Introduction
The perception of pain in newborns has been recognized since the 1980s. However, up to 80% of them do not receive any management before painful procedures. The problem is greater if one considers that, on average, there are 15 such procedures per day during hospitalization (1). Multiple clinical practice guidelines, such as those published by the American Academy of Pediatrics (2) and the Canadian Pain Management Society (3), recognize its importance and propose guidelines for its management, but adherence to these recommendations is low. The reasons for this include that health care personnel underestimate pain sensation, do not know the mechanisms for its evaluation or limit management to maximum pain procedures (4).
The lack of knowledge regarding the evaluation and management of pain in neonates is a widespread problem, as evidenced in studies carried out in Korea (4), China (5), Brazil (6), India (7), the United States (8) and Japan (9). These studies highlight the importance of designing a strategy that comprehensively addresses the diagnosis and management of pain in this population.
There are findings of the consequences of inadequate pain management, such as physiological or hemodynamic instability, alteration in brain development and neurodevelopment, abnormalities in stress response, and somatosensory systems, which may persist throughout childhood (8).
The objectives of the research were, on the one hand, to evaluate the impact of designing and implementing an educational strategy on the perceptions and knowledge of health personnel working in three newborn units in the city of Bogotá (Colombia), both public and private; on the other hand, to evaluate whether there is a change in clinical practice regarding the evaluation and management of pain, comparing a period before and after the implementation of this educational strategy.
Methodology
The present work corresponds to a before and after study. It was carried out at the Hospital Universitario San Ignacio (private fourth level of care institution), at the Fundación Hospital de La Misericordia (private fourth level of care institution), and at the Instituto Materno Infantil de Bogotá (public third level of care institution) between June and December 2018. It was submitted to the Ethics Committee of the three hospitals where it was performed (Minute 10-2018, Minute 251 of September 24, 2018, and Minute 68-2018, respectively). Survey participants signed informed consent. The work was conducted in three phases.
Initial phase
Seventy-five medical records were analyzed (25 in each institution) that included neonates who had undergone a minor diagnostic or painful procedure (venipuncture, tube passing, aspiration, or injection), or a major or therapeutic painful procedure (intubation, umbilical catheter insertion, lumbar puncture, abdominal surgery, etc.). The medical records were reviewed to see if any pain assessment scale had been applied, if there was a record and management of the first diagnostic or minor pain procedure, and, if there was, of the first therapeutic or major pain procedure, both at a non-pharmacological and pharmacological level.
The following patients were excluded from the analysis of the medical records:
-
In end-of-life protocol (see definition of variables), because the management is within the framework of a standardized protocol that includes analgesia and sedation, to avoid or reduce pain in known incurable or untreatable pathologies.
-
With a diagnosis of moderate-severe perinatal asphyxia in hypothermia protocol, given that, in addition to being in minimal manipulation protocol, they usually receive intravenous opioids which make pain assessment not objective.
-
Hospitalized due to absence of caregiver, because they are healthy and do not require pain intervention.
Following that assessment, a survey was conducted between June and July 2018, targeting all care staff working in the three newborn units, including specialist physicians, resident physicians, nurses, nursing assistants, and respiratory therapists. Students, personnel with less than one month of seniority, interconsultant physicians or circumstantial personnel, and those who freely did not wish to participate in the study were excluded.
The survey had a Likert-type format (see annex). The survey diffusion mechanism was via institutional e-mail, and the Research Electronic Data Capture (REDCap) tool was used, which is a secure web application for creating and managing online surveys and databases. (https://redcap.husi.org.co/)
Second phase
This strategy had different moments in its second phase:
Search and analysis of the best available evidence. The existing guidelines in the literature were analyzed (2,3,10-20) and two were chosen: the guidelines of the American Academy of Pediatrics (2) and the Canadian Pain Management Society (3), considering that their recommendations are recognized worldwide and could be applied to our patients.
Programmed activities with physicians and nurses. The guidelines were presented to all personnel working in the three units, according to shift schedules, where doubts were clarified and clinical cases were presented with possible scenarios.
Teaching the Premature Infant Pain Profile (PIPP) scale through a video. Subsequently, and interactively, a video was exhibited showing a newborn who had just arrived from surgery, and how to use the PIPP scale was taught (21), analyzing each item step by step. This scale was selected because of the simplicity of its diligence, the short time it takes to apply it, and its validation in both preterm and term newborns (23-28).
Request for the implementation of an electronic pain record in the clinical history. It was suggested to the coordinators of the three units that there should be a box in the clinical history corresponding to the value of the pain scale next to the vital signs.
Maintenance of the program. Visible copies of the PIPP scale were left in the different units, as well as a laminated infographic with data such as the scale and a table with pain management according to each procedure, visible with the phrase: "Remember to diagnose and treat pain". There was additional training in the use of the scale with the nursing group, at the direct request of that same group.
Final phase
The final phase consisted of evaluating the outcome of the educational intervention five months after implementation:
Seventy-five new medical records were analyzed. In them, we again evaluated if any scale was applied and if there was a record and management of pain associated with the first diagnostic or minor painful procedure, and in the first therapeutic or major painful procedure, both at a non-pharmacological and pharmacological level.
In addition, the same survey (see appendix) was applied to the professionals to compare the knowledge and skills of the health personnel before and after the training.
Statistical analysis
The sample size was calculated based on results of previous studies, where it was reported that the use of pain relief methods varies between 30.8 % and 75.7 %; the use of pain assessment scales ranges between 22.5 % and 65.6%; and the collection of information on pain management in hospitalized patient ranges between 51.2 % and 81.2 % (29). McNemar's method was used to evaluate a paired difference of proportions, with a power of 80% and an alpha error of 0.05, assuming a one-tailed hypothesis. The calculated sample size was 72 patients in the three institutions.
Mean and median, standard deviation or median and interquartile range is reported, depending on whether the assumption of normality in the data distribution was met, which was evaluated through a Shapiro-Wilk test. To compare continuous variables, a t-test and a Mann-Whitney test were used, depending on the type of variable. A McNemar´s test was used for paired proportions. The indicators taken from the medical records for the paired analysis of proportions were: recording of pain in the first diagnostic procedure, in the first therapeutic procedure, recording of pain scales, and recording of the use of non-pharmacological analgesia and pharmacological analgesia at either of the two points in time.
Results
Results of the evaluation of the change in clinical practice.
The characteristics of the patients evaluated before and after the implementation of the educational strategy are presented in Table 1. The mean gestational age, median chronological age, and the diagnoses for which they were admitted to the neonatal unit were similar in the two timepoints.
Tabla 1
Characteristics of patients evaluated before and after implementation of the educational strategy
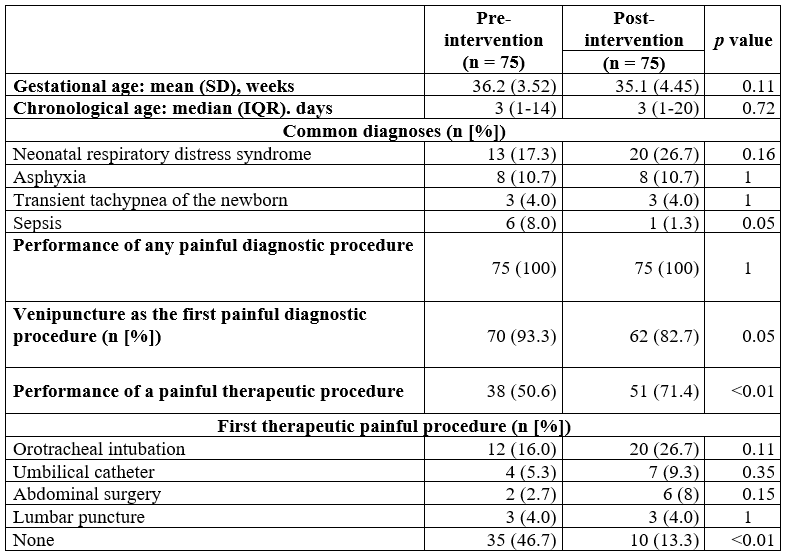
SD: standard deviation; IQR: interquartile range.
Diagnostic or minor procedures were performed in 100 % of the patients; the first painful diagnostic procedure was venipuncture, in more than 80 % of the neonates.
Table 2 shows the pain recording and management activities recorded in the clinical history, before and after the implementation of the educational strategy. A significant change was evidenced in the proportion of patients in whom some scale was used to evaluate pain related to diagnostic (1.3% vs. 20%; p < 0.01) and therapeutic procedures (0% vs. 56.7%; p < 0.01), and in the proportion of patients in whom pharmacological measures were administered (17.3% vs. 53.7%; p < 0.01). There were no differences in the recording of non-pharmacological analgesia. Medical personnel were the group with the greatest increase in pain records in medical records (22.6 % vs. 54.7 %; p < 0.01); however, the change was also significant in other health professionals.
Tabla 2
Recording and management of pain before and after the implementation of the educational strategy
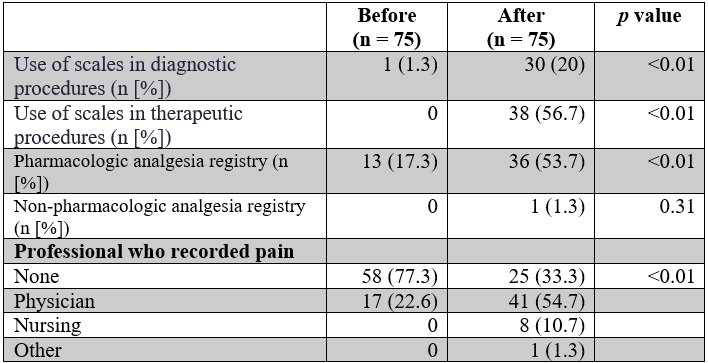
Survey results
A total of 102 health professionals were invited to participate. Of these, 70 professionals participated in each period. The characteristics of the surveyed population are presented in Table 3. This participation corresponds to 75% of the medical staff and 74% of the nursing staff of the three institutions.
Tabla 3
Characterization of the surveyed population
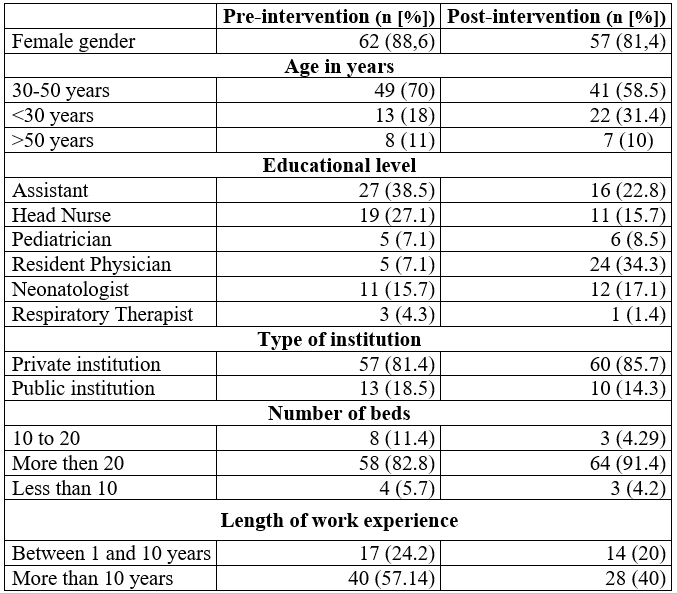
In both the pre- and post- intervention periods, participation was predominantly female, middle-aged professionals (30 to 50 years), working in private institutions with units with more than 20 newborn beds. Given the turnover of personnel in the units, the characteristics of the population at the two points in time were different in terms of profession, with a higher representation of physicians in the post-intervention period (see Table 3).
Regarding knowledge and perceptions before the educational intervention, 64.2 % of respondents stated that they agreed or strongly agreed with the statement "I have received training or training in newborn pain management"; however, only 57.1 % agreed with the statement "I record pain", and 44.2 % with "I apply a pain scale". Similarly, 78.5 % agreed with the statement "I know the non-pharmacological measures for pain management", but only 69.2 % indicated applying them. In the case of pharmacological measures, the percentages were 86.9% and 68.5%, respectively.
Tables 4 and 5 show the knowledge and skills of health personnel before and after the implementation of the educational strategy. A significant change was observed in the proportion of participants who agreed or strongly agreed with the following statements: "I know the non-pharmacological measures for pain management" (78.5 % vs. 91.3 %; p < 0.01); "Pain scales are applied in my unit" (62.8 % vs. 88.5 %; p = 0.03); "I apply a pain scale" (44.2 % vs. 72.8 %; p = 0.003); "I feel that pain in newborns is adequately managed in my unit" (34.2 % vs. 47.0 %; p < 0.001). Similarly, the degree of agreement with the statement "I use my own perception of pain instead of scales" was reduced (44,2% vs. 27%; p = 0,001).
Tabla 4
Knowledge of the surveyed population
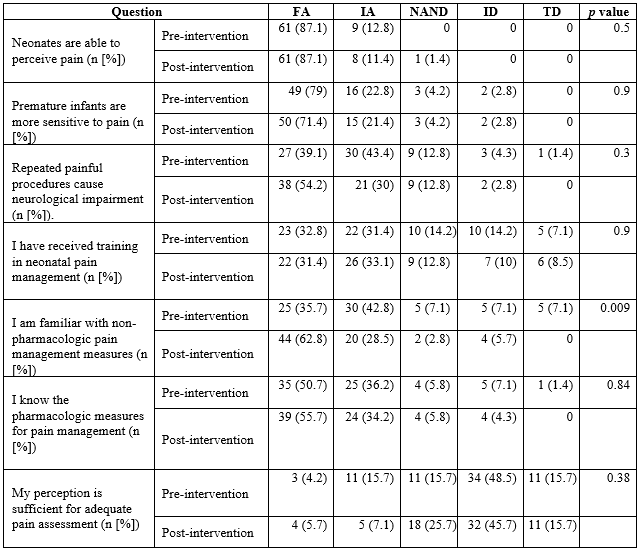
FA: fully agree; IA: in agreement; NAND: neither agree nor disagree; ID: in disagreement; TD: totally disagree.
Tabla 5
Skills of the surveyed population
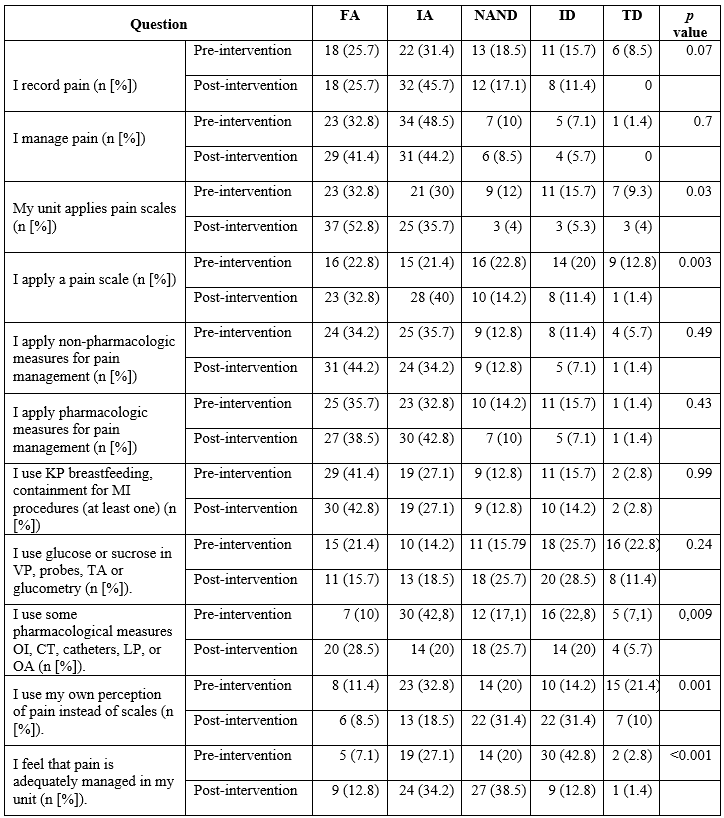
FA: fully agree; IA: in agreement; NAND: neither agree nor disagree; ID: disagreement; TD: totally disagree. PC: kangaroo position; MI: minimally invasive; VP: venipunctures; TA: tracheal aspirate; OI: orotracheal intubation; CT: chest tubes; LP: lumbar puncture; OA: ophthalmologic assessment.
When analyzing separately the groups of medical personnel, with non-medical health professionals, including nurses and therapists, it was evident that the change in the proportion of participants who agreed or strongly agreed with the following statements: "I am aware of non-pharmacological measures for pain management" (73.5 % vs. 92.8 %; p < 0.01); "Pain scales are applied in my unit" (59.2 % vs. 89.3 %; p < 0.01); "I apply a pain scale" (30.6 % vs. 60.7 %; p = 0.01), and "I feel that newborn pain is adequately managed in my unit" (36.7 % vs. 60.7 %; p = 0.04), higher among non-medical staff than among physicians, in whom the change did not reach statistical significance. Concerning the change in the degree of agreement with the statement "I use my own perception of pain instead of scales", again significance was only reached in the non-medical staff group (51.0 % vs. 28.6; p = 0.05).
Discussion
In this work, pioneer in Colombia, it was found that after developing and implementing an educational intervention strategy for health personnel working with hospitalized newborns, a significant increase in the use of pain management scales is achieved, adherence to the recording of pain in clinical histories is increased, and pharmacological measures to prevent and treat pain are used more frequently when painful procedures are performed.
In our study we found that the change was moderate in the perception of health personnel regarding the recording of pain (78.4 % vs. 85.2 % % %), in contrast to other authors (28), who reported larger changes (54.1 % vs. 78.1 %); however, the actual clinical impact when recording pain in the medical record was greater (1.3% vs. 54.4%), suggesting that the actual changes in practice may be even greater than the perception of health personnel. It was striking that the change in perceptions was greater in the non-medical staff group, possibly associated with the lower level of baseline training in nursing and therapy programs. In contrast, the physicians, since the previous period, manifested a greater knowledge and willingness to manage pain.
Regarding the use of methods (pharmacological and non-pharmacological) to relieve pain, we found a lower increase than that reported by Aymar et al. (28). Both with a higher proportion of pharmacological than non-pharmacological measures. This may be because in the three institutions where the present study was conducted, the use of oral sucrose is not established, and its availability in Colombia is limited. An alternative is to perform a daily preparation with sugar and distilled water, as is done in many neonatal units in the country, but there is a fear that this manipulation may favor infections, such as necrotizing enterocolitis of the newborn if it is not performed with the pertinent biosafety and pharmacovigilance measures.
There are also studies showing that it is also possible to use 20% or 30% glucose with doses similar to those recommended for sucrose. A systematic review of 38 studies, including 3,785 neonates, demonstrated a reduction in the score on pain scales, without side effects (29). Kangaroo position, restraint, and breastfeeding are also very important non-pharmacological measures; however, we may not have detected changes in their use since they are not recorded in the histories as measures to reduce pain.
The performance of kangaroo procedures such as venipunctures, aspirations, heel punctures, probe insertion, transfontanelar ultrasounds, ophthalmology evaluations, and echocardiograms (with inverted kangaroo), require some time for their implementation, but their benefits and safety merit their routine use. Pharmacological measures may be reserved for more invasive procedures, such as surgery, catheter insertion, lumbar puncture, insertion, or removal of thoracostomy tubes (30-32).
The data recorded in the literature are consistent with those found in this study. In our case, a higher proportion of participants consider that they record more pain, apply collectively and individually more pain scales, know more about non-pharmacological measures, use more pharmacological measures for major therapeutic pain procedures and consider that after the intervention pain is well managed in their unit; but the same does not occur with non-pharmacological measures.
In the records analyzed in the clinical histories, statistically significant differences were found, except in non-pharmacological management. The frequency of recording pain in diagnostic painful procedures before and after the intervention was higher, with an increase of more than 30% in therapeutic procedures, such as surgeries and catheter insertion, and a much smaller increase in minor procedures, such as heel punctures or venipunctures, which are the most frequent.
In pilot testing the implementation of the strategy, we found that using a pain scale that was difficult to understand or apply, with multiple items, would not achieve the necessary adherence (23-28); therefore, we preferred the PIPP scale. In the future, we could add the Comfort-Neo scale, which would evaluate very well ventilated and sedated patients at term, with acute and prolonged pain, but which requires much more experience and time, given the number of items it evaluates.
The main limitation of this study is the absence of a control group of units in which an educational strategy was not implemented; however, during the execution of this work, no measures were implemented to which the observed changes could be attributed. Additionally, a limitation is that the health personnel evaluated before and after the intervention were not exactly the same, which reflects the reality of intensive care units in Colombia, where there is a high turnover of personnel. Nevertheless, these data suggest that the benefit of interventions can be significant, even under these conditions, as long as training strategies that include new staff entering each institution are maintained, as was done in our strategy.
Conclusions
This study demonstrated that implementing an educational strategy improves sensitivity to pain management, reflected in the diagnosis and therapy applied promptly. These findings suggest that it is necessary to insist on the development of standardized protocols for pain management in each health institution, including scales that allow an objective evaluation of pain and the establishment of the appropriate therapy.
Conflict of interests
None of the authors declare any conflict of interest.
References
1. Ávila-Álvarez A, Carvajal R, Courtois E, Pertega-Díaz S, Muñiz-García J, Anand KJS. Manejo de la sedación y analgesia en las unidades de cuidados intensivos neonatales españolas. An Peditr (Barc). 2015;83(2):75-84. https://doi.org/10.1016/j.anpedi.2015.03.017
2. Committee on Fetus and Newborn and Section on Anesthesiology and Pain Medicine. Prevention and management of procedural pain in the neonate: an update. Pediatrics. 2016 Feb;137(2):e20154271. https://doi.org/10.1542/peds.2015-4271
3. The Ottawa Neonatal Pain Interest Group. Newborn pain management: a practical approach [Internet]. 2015. Available from: http://www.cmnrp.ca/uploads/documents//Newborn_Pain_SLM_2015_02_19_FINAL.pdf
4. Jeong IS, Park SM, Lee JM, Choi YJ, Lee J. Perceptions on pain management among Korean nurses in neonatal intensive care units. Asian Nurs Res (Korean Soc Nurs Sci). 2014 Dec;8(4):261-6. https://doi.org/10.1016/j.anr.2014.05.008
5. Cong X, McGrath J, Cusson R, Zhang D. (2018). Pain assessment and measurement in neonates: an updated review. Adv Neonatal Care. 2013 Dec;13(6):379-95. https://doi.org/10.1097/ANC.0b013e3182a41452
6. Christoffel MM, Castral TC, Daré MF, Montanholi LL, Scochi CG. Knowledge of healthcare professionals on the evaluation and treatment of neonatal pain. Rev Bras Enferm. 2016 Jun;69(3):552-8. English, Portuguese. https://doi.org/10.1590/0034-7167.2016690319i
7. Nimbalkar AS, Dongara AR, Phatak AG, Nimbalkar SM. Knowledge and attitudes regarding neonatal pain among nursing staff of pediatric department: an Indian experience. Pain Manag Nurs. 2014 Mar;15(1):69-75. https://doi.org/10.1016/j.pmn.2012.06.005
8. Dunbar AE 3rd, Sharek PJ, Mickas NA, Coker KL, Duncan J, McLendon D, Pagano C, Puthoff TD, Reynolds NL, Powers RJ, Johnston CC. Implementation and case-study results of potentially better practices to improve pain management of neonates. Pediatrics. 2006 Nov;118 Suppl 2:S87-94. https://doi.org/10.1542/peds.2006-0913E
9. Ozawa M, Yokoo K. Pain management of neonatal intensive care units in Japan. Acta Paediatr. 2013 Apr;102(4):366-72. https://doi.org/10.1111/apa.12160
10. Sharek PJ, Powers R, Koehn A, Anand KJ. Evaluation and development of potentially better practices to improve pain management of neonates. Pediatrics. 2006 Nov;118 Suppl 2:S78-86. https://doi.org/10.1542/peds.2006-0913D
11. Dunbar AE 3rd, Sharek PJ, Mickas NA, Coker KL, Duncan J, McLendon D, Pagano C, Puthoff TD, Reynolds NL, Powers RJ, Johnston CC. Implementation and case-study results of potentially better practices to improve pain management of neonates. Pediatrics. 2006 Nov;118 Suppl 2:S87-94. https://doi.org/10.1542/peds.2006-0913E
12. Anand KJ, Hall RW. Pain management in newborns. Clin Perinat. 2014;41 (4): 895-924.
13. Hall R, Anand KJS. Physiology of pain and stress in the newborn. Neoreviews. 2005;6;e61.
14. Anand KJ; International Evidence-Based Group for Neonatal Pain. Consensus statement for the prevention and management of pain in the newborn. Arch Pediatr Adolesc Med. 2001 Feb;155(2):173-80. https://doi.org/10.1001/archpedi.155.2.173
15. Lemus-Varela ML, Sola A, Golombek S, Baquero S, Borbonet D, Dávila-Aliaga C, et al. Consenso sobre el abordaje diagnóstico y terapéutico del dolor y el estrés en el recién nacido. Rev Panam Salud Publica. 2014; 36(5):348-54.
16. Sociedad Internacional para el Estudio del Dolor [Internet]. Available from: http://www.iasp-pain.org
17. Witt N, Coynor S, Edwards C, Bradshaw H. A Guide to Pain Assessment and Management in the Neonate. Curr Emerg Hosp Med Rep. 2016;4:1-10. https://doi.org/10.1007/s40138-016-0089-y
18. Hohmeister J, Kroll A, Wollgarten-Hadamek I, Zohsel K, Demirakça S, Flor H, Hermann C. Cerebral processing of pain in school-aged children with neonatal nociceptive input: an exploratory fMRI study. Pain. 2010 Aug;150(2):257-267. https://doi.org/10.1016/j.pain.2010.04.004
19. Mitchell A, Boss BJ. Adverse effects of pain on the nervous systems of newborns and young children: a review of the literature. J Neurosci Nurs. 2002 Oct;34(5):228-36. https://doi.org/10.1097/01376517-200210000-00002
20. van Dijk M, Roofthooft DW, Anand KJ, Guldemond F, de Graaf J, Simons S, de Jager Y, van Goudoever JB, Tibboel D. Taking up the challenge of measuring prolonged pain in (premature) neonates: the COMFORTneo scale seems promising. Clin J Pain. 2009 Sep;25(7):607-16. https://doi.org/10.1097/AJP.0b013e3181a5b52a
21. Stevens BJ, Gibbins S, Yamada J, Dionne K, Lee G, Johnston C, Taddio A. The premature infant pain profile-revised (PIPP-R): initial validation and feasibility. Clin J Pain. 2014 Mar;30(3):238-43. https://doi.org/10.1097/AJP.0b013e3182906aed
22. Taylor BJ, Robbins JM, Gold JI, Logsdon TR, Bird TM, Anand KJ. Assessing postoperative pain in neonates: a multicenter observational study. Pediatrics. 2006 Oct;118(4):e992-1000. https://doi.org/10.1542/peds.2005-3203
23. Hummel P, Puchalski M, Creech S, Weiss M. Clinical reliability and validity of the N-PASS: neonatal pain, agitation and sedation scale with prolonged pain. J Perinatol. 2018; 28(1):55-60.
24. Pölkki T, Korhonen A, Axelin A, Saarela T, Laukkala H. (2014). Development and preliminary validation of the Neonatal Infant Acute Pain Assessment Scale (NIAPAS). Int J Nurs Stud. 2014; 51(12):1585-94.
25. Lawrence J, Alcock D, McGrath P, Kay J, MacMurray SB, Dulberg C. The development of a tool to assess neonatal pain. Neonatal Netw. 1993 Sep;12(6):59-66.
26. Bordin C, Lecalire M, Demeester A. L’échelle de douleur et d’inconfort du nouveau-né (EDIN): étude de validité portant sur 160 nouveau-nés en maternité entre quatre et 12 heures de vie. La Revue Sage-Femme. 2012;11(3):120-7.
27. Villamil González AL, Ríos Gutiérrez MM, Bello Pacheco MS, López Soto NC, Pabón Sánchez IC. Valoración del dolor neonatal: una experiencia clínica. Aquichan [Internet]. 2009 [cited 2022 ago 2];7(2). Available from: https://aquichan.unisabana.edu.co/index.php/aquichan/article/view/107
28. Aymar CL, Lima LS, Santos CM, Moreno EA, Coutinho SB. Pain assessment and management in the NICU: analysis of an educational intervention for health professionals. J Pediatr (Rio J). 2014 May-Jun;90(3):308-15. https://doi.org/10.1016/j.jped.2013.09.008
29. Bueno M, Yamada J, Harrison D. A systematic review and meta-analyses of nonsucrose sweet solutions for pain relief in neonates. Pain Res Manag. 2013;18(3):153-61.
30. Choudhary M, Dogiyal H, Sharma D, Datt Gupta B, Madabhavi I, Choudhary JS, Choudhary SK. To study the effect of Kangaroo Mother Care on pain response in preterm neonates and to determine the behavioral and physiological responses to painful stimuli in preterm neonates: a study from western Rajasthan. J Matern Fetal Neonatal Med. 2016 Mar;29(5):826-31. https://doi.org/10.3109/14767058.2015.1020419
31. Lefrak L, Burch K, Caravantes B. Sucrose analgesia: identifying potentially better practices. Pediatrics. 2006;118(suppl. 2):S197-S202.
32. Harrison D, Reszel J, Bueno M, Sampson M, Shah VS, Taddio A, Larocque C, Turner L. Breastfeeding for procedural pain in infants beyond the neonatal period. Cochrane Database Syst Rev. 2016 Oct 28;10(10):CD011248. https://doi.org/10.1002/14651858.CD011248.pub2
Annex. Survey conducted among professionals
A. Population
2. Age
-
Under 30 years
-
30-50 years
-
Older than 50 years
3. Educational level
-
Neonatologist
-
Pediatrician
-
Resident physician
-
General Practitioner
-
Head nurse
-
Nursing assistant
-
Respiratory therapist
4. Nature of the institution where you work
-
Public
-
Private
5. Number of inpatient beds in your unit
-
Less than 10 beds
-
10 to 20 beds
-
More than 20 beds
6. Time of experience in neonatal care
-
Less than five years
Answer the statements of items B and C with one of the following options
-
1 = Strongly agree
-
2 = Agree
-
3 = Neither agree nor disagree
-
4 = Disagree
-
5 = Strongly disagree
B. Pain knowledge and practices
-
7. Neonates are able to perceive pain.
-
8. Premature infants are more sensitive to pain.
-
9. Repeated painful procedures cause neurological deterioration.
-
10. I have received training in newborn pain management.
-
11. Pain recording and management.
-
12. Pain scales are applied in my unit.
-
13. I apply a pain scale.
-
14. I know and apply pharmacological measures for pain management.
-
15. I know and apply non-pharmacological pain management measures.
-
16. I use the kangaroo position, breastfeeding, restraint for minimally invasive procedures.
-
17. I use glucose or sucrose for venipunctures, probing, tracheal suctioning or glucometry.
-
18. I use any pharmacological measure for orotracheal intubation, chest tubes, catheter insertion, lumbar puncture, or ophthalmologic assessment.
-
19. I use my own perception of pain rather than scales.
-
20. My perception is sufficient for an adequate assessment of pain.
-
21. I feel that my unit adequately manages newborn pain.
C. Intervention
-
22. I would like to receive group training
-
23. I would like to receive individual training
-
24. I would like to receive an incentive for applying the pain protocol
-
25. I would like to see a pain management leadership group in our unit.
-
26. I would like to have observations in our unit and then feedback.
Author notes
a Correspondence author: claudevia1@hotmail.com
Additional information
How to cite: Devia Neira CP, Atencia Herrera CM, Lonngi G, Muñoz Velandia OM. Educational intervention to improve the diagnosis and management of pain in newborn units in Colombia. Univ. Med. 2022;63(3). https://doi.org/10.11144/Javeriana.umed63-2.eiep