1. Hughes JP, Baron R, Buckland DH, Cooke MA, Craig JD, Duffield DP, Grosart AW, Parkes PW, Porter A. Phosphorus necrosis of the jaw: a present-day study. Br J Ind Med. 1962 Apr; 19(2): 83-99. http://doi.org/10.1136/oem.19.2.83
2. Marx RE. Pamidronate (Aredia) and zoledronate (Zometa) induced avascular necrosis of the jaws: a growing epidemic. J Oral Maxillofac Surg. 2003 Sep; 61(9): 1115-1117. http://doi.org/10.1016/s0278-2391(03)00720-1
3. Regaud C. Sur la necrose des os atteints par un processus cancereux et traites par les radiations. Compt Rend Soc Biol. 1922; 87: 427-629.
4. Ewing J. Radiation osteitis. Acta Radiol. 1926; 6(1-6): 399-412. https://doi.org/10.3109/00016922609139503
5. Kanthak FF. X-Ray irradiation and osteonecrosis of the jaws. J Am Dent Assoc. 1941; 28(12): 1925-1929. https://doi.org/10.14219/jada.archive.1941.0301
6. Marx RE. Osteoradionecrosis: A new concept of its pathophysiology. J Oral Maxillofac Surg. 1983; 41(5): 283-288. https://doi.org/10.1016/0278-2391(83)90294-X
7. Ruggiero SL, Dodson TB, Fantasia J, Goodday R, Aghaloo T, Mehrotra B, O'Ryan F, American Association of Oral and Maxillofacial Surgeons. American Association of Oral and Maxillofacial Surgeons position paper on medication-related osteonecrosis of the jaw-2014 update. J Oral Maxillofac Surg. 2014 Oct; 72(10): 1938-1956. https://doi.org/10.1016/j.joms.2014.04.031
8. Ng EW, Adamis AP. Targeting angiogenesis, the underlying disorder in neovascular age-related macular degeneration. Can J Ophthalmol. 2005 Jun; 40(3): 352-368. https://doi.org/10.1016/S0008-4182(05)80078-X
9. llahi M. Long term bisphosphonate use in osteoporotic patients; a step forward, two steps back. J Pharm Pharmaceut Sci. 2012 15(2): 305. https://doi.org/10.18433/J3RK5J
10. Allen MR, Ruggiero SL. Higher bone matrix density exists in only a subset of patients with bisphosphonate-related osteonecrosis of the jaw. J Oral Maxillofac Surg. 2009 Jul; 67(7): 1373-1377. https://doi.org/10.1016/j.joms.2009.03.048
11. Migliorati CA, Brennan MT, Peterson DE. Medication-related osteonecrosis of the jaws. J Natl Cancer Inst Monogr. 2019 Aug 1; 2019(53): lgz009. https://doi.org/10.1093/jncimonographs/lgz009
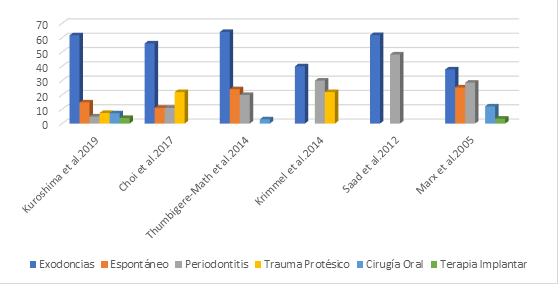
12. Choi WS, Lee JI, Yoon HJ, Min CK, Lee SH. Medication-related osteonecrosis of the jaw: a preliminary retrospective study of 130 patients with multiple myeloma. Maxillofac Plast Reconstr Surg. 2017 Jan 5; 39(1): 1. https://doi.org/10.1186/s40902-016-0099-4
13. MedlinePlus. Inyección de Denosumab. Washington, DC: Biblioteca Nacional de Medicina; 2019 ago 18. https://medlineplus.gov/spanish/druginfo/meds/a610023-es.html
14. Wang Y, Fei D, Vanderlaan M, Song A. Biological activity of bevacizumab, a humanized anti-VEGF antibody in vitro. Angiogénesis. 2004; 7(4): 335-345. https://doi.org/10.1007/s10456-004-8272-2
15. Fujita K, Sano D, Kimura M, Yamashita Y, Kawakami M, Ishiguro Y, Nishimura G, Matsuda H, Tsukuda M. Anti-tumor effects of bevacizumab in combination with paclitaxel on head and neck squamous cell carcinoma. Oncol Rep. 2007 Jul; 18(1): 47-51.
16. Chung BL, Toth MJ, Kamaly N, Sei YJ, Becraft J, Mulder WJ, Fayad ZA, Farokhzad OC, Kim Y, Langer R. Nanomedicines for endothelial disorders. Nano Today. 2015 Dec 1; 10(6): 759-776. https://doi.org/10.1016/j.nantod.2015.11.009
17. Ruggiero SL, Fantasia J, Carlson E. Bisphosphonate-related osteonecrosis of the jaw: background and guidelines for diagnosis, staging and management. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006 Oct; 102(4): 433-441. https://doi.org/10.1016/j.tripleo.2006.06.004
18. Sarin J, DeRossi SS, Akintoye SO. Updates on bisphosphonates and potential pathobiology of bisphosphonate-induced jaw osteonecrosis. Oral Dis. 2008 Apr; 14(3): 277-285. https://doi.org/10.1111/j.1601-0825.2007.01381.x
19. Peer A, Khamaisi M. Diabetes as a risk factor for medication-related osteonecrosis of the jaw. J Dent Res. 2015 Feb; 94(2): 252-260. https://doi.org/10.1177/0022034514560768
20. Chang J, Hakam AE, McCauley LK. Current understanding of the pathophysiology of osteonecrosis of the jaw. Curr Osteoporos Rep. 2018 Oct; 16(5): 584-595. https://doi.org/10.1007/s11914-018-0474-4
21. Khan AA, Morrison A, Hanley DA, Felsenberg D, McCauley LK, O'Ryan F, Reid IR, Ruggiero SL, Taguchi A, Tetradis S, Watts NB, Brandi ML, Peters E, Guise T, Eastell R, Cheung AM, Morin SN, Masri B, Cooper C, Morgan SL, Obermayer-Pietsch B, Langdahl BL, Al Dabagh R, Davison KS, Kendler DL, Sándor GK, Josse RG, Bhandari M, El Rabbany M, Pierroz DD, Sulimani R, Saunders DP, Brown JP, Compston J; International Task Force on Osteonecrosis of the Jaw. Diagnosis and management of osteonecrosis of the jaw: a systematic review and international consensus. J Bone Miner Res. 2015 Jan; 30(1): 3-23. https://doi.org/10.1002/jbmr.2405
22. Sedghizadeh PP, Kumar SK, Gorur A, Schaudinn C, Shuler CF, Costerton JW. Identification of microbial biofilms in osteonecrosis of the jaws secondary to bisphosphonate therapy. J Oral Maxillofac Surg. 2008 Apr; 66(4): 767-775. https://doi.org/10.1016/j.joms.2007.11.035
23. Sedghizadeh PP, Kumar SK, Gorur A, Schaudinn C, Shuler CF, Costerton JW. Microbial biofilms in osteomyelitis of the jaw and osteonecrosis of the jaw secondary to bisphosphonate therapy. J Am Dent Assoc. 2009 Oct; 140(10): 1259-1265. https://doi.org/10.14219/jada.archive.2009.0049
24. Kumar SK, Gorur A, Schaudinn C, Shuler CF, Costerton JW, Sedghizadeh PP. The role of microbial biofilms in osteonecrosis of the jaw associated with bisphosphonate therapy. Curr Osteoporos Rep. 2010 Mar; 8(1):40-8. https://doi.org/10.1007/s11914-010-0008-1
25. Kalyan S, Wang J, Quabius ES, Huck J, Wiltfang J, Baines JF, Kabelitz D. Systemic immunity shapes the oral microbiome and susceptibility to bisphosphonate-associated osteonecrosis of the jaw. J Transl Med. 2015 Jul 4; 13: 212. https://doi.org/10.1186/s12967-015-0568-z
26. Krimmel M, Ripperger J, Hairass M, Hoefert S, Kluba S, Reinert S. Does dental and oral health influence the development and course of bisphosphonate-related osteonecrosis of the jaws (BRONJ)? Oral Maxillofac Surg. 2014 Jun; 18(2): 213-218. https://doi.org/10.1007/s10006-013-0408-3
27. Khosla S, Burr D, Cauley J, Dempster DW, Ebeling PR, Felsenberg D, Gagel RF, Gilsanz V, Guise T, Koka S, McCauley LK, McGowan J, McKee MD, Mohla S, Pendrys DG, Raisz LG, Ruggiero SL, Shafer DM, Shum L, Silverman SL, Van Poznak CH, Watts N, Woo SB, Shane E; American Society for Bone and Mineral Research. Bisphosphonate-associated osteonecrosis of the jaw: report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res. 2007 Oct; 22(10): 1479-1491. https://doi.org/10.1359/jbmr.0707onj
28. Khan A, Morrison A, Cheung A, Hashem W, Compston J. Osteonecrosis of the jaw (ONJ): diagnosis and management in 2015. Osteoporos Int. 2016 Mar; 27(3): 853-859. https://doi.org/10.1007/s00198-015-3335-3
29. Ruggiero SL. Diagnosis and staging of medication-related osteonecrosis of the jaw. Oral Maxillofac Surg Clin North Am. 2015 Nov; 27(4): 479-487. https://doi.org/10.1016/j.coms.2015.06.008
30. Marx RE, Sawatari Y, Fortin M, Broumand V. Bisphosphonate-induced exposed bone (osteonecrosis/osteopetrosis) of the jaws: risk factors, recognition, prevention, and treatment. J Oral Maxillofac Surg. 2005 Nov; 63(11): 1567-1575. https://doi.org/10.1016/j.joms.2005.07.010
31. Khamaisi M, Regev E, Yarom N, Avni B, Leitersdorf E, Raz I, Elad S. Possible association between diabetes and bisphosphonate-related jaw osteonecrosis. J Clin Endocrinol Metab. 2007 Mar; 92(3): 1172-1175. https://doi.org/10.1210/jc.2006-2036
32. Junquera LM, Martín-Granizo R. Diagnóstico, prevención y tratamiento de la osteonecrosis de los maxilares por bisfosfonatos: Recomendaciones de la Sociedad Española de Cirugía Oral y Maxilofacial (SECOM). Rev Esp Cirug Oral Maxilofac. 2008 jun; 30(3): 145-156.
33. Kuroshima S, Sasaki M, Sawase T. Medication-related osteonecrosis of the jaw: A literature review. J Oral Biosci. 2019 Jun; 61(2): 99-104. https://doi.org/10.1016/j.job.2019.03.005
34. Yamazaki T, Yamori M, Ishizaki T, Asai K, Goto K, Takahashi K, Nakayama T, Bessho K. Increased incidence of osteonecrosis of the jaw after tooth extraction in patients treated with bisphosphonates: a cohort study. Int J Oral Maxillofac Surg. 2012 Nov; 41(11): 1397-1403. https://doi.org/10.1016/j.ijom.2012.06.020
35. Thumbigere-Math V, Michalowicz BS, Hodges JS, Tsai ML, Swenson KK, Rockwell L, Gopalakrishnan R. Periodontal disease as a risk factor for bisphosphonate-related osteonecrosis of the jaw. J Periodontol. 2014 Feb; 85(2): 226-233. https://doi.org/10.1902/jop.2013.130017
36. Choi WS, Lee JI, Yoon HJ, Min CK, Lee SH. Medication-related osteonecrosis of the jaw: a preliminary retrospective study of 130 patients with multiple myeloma. Maxillofac Plast Reconstr Surg. 2017 Jan 5; 39(1): 1. https://doi.org/10.1186/s40902-016-0099-4
37. Saad F, Brown JE, Van Poznak C, Ibrahim T, Stemmer SM, Stopeck AT, Diel IJ, Takahashi S, Shore N, Henry DH, Barrios CH, Facon T, Senecal F, Fizazi K, Zhou L, Daniels A, Carrière P, Dansey R. Incidence, risk factors, and outcomes of osteonecrosis of the jaw: integrated analysis from three blinded active-controlled phase III trials in cancer patients with bone metastases. Ann Oncol. 2012 May; 23(5): 1341-1347. https://doi.org/10.1093/annonc/mdr435
38. Saad F, Brown JE, Van Poznak C, Ibrahim T, Stemmer SM, Stopeck AT, Diel IJ, Takahashi S, Shore N, Henry DH, Barrios CH, Facon T, Senecal F, Fizazi K, Zhou L, Daniels A, Carrière P, Dansey R. Incidence, risk factors, and outcomes of osteonecrosis of the jaw: integrated analysis from three blinded active-controlled phase III trials in cancer patients with bone metastases. Ann Oncol. 2012 May; 23(5): 1341-1347. https://doi.org/10.1093/annonc/mdr435
39. Dodson TB. The Frequency of medication-related osteonecrosis of the jaw and its associated risk factors. Oral Maxillofac Surg Clin North Am. 2015 Nov; 27(4): 509-516. https://doi.org/10.1016/j.coms.2015.06.003
40. Boquete-Castro A, Gómez-Moreno G, Calvo-Guirado JL, Aguilar-Salvatierra A, Delgado-Ruiz RA. Denosumab and osteonecrosis of the jaw. A systematic analysis of events reported in clinical trials. Clin Oral Implants Res. 2016 Mar; 27(3): 367-375. https://doi.org/10.1111/clr.12556
41. Nicolatou-Galitis O, Schiødt M, Mendes RA, Ripamonti C, Hope S, Drudge-Coates L, Niepel D, Van den Wyngaert T. Medication-related osteonecrosis of the jaw: definition and best practice for prevention, diagnosis, and treatment. Oral Surg Oral Med Oral Pathol Oral Radiol. 2019 Feb; 127(2): 117-135. https://doi.org/10.1016/j.oooo.2018.09.008
42. Ünsal G, Orhan K, What do we expect to visualize on the radiographs of mronj patients? J Exp Clin Med 2021; 38(S2): 98-103 https://doi.org/10.52142/omujecm.38.si.dent.4
43. Advisory Task Force on Bisphosphonate-Related Osteonecrosis of the Jaws. American Association of Oral and Maxillofacial Surgeons position paper on bisphosphonate-related osteonecrosis of the jaws. J Oral Maxillofac Surg. 2007; 65:369-376. https://doi.org/10.1016/j.joms.2006.11.003
44. Ripamonti CI, Maniezzo M, Campa T, et al. Decreased occurrence of osteonecrosis of the jaw after implementation of dental preventive measures in solid tumor patients with bone metastases treated with bisphosphonates. The experience of the National Cancer Institute of Milan. Ann Oncol. 2009; 20(1): 137-145. https://doi.org/10.1093/annonc/mdn526
45. Dimopoulos MA, Kastritis E, Bamia C, et al. Reduction of osteonecrosis of the jaw (ONJ) after implementation of preventive measures in patients with multiple myeloma treated with zoledronic acid. Ann Oncol. 2008 20(1): 117-120. https://doi.org/10.1093/annonc/mdn554
46. Bonacina R, Mariani U, Villa F, et al. Preventive strategies and clinical implications for bisphosphonate-related osteonecrosis of the jaw: a review of 282 patients. J Can Dent Assoc. 2011; 77: b147.
47. American Dental Association Council on Scientific Affairs. Dental management of patients receiving oral bisphosphonate therapy. Expert panel recommendations. J Am Dent Assoc. 2006; 137: 1144-1150. https://doi.org/10.14219/jada.archive.2006.0355
48. National Health Service Education for Scotland. Oral health management of patients at risk of medication-related osteonecrosis of the jaw: Dental clinical guidance. Scotland: SDCEP; 2017. https://www.sdcep.org.uk/published-guidance/medication-related-osteonecrosis-of-the-jaw/
49. Beth-Tasdogan NH, Mayer B, Hussein H, Zolk O. Interventions for managing medication-related osteonecrosis of the jaw. Cochrane Database Syst. Rev. 2017; 10. https://doi.org/10.1002/14651858.cd012432.pub2
50. Wan JT, Sheeley DM, Somerman MJ, Lee JS. Mitigating osteonecrosis of the jaw (ONJ) through preventive dental care and understanding of risk factors. Bone Res. 2020; 8(1). https://doi.org/10.1038/s41413-020-0088-1
51. Song M. Dental care for patients taking antiresorptive drugs: a literature review. Rest Dent Endod. 2019; 1:44(4): e42. https://doi.org/10.5395/rde.2019.44.e42
52. Dhesy-Thind S, Fletcher G, Blanchette P, Clemons M, Dillmon M, Frank E, et al. Use of adjuvant bisphosphonates and other bone-modifying agents in breast cancer: a Cancer Care Ontario and American Society of Clinical Oncology Clinical Practice Guideline. J Clin Onc. 2017; 35(18): 2062-2081. https://doi.org/10.1200/jco.2016.70.7257
53. Yoshiga D, Yoshioka I, Habu M, Sasaguri M, Tominaga K. Effective ancillary role and long-term course of daily or weekly teriparatide treatment on refractory medication-related osteonecrosis of the jaw (MRONJ): a clinical case series. Brit J Oral Maxillofac Surg. 2021. https://doi.org/10.1016/j.bjoms.2021.10.004
54. Anabtawi, M, Tweedale, H, Mahmood, H. The role, efficacy, and outcome measures for teriparatide use in the management of medication-related osteonecrosis of the jaw. Int J Oral Maxillofac Surg. 2020; https://doi.org/10.1016/j.ijom.2020.07.021
55. Javelot M-J, et al. Rituximab as a trigger factor of medication-related osteonecrosis of the jaw. A case report. J Stomatol Oral Maxillofac Surg. 2019. https://doi.org/10.1016/j.jormas.2019.06.009
56. Sacco R, Shah S, Leeson R, Moraschini V, et al. Osteonecrosis and osteomyelitis of the jaw associated with tumour necrosis factor-alpha (TNF-α) inhibitors: a systematic review. Br J Oral Maxillofac Surg. 2020; 58: 25-33. https://doi.org/10.1016/j.bjoms.2019.09.023
57. Brijs K, Miclotte I, Vermeire S, Darche V, Politis C. Osteonecrosis of the jaw in patients with inflammatory bowel disease treated with tumour necrosis factor alpha inhibitors. Int J Oral Maxillofac Surg. 2020; 49: 317-324. https://doi.org/10.1016/j.ijom.2019.08.007
58. Fleissig Y, Regev E, Lehman H. Sunitinib related osteonecrosis of jaw: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012; 113: e1-e3. https://doi.org/10.1016/j.tripleo.2011.06.023
59. Mauceri R, Panzarella V, Morreale I, Campisi G. Medication-related osteonecrosis of the jaw in a cancer patient receiving lenvatinib, Case Report. Int J Oral Maxillofac Surg. 2019; 48: 1530-1532. https://doi.org/10.1016/j.ijom.2019.07.010
60. Zarringhalam P, Brizman E, Shakib K. Medication-related osteonecrosis of the jaw associated with aflibercept. Br J Oral Maxillofac Surg. 2017; 55: 314-315. https://doi.org/10.1016/j.bjoms.2016.11.315
61. Kim DW, Jung YS, Park HS, Jung HD. Osteonecrosis of the jaw related to everolimus: a case report. Br J Oral Maxillofac Surg. 2013; 51: 302-304. https://doi.org/10.1016/j.bjoms.2013.09.008
62. Akkach S, Shukla L, Morgan D. Everolimus-induced osteonecrosis of the jaw in the absence of bisphosphonates: a case report. Br J Oral Maxillofac Surg. 2019; 57: 688-690. https://doi.org/10.1016/j.bjoms.2019.05.017
63. Komatani T, Sonobe J, et al. Methotrexate-related osteonecrosis of the jaw: Report of two cases. J Oral Maxillofac Surg Med Pathol. 2017; 29: 546-549.
64. Sato T, et al. Osteonecrosis of the jaw with pancytopenia in a patient receiving methotrexate for rheumatoid arthritis without antiresorptive or antiangiogenic agents: Report of a case. J Oral Maxillofac Surg Med Pathol. 2018; 30: 418-421.
65. King R, et al. Medication-related osteonecrosis of the jaw unrelated to bisphosphonates and denosumab-a review. Oral Surg Oral Med Oral Pathol Oral Radiol. 2019; 127: 289-299. https://doi.org/10.1016/j.oooo.2018.11.012