Introduction
The use of alternative and complementary medicines (CAMs) by cancer patients is widely practiced in different cultural contexts. However, prevalences differ greatly among countries (ranging from 5% to 74.8%), and even within countries there are marked differences among reported studies (1). There is little information on the use of CAMs in cancer patients in Colombia, and the available data from reference centers in Bogota indicate figures between 70% and 80% (2,3).
The high frequency with which these therapies are used has led more and more cancer centers to incorporate them into the comprehensive management of patients in coordination with allopathic medicine. But despite the high acceptance and use of CAMs by patients, integrative medicine has not expanded much in our environment, and practices in this context continue to be given outside the main course of treatment. This follows from the limited availability of CAM services in Colombia and the fact that most of these services are carried out in independent private practice (4).
A contributing factor to this situation may be the lack of understanding of the perceptions of patients, professionals and caregivers regarding alternative medicines, which in turn can lead to communication problems between these actors. In Colombia there is very little information on this subject. A study in the department of Cundinamarca showed that, although nearly 50% of public sector doctors have a positive attitude towards the use of alternative medicines, only 18% of them recommend them to their patients (5). However, this information does not discriminate between general practitioners and specialists, and it is not clear what the perception of professionals may be in a highly specialized environment with great technological development and influence by the pharmaceutical industry such as cancer care.
Given the growing burden of malignant neoplasms, which represent the second leading cause of death in the country and generate more than 100,000 new cases per year (6), added to the high frequency of CAM use in a life-threatening conditions, it is necessary to better understand the perceptions of patients and professionals regarding these practices. This in order to build knowledge and improve communication and cancer care in the country. This article presents the results of an exploratory study that investigated the perception of patients and caregivers and analyzed coincidences and divergences of the two perspectives on the use of alternative medicines in cancer patients.
Methods
A phenomenological interpretative analysis (7) was carried out in order to identify the meaning and significance of personal experiences in relation to the use of CAMs for cancer care. The project was approved by the Ethics and Research Committee of the Hospital Universitario San Ignacio/School of Medicine of the Pontificia Universidad Javeriana.
We used the technique of focus groups, which were made up of patients, caregivers and professionals. A focus group was held with patients and caregivers, and a focus group with cancer care professionals. Informed consent was obtained from all participants. For the patient focus group, representation of both sexes, different age groups, different types of cancer, and different times in the course of the disease and treatment was sought. For the professional focus group, specialists in clinical oncology, hemato-oncology, radiation therapy, surgery, palliative care, nursing and alternative medicine were invited both in their practice (mind-body therapy) and in the research area.
The Integrative Medicine Service and the nurses managing the functional cancer units of the Javeriana Center of Oncology made the call for patients and caregivers. The call was initially oriented to individuals with high information potential. In view of the low response to the personalized call, finally an open call was made. The call for professionals was personalized so that there would be representation of the areas described.
To develop the focus groups, a guide was created that included the description of the project and the context of the focus group, the presentation of the facilitators, the expected duration of the focus group (one hour and fifteen minutes) and the domains or categories to be investigated with the guiding questions. The domains in the patient focus group were:
-
Understanding of what is complementary medicine and the denominations used to refer to it.
-
Types of practice.
-
Usual sources of complementary medicines.
-
Times when they are used in relation to the evolution of the disease.
-
Reasons for use.
The domains in the professional focus group were:
-
Understanding of what is complementary medicine.
-
Known practices.
-
Recommended practices and contraindicated or discouraged practices.
The focus groups were developed with a moderator and two observers who were part of the research team. The sessions were recorded in audio and video, and the content of each session was transcribed by administrative personnel for analysis. A research assistant verified the content for accuracy. Finally, it was reviewed by the principal investigator, in order to guarantee reading comprehension and the procedures carried out before coding and interpreting the data.
Each of the domains was coded by three members of the research group independently and blindly, both in the patient focus group and in the professional focus group. The codes were then grouped for interpretation. The identification of categories was initially carried out by two members of the research team, and these were reviewed by a third member of the team, who re-categorized them by grouping the initial categories. Such proposed grouping was triangulated with the entire research team to generate definitive categories.
Results
The focus group of patients and caregivers had 17 participants, 13 women and 4 men. In total, there were 4 caregivers and 11 patients, 2 participants did not indicate whether they were patients or caregivers. The types of cancer represented include breast cancer, prostate cancer, stomach cancer, and hematolymphoid neoplasms, with an age range of 49 to 77 years. The professional focus group had 7 participants, 2 women and 5 men. Areas of practice represented included hemato-oncology, surgery, clinical oncology, mind-body therapy (yoga teacher), and alternative medicine research (biologist).
The results represent the emerging categories on the topics of interest. Both from the perspective of patients/caregivers and professionals, two categories associated with their perception, knowledge, experiences and practices in relation to CAMs emerged, namely: conceptualization and experience. Each of these includes subcategories that are illustrated by excerpts from what the participants expressed (tables 1 and 2).
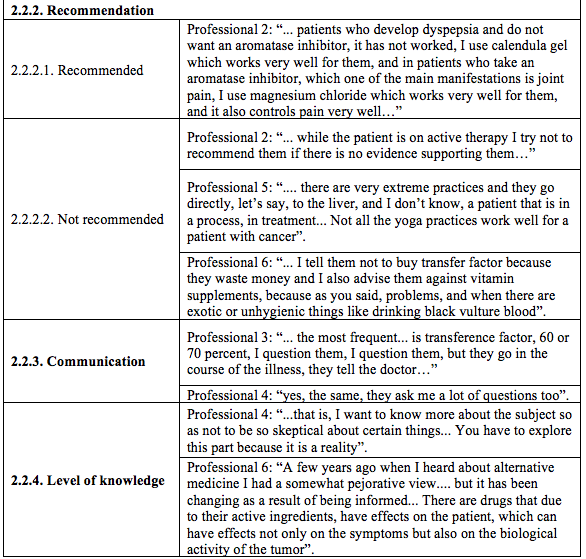
Table 1
Examples supporting the emerging categories as described by the patientcaregiver group
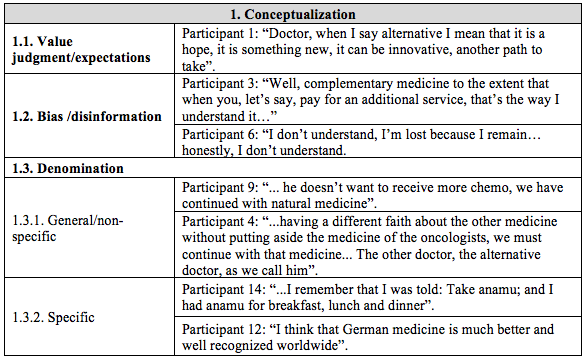
Table 1 (cont.)
Examples supporting the emerging categories as described by the patientcaregiver group
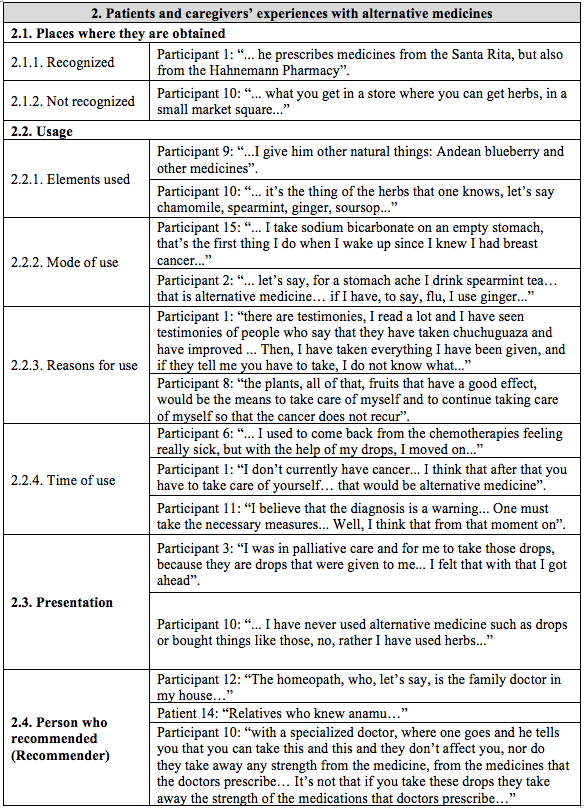
Table 2.
Examples that support the emerging categories according to the description of the group of professionals
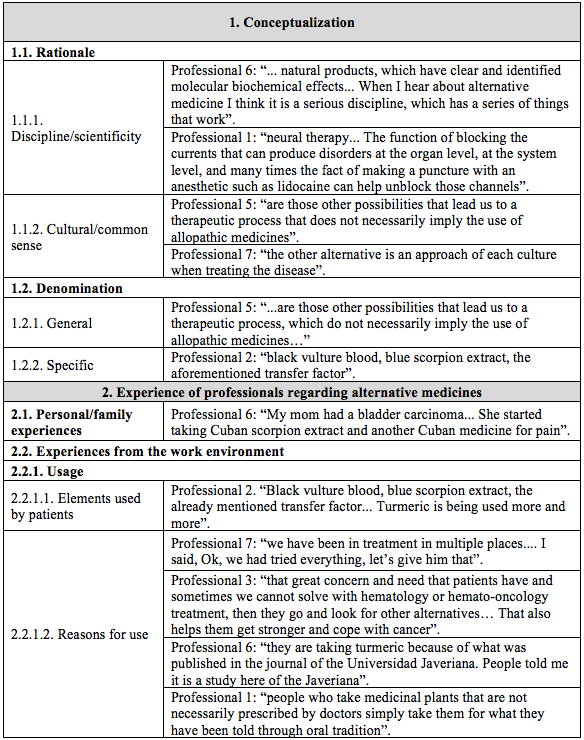
Table 2 (cont.)
Examples that support the emerging categories according to the description of the group of professionals
Conceptualization about alternative and complementary medicines
Conceptualization refers to aspects that the participants include in their discourse to characterize what the CAMs are for them. Three subcategories were found in patients/caregivers and two subcategories for professionals (Figure 1).
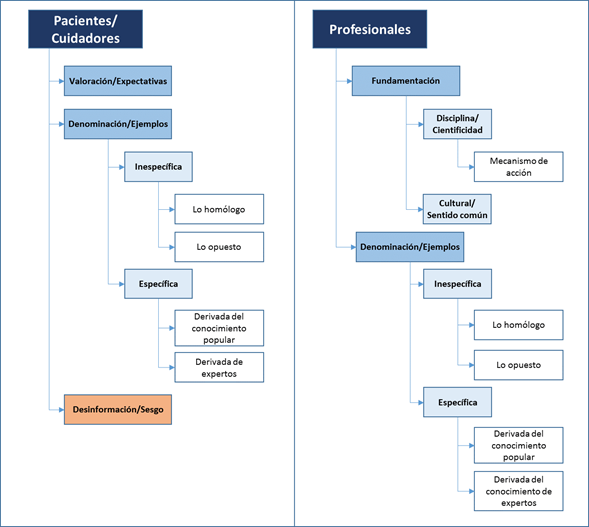 Figure 1.
Emerging categories on the conceptualization of alternative and complementary medicines by patients/caregivers and professionals
Figure 1.
Emerging categories on the conceptualization of alternative and complementary medicines by patients/caregivers and professionals
Value judgment/expectation reflects what is expressed by some patients and caregivers, for whom CAMs are defined in terms of positive effects on the health condition. It also implies a concept based on what they could expect from CAMs as an alternative treatment for their disease, admitting a hopeful path that includes characteristics of innovation and therapeutic complementarity.
The denominations (expressed as examples) allow identifying how the CAMs are conceptualized (Figure 1) and include two perspectives: general and specific (Table 3). General or non-specific denominations include both terms related to CAMs such as “naturist” or “natural”, which have been nominated as the homolog, as well as names such as “alternative”, assigned according to types of medicine that would be in opposition to what is considered CAM as “alternative” (Table 1: 1.3.1; Table 2: 1.2.1). In the case of examples with specific denomination, both patients and professionals identify practices or elements derived from popular knowledge or expert knowledge (Table 1: 1.3.2; Table 2: 1.2.2).
Table 3
Denominationsexamples that define alternative or complementary medicines
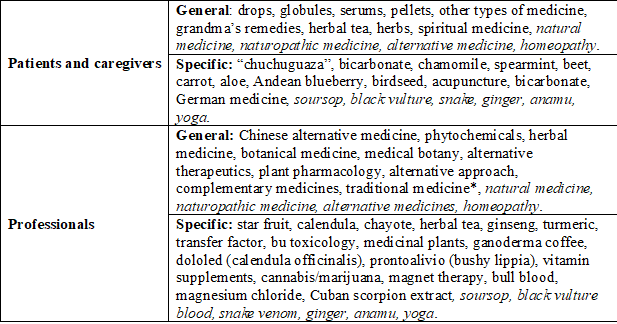
*Some professionals use the term to denote allopathic medicine Table 2: 1.2.1.
Finally, in the discourse of the professionals, the conceptualization of the CAMs was identified from their rationale, referring to lines of explanation or argumentation regarding the theoretical-conceptual elements that underlie CAMs. There are, in the first place, explanations from disciplines that give them a certain degree of scientificity. From this group comes the consideration of the mechanisms of action of CAMs that represent the way in which certain elements or activities affect the body and the health condition. Secondly, there are explanations based on common sense and cultural elements (Table 2: 1.1).
As an important element, some degree of bias or disinformation emerging among patients and caregivers was identified. This refers to inaccurate, incomplete and, sometimes, erroneous information regarding what CAMs are, such as their confusion with the benefit plans of the Colombian health system (complementary medicine as a complementary health plan); there are even doubts about the recognition of whether some practices or elements they use could be considered CAM (Table 1: 1.2) . On the other hand, there are discrepancies in the use of some terms such as traditional medicine, which may have the opposite meaning according to the point of view of the actors: for some oncology specialists it represents allopathic medicine and for CAM professionals it represents alternative and complementary medicine.
Experience with alternative and complementary medicines
In this category, the ways and means in which participants relate to CAMs are identified, according to their role in requiring or providing cancer care. There is evidence of direct contact with CAMs; but also indirect contact, through third parties such as family members (both of patients and professionals), or through the patients in the case of professionals (experience from the work environment) (Figure 2).
In the experience of patients and caregivers, four relevant aspects were identified: the place where they obtain the CAMs, their use, the presentation, and who recommends them. In the case of professionals, the experience in the work environment includes appreciations about the actions and behaviors observed in their patients and aspects resulting from their own professional practice, grouped in four areas, which include the use, the recommendation they make about the CAMs, the communication about them and the level of knowledge (Figure 2).
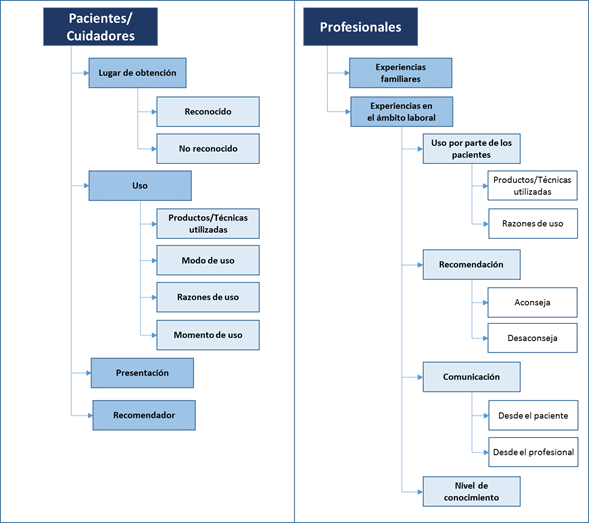 Figure 2.
Emerging categories from the experience of patients/caregivers and professionals with alternative and complementary medicines
Figure 2.
Emerging categories from the experience of patients/caregivers and professionals with alternative and complementary medicines
From the personal point of view, professionals refer experiences with close relatives (mother, father), especially those who are oncologists, and in some cases they report favorable effects. They attribute their use to having no other options after the failure of other therapeutic routes, or to considering that some CAM practices work to alleviate symptoms, an argument that is logically expressed also for use in the work environment.
For patients and caregivers, the place where they obtain CAMs is important, as the characteristics of the source favor a positive perception of them. They identify recognized places, such as homeopathic laboratories or naturopathic centers, referred to as sites for exclusive provision of CAMs. However, it is considered that some CAM elements can be obtained in places without such recognition, such as market squares (Table 1: 2.1).
Usage is the second aspect of interest. For patients and caregivers, there are features related to the way certain elements of CAMs are used that allow them to describe nuances of the experiences they have had. This view is also perceived by professionals in the approach they make to their experience from what is reported by patients. In this regard, the use of regularly consumed products such as fruits is considered in certain circumstances an element of CAM (Table 1: 2.2.1). In other cases, the positive effect refers not only to the element, but to the way it is used (e.g., on an empty stomach) and the specific indication (e.g., stomach pain vs. flu) (Table 1: 2.2). There are also reasons for use that include general health care (physical and emotional well-being), the search for alternatives other than allopathic medicine, the perception of effectiveness for the management of specific circumstances (pain, depression and anxiety), and the possibility of curing or controlling the disease as a complementary tool to oncological management (Table 1: 2.2.3; Table 2: 2.2.1). Finally, the use of CAMs in relation to the moment of evolution of the disease is identified as an element of the experience. Thus, for most participants the diagnosis triggers the use of CAMs, and these are used throughout the evolution of the disease. For others it varies according to particular situations, for example, parallel to chemotherapy to reduce side effects or, conversely, only at the end of treatment as part of health care or with the intention of not interfering with cancer treatment (Table 1: 2.2.4).
Presentation is an aspect recognized mainly by patients and caregivers. It refers to the physical presentation of the products and how this relates to particular value judgments. For some patients the presentation is more than an element of recognition of CAMs: it is what they associate with positive effects. In addition, certain presentations are viewed with more confidence and less fear. For example, preferring fruits or herbs to drops or other processed products (Table 1: 2.3).
The recommender is the fourth element considered as part of the experience by patients and caregivers. However, a hierarchy in relation to the recommender is not clearly observed, although approval by the physician generates reassurance (Table 1: 2.4). The actors include physicians (allopathic and alternative), relatives and peers. The role that social networks can play is mentioned, without it being clear whether or not the origin of the information (who sends it) plays an important role in decision-making regarding the use of CAMs. This subcategory connects with other sources of information accessed by patients interested in using CAMs (internet, media), with their information needs (treatment options, effectiveness, indication, interaction with their oncology treatments) and with the reasons why some use them.
On the other hand, advising or discouraging as a recommendation from professionals reflects their position regarding the use of CAMs by their patients. Some discourage the use of any type of CAM, others discourage using specific types of CAM in all circumstances (transfer factors), and still others discourage the use of certain forms of CAM in specific circumstances (Table 2: 2.2.2). Reversely, there are some forms of CAM that are recommended for the management of specific conditions such as dyspepsia associated with the use of aromatase inhibitors.
From the professionals’ perspective, the communication subcategory emerges, which includes considerations on how they perceive the actions of patients and physicians, aimed at clarifying doubts, requesting or restricting information on the use of CAMs. There is a general appreciation in relation to the importance of inquiring with the patient and the recognition of a communicative process in which, upon questioning the patient, information is received about how they are using CAMs and allows for feedback.
To finish this segment, the subcategory of level of knowledge is included, which arises from the statements of some professionals. It refers to the identification of a need for information and knowledge on the part of professionals about CAMs, which they associate with the possibility of better professional practice in the face of the reality of patients who use CAMs. It is also evident the change of perspective of some professionals in relation to CAMs after gaining more knowledge; they move from a derogatory opinion to a perspective of recognition of the effectiveness in some practices that provide scientific evidence.
Discussion
In this study, relevant differences were found between patients and professionals related to oncological care both in the conceptualization and in the experience with alternative medicines.
From the point of view of conceptualization, even the specific and non-specific denominations as categories common to the two groups (Figure 1) denote differences in the terms and examples used (Table 3). This suggests uneven language, and probably significant discrepancies in the origin of the information. This becomes more evident if the emphasis on the scientific foundation is taken into account as the basis of conceptualization for professionals versus conceptualization based on the expectation of CAMs as a promising option for patients and caregivers.
Previous studies have shown similar findings, in which scientific evidence on the part of care providers is associated with indifference or opposition to the use of alternative medicines and, consequently, generates an anticipation of negative responses from patients. This situation limits the communication on the subject (8,9), since, as it is derived from the results, the scientific evidence does not seem to be a relevant aspect for them. Along the same lines, discrepancies are identified in the perspectives of patients and oncologists with respect to decision-making on the use of CAMs. It has been observed that for oncologists adverse effects constitute a criterion for whether or not recommending their use. However, for patients this is not so relevant, while their possible therapeutic effectiveness is (10,11). This coincides with what our study reveals in relation to what the professional advises against and what the patient considers reason for use.
It has also been seen that personal experience by trial and error, testimonies and popular literature become relevant sources of information if they coincide with the patients’ previous beliefs and views (12, 13, 14). Similarly, our results indicate that the source of information (Recommender in Figure 2) and the place where they are obtained play a relevant role in the decision to use CAMs, without the treating physician playing a leading or a hierarchical role. However, both the degree of recognition of the source for obtaining them and the approval of the doctor generate greater reassurance with the use of CAMs. Recent studies indicate that the CAM user sees himself/herself as the primary administrator of his/her health care (expressed as reasons for use in our study), but considers that better communication with the health care provider provides more security, as does his/her belonging to a community of practitioners (15).
It has been seen that the structure of an individual’s social network, as well as the role he or she plays in the network, determines the possibility of using CAMs by allowing greater access to sources of information and conditioning possibilities of knowing and evaluating various alternative therapies (16). This coincides with what was reported by some participants regarding who recommended the use and, in general, with the sources of information, since on repeated occasions it was their peers, friends and relatives who told them about the CAMs. This coincides with previous studies that indicate that family and friends occupy an important place as a source of information on CAMs (12,17).
The decision is a personal and complex process. The information that patients take and consider as adequate depends on their history, beliefs, personal situation and disease process (12). On the other hand, the person who appears as a recommender and provides information constitutes verbal authority, and can be either the doctor or the peer who gives his/her testimony, or the person who claims to have the solution to the problem. Each of them represents a different value (expertise), identification or hope in the face of the patient’s need.
Approval/disapproval of traditional practices is closely related to how communities shape human behavior. In this context, it has been seen that the use of CAMs can serve as a bridge to belonging to a community (a fact that could have greater relevance in the face of a life-threatening disease). But, in turn, belonging to a community of practitioners can be perceived as a way to increase access to information about treatment options and as a way to reduce the risk of social sanction if there is a deviation from the traditional form of treatment (16). Accordingly, for the professionals in our study there are practices that should be discouraged, but among patients this category does not emerge from communication with the physician (Figure 2). Again, physician approval creates greater reassurance, but it seems that physician approval/disapproval is not as decisive in the use of CAMs as belonging to a community of practitioners. Despite this, some patients highlight the use of CAMs only when they finish conventional therapy (time of use), which could be related to adverse medical advice.
Access to social networks through electronic media can play a relevant role in the use of CAMs, and was identified as a source of information in our study (15,18). Some studies show the relationship between Internet use and the patient’s perception of self-management and the possibility of receiving support (19,20). Cancer patients have multiple psychosocial needs, as they are forced to assume changes associated with conditions of physical and emotional vulnerability. Therefore, regaining the perception of control is important, and when they autonomously make certain decisions regarding their treatment, they can experience emotional well-being.
Communication emerges as a category of experience only from the perspective of professionals. A review on the subject shows that communication difficulties are a relevant indirect risk for patient safety, referred to four categories that include differences in the philosophical values attributed to CAM between users and conventional care providers, difficulties in prescribing complementary medicines due to the lack of scientific evidence (rationale), and lack of information on CAM from conventional care providers (knowledge) (21). Communication and level of knowledge emerge from work experience, possibly related to the high frequency of use of CAMs by cancer patients (2,3) and the evidence on adverse effects and interaction with systemic treatment of cancer (21). However, it is possible that family experiences play some role in the perception of professionals regarding the use of CAMs and generate a greater interest in understanding them better.
In any case, the differences in the perception of patients and professionals could have unfavorable consequences for the comprehensive care of cancer patients, referring above all to an affectation in the patient’s adherence to treatment, deficient communication and inappropriate decision-making from both perspectives. This possibility suggests the need for additional research on the subject in our environment, because despite the coincidence of our results with previous studies, the cultural context and the Colombian health system may determine particular conditions for decision making regarding cancer treatment. In addition, these differences and their potential implications for patient care invite care providers to learn more about CAMs so that they can approach the issue with their patients with more evidence and facilitate effective communication in consultation that will decrease the risks associated with CAM use.
Our study has several limitations. We believe that despite the lower attendance at the professional focus group, the number of participants is appropriate to obtain the required information (22). However, only one group per population type was able to restrict the theoretical saturation of the data. In turn, the inclusion of non-medical participants could interfere with the open expression of the attendees given the differences in role and knowledge about CAMs. However, this possible effect was countered by working with a small group, where the moderator favored the free participation of all members, and we believe that, on the contrary, the variability enriched the discourse and revealed dissimilar perspectives. Even so, reference is made to the necessary balance between intragroup heterogeneity and homogeneity, since they also share aspects such as contact with CAMs. Similarly, we believe that the participation of a small number of caregivers gives a voice to patients who because of their clinical condition would not be able to express their opinion.
Although this was an exploratory study, the results coincide with previous reports. Additionally, we are not aware of previous studies on the subject in Colombia, so we consider that although our study was exploratory, it constitutes a relevant contribution to promote comprehensive care that properly incorporates other dimensions of care in the main course of cancer treatment, and also to stimulate research in this area.
Conflict of interest
None of the authors have any conflict of interest.
Acknowledgments
This study was funded by the Colombia Científica program of the Ministry of Science and Technology and the Pontificia Universidad Javeriana. Call Ecosistema Científico, contract FP44842-221-2018
Referencias
1. Frass M, Strassl RP, Friehs H, Müllner M, Kundi M, Kaye AD. Use and acceptance of complementary and alternative medicine among the general population and medical personnel: a systematic review. Ochsner J [internet]. 2012;12(1):45-56. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3307506/
2. Sánchez R, Venegas M. Aproximaciones complementarias y alternativas al cuidado de la salud en el Instituto Nacional de Cancerología: estudio de prevalencia. Rev Colomb Cancerol [internet]. 2010;14(3):135-43. Disponible en: https://www.revistacancercol.org/index.php/cancer/article/view/457
3. Sánchez R, Ibáñez C, Suárez A. Utilización de terapias complementarias y alternativas en niños con cáncer. Rev Salud Pública. 2016;17(5):699-712. https://doi.org/10.15446/rsap.v17n5.38695
4. Rojas-Rojas A. Servicios de medicina alternativa en Colombia. Rev Salud Pública [internet]. 2012;14(3):470-7. Disponible en: http://www.scielo.org.co/pdf/rsap/v14n3/v14n3a10.pdf
5. Sierra-Ríos SP, Urrego-Mendoza DZ, Jaime-Jaimes JD. Conocimientos, actitudes y prácticas acerca de la medicina alternativa en médicos vinculados a hospitales públicos de Cundinamarca, Colombia. Rev Salud Pública [internet]. 2012;14(3):478-90. Disponible en: https://revistas.unal.edu.co/index.php/revsaludpublica/article/view/24915
6. International Agency for Research on Cancer. Global Cancer Observatory, Cancer Today [internet]. Population Fact Sheets, Colombia. 2018 [citado 2020 mar 11]. Disponible en: https://gco.iarc.fr/today/data/factsheets/populations/170-colombia-fact-sheets.pdf
7. Smith JA, Osborn M. Interpretative phenomenological analysis. En: Qualitative psychology: a practical guide to research methods. 2.ª ed. Londres: Sage; 2008. p. 53-80.
8. Tasaki K, Maskarinec G, Shumay DM, Tatsumura Y, Kakai H. Communication between physicians and cancer patients about complementary and alternative medicine: exploring patients’ perspectives. Psychooncology. 2002;11(3):212-20.
9. Gall A, Anderson K, Adams J, Matthews V, Garvey G. An exploration of healthcare providers’ experiences and perspectives of traditional and complementary medicine usage and disclosure by Indigenous cancer patients. BMC Complement Altern Med. 2019;19(1):259. https://doi.org/10.1186/s12906-019-2665-7
10. Yang G, Zhang H, Gan Z, Fan Y, Gu W, Ling C. Discrepant views of oncologists and cancer patients on complementary and alternative medicine in a Chinese general hospital. Integr Cancer Ther. 2018;17(2):451-7. https://doi.org/10.1177/1534735417725579
11. Keene MR, Heslop IM, Sabesan SS, Glass BD. Complementary and alternative medicine use in cancer: a systematic review. Complement Ther Clin Pract. 2019;35:33-47. https://doi.org/10.1016/j.ctcp.2019.01.004
12. Verhoef MJ, Mulkins A, Carlson LE, Hilsden RJ, Kania A. Assessing the role of evidence in patients’ evaluation of complementary therapies: a quality study. Integr Cancer Ther. 2007;6(4):345-53.
13. McLaughlin D, Lui C-W, Adams J. Complementary and alternative medicine use among older Australian women: a qualitative analysis. BMC Complement Altern Med. 2012;12(34). https://doi.org/10.1186/1472-6882-12-34
14. Schafer MH. Discussion networks, physician visits, and non-conventional medicine: probing the relational correlates of health care utilization. Soc Sci Med. 2013;87:176-84.
15. Ávila C, Grace S, Bradbury J. How do patients integrate complementary medicine with mainstream healthcare? A survey of patients’ perspectives. Complement Ther Med. 2020;49:102317. https://doi.org/10.1016/j.ctim.2020.102317
16. Goldman AW, Cornwell B. Social network bridging potential and the use of complementary and alternative medicine in later life. Soc Sci Med. 2015;140:69-80.
17. Labidi S, Ennouri S, Rachdi H, El Benna H, Mejri N, Daoud N, et al. Use of complementary and alternative medicine in cancer: A Tunisian single-center experience. Bull Cancer (Paris). 2020;107(2):209-14. https://doi.org/10.1016/j.bulcan.2019.10.007
18. Bauer F, Schmidt T, Eisfeld H, Dubois C, Kastrati K, Hochhaus A, et al. Information needs and usage of complementary and alternative medicine in members of a German self-help group for gastrointestinal stroma tumours, sarcoma, and renal cancer. Complement Ther Med. 2018;41:105-10. https://doi.org/10.1016/j.ctim.2018.09.008
19. Holmes MM. Why People living with and beyond cancer use the internet. Integr Cancer Ther. 2019;18(1):1-6. https://doi.org/10.1177/1534735419829830
20. Lleras de Frutos M, Casellas‐Grau A, Sumalla EC, Gracia M, Borràs JM, Ochoa Arnedo C. A systematic and comprehensive review of internet use in cancer patients: Psychological factors. Psychooncology. 2020;29(1):6-16. https://doi.org/10.1002/pon.5194
21. Stub T, Quandt SA, Arcury TA, Sandberg JC, Kristoffersen AE, Musial F, et al. Perception of risk and communication among conventional and complementary health care providers involving cancer patients’ use of complementary therapies: a literature review. BMC Complement Altern Med. 2016;16(353):14.
22. Johnson RB, Christensen L. Educational research: quantitative, qualitative, and mixed approaches. New York: Sage; 2014.
Author notes
a Corresponding author: mpgarcia@husi.org.co
Additional information
How to cite: García-Padilla P, Ordóñez Reyes C, Medina P, Fernández Deaza G, Morales OL, Murillo R. Perception of alternative and complementary medicine for cancer care among patients and health professionals: an exploratory study. Univ. Med. 2021;62(1). https://doi.org/10.11144/Javeriana.umed62-1.pppu