Introduction
Obstructive sleep apnea-hypopnea syndrome (OSAHS) refers to the set of signs and symptoms that accompany recurrent episodes of limited or decreased airflow during sleep, resulting from a functional anatomical alteration of the upper airway (VAS) (1). This disease has become an important public health problem in industrialized countries due to its significant morbimortality since it generates high health costs due to its association with other diseases such as arterial hypertension, diabetes mellitus, and depression. All of the above increases the risk of cardiovascular diseases such as myocardial infarction and stroke (1,2).
Although in Colombia the prevalence of this disease is not known exactly, data obtained from a meta-analysis published in Sleep Medicine Reviews, 2016, based on polysomnographic findings, indicate that in the general adult population it is between 6% and 17% and increases with age; moreover, it is higher in obese men and postmenopausal women (1). However, the overall prevalence of respiratory sleep disorders is 24% in men and 9% in women, and the prevalence of OSAHS is 4% in men and 2% in women. (3).
Assessing the site, extent, and severity of the obstructive event in the sleeping patient is a clinical challenge, given the difficulties in adequately measuring the pharynx, mostly due to morphometric changes due to the individual's position, respiration, and state of consciousness (4). Accurate location of the site(s) of obstruction is essential to achieve satisfactory success rates in treatment but is limited because the examination is performed on awake subjects (5).
Although drug-induced sleep endoscopy (DISE) allows for a comprehensive and specific evaluation of pharyngeal obstruction in the sleeping patient, there is limited data correlating the area of obstruction with each type of patient, taking into account age, gender, body mass index (BMI), apnea and hypopnea index (AHI), and the Epworth scale score. Hence, knowing the areas of airway obstruction in detail and predicting mandibular movements during sleep according to each patient individualizes each case and focuses the type of treatment for each patient, especially in those who cannot tolerate continuous positive airway pressure and in whom other surgical techniques or other treatments have failed.
The objective of the study was to identify the most affected areas of obstruction, associating them with the clinical characteristics of each patient, and thus establish possible causes of OSAHS, relating them to the need for a surgical or non-surgical treatment plan based on the effectiveness of the maneuvers during the examination. It was decided to perform it at the Hospital San Ignacio (HUSI), because it is one of the few Colombian institutions that performs this test, which, in addition to predicting airway collapse, also predicts the effect of mandibular advancement in any type of obstruction.
Materials and methods
Subject to the approval of the Research and Ethics Committee of the Faculty of Dentistry of the Pontificia Universidad Javeriana and the HUS), a retrospective descriptive study was conducted, reviewing a total of 110 medical records of patients with a diagnosis of OSAHS who had attended the Otolaryngology and Maxillofacial Surgery unit between 2017 and 2020. Medical records of patients older than 18 years with AHI result according to polysomnography greater than 5, with obstructive component and DISE examination were included. Patient histories with central-type apnea and histories that did not have complete data on the variables to be evaluated were excluded. Data were recorded in Microsoft Excel® as age range, gender, BMI, Epworth score, AHI, surgical history in the VAS, sedative agent, improvement to the Esmarch maneuver and chin elevation, degree and direction of obstruction of the velopharynx, oropharynx, the base of the tongue, epiglottis, and adverse effects. Subsequently, they analyzed variables that identified the site, degree, and direction of obstruction; severity of apnea; BMI; Epworth score; effectiveness of Esmarch maneuvers; and chin lift, by gender and age range, in addition to findings associated with the sedative agent and adverse effects.
Results
We reviewed 110 medical records of adult patients with a diagnosis of OSAHS who underwent DISE. Nineteen patients were discarded due to data not reported in the clinical history, and 2 patients were discarded due to a diagnosis of Down syndrome, for whom the Epworth scale was not performed because of their neurological function. A total of 89 patients were included in the study: 64 males (71.91%) and 25 females (28.09%) with a mean age of 47.71 years. The distribution of age ranges, the severity of OSAHS, Epworth score, and BMI of the study population can be seen in Figures 1 to 4. The summary of demographic characteristics is shown in Table 1.
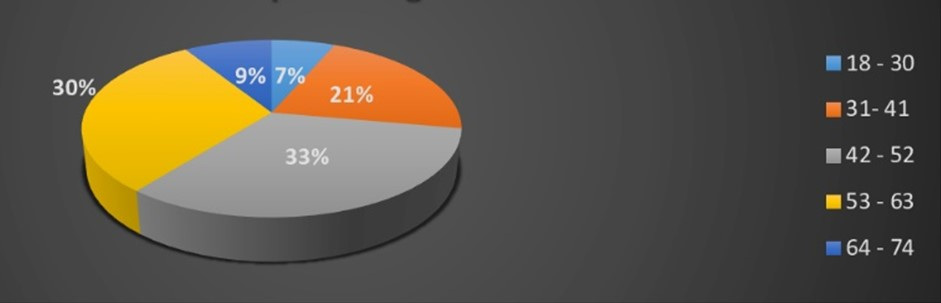 Figure 1.
Distribution by age ranges
Figure 1.
Distribution by age ranges
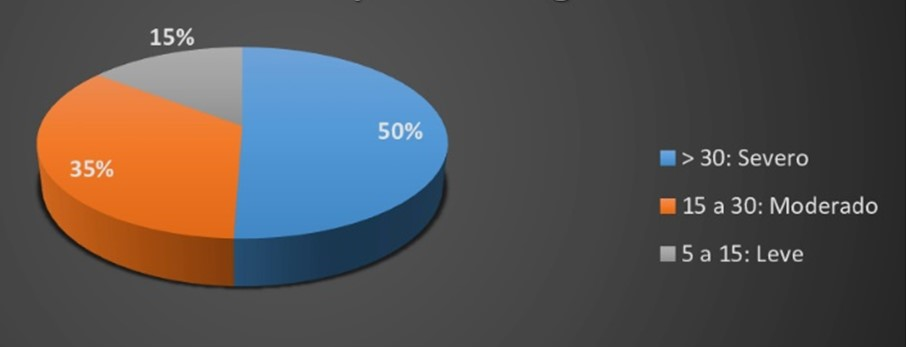 Figure 2.
Distribution of the apnea and hypopnea index
Figure 2.
Distribution of the apnea and hypopnea index
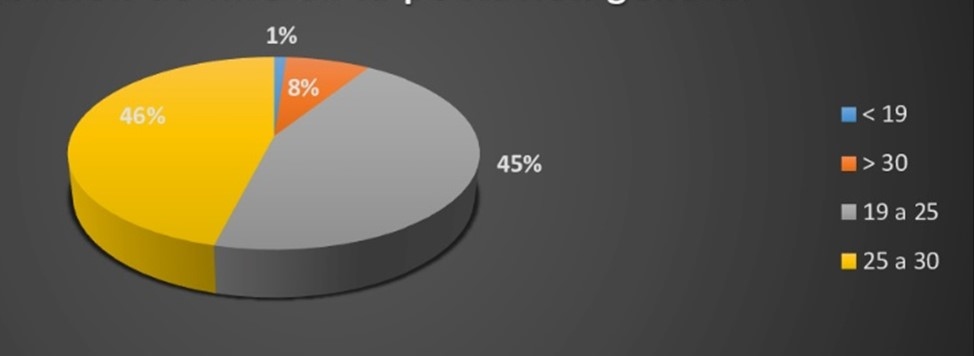 Figure 3.
Distribution of the body mass index
Figure 3.
Distribution of the body mass index
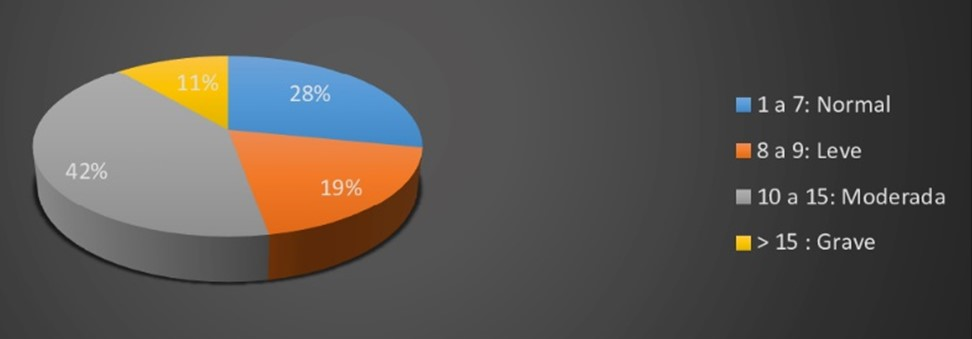 Figure 4.
Distribution of the Epworth scale
Figure 4.
Distribution of the Epworth scale
Tabla 1.
Demographic characteristics
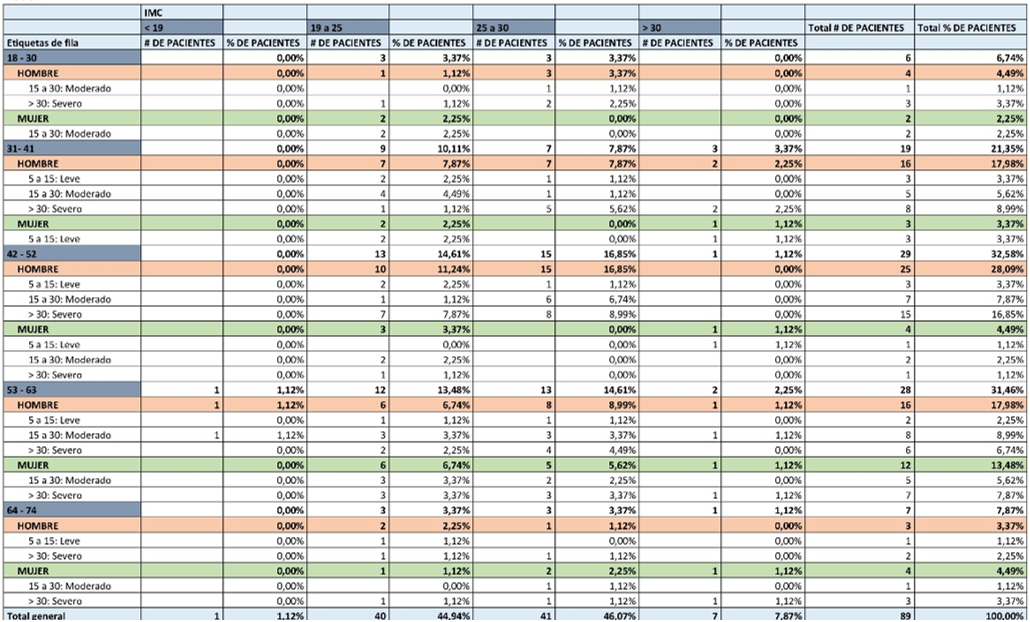
Evaluation of the degree and direction of obstruction
According to the VOTE classification, in the velopharynx, 83.15% presented an obstruction greater than 75%, although it is greater in the anteroposterior direction in men and the concentric direction in women (Figure 5).
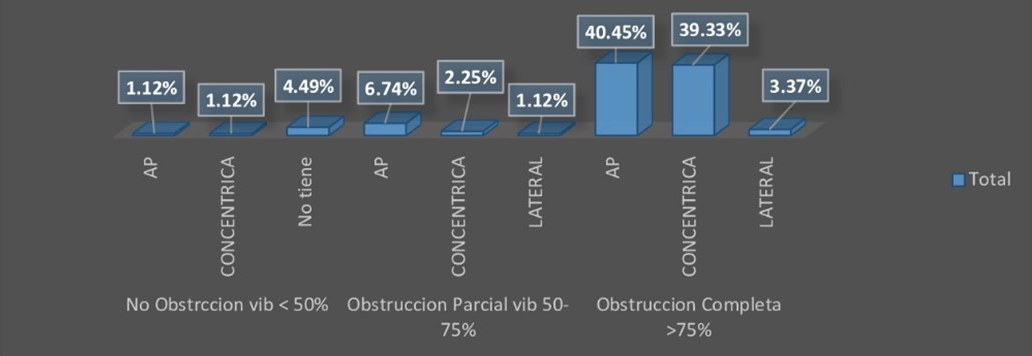 Figure 5.
Distribution of the degree and direction of obstruction in the velopharynx
Figure 5.
Distribution of the degree and direction of obstruction in the velopharynx
In the oropharynx, the majority of patients between 53 and 63 years of age presented an obstruction of less than 50%. There was no obstruction at all when evaluating the direction in 37 patients and lateral obstruction in 8 (Figure 6).
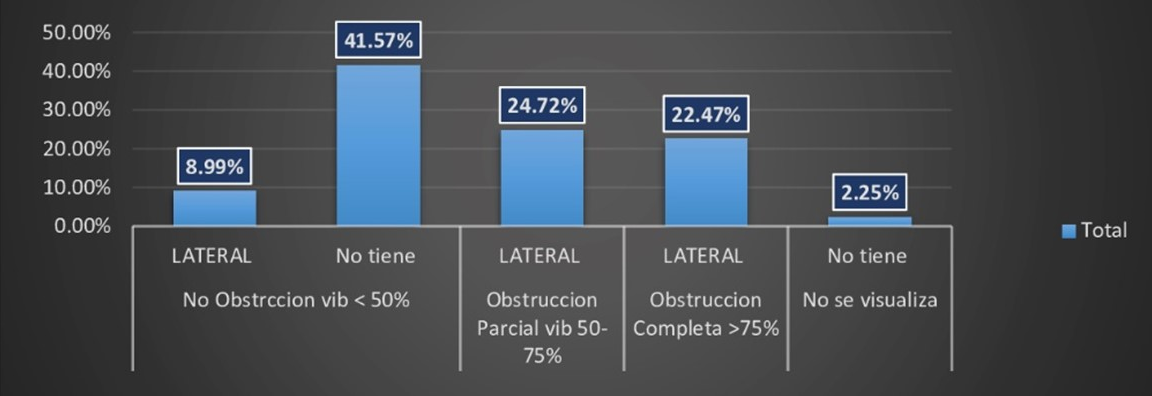 Figure 6.
Distribution of the degree and direction of obstruction in the oropharynx
Figure 6.
Distribution of the degree and direction of obstruction in the oropharynx
At the base of the tongue, the degree of obstruction in the general population was less than 50% in the anteroposterior direction, for a total of 37.08%. There was partial obstruction in 32.08% of the patients, mainly in women, and complete obstruction in 30.34% of the cases (Figure 7).
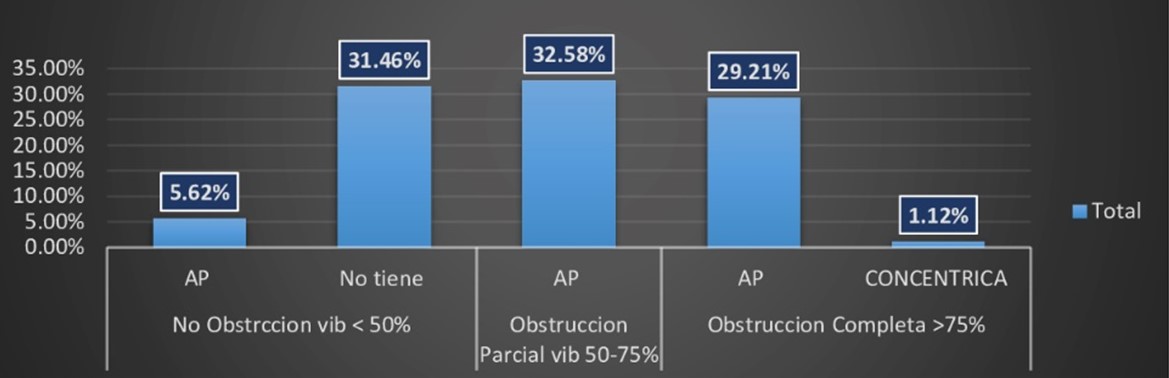 Figure 7.
Distribution and degree of the direction of obstruction at the base of the tongue
Figure 7.
Distribution and degree of the direction of obstruction at the base of the tongue
88.46% of the patients had no obstruction in the epiglottis, followed by 7.69% who presented partial obstruction in the lateral direction (Figure 8).
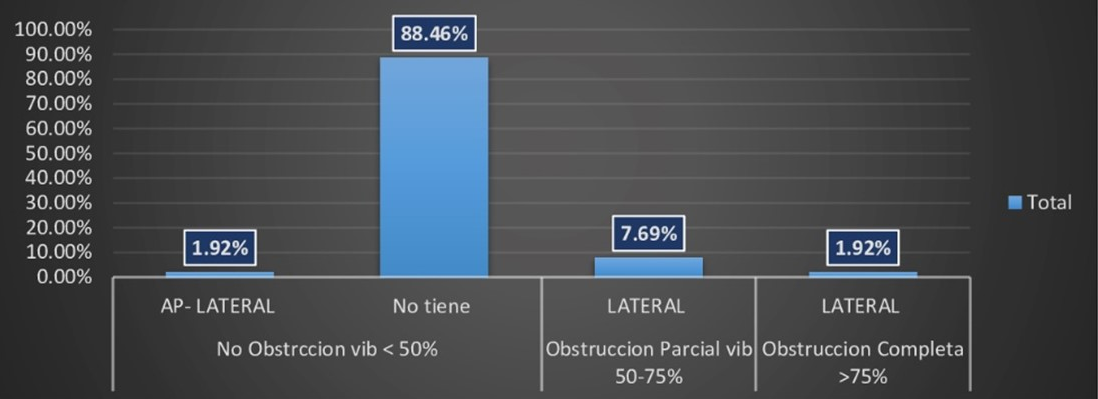 Figure 8.
Distribution and degree of the direction of obstruction in the epiglottis
Figure 8.
Distribution and degree of the direction of obstruction in the epiglottis
Effectiveness of maneuvers during drug-induced sleep
The Esmarch maneuver proved to be effective in 91.01% of the general population: 100% in women and 87.5% in men, in all age ranges. Men in whom this maneuver was not effective presented an obstruction greater than 75% in the velopharynx and between 50% and 70% in the oropharynx and at the base of the tongue.
Some improvement was evidenced by performing the Esmarch maneuver in all patients with BMI < 19 to > 30; however, in proportion and concerning the number of patients, one (14.29%) out of 7 patients with BMI > 30 did not report improvement, which predisposes to the ineffectiveness of the Esmarch maneuver in patients with obesity (Figure 9).
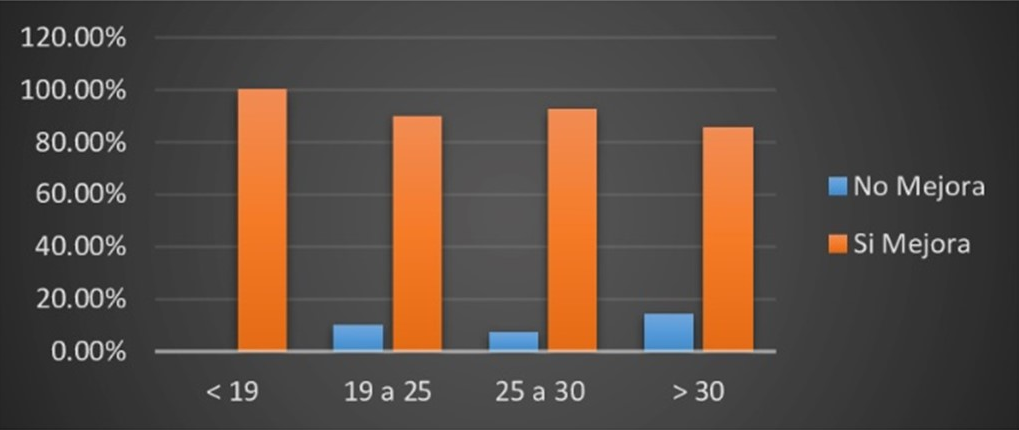 Figure 9.
Effectiveness of the Esmarch maneuver concerning the body mass index
Figure 9.
Effectiveness of the Esmarch maneuver concerning the body mass index
Results of the chin lift maneuver
The chin lift maneuver reported effectiveness of 86.52% in the general population analyzed. Patients who did not show improvement, in turn, did not show improvement compared to the Esmarch maneuver, with >75% obstruction in the velopharynx and >50% obstruction in the oropharynx. Likewise, the chin lift maneuver reported effectiveness in the great majority of patients, but in patients with a BMI > 30, a total of 2 patients (28.57%) reported no improvement. This leads to the conclusion that BMI is related to the effectiveness of the maneuvers (Figure 10).
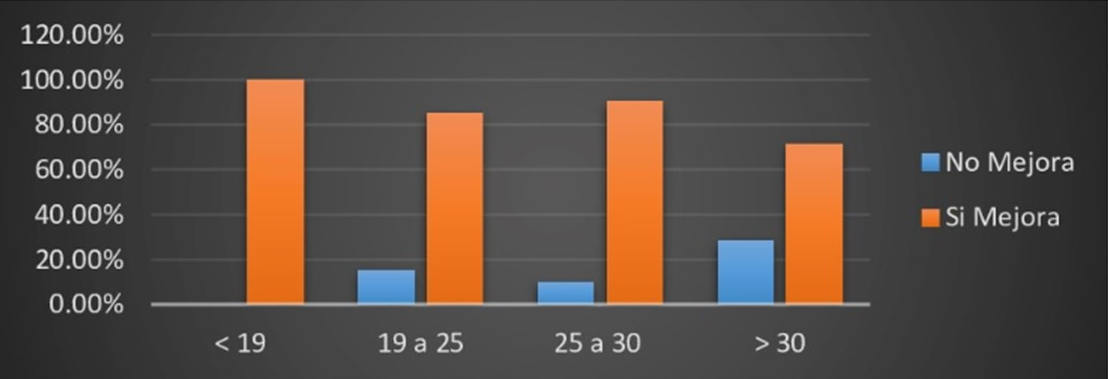 Figure 10.
Effectiveness of the chin lift maneuver regarding body mass index
Figure 10.
Effectiveness of the chin lift maneuver regarding body mass index
The Esmarch maneuver and the chin lift maneuver were effective regardless of the surgical history and the sedative agent used.
A total of 51 (57.3%) patients had adverse effects, ranging in age from 42 to 52 years. Of these, 49 had desaturation <80% with any type of sedative agent. As a finding, the most commonly used sedative agent was propofol. One of the women sedated with propofol presented, in addition to desaturation of less than 80%, aspiration symptoms and sphincter relaxation. On the other hand, a 37-year-old man became aggressive during sedation with propofol. The use of the latter, together with another sedative agent, is associated with the occurrence of arrhythmias.
A total of 6 patients (11.76%) with obesity presented desaturation <80%, as did 24 patients (47.06%).
Discussion
Our study showed a higher prevalence of OSAHS in men in an age range of 42 to 52 years, similar to that reported in the literature. This shows that OSAHS is higher in men than in women with an age prevalence of 30 to 69 years, without excepting that it can occur in older population groups and that postmenopausal and obese women are at higher risk (6,3).
Risk factors such as BMI and age are highly significant and play an important role in the severity of sleep apnea, as well as in DISE since overweight and obese patients are susceptible to adverse effects during this test. In this study, a total of 7 patients presented with obesity, and of these, 3 (2 women and 1 man) had moderate to severe AHI, using BMI as a reference. Although in this population, sleep disorders may be related to medications, chronic diseases, physical and mental conditions, and lifestyle, in this group of patients BMI cannot be used as a reference due to the loss of muscle mass and weight, so it is recommended to use neck circumference or a waist-hip ratio (6).
In an article by Lee et al. (7), 2017, BMI was shown to be a risk factor because it is a strong indicator of complications with cardiovascular diseases and increased cases of OSAHS, especially in middle-aged people. Likewise, in patients with a high BMI, body fat in the ASV increases, which decreases airway amplitude and causes apneas. Based on the above, in our study, it was observed that overweight and obesity increase the risk of obstruction in high anatomical areas, such as the velopharynx and oropharynx; in addition, this type of patients were susceptible to present adverse effects during DISE. However, although the vast majority of patients with OSAHS are obese, not all obese patients have OSAHS (8).
Data from a Wisconsin cohort study aimed at determining the natural history of cardiopulmonary effects of sleep breathing disorders and its prevalence indicate that one standard deviation in BMI gain is associated with a 4- to 5-fold increase in the risk of sleep breathing disorders and that each percent change in weight is associated with an approximate mean change in AHI of 3% (9).
Complete collapse of the pharyngeal walls is strongly associated with disease severity in patients with obstructive sleep apnea. The most frequent area of collapse of the ASV is the velopharyngeal sphincter (10), and although this is not the only area of obstruction, since the base of the tongue can play a prominent role and in many cases even be associated with multilevel obstruction, this is due to the absence of an osteocartilaginous support that makes it an easily collapsible area (10).
In this study, there were a total of 6 patients with >75% obstruction in all four areas evaluated, mostly men with a BMI of 25 to 30, with a moderate Epworth scale score and moderate AHI. All improved with the Esmarch maneuver and chin elevation, and in patients where the Esmarch maneuver was not effective, 100% presented obstruction >75% in the velopharynx, 75% obstruction >50% in the oropharynx, and 62% of patients had obstruction >50% at the base of the tongue. This shows that the effectiveness of the maneuvers is not related to the degree of airway obstruction.
Although the awake patient is useful for assessing any anatomic variations in upper airway structures, this assessment is less useful for predicting the soft tissue collapse of the ASV that occurs during sleep (11). DISE, unlike polysomnography, allows direct clinical visualization of the degree of airway collapse during sleep, so it has been generally accepted as an important part of the preoperative evaluation in patients with OSAHS, as it determines the impact of mandibular advancement maneuvers and thus predicts the success of surgical treatments and mandibular advancement appliances. This is also part of the postoperative evaluation, which assesses the degree of stability of the lateral pharyngeal walls and residual sites of obstruction (12,13).
The most commonly used sedative agents documented in the literature include midazolam, propofol, and dexmedetomidine. In a study by Charakorn and Kesirian, cited in the article by Chong et al. (11), propofol sedation decreases genioglossus muscle tone and increases upper airway collapsibility in a deeper sedation, which may result in inaccuracies in assessment. Therefore, electroencephalographic parameters processed as a bispectral index should be taken into account. At HUSI, the most commonly used drug was propofol, because has a rapid onset of action, a short half-life, and a rapid reversal of sedation. Most of the sedated patients presented as adverse effect desaturation <80 and the combination of propofol plus another sedative agent was associated with the presentation of arrhythmias.
However, prospective studies comparing the use of different anesthetic techniques for DISE are lacking, so the choice of sedative agent will depend on institutional preference (14).
Conclusions
The study proved that male gender and middle age is the population most affected by OSAHS, as well as the most collapsed site of the ASV is the velopharynx, according to the literature, with an obstruction >75% in this area, reported in our study. Obesity and overweight have been considered important factors, since they increase the risk of obstruction in the upper anatomical areas (velopharynx and oropharynx), which also predisposes to adverse effects during the examination and the ineffectiveness of the maneuvers during the examination.
Both the Esmarch maneuver and the chin lift maneuver improve obstruction in the vast majority of patients, and in all age ranges. They also mimic the effect of mandibular repositioning, so that DISE, in addition to being a supplementary diagnostic test to polysomnography (considered the gold standard), can predict the likelihood of effectiveness of both a mandibular advancement appliance and maxillomandibular advancement surgical procedures (15).
DISE is considered to be very useful because, unlike polysomnography, it allows direct clinical visualization of the sites of obstruction in a sleep-like state; therefore, it should be used to individualize treatments according to the clinical characteristics of each patient. However, it should be noted that the risks and complications that can occur during the procedure range from rapid oxygen desaturation, allergic reactions associated with sedatives, epistaxis due to trauma to the nasal mucosa, bradycardia, hypotension, and oversedation. This test is contraindicated in those patients with ASA 4 anesthetic risks and pregnant women, so they should be taken for pre-anesthetic assessment. Consequently, its use and protocol should be standardized.
Conflict of interests
The authors declare that they have no conflict of interest with the pharmaceutical industry.