INTRODUCTION
Incisor-molar hypomineralization (IMH), also called incisor-molar syndrome, was a term proposed by Weerheijm et al. in 2001 and has been defined as a series of differentiated enamel defects of systemic origin, mainly affecting first molars, with or without incisors, although they can sometimes affect multiple teeth (1). Prevalence studies have suggested that IMH appears to be a genetic condition in that it may involve genes that are expressed in the formation of enamel (2,3,4). A recent study indicates that the gene that codes for transforming growth factor alpha (TGFA), which contributes to cell regulation, and the gene that codes for interferon regulatory factor 6 (IFR6), which acts in the development of head and neck, may be associated in the etiology of IMH (5).
Clinically, IMH expresses as chalky white opacities that affect enamel translucency and sometimes has a porous appearance similar to the hypocalcified/hypomineralized phenotype of amelogenesis imperfecta (AI). Its severity can vary between patients, rarely affecting mandibular incisors and frequently maxillary incisors. IMH has been associated with respiratory tract problems, exposure to dioxins (toxic chemicals found in the environment), low birth weight, and metabolic disorders of calcium and phosphate (6). Guica et al., in 2018 (7) reported a positive correlation with the use of antibiotics and respiratory diseases of the upper airways (ears, nose, and throat) in the first years of life.
IMH is important because it affects dental tissue causing enamel loss after eruption. Thus, it is a risk factor for the development of carious lesions that can become serious. Likewise, aesthetic problems occur that can affect a person’s self-esteem (8,9). Epidemiological evidence of IMH indicates the highest prevalence in European countries such as Sweden (3.6 % -18.4 %), Finland (17 % -25 %), Great Britain (14.6 %), and Spain 21.8 % (10,11,12,13,14). In Latin America, the prevalence of IMH shows approximate data of 15.8 % in Buenos Aires (15) and 18.4 % in Brazil (16,17). In Mexico City, a prevalence of 13.9 % (18) has been reported, while in Uruguay the epidemiological data of IMH are not conclusive (19).
In Colombia, the prevalence of dental structure anomalies has been described in 63.4 % of the population. However, the frequency according to the type of anomaly has not been identified (20). The IV National Oral Health Study in Colombia (ENSAB IV, 2013-2014) indicated that defined opacities were found in 5-year-olds (29.20 %), 12-year-olds (33.35 %), and the group of 20-34 years of age (30.41 %). No differences were found regarding the prevalence of sex-associated opacities (21). In the specific case of the city of Medellín, the prevalence of IMH, identified by Escobar et al., in 2015 (22) shows data close to 11.2 %.
AI, on the other hand, is a group of hereditary disorders characterized by defects in enamel quality and quantity. It occurs in both deciduous and permanent dentitions (23). AI phenotypes have been classified as: 1) hypoplastic, which presents a thin enamel and, when it is severe, it is absent; 2) hypomineralized, which is characterized by an enamel with normal thickness in which calcification fails, which causes it to wear easily; and 3) hypo maturated, which is caused by the incomplete removal of proteins from the enamel matrix and causes enamel to have a mottled appearance. The latter phenotype can be associated with taurodontism. Sometimes phenotypes can also be mixed, which diagnostic confusion (24,25,26).
The frequency of IA in different populations ranges from 1:700 to 1:14,000 (27). Severe cases are accompanied by dental sensitivity that makes eating difficult and cause poor aesthetics generating low self-esteem (28). Similarly, this pathology has been associated with dental alterations such as dental agenesis, taurodontism, and apical dilaceration. It is also associated with skeletal alterations such as anterior open bite and mandibular micrognathism (29). Its treatment is based on aesthetic and functional interventions (30). Some studies indicate the need to make a differential diagnosis with enamel defects such as IMH (31), fluorosis, and enamel defects caused by systemic problems (32).
IMH is a public health problem that is suffered by, at least, one in five children. Clinically, this pathology expresses in several ways making differential diagnosis with other enamel abnormalities confusing (33). Currently, there are no studies on the facial and skeletal characteristics of people with IMH that could help to complement clinical diagnosis. As a consequence, this study identified the facial and skeletal characteristics of patients with IMH and compared them with those of patients with AI. The research question was: What are the phenotypic differences between two IMH and AI that would support differential diagnosis?
MATERIALS AND METHODS
This was an exploratory study with an analytical observational design that was approved by the Ethics and Research Committee of the Pontificia Universidad Javeriana’s Dental School (PUJDS) from Bogotá, on 18 February 2011, as recorded in the document No. 003.
Population and Sample
Participants in this study consisted of 8 women and 4 men who met the following inclusion criteria: age group 7-10 years, complete eruption of upper and lower permanent incisors and first molars, diagnosis of IMH and be active patients at the PUJDS’s undergraduate and graduate pediatric dental clinics. Patients with any type of syndrome, history of dentoalveolar trauma, and only primary dentition were excluded. Likewise, people with diffuse opacities in permanent incisors and first molars that were not characteristic of IMH, and individuals with diagnosed dental fluorosis were excluded.
Participants’ guardians were explained the characteristics and risks of the study and signed the informed consent form. On the other hand, patients diagnosed with AI were taken as a reference for comparison, using Witkop et al. 1989 (23) classification. The latter sample consisted of 10 people (7 women and 3 men, aged 8 to 49 years), who attended the same clinics and were part of a study on phenotypic facial, dental, skeletal, and histological characteristics in families with AI in 2017 (34).
Clinical Analysis in Patients with IMH
Measurements of skeletal and facial characteristics and occlusal alteration analysis were performed by a single operator calibrated using the Kappa index with 99 % agreement (intra-operator). After dental prophylaxis, clinical examination of patients was performed, including tooth occlusal, buccal, lingual and palatal surfaces. Data were recorded in a form that also included age, gender, socioeconomic level, affected tooth surfaces, severity, and criteria used for diagnosis. The socioeconomic level was determined through the domiciliary public utility bills (6 levels).
Analysis of Dental Characteristics
Measurements of dental characteristics were carried out by two non-calibrated expert operators (researchers), who followed the European Academy of Pediatric Dentistry (EAPD) diagnostic criteria. It included presence of defined opacities, post-eruption enamel fractures, atypical restorations, absence of one or more molars due to extraction, and non-erupted teeth (35). The classification of severity of injuries was performed following Mathu-Maju and Wright’s (36) 2006 criteria, who established the severity of IMH as: 1 (low), 2 (moderate), and 3 (severe). Phenotype classification used Neeti Mittal’s (37) 2016 criteria, which consist of:
-
I (MH): Enamel hypomineralization affecting only first permanent molars (FPMs).
-
II (IH): Enamel hypomineralization affecting only the permanent incisors (PIs).
-
III (M + IH): Enamel hypomineralization affecting PFMs and PIs, without affecting another tooth.
-
IV (MIOH): Enamel hypomineralization affecting at least one canine/premolar or second molar with at least one PFM. PIs could be affected as well.
-
V (NoPFM): Enamel hypomineralization affecting at least one canine/premolar or second molar with PIs, but no FPMs.
Analysis of Dental Anomalies
Dental anomalies such as supernumerary teeth, macrodontia, taurodontism, dental agenesis, pulp calcifications, apical dilaceration, acceleration of dental development, enamel hypoplasias, altered eruption sequence, hypodontia, oligodontia, gemination, fusion, concrescence, and dens in dent were diagnosed in patients with IMH using intraoral photographs and panoramic radiographs (Orthopantomograph OP200 D®).
Analysis of Skeletal Features
Skeletal analysis of sagittal and vertical planes was carried out using lateral cephalic radiographs taken with an Orthoceph OC200D® equipment. Steiner, McNamara, Bjork, and Legan soft cephalometric analyzes were conducted (convexity angle G-Sn-Pg, maxillary prognathism SNA, mandibular prognathism SNB, type of ANB malocclusions, palatal plane angle SN-SN-PP, SN-PM, maxillo-mandibular, facial height ENA-M, NS-Ar (1), S-Ar-GoC (2), gonion angle Ar-GocM (3) and the sum of angles (1,2,3) polygon). All cephalometric measurements were hand-performed (Figure 1, Table 1).
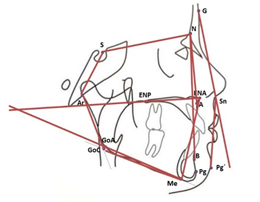 Figure 1
Cephalometric traces of individuals with IMH (n=12)
Figure 1
Cephalometric traces of individuals with IMH (n=12)
Table 1
Reference Values for Cephalometric Analysis of Individuals with IMH (n=12)
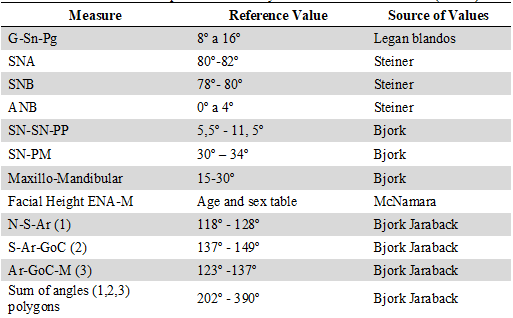
Source: the authors.
Analysis of Occlusal Alterations
The three planes of space were considered: sagittal (molar class, canine class, overjet, anterior length), vertical (overbite) and transverse (anterior and posterior width of the arch). This analysis was used as a complement to the cephalometric analysis. For the IMH group, physical and digital study models were obtained. Only models were obtained on patients with AI.
Facial Feature Analysis
Frontal and profile facial photographs were used to determine facial characteristics: facial symmetry, facial thirds analysis, facial fifths analysis, upper and lower lip position, and profile type. All measurements in diagnostic aids were performed by a previously trained and standardized operator.
Statistical analysis
All data were populated in an Excel® spreadsheet and analyzed through the SPSS 22.0.0 (IBM®) software. Descriptive analysis was performed for dental, facial, and skeletal characteristics of individuals diagnosed with IMH and AI, using frequency, central tendency, dispersion, and normality (Shapiro Wilk test). A bivariate inferential analysis was carried out between diagnostic groups comparing continuous data by means of the Mann-Whitney and T tests. Then a normality analysis was conducted. For the comparison of frequencies of dental, facial and skeletal characteristics by groups, the Chi. and exact Fisher's tests were used (p = 0.05).
RESULTS
The average age of the 12 patients with IMH was 8.9 years, with a higher frequency in women than in men. Regarding the socioeconomic level, the most frequent was 2 among 7 subjects, followed by 5 in 2 people and levels 1, 3 and 4 with one individual each.
Analysis of Dental Features in Individuals with IMH and AI
Dental characteristics were analyzed using the Chi. and exact Fisher's tests. Most of the people with IMH had phenotype III, with involvement of molars rather than incisors. Lower molars were more affected than upper ones. Regarding severity, the majority presented combinations of the 3 degrees (low, moderate and severe) (Figure 2).
When comparing dental characteristics in patients with IMH, with respect to the characteristics described in people with AI (reference population), statistically significant differences were found in terms of the presence of apical dilaceration and taurodontism in AI mainly. Dental agenesis was also found in those with AI and no cases were identified in people with IMH. No statistically significant differences were observed with respect to pulp calcification and no person with IMH had hypodontia, oligodontia, gemination, fusion, concrescence, dens in dent, or acceleration of root development (Table 2).
Table 2
Dental Features by Group
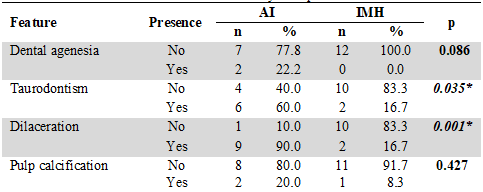
Chi2 and exact Fisher’s test (p≤ 0,05)
*Statistically significant findings.
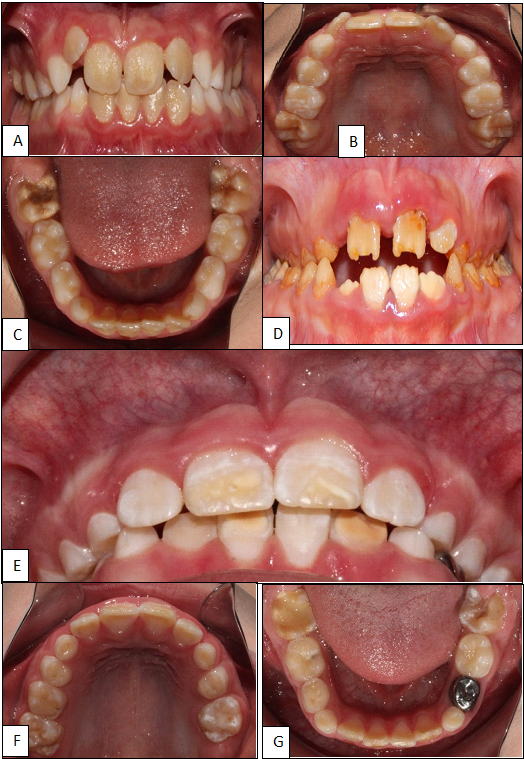 Figure 2
Intraoral Photographs of Individuals with IMH and AI*
Figure 2
Intraoral Photographs of Individuals with IMH and AI*
*A, B y C: Intraoral photographs corresponding to a person with a type III phenotype. This person had severe enamel hypomineralization on all four molars and mild on the incisors. Delimited cream-like white lesions were observed. D: Intraoral photograph corresponding to a patient with IA and with a hypomineralized (hypocalcified) phenotype. Photo courtesy of doctors Grace Abad and Silvana Guerrero (34), which shows yellowish enamel lesions, large surface wear, fractures in anterior and posterior teeth and lesions spread to a greater number of teeth. E, F and G: Intraoral photographs corresponding to another person with IMH, also with phenotype III. The lesions were classified as mild on an upper molar and severe on the lower molars. The upper and lower anterior teeth had defined enamel lesions, the upper anterior teeth being more severe than the lower ones.
Source: Photos posted with patient permission.
Analysis of Facial Characteristics in People with IMH and AI
In all patients with IMH asymmetry was observed between the right and left sides of the face, decreased lower third, upper and lower prochelia, and convex profile. When comparing these facial characteristics with the AI group, there were coincidences in the same variables. The analysis of categorical facial characteristics was performed using the exact Fisher's test. No statistically significant differences were found between the AI and IMH groups. Regarding facial symmetry, it was found that people with AI had a higher proportion of facial asymmetry than those with IMH.
In the thirds analysis, patients with AI had a decreased lower third compared to the middle third. The analysis of the facial fifths showed a greater disproportion in AI than in IMH, an increased intercanthal distance in those with AI and IMH. Regarding the upper lip position in people with AI prochelia was found in a higher proportion than in those with IMH. According to the position of the lower lip, prochelia was observed to a lesser extent in subjects with AI than in those with IMH. Regarding the profile type, convexity was more frequent in patients with AI than in patients with IMH (Figure 3). Table 3 summarizes the comparison of facial characteristics between people with IMH and AI.
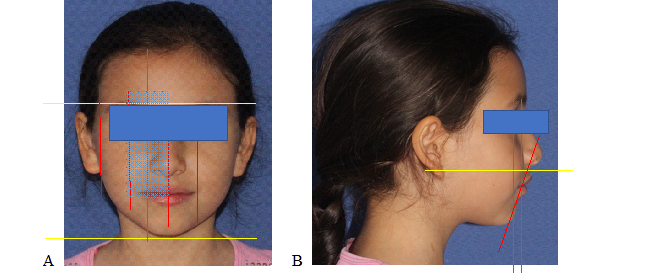 Figure. 3.
Facial Analysis on Photographs
Figure. 3.
Facial Analysis on Photographs
A: Front photograph in which the analysis of facial symmetry, proportion of facial thirds and fifths were performed. B: Profile photograph in which the type of profile and the position of the upper and lower lips were observed, taking the Schwarz aesthetic line (Sn-Pg) as a reference.
Source: photos published with patient permission.
Table 3
Facial Characteristics by Group
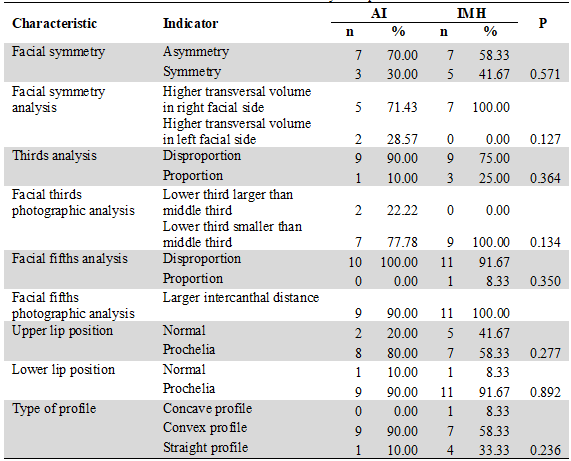
Analysis through exact Fisher’s test (p≤ 0,05). There were no statistically significant differences.
Analysis of Skeletal Characteristics in People with IMH and AI
The most frequent skeletal alterations in people with IMH were convex profile, skeletal Class I, mandibular retrognathism, downward and backward rotation of the mandibular body (post-rotation), vertical growth trend, and decreased anterior arch length. In cross-sectional relationships, people with IMH more frequently presented mandibular micrognathism. When comparing them with the group with AI, there were some differences. The AI group more frequently presented a convex profile, while half of the IMH group had a convex profile and half had a straight profile. Regarding the skeletal relationships of IMH, there was a higher frequency of Class I people, while in the AI group half were Class II and half were Class I. With respect to the maxillary sagittal relationships, there was variation in the two groups regarding the mandibular sagittal position, but there was a coincidence in the mandibular retrognathic position and the predominance of mandibular rotation downwards and backwards. Regarding the growth trend, the IMH group presented a higher frequency of vertical growth, while in the AI group, half showed vertical growth and the other half neutral growth. The categorical skeletal variables between the two groups are shown in Table 4.
Regarding the sum of angles (1, 2, 3) polygon, individuals with IMH tended to present severe vertical growth, while those with AI tended to show normal growth. Among the other categories, that is, SNA and SNB angles, type of ANB malocclusions, palatal plane angle to SN-SN-PP, angle SN-PM, maxillo-mandibular angle, facial height ENA-Angle N-S-Ar (1), S-Ar-GoC angle (2) (branch flexion), and AR-GoC-M gonion angle (3), no statistically significant differences were found (Table 4).
Table 4
Skeletal Features in each Group
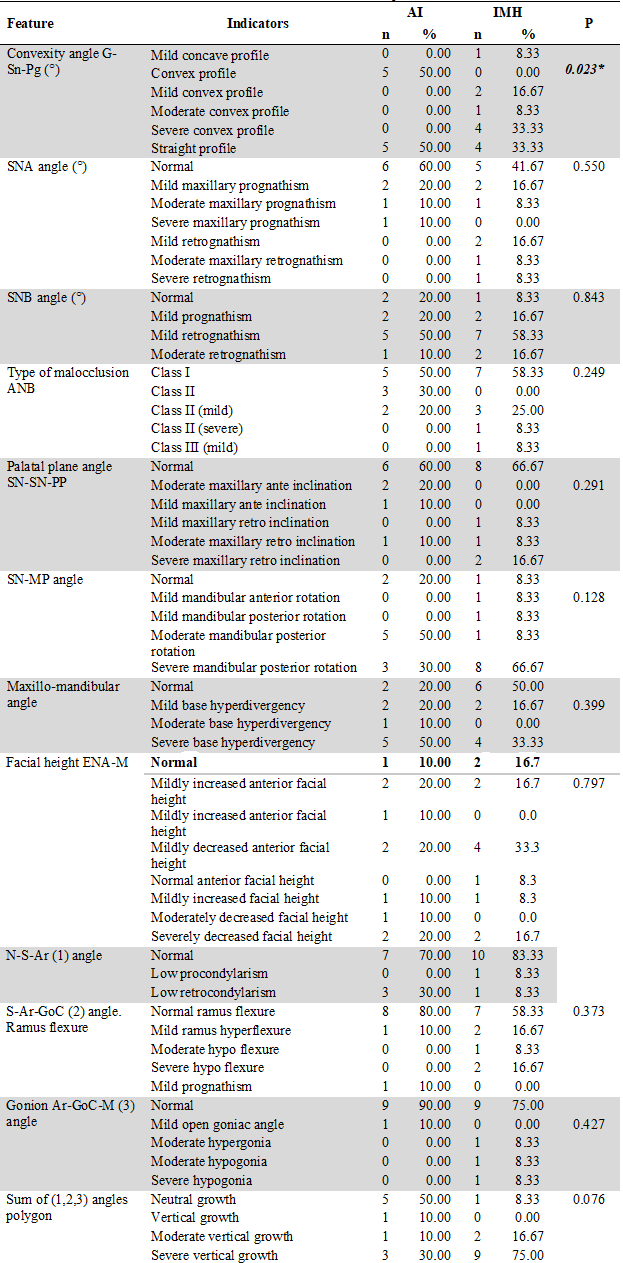
Analysis performed through Chi2 and exact Fisher’s tests (p ≤0,05).
*Statistically significant results.
Analysis of Occlusal Characteristics in People with IMH and LA
People with IMH did not present a defined trend in molar and canine relationships or in overjet. However, overbite was found to be increased. Deep bite was greater than in the AI group (7 people). In the AI group, half of the participants had an open bite, one had a normal bite, and 4 showed a tendency to a deep bite. Data were analyzed through Chi2 and exact Fisher’s tests (p <0.05).
Regarding the right molar ratio (p = 0.115), the left molar ratio (p = 0.414), the right canine ratio (p = 0.995) and the left canine ratio (p = 0.561), no statistically significant differences were found. Regarding the anterior length of the upper and lower arch, upper jaw (distance from first premolar to first premolar [4-4]), upper jaw (distance from first molar to first molar [6-6]), and lower jaw (distance 6-6 or transversal development of the arch at the posterior level), the only statistically significant differences were found in the 4-4 distance (transversal development of the anterior arch) (Table 5).
Table 5
Occlusal Characteristics in Individuals with IMH and AI
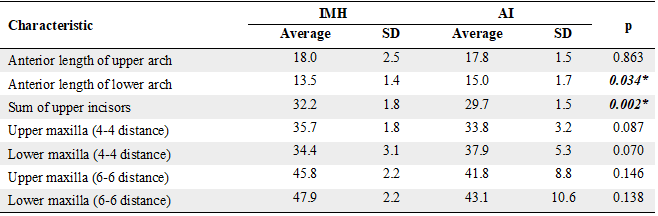
Performed through t-test (p ≤ 0.05)
*Statistically significant results.
DISCUSSION
Knowing phenotypic characteristics of one of the most frequent enamel defects such as IMH is necessary since it generates diagnostic confusion with other enamel defects such as AI. This is the first study that reports IMH phenotypic characteristics and compares them to those of AI. Specifically, it is the first to describe skeletal and facial aspects and associated dental alterations. These findings provide evidence for the differential diagnosis.
One of the variables analyzed in this study was the prevalence of IMH with respect to sex. A higher frequency was found in women (66%) than in men (34%). This finding contrasts with the study by Padavala et al. (38), who found no differences associated with sex. However, it is close to Morenike et al. (39), who found IMH in 58.8% men and 43.9% women.
Regarding the socioeconomic level, in this study IMH predominance was found at level 2 (low, which is determined by sectorization based on the value of home utilities). It coincides with Corral-Núñez et al. (40) in Chilean population, among whom IMH predominated in low socioeconomic levels. This could suggest an influence from the context. More studies should be carried out in this regard.
On the other hand, the analysis of dental phenotype showed that the most frequent IMH type was III (hypomineralization of the enamel with concomitant hypomineralization of one or more first permanent molars and of the permanent incisors, without affecting another tooth) by 90.91 %. The remaining 9.09 % corresponded to type I (enamel hypomineralization in first permanent molars) (Figure 2 A-C, E-G). In contrast, in an IMH prevalence study carried out by Mittal (37) in Indian population, phenotype II (enamel hypomineralization affecting only the permanent incisors) was 71 % more frequent. To date, this is the only study found in the reviewed literature that used of phenotype classification in people with IMH. This suggests that IMH is a highly heterogeneous pathology, which could support the recently described genetic etiology (2-5).
Likewise, with respect to severity (36), most of the people with IMH in the present study also showed great variability of molar and incisor defects (Figure 2 A-C, E-G). A combination of mild and severe IMH was more frequent, and the mild level was less frequent. It was found that in the same patient some teeth were severely affected, while their counter laterals were healthy or had just minor defects. These findings coincide with those of Guica et al. (7) and Padavala et al. (38).
The phenotypes of people in the AI group (considered for comparison purposes in this study) were also variable and heterogeneous, even among the same teeth. Enamel lesions were also found in combination. Specifically, in the severe hypomineralized phenotype, worn enamel surface was greater, its color was more yellow-like, and poorly defined lesions were more generalized (Figure 2D) when compared with teeth with IMH (34). It should be noted that, when the hypomineralized phenotype of AI was less severe, lesions were very similar to those of IMH.
Additionally, according to the latest IMH classification published by Mittal in 2016 (37), in phenotypes IV and V almost all teeth are affected by IMH, which makes differential diagnosis with IA more difficult. However, most of the mandibular molars in the present study were affected by IMH, followed by incisors (Figure 2A-C, E-G), which is contrary to the findings of Lima et al. (17), according to whom upper molars were the teeth most affected by IMH.
Regarding associated dental alterations in IMH, no published studies were found. Neither were these alterations considered among the diagnostic criteria for IMH. Thus, this study is the first to analyze this. It was found that 27.27 % of the participants diagnosed with IMH had enamel hypoplasia and 36.36 % had eruption sequence alterations. When comparing other alterations among people with IA, statistically significant differences were found in terms of the presence of dilacerations and taurodontism (Table 3), which could contribute as indicators for differential diagnosis.
On the other side, facial characteristics were similar between these two enamel alterations, with the exception of the facial profile, which was more convex in people with AI. This feature could contribute to upper prochelia identified in people with AI. In individuals with IMH, lower prochelia was more frequent, which was more frequently in the straight profile (Figure 3, Table 3). Skeletal characteristics were also variable. It should be noted that both the skeletal profile and the mandible vertical growth resulted in statistically significant differences that could provide important indicators in the differential diagnosis between these two entities. Likewise, in terms of vertical occlusal characteristics, deep bite stood out among patients with IMH (Tables 4 and 5).
Findings of this study regarding facial, skeletal, and dental characteristics among people with IMH and compared to those with AI seem to suggest that the pleiotropic effect of the genes causing AI is more revealing and exerts a greater effect on the genes that cause AI, and govern tooth formation and facial, occlusal, and skeletal structures. This is supported by studies such as Padavala et al. (38), who indicate that IMH is an autosomal recessive disorder (localized amelogenesis imperfecta), with a possible association with genes related to enamel formation, such as ameloblastin (AMBN) and tuftelin (TUFT1) genes interacting with protein 11 (TFIP11), which indicates its origin seems to have a strong genetic component. Another study, Busanelli et al. (3), also indicates an association between single nucleotide polymorphisms of the TGF BR1 gene and genes that act in amelogenesis with the etiology of IMH.
IMH and AI appear to have a similar genetic etiology, resulting in a similar phenotype. However, findings about the facial, skeletal, and occlusal characteristics of IMH are novel since they are analyzed here for the first time. This favors the establishment of criteria for differential diagnosis of this pathology with respect to AI and could be used as a basis to establish differences with other enamel alterations, such as those caused by fluorosis. The latter, despite the fact that most studies suggest it is caused by excess intake of fluoride, which interferes during the amelogenesis process (41,42), its etiology has also been attributed to the influence of genes related to enamel formation (43,44).
Therefore, it is important that dentists not only limit themselves to daily examinations for these enamel alterations, but also carry out more in-depth clinical, radiographic, and genetic studies. A complete anamnesis is necessary to identify other possible characteristics that may contribute to determining a differential diagnosis between each of the pathologies that affect enamel.
CONCLUSIONS
In this study, although a limited sample size was used, people with IMH did not present associated dental alterations such as taurodontism, root dilaceration, pulp calcification, or other alterations of structure, shape and number, which were characteristic of AI.
Facial characteristics such as facial asymmetry, increased intercanthal distance, biprochelia, decreased lower third, and convex profile of people with IMH were similar to those of patients with AI.
Skeletal characteristics varied between people with IMH and AI. Only two variables coincided: mandibular retrognathism and posterior rotated mandibular position. Regarding the transverse development of the arches, all measurements in the upper and lower arches of patients with IMH showed micrognathism and a decreased anterior length in most of the people.
Regarding the occlusal characteristics of patients with IMH and AI, a definite trend was not found with respect to the molar relationship, the canine, and the horizontal overbite. However, regarding overbite, the deep bite predominated in subjects with IMH.
RECOMMENDATIONS
Carry out prevalence studies of IMH in Colombian population, in order to determine its distribution and magnitude over time.
Conduct studies with a greater number of individuals with IMH to establish differential diagnostic criteria, not only with AI, but also with other enamel alterations such as fluorosis.
Acknowledgments
To the Pontificia Universidad Javeriana, its Dental School, and the Center for Dental Research, for the logistical and financial support.
This study was approved by the Ethics and Research Committee of Pontificia Universidad Javeriana’s Dental School, on 18 February 2011, as recorded in minutes No. 003, and is part of the line of research on Amelogenesis Imperfecta.
REFERENCES
1. Weerheijm K, Jälevik B, Alaluusua S. Molar-incisor hypomineralisation. Caries Res. 2001 Sep-Oct; 35(5): 390-391. https://doi.org/10.1159/000047479
2. Jeremias F, Koruyucu M, Küchler EC, Bayram M, Tuna EB, Deely K, Pierri RA, Souza JF, Fragelli CM, Paschoal MA, Gencay K, Seymen F, Caminaga RM, dos Santos-Pinto L, Vieira AR. Genes expressed in dental enamel development are associated with molar-incisor hypomineralization. Arch Oral Biol. 2013 Oct; 58(10): 1434-1442. https://doi.org/10.1016/j.archoralbio.2013.05.005
3. Bussaneli DG, Restrepo M, Fragelli CMB, Santos-Pinto L, Jeremias F, Cordeiro RCL, Bezamat M, Vieira AR, Scarel-Caminaga RM. Genes regulating immune response and amelogenesis interact in increasing the susceptibility to molar-incisor hypomineralization. Caries Res. 2019; 53(2): 217-227. https://doi.org/10.1159/000491644
4. Vieira AR, Manton DJ. On the variable clinical presentation of molar-incisor hypomineralization. Caries Res. 2019; 53(4): 482-488. https://doi.org/10.1159/000496542
5. Bezamat M, Souza JF, Silva FMF, Corrêa EG, Fatturi AL, Brancher JA, Carvalho FM, Cavallari T, Bertolazo L, Machado-Souza C, Koruyucu M, Bayram M, Racic A, Harrison BM, Sweat YY, Letra A, Studen-Pavlovich D, Seymen F, Amendt B, Werneck RI, Costa MC, Modesto A, Vieira AR. Gene-environment interaction in molar-incisor hypomineralization. PLoS One. 2021 Jan 6; 16(1): e0241898. https://doi.org/10.1371/journal.pone.0241898
6. Weerheijm KL. Molar incisor hypomineralization (MIH): clinical presentation. aetiology and management. Dent Update. 2004 Jan-Feb; 31(1): 9-12. https://doi.org/10.12968/denu.2004.31.1.9
7. Giuca MR, Cappè M, Carli E, Lardani L, Pasini M. Investigation of clinical characteristics and etiological factors in children with molar incisor hypomineralization. Int J Dent. 2018 May 9; 2018: e7584736. https://doi.org/10.1155/2018/7584736
8. Grošelj M, Jan J. Molar incisor hypomineralisation and dental caries among children in Slovenia. Eur J Paediatr Dent. 2013 Sep; 14(3): 241-245.
9. William V, Messer LB, Burrow MF. Molar incisor hypomineralization: review and recommendations for clinical management. Pediatr Dent. 2006 May-Jun; 28(3): 224-232.
10. Muratbegovic A, Markovic N, Ganibegovic Selimovic M. Molar incisor hypomineralisation in Bosnia and Herzegovina: aetiology and clinical consequences in medium caries activity population. Eur Arch Paediatr Dent. 2007 Dec; 8(4): 189-194. https://doi.org/10.1007/BF03262595
11. Bhaskar SA, Hegde S. Molar-incisor hypomineralization: prevalence. severity and clinical characteristics in 8- to 13-year-old children of Udaipur. India. J Indian Soc Pedod Prev Dent. 2014 Oct-Dec; 32(4): 322-3229. https://doi.org/10.4103/0970-4388.140960
12. Garcia-Margarit M, Catalá-Pizarro M, Montiel-Company JM, Almerich-Silla JM. Epidemiologic study of molar-incisor hypomineralization in 8-year-old Spanish children. Int J Paediatr Dent. 2014 Jan; 24(1): 14-22. https://doi.org/10.1111/ipd.12020
13. Calderara PC, Gerthoux PM, Mocarelli P, Lukinmaa PL, Tramacere PL, Alaluusua S. The prevalence of molar incisor hypomineralisation (MIH) in a group of Italian school children. Eur J Paediatr Dent. 2005 Jun; 6(2): 79-83.
14. Ng JJ, Eu OC, Nair R, Hong CH. Prevalence of molar incisor hypomineralization (MIH) in Singaporean children. Int J Paediatr Dent. 2015 Mar; 25(2): 73-78. https://doi.org/10.1111/ipd.12100
15. Biondi AM, Cortese SG, Martínez K, Ortolani AM, Sebelli PM, Ienco M, Paván VH, Mendel N, Bertolino M, Hecht P. Prevalence of molar incisor hypomineralization in the city of Buenos Aires. Acta Odontol Latinoam. 2011; 24(1): 81-85.
16. da Costa-Silva CM, Jeremias F, de Souza JF, Cordeiro Rde C, Santos-Pinto L, Zuanon AC. Molar incisor hypomineralization: prevalence. severity and clinical consequences in Brazilian children. Int J Paediatr Dent. 2010 Nov; 20(6): 426-434. https://doi.org/10.1111/j.1365-263X.2010.01097.x
17. de Lima M de D, Andrade MJ, Dantas-Neta NB, Andrade NS, Teixeira RJ, de Moura MS, de Deus Moura L de F. Epidemiologic study of molar-incisor hypomineralization in schoolchildren in north-eastern Brazil. Pediatr Dent. 2015 Nov-Dec; 37(7): 513-519.
18. Murrieta Pruneda JF, Torres Vargas J, Sánchez Meza J del C. Frecuencia y severidad de hipomineralización incisivo molar (HIM) en un grupo de niños mexicanos. Rev Nac Odontol (México) 2014; 12(23): 7-14. https://doi.org/10.16925/od.v12i23.1377
19. López Jordi M, del Carmen Álvarez L, Salveraglio I. Prevalencia de la hipomineralización molar-incisiva (MIH) en niños con diferente cobertura asistencial (privada y pública) en Montevideo, Uruguay. Odontoestomatol. 2013; 15(22): 4-15.
20. Espinal G, Manco HA, Aguilar G, Castrillón L, Rendón JE, Marín ML. Retrospective study of dental anomalies and bone alterations of the jawbones in children 5 to 14 years old of the clinics of the Dental School, University of Antioquia. Rev Fac Odontol Univ Antioq. 2009; 21(1): 50-64.
21. Tovar S, Ziga E, Franco A, Jácome S, Ruiz III J. Estudio Nacional en Salud Bucal (ENSAB IV). Bogotá. Colombia: Ministerio de Salud; 2014.
22. Castaño-Lopez L, Mejía-Roldan J, Escobar- Rojas A. Prevalencia y severidad de la hipomineralizacion incisivo-molar (HIM) en pacientes escolarizados de la ciudad de Medellín. Medellin, Colombia: Repositorio Universidad CES; 2015.
23. Witkop CJ, Sauk JJ. Defectos hereditarios del esmalte. En Stewart RE, Prescott GH, editores. Genética facial oral. St. Louis, MO: Mosby; 1976. pp. 151-226.
24. Witkop CJ. Amelogenesis imperfecta. dentinogenesis imperfecta and dentin dysplasia revisited: problems in classification. J Oral Pathol. 1988 Nov; 17(9-10): 547-553. https://doi.org/10.1111/j.1600-0714.1988.tb01332.x
25. Aldred MJ, Savarirayan R, Crawford PJ. Amelogenesis imperfecta: a classification and catalogue for the 21st century. Oral Dis. 2003 Jan; 9(1): 19-23. https://doi.org/10.1034/j.1601-0825.2003.00843.x
26. Crawford PJ, Aldred M, Bloch-Zupan A. Amelogenesis imperfecta. Orphanet J Rare Dis. 2007 Apr 4; 2: 17. https://doi.org/10.1186/1750-1172-2-17
27. Bäckman B, Holm AK. Amelogenesis imperfecta: prevalence and incidence in a northern Swedish county. Community Dent Oral Epidemiol. 1986 Feb; 14(1): 43-47. https://doi.org/10.1111/j.1600-0528.1986.tb01493.x
28. Hashem A, Kelly A, O'Connell B, O'Sullivan M. Impact of moderate and severe hypodontia and amelogenesis imperfecta on quality of life and self-esteem of adult patients. J Dent. 2013 Aug; 41(8): 689-694. https://doi.org/10.1016/j.jdent.2013.06.004
29. Bailleul-Forestier I, Molla M, Verloes A, Berdal A. The genetic basis of inherited anomalies of the teeth. Part 1: clinical and molecular aspects of non-syndromic dental disorders. Eur J Med Genet. 2008 Jul-Aug; 51(4): 273-291. https://doi.org/10.1016/j.ejmg.2008.02.009
30. Dashash M, Yeung CA, Jamous I, Blinkhorn A. Interventions for the restorative care of amelogenesis imperfecta in children and adolescents. Cochrane Database Syst Rev. 2013 Jun 6; (6): CD007157. https://doi.org/10.1002/14651858.CD007157
31. Gotler M, Ratson T. [Molar incisor hypomineralization (MIH)--a literature review]. Refuat Hapeh Vehashinayim (1993). 2010 Apr; 27(2): 10-18, 60.
32. Salanitri S, Seow WK. Developmental enamel defects in the primary dentition: aetiology and clinical management. Aust Dent J. 2013 Jun; 58(2): 133-40; quiz 266. https://doi.org/10.1111/adj.12039
33. Kuscu OO, Sandalli N, Dikmen S, Ersoy O, Tatar I, Turkmen I, Caglar E. Association of amoxicillin use and molar incisor hypomineralization in piglets: visual and mineral density evaluation. Arch Oral Biol. 2013 Oct; 58(10): 1422-1433. https://doi.org/10.1016/j.archoralbio.2013.04.012
34. Abad G, Guerrero S, Gutiérrez S, Méndez P, López E, Suarez A. Características fenotípicas faciales. dentales. esqueléticas e histológicas en familias con amelogénesis imperfecta. [trabajo de grado]. Bogota, Colombia: Pontificia Universidad Javeriana; 2017.
35. Weerheijm KL, Duggal M, Mejàre I, Papagiannoulis L, Koch G, Martens LC, Hallonsten AL. Judgement criteria for molar incisor hypomineralisation (MIH) in epidemiologic studies: a summary of the European meeting on MIH held in Athens. 2003. Eur J Paediatr Dent. 2003 Sep; 4(3): 110-113.
36. Mathu-Muju K, Wright JT. Diagnosis and treatment of molar incisor hypomineralization. Compend Contin Educ Dent. 2006 Nov; 27(11): 604-610; quiz 611.
37. Mittal N. Phenotypes of enamel hypomineralization and molar incisor hypomineralization in permanent dentition: identification. quantification and proposal for classification. J Clin Pediatr Dent. 2016; 40(5): 367-374. https://doi.org/10.17796/1053-4628-40.5.367
38. Padavala S, Sukumaran G. Molar incisor hypomineralization and its prevalence. Contemp Clin Dent. 2018 Sep; 9(Suppl 2): S246-S250. https://doi.org/10.4103/ccd.ccd_161_18
39. Folayan MO, Oyedele TA, Oziegbe E. Time expended on managing molar incisor hypomineralization in a pediatric dental clinic in Nigeria. Braz Oral Res. 2018 Aug 6; 32: e79. https://doi.org/10.1590/1807-3107bor-2018.vol32.0079
40. Corral-Núñez C, Rodríguez H, Cabello R, Bersezio-Miranda C, Cordeiro R, Fresno-Rivas MC. Impacto de la hipomineralización incisivo molar en la experiencia de caries en escolares de 6-12 años en Santiago, Chile. Rev Clin Period Implantol Rehabil Oral. 2016; 9(3). http://dx.doi.org/10.1016/j.piro.2016.10.003
41. Bronckers AL, Lyaruu DM, DenBesten PK. The impact of fluoride on ameloblasts and the mechanisms of enamel fluorosis. J Dent Res. 2009 Oct; 88(10): 877-893. https://doi.org/10.1177/0022034509343280
42. Aoba T, Fejerskov O. Dental fluorosis: chemistry and biology. Crit Rev Oral Biol Med. 2002; 13(2): 155-70. https://doi.org/10.1177/154411130201300206
43. Küchler EC, Dea Bruzamolin C, Ayumi Omori M, Costa MC, Antunes LS, Pecharki GD, Trevilatto PC, Vieira AR, Brancher JA. Polymorphisms in nonamelogenin enamel matrix genes are associated with dental fluorosis. Caries Res. 2018; 52(1-2): 1-6. https://doi.org/10.1159/000479826
44. Küchler EC, Tannure PN, Oliveira DS, Charone S, Nelson-Filho P, Silva RA, Costa MC, Antunes LS, Calasans Maia MD, Antunes LA. Polymorphisms in genes involved in enamel development are associated with dental fluorosis. Arch Oral Biol. 2017 Apr; 76: 66-69. https://doi.org/10.1016/j.archoralbio.2017.01.009
Notes
*
Original research.
Additional information
How to cite: Casas Araya M, López Panqueva E, Suárez Castillo A, Gutierrez Prieto SJ. Incisor-molar hypomineralization phenotype characteristics and comparison with amelogenesis imperfecta: an approach to a differential diagnosis. Univ Odontol. 2021; 40. https://doi.org/10.11144/Javeriana.uo40.imhp