cases by sex related to gestational
age, birth weight, cephalic perimeter, Apgar, or type of delivery. Abnormal
electroencephalographic activity of moderate type predominated and was present
in 61% of cases. *Based on 20 observations. **Based on 18 observations ***Based
on 19 observations +Based on 17 observations. SD: Standard
deviation. N: normal. MiA: mild abnormal. MA:
moderate abnormal. SA: severe abnormal. C: convulsive. +Mean
differences with equal variances. +++Difference of proportions. ‡Kruskal-Wallis.
The treatment was performed
for 72 hours. Table 2 shows the main postnatal complications. Clinical seizures
were evident in 65% of the subjects, and respiratory difficulty in 48% of the
subjects. The most frequent electrolyte disorders were hyponatremia,
in 56% of cases; hypokalemia, in 31%, and hypocalcemia,
in 26% of patients. 29% of the patients presented pulmonary hypertension, and
26% presented clotting disorders. Bradycardia is
commonly observed during therapy, without hemodynamic repercussion. There were
no cases of venous thrombosis or hemoconcentration.
Table 2
Adverse events during therapy
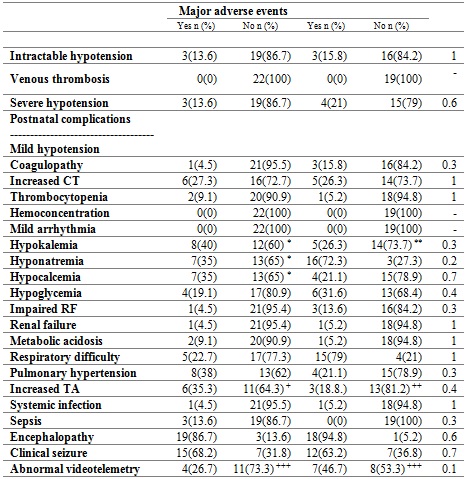
Proportion
of patients by type of complication. CT: clotting time. RF: renal function. TA: Transaminases. *Percentage
out of a total of 20 patients. **Percentages based on a total of 18 patients. +Percentages
based on 17 patients. ++Percentages based on 16 patients. +++Abnormal/Normal.
Percentages based on 15 patients. ‡Fisher’s exact test.
The main clinical outcome at
discharge was encephalopathy (90%), determined on the basis of three criteria: videotelemetry, brain magnetic resonance taken at 3 and 5
days, respectively, after the end of therapy, and clinical examination
performed by pediatric neurology before discharge. Some degree of
encephalopathy was considered if there was abnormality in one or more criteria.
In our study, follow-up was carried out from admission to therapy until
discharge. Of all patients, 63.3% had abnormal videotelemetry,
and 51% had abnormal resonance imaging. When comparing complications after the
intervention in relation to the average time from birth to initiation of
hypothermia, there was only a significant difference in the late initiation of
the intervention with the onset of clinical seizures. It is worth mentioning
that only 5 patients received the therapy in the first 6 hours (Table 3).
Table 3
Complications of treatment in relation to the time of
initiation of care
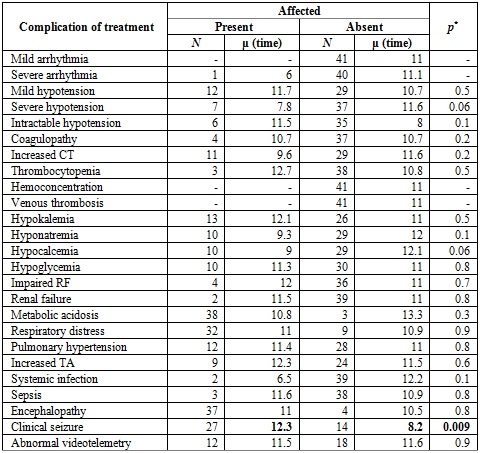
Note:The complications presented after the intervention are compared in relation to the average time in which hypothermia was initiated (average number of hours from birth to initiation of the intervention). The average hours of initiation of care was significantly higher in the case of patients with clinical seizure.
CT: clotting time; RF: renal function. TA: Transaminases.
*Student's T
Figures 1 and 2 show a comparison of the outcomes of survival or death after the intervention in relation to the same clinical variables of interest for each newborn. Patients with lower Apgar scores at 10 minutes and acidemia had higher mortality, which corresponded to 17%. All patients who died had cord blood gas < 6.91 and base excess > – 19; 14% of the patients who entered the therapy had a pH of 7.0 in umbilical cord blood, and 17% had a PH greater than 7.0.
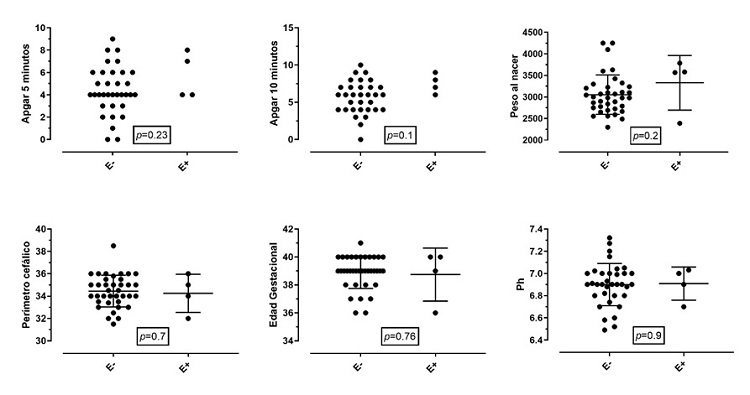 Figure 1
Events of encephalopathy related to clinical
variables of interest
Figure 1
Events of encephalopathy related to clinical
variables of interest
Note: The clinical
determinants of the birth of the newborn are compared with the presence of
encephalopathy. Proportionally, no significant differences were found between
the two groups. Birth weight in grams. Cephalic perimeter in centimeters. Gestational
age in weeks. E+: encephalopathy present. E-: encephalopathy absent. The
Apgar graph only shows the events, without mean or SD.
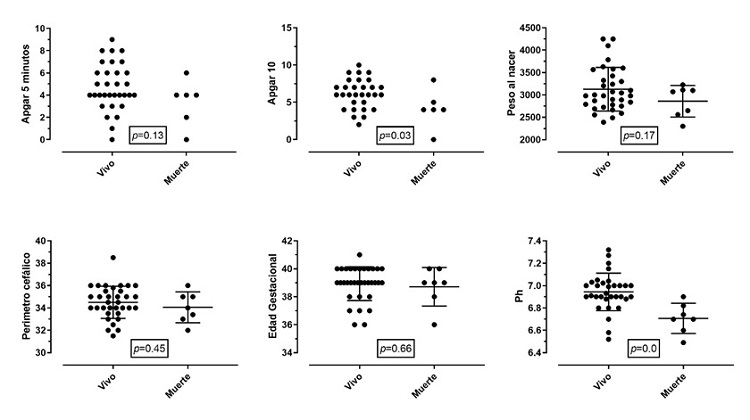 Figure 2
Outcome of patients (alive or dead)
Figure 2
Outcome of patients (alive or dead)
Note: The clinical determinants of the birth of the newborn are compared
with the outcome of death. Proportionally, no significant differences were
found between the two groups, except for 10-minute Apgar and the presence of acidemia. Birth weight in grams. Cephalic perimeter in centimeters. Gestational
age in weeks. The Apgar graph only shows the events, without mean or DE.
The outcomes of mortality
and encephalopathy were compared in relation to the time of care from the
moment of birth until the initiation of the intervention. Figure 3 shows each
of the events.
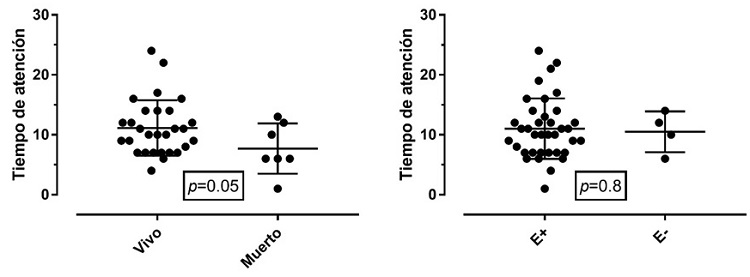 Figure 3
Time of care in relation to mortality
Figure 3
Time of care in relation to mortality
Note: Comparison of the
average time for initiation of the intervention after birth in relation to
mortality outcomes and the presence of encephalopathy. E+: encephalopathy
present. E-: encephalopathy absent.
Table 4 shows the comparison
of the prevalence ratio (PR) of encephalopathy and death according to exposures
of clinical interest. Regarding the outcome of
encephalopathy, PRs > 1 were evidenced in cases of metabolic acidosis,
respiratory distress, pulmonary hypertension and clinical seizures. However,
95% CIs go through a PR of 1. For the outcome of death, PRs > 1 are seen in
the case of cesarean section, increased clotting time, thrombocytopenia, hypocalcemia and impaired renal function (p < 0.05
and 95% CIs > 1).
Table 4
Prevalence ration
between the exposure of variables of clinical interest and the outcomes of
encephalopathy and death
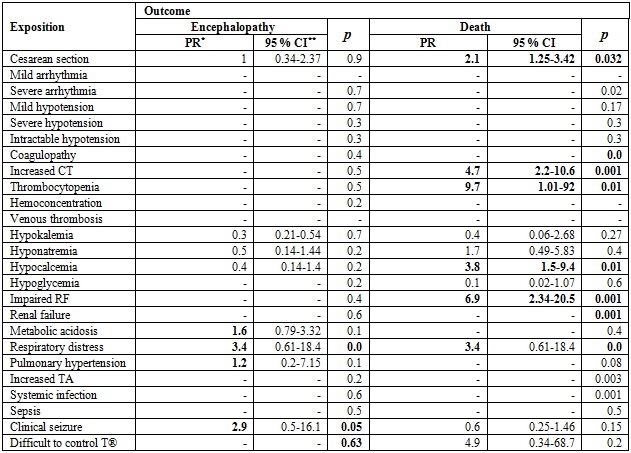
PR: Prevalence ratio. 95% CI: 95% confidence interval. RF: Renal function. TA: transaminases.
One patient had baseline gases compatible with
asphyxia, so he entered the protocol, but later it was determined that he had panhipotuitarianism.
Discussion
According to the data provided by the Public Health Surveillance Area of the District Department of Health, based on records from the Unified Registry of Affiliates, the perinatal mortality rate in Bogotá has shown an important decrease, of up to 13.4 per each 1,000 births for 2017. Early neonatal mortality had remained around 5.9 per 1,000 births until 2013 and began to fall to 4.3 per 1,000 births by 2014 (13). These trends are similar to the decrease in mortality in developing countries (14,15), emerging economies (16) and developed countries (17,18). This reduction is due to the control of perinatal infectious pathologies (19) and to the better management of complications derived from childbirth (20) and other newborn pathologies, including congenital malformations (21), as well as to an improvement in resuscitation techniques (22).
Since 2015, the Hospital Universitario San Ignacio is part of the District Neuroprotection Network and offers a proven clinical efficacy management (23) to neonates with moderate or severe asphyxia referred from different health institutions in the District and the department, regardless of their affiliation to social security.
Table 1 shows that the EEG activity before the intervention has significant moderately and severely abnormal results. EEG activity is a sensitive marker of brain damage in both preterm (24) and term infants (25). Encephalopathy is a progressive syndrome, so this tool becomes more and more important and helps us determine if a patient could benefit from entering the protocol reported in the literature with a 75% PPV for an event adverse, and the combination of this with an altered test has a PPV higher than each one separately (26).
Several clinical alterations are produced both by the underlying pathology and by therapy, and cannot be accurately distinguished (27). In our study, however, some of them were predictors of mortality, such as a low 10-minute Apgar, acidemia, history of cesarean section, increased clotting times, thrombocytopenia, hypocalcemia, and impaired kidney function (27).
90% of patients were diagnosed with some degree of encephalopathy at discharge, determined by some alteration in videotelemetry, brain magnetic resonance or neurological physical examination. However, only one of the surviving patients required gastrostomy, and was diagnosed with panhypopituitarism. The others were discharged with adequate sucking. 41.46% of the patients were discharged with mild encephalopathy.
A longer follow-up was not possible, because health insurers do not refer these patients to our institution for control. Unlike the study by Manotas et al. (11) on total body hypothermia, the mortality of our patients was not related to the time of initiation of therapy. All patients who died in our study had a cord blood gas pH < 6.91 and base excess > – 19, and 6 of them had a pH < 6.7. We share thrombocytopenia as a mortality risk factor when it is below 100,000.
Patients who took longer to receive active hypothermia therapy had more seizures and encephalopathy. However, for mortality, the average attention time in both types of outcome was similar. This finding could be considered important to support the entry of patients to hypothermia even after the 6 hours of therapeutic window initially described for the protocol, although with greater risk of having clinical seizures. Recent studies support this hypothesis (28).
14% of the patients who received the therapy had an umbilical cord blood pH equal to 7, and 17%, greater than 7. However, they were admitted to therapy because they met criteria A and B, which leads to the conclusion that it is not the only or most important criterion to define which patients require therapy, but it is considered a predictor of mortality, because none of these patients died. Some patients have differential diagnoses that should be taken into account and that can simulate asphyxia states, as happened with our patient with panhipotuitarianism.
Conclusions
Patients who had a low 10-minute Apgar score and severe acidemia had higher mortality. All patients who died had cord blood gas < 6.91 and excess base > – 19. There was a greater prevalence of clotting, electrolyte and renal alterations in the group with fatal outcome.
The results show that it is a priority to more accurately define the process of timely referral of patients and in the future to have the asphyxia clinic to ensure a comprehensive and multidisciplinary follow-up of patients managed with this therapy. However, in our study we did not find an important difference in mortality when the therapy was started after six hours.
Given the difference in mortality, compared with that of body hypothermia, additional studies are required to determine if in our context the two therapies are equally effective.
References
1.Almeida MFB, Kawakami MD, Moreira LMO, Santos RMVD, Anchieta LM, Guinsburg R. Early neonatal deaths associated with perinatal asphyxia in infants ≥2500g in Brazil. J Pediatr (Rio J). 2017;93(6):576-84.
2.Daripa M, Caldas HM, Flores LP, Waldvogel BC, Guinsburg R, de Almeida MF. Perinatal asphyxia associated with early neonatal mortality: populational study of avoidable deaths. Rev Paul Pediatr. 2013;31(1):37-45.
3.Penela-Vélez de Guevara MT, Gil-López SB, Martín-Puerto MJ, Romero-Escós MD, Herrera-Martín M, Urbón-Artero A. A descriptive study of perinatal asphyxia and its sequelae. Rev Neurol. 2006;43(1):3-6.
4.Secretaría Distrital de Salud. Lineamiento técnico para el manejo de la asfixia perinatal. Bogotá: Secretaría; 2015.
5.Shankaran S. Outcomes of hypoxic-ischemic encephalopathy in neonates treated with hypothermia. Clin Perinatol. 2014;41(1):149-59.
6.Volpe J. Neurología del recién nacido. 5 ed. Madrid: McGraw Hill; 2013.
7.Centro Nacional de Investigación en Evidencia. Guía de práctica clínica del recién nacido con asfixia perinatal. Bogotá; Ministerio de Salud; 2013.
8.Perlman JM, Wyllie J, Kattwinkel J, Atkins DL, Chameides L, Goldsmith JP, et al. Neonatal resuscitation: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science with Treatment Recommendations. Pediatrics. 2010;126(5):e1319-44.
9.Jacobs SE, Berg M, Hunt R, Tarnow-Mordi WO, Inder TE, Davis PG. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst Rev. 2013(1):CD003311. https://doi.org/10.1002/14651858.CD003311.pub3
10.Shah PS. Hypothermia: A systematic review and meta-analysis of clinical trials. Semin Fetal Neonatal Med. 2010;15(5):238-46.
11.Manotas H, Troncoso G, Sánchez J, Molina G. Descripción de una cohorte de pacientes neonatos con diagnóstico de asfixia perinatal tratados con hipotermia terapéutica. Perinatol Reprod Hum. 2018;32(2):70-7.
12.Shankaran S, Pappas A, McDonald SA, Vohr BR, Hintz SR, Yolton K, et al. Childhood outcomes after hypothermia for neonatal encephalopathy. N Engl J Med. 2012;366(22):2085-92.
13.Secretaría Distrital de Salud de Bogotá. Base de datos SDS y aplicativo Web RUAF_ND: datos Preliminares. Bogotá: Secretaría; 2017.
14.Mah-Mungyeh E, Chiabi A, Tchokoteu FL, Nguefack S, Bogne JB, Siyou HH, et al. Neonatal mortality in a referral hospital in Cameroon over a seven year period: Trends, associated factors and causes. Afr Health Sci. 2014;14(4):985-92.
15.Akinyemi JO, Bamgboye EA, Ayeni O. Trends in neonatal mortality in Nigeria and effects of bio-demographic and maternal characteristics. BMC Pediatr. 2015;15:36.
16.Wu QJ, Li LL, Li J, Zhou C, Huang YH. Time trends of neonatal mortality by causes of death in Shenyang. 1997-2014. Oncotarget. 2016;7(13):16610-8.
17.Dallolio L, Lenzi J, Fantini MP. Temporal and geographical trends in infant, neonatal and post-neonatal mortality in Italy between 1991 and 2009. Ital J Pediatr. 2013;39:19.
18.Gregory EC, MacDorman MF, Martin JA. Trends in fetal and perinatal mortality in the United States. 2006-2012. NCHS Data Brief. 2014(169):1-8.
19.Battin MR, Knight DB, Kuschel CA, Howie RN. Improvement in mortality of very low birthweight infants and the changing pattern of neonatal mortality: the 50-year experience of one perinatal centre. J Paediatr Child Health. 2012;48(7):596-9.
20.Shah V, Warre R, Lee SK. Quality improvement initiatives in neonatal intensive care unit networks: Achievements and challenges. Acad Pediatr. 2013;13(6 Suppl):S75-83.
21.Marantz P, Sáenz Tejeira MM, Peña G, Segovia A, Fustiñana C. Fetal and neonatal mortality in patients with isolated congenital heart diseases and heart conditions associated with extracardiac abnormalities. Arch Argent Pediatr. 2013;111(5):418-22.
22.Van Heerden C, Maree C, Janse van Rensburg ES. Strategies to sustain a quality improvement initiative in neonatal resuscitation. Afr J Prim Health Care Fam Med. 2016;8(2):e1-e10.
23.Galvao TF, Silva MT, Marques MC, de Oliveira ND, Pereira MG. Hypothermia for perinatal brain hypoxia-ischemia in different resource settings: a systematic review. J Trop Pediatr. 2013;59(6):453-9.
24.Ranasinghe S, Or G, Wang EY, Ievins A, McLean MA, Niell CM, et al. Reduced cortical activity impairs development and plasticity after neonatal hypoxia ischemia. J Neurosci. 2015;35(34):11946-59.
25.Jose A, Matthai J, Paul S. Correlation of EEG, CT, and MRI brain with neurological outcome at 12 months in term newborns with hypoxic ischemic encephalopathy. J Clin Neonatol. 2013;2(3):125-30.
26.Gluckman PD, Wyatt JS, Azzopardi D, Ballard R, Edwards AD, Ferriero DM, et al. Selective head cooling with mild systemic hypothermia after neonatal encephalopathy: Multicentre randomised trial. Lancet. 2005;365(9460):663-70.
27.Wayock CP, Meserole RL, Saria S, Jennings JM, Huisman TA, Northington FJ, et al. Perinatal risk factors for severe injury in neonates treated with whole-body hypothermia for encephalopathy. Am J Obstet Gynecol. 2014;211(1):41 e1-8.
28.Laptook A, Shanakaran S, Tyson J, et al. Effect of therapeutic hypothermia initiated afeter 6 hours of age on death or disability among newborns with hypoxic-isquemic encephalopathy. JAMA. 2017;318(16):1530-60.
Author notes
a Correspondence: fernando.suarez@javeriana.edu.co
Additional information
How to cite: Vargas-Vaca Y, Devia C, Bertolotto AM, Suárez-Obando F. Characterization
of newborns with moderate or severe perinatal asphyxia managed with selective
cerebral hypothermia in the newborn unit of the Hospital Universitario San Ignacio from June 2015 to March 2017. Univ. Med.
2019;60(4). https://doi.org/10.11144/Javeriana.umed60-4.crna