INTRODUCTION
Currently, there has been evidence of an increase in chronic noncommunicable diseases due to changes in lifestyles, the concentration of the population in urban centers, and technological development (1). One of these diseases is type 2 diabetes mellitus (DM2), which the International Diabetes Federation (IDF) describes as one of the main causes of death in the adult population ≤60 years (2).
The National Demographic and Health Survey (ENDS) in Colombia showed a prevalence of DM2 of 11.2% in 2011 (3). In 2019, the number of people with diabetes in Latin America was estimated to be 31.6 million (4). In the case of Colombia, no data is available, but there are currently two registries, the Comprehensive Social Protection Information System (SIPAS) and the High-Cost Account (CAC) that show a prevalence of DM2 between 1.4 % and 12%, although they are limited because they do not cover 100% of the population (3).
Diabetes mellitus or metabolic syndrome is a disease that generates various sequelae in the state of general health and deterioration of oral health (4). Oral conditions such as geographic tongue, dental caries, xerostomia, periodontitis, edentulism, denture stomatitis, lichen planus and oral pain are the most prevalent in DM2. However, such oral lesions and conditions are not pathognomonic of the disease (5) but may have an unfavorable course due to elevated blood glucose levels (4,5). Such is the case of the bidirectional link between DM2 and chronic periodontitis, which results in greater systemic involvement (6).
Studies in Colombia indicate how chronic pathologies such as DM2 and the pharmacological measures for its treatment can impact the oral health of patients (7), which can compromise the daily routine and affect certain individual, family, and social functions and activities. (8, 9). It is recognized that xerostomia can cause difficulty in swallowing food, chewing, or speaking and can increase susceptibility to caries and oral infections, as well as taste disorders, halitosis, and friability of the oral mucosa in these patients (10). Regarding periodontitis, research in Colombia confirms its character as a chronic inflammatory reaction to the biofilm accumulated around the surfaces of the teeth, which, in the absence of adequate oral hygiene in patients with DM2, generates a greater loss of clinical attachment that contributes to the formation of periodontal pockets, is accompanied by bleeding on probing and ends with tooth loss (11). DM2 is also a source of stress due to the meaning it has for the person to suffer from a chronic disabling disease, which imposes limitations on behavior and predisposes to the appearance of psychopathological disorders such as depression and anxiety (12-13).
Thus, the state of oral health in patients can compromise the different domains related to the concept of oral health-related quality of life (OHRQoL), such as physical, psychosocial, and pain domains, affecting the well-being of people who suffer from DM2 (14). Numerous investigations show important assessments of the social determinants of health and their impact on glycemic control, cost, and quality of life (15). These investigations serve as a precedent for this study and propose to evaluate sociodemographic conditions (social, economic, and health policies), because they impact people's health in the same way as they do on their OHRQoL (15,16).
In Colombia, there are studies that relate oral health and quality of life, in adults without systemic conditions, in which a direct interaction with general health states and a negative self-perception of well-being has been recognized (17). At the end of the search in the scientific literature in relation to the study population, no local studies were found that, exclusively, allow us to answer the question: What is the impact of oral health on the OHRQoL of patients with DM2?
This study is one of the first conducted in Colombia on OHRQoL in patients with DM2. The contribution to knowledge is aimed at the comprehensive care of patients with esDM2, considering physiological and psychosocial aspects of management. Treatments can be conducted from the perspective of the patient, not only from the health professions and, from public health, it becomes a tool to implement more effective cost- and usefulness-based interventions. Also, the study can be replicated in other populations with chronic non-communicable diseases, including oral health as another fundamental aspect in the general health of people.
MATERIALS AND METHODS
An analytical study was conducted in 2018 with patients with DM2, who had been treated at the MEDICUS Foundation. It is a private health care center, located in the city of Cartagena, Colombia, which provides specialized medical care in diabetes mellitus and comprehensive management of its complications. MEDICUS treats approximately 200 patients diagnosed with DM1 and DM2 per month, most of whom are over 50 years of age. The population served comes to MEDICUS from urban and rural areas of the Cartagena district, 90% and 10%, respectively. The ethnic composition of the patients was: white and mestizo 63.2%, Afro-descendant 36.1%, and Indigenous and other 0.7%.
A total of 152 patients participated, for convenience, according to their availability at the time of the study. They met the following inclusion criteria: being over 18 years old, with a single diagnosis of DM2, not having received dental treatment in the previous three months to assess the impact of the injuries on the OHRQoL, agreeing to participate, and not having had less than two years in MEDICUS. Patients with motor or cognitive disabilities were excluded. All patients received information about the purpose of the study and signed the informed consent indicating that there was no health risk.
First, a questionnaire was designed and applied to investigate sociodemographic variables and quality of life related to oral health, before performing the oral clinical examination. The interviews were conducted by two dental assistants who were unaware of the clinical oral examinations of the patients. The interviewers received training in intonation and command of the questionnaire.
Sociodemographic data were then categorized for statistical analysis as follows: age (≤44; ≥45 years), sex (male; female), occupation (employed; unemployed), health system affiliation (yes; no ), socioeconomic income (measured in terms of the current legal monthly minimum wage [SMMLV] of Colombia, with a standard for this type of evaluation, which corresponds to approximately US$233.78 per month, about COP$908,526 Colombian pesos for the date of completion of this study) (≤ 1 SMMLV; ≥ 2 SMMLV), educational level (low, <10 years of study; high, ≥ 10 years of study), religious affiliation (yes; no), evolution of T2DM (> 5 years; ≤5 years) and pharmacological treatment for T2DM (yes; no). There were questions about general oral changes due to diabetes (yes; no), the type of oral changes (xerostomia, changes in food taste, dysphasia, bleeding on brushing, or halitosis), and habits such as smoking and alcohol consumption.
To assess OHRQoL, the General Oral Health Assessment Index (GOHAI) was used, which was originally developed for older adult populations (16). However, in 1998 it was suggested to extend its use to the general adult population, to measure oral function problems described by patients and to quantify the efficacy of dental treatments, but specifically to estimate the psychological impact associated with oral diseases (18 ).
The GOHAI index provides scores based on responses to 12 questions that ask about reported self-perception of OHRQoL in the past three months (16). Most of the questions are designed on a Likert scale that gives each answer a score ranging from 1 to 5. Questions 1, 2, 4, 6, 8, 9, 10, 11, and 12 display categories Likert from 1 to 5. Questions 3, 5 and 7 display the Likert scale in reverse (19). The associated questions assess three domains of the OHRQoL: physical function (FF), which includes feeding, speaking, and swallowing; psychosocial function (PSF), including oral health worry or worry, dissatisfaction with physical appearance, oral health self-awareness, and avoiding social contact because of oral problems; and pain function (PF), which includes the use of pain- and discomfort-relieving and medications to relieve pain or discomfort in the mouth (20). There are Spanish-language adaptations (18), but for this study the version validated in Colombian Spanish in the adult population was used, which shows excellent psychometric properties (18,19,20).
Two pre-calibrated examiners who were dental graduates performed the oral evaluation of the patients according to the World Health Organization (WHO) guidelines (18,19). All examiners underwent two-hour training sessions, calibration exercises calculating intra- and inter-examiner Kappa values for all clinical conditions with results of 0.90 and 0.85, respectively.
A pilot test of the instruments was conducted with 10 patients with DM2 from the Dental School of the University of Cartagena with sociodemographic characteristics similar to those of the study population. The oral clinical examination described the number of teeth present (≥19 teeth; <19 teeth, according to WHO criteria) (21), presence of retained roots, DMF index (decayed, missing, and filled teeth), presence of gingivitis and periodontitis, presence and types of lesions in hard and soft tissues typical of DM2, use of dental prostheses, temporomandibular disorders (TMD) and salivary characteristics: pH (alkaline; acid) and salivary flow (high; low). Patients were advised to refrain from eating, drinking, chewing gum, smoking and/or rinsing their mouths for one hour before collecting saliva samples for pH assessment using pH 0-14 indicator slides (MQuant® Merck , Darmstadt, Germany). The reading was determined by color change after 5 minutes and compared to the color scale.
Data analysis was performed with the statistical program STATA 11.0 (Stata Corp, College Station, TX, USA), through which absolute and relative frequencies of the total and individual scores of the GOHAI domains were described. Univariate analysis was performed through Poisson regression with robust variance to associate domain scores and GOHAI total score with oral clinical conditions and sociodemographic variables and select variables with a p value ≤0.20 to enter the final adjusted multivariate model. Only those associations with a p value ≤ 0.05 remained in the final model. Relative risks (RR), 95% confidence intervals, and 5% alpha error were calculated.
RESULTS
Most of the patients were in the ≥ 45 years of age range (92.11%); 52.63% were female; 27.63% were unemployed; and 96.05% reported being affiliated with the health care system. 82.24% reported economic income of ≤ 1 SMMLV, 40.13% had ≥ 10 years of schooling, and only 9.21% declared not having religious beliefs. 74.34% of the patients had been diagnosed with DM2 for more than five years.
Regarding the oral diagnosis, 98.68% had missing teeth according to the DMF index and 42.11% had <19 teeth according to the WHO criteria. 48.03% had gingivitis and 32.24% periodontitis. Palatal torus (63.82%) was the most frequent hard tissue feature and geographic tongue was the most frequent soft tissue feature (29.61%). Xerostomia was the main change in the mouth due to DM2 (Table 1).
TABLE 1
Oral Diagnosis and Related Factors of Patients with DM2
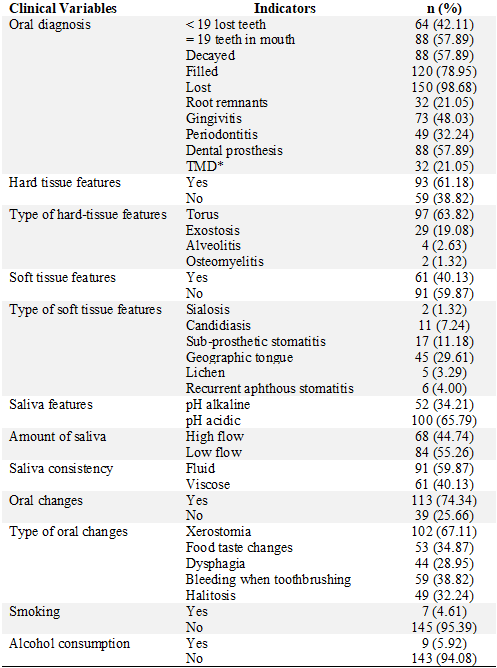
*TMD: Temporo-mandibular disorders.
Source. The authors.
When performing the univariate analysis of the sociodemographic variables, conditions, and oral lesions with the total score and by domains of the GOHAI, the vast majority of the variables showed statistically significant associations (Table 2).
TABLE 2
Univariate Analysis between Sociodemographic Variables and Oral Clinical Conditions Associated with the Total Score and by Domains of the GOHAI
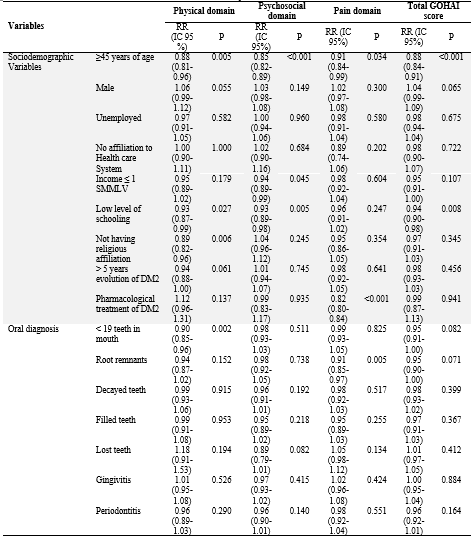
TABLE 2 (cont.)

TABLE 2 (cont.)

Díaz Cárdenas, et al., Quality of Life and Oral Health in Colombians with Diabetes Mellitus 2
*TMD: Temporomandibular disorders.
Source. The authors.
In the multivariate analysis, the variables that best explain the impact of oral health on the quality of life of patients with DM2, according to the total GOHAI score, were: ≥ 45 years of age, < 10 years of schooling, changes in mouth, <19 teeth in the mouth (WHO criteria), periodontitis, sialosis, geographic tongue, sub-prosthetic stomatitis, and low salivary flow (Table 3).
TABLE 3
Multivariate Analysis between Sociodemographic Variables and Oral Clinical Conditions Associated with the Total Score and by GOHAI Domains
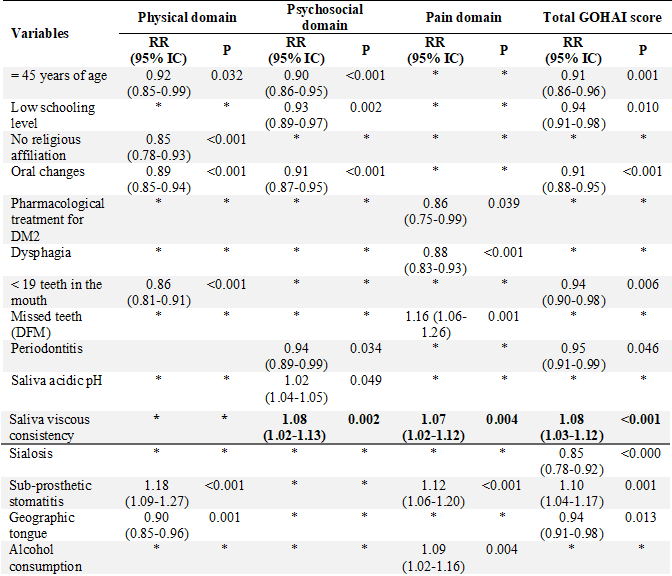
Physical domain: Xi2: 88.97, p < 0.001. Psychosocial domain: Xi2: 85.54, p < 0.001. Pain domain: Xi2: 103.05, p < 0.001. Total score: Xi2: 82.71, p < 0.
Source: the authors.
DISCUSSION
This is one of the first studies in Colombia to estimate the impact of oral conditions and injuries on the quality of life in people with DM2. The GOHAI, which is a reliable instrument previously validated in the Colombian social and cultural context, was used to collect data about oral health (19). Other instruments, such as the OHIP-14, have been used successfully in other contexts to analyze OHRQoL, but there are no studies in Colombia that have validated that instrument (20).
All patients with DM2 showed a negative impact on their OHRQoL. DM2 impacts the oral health of patients, not only in physical function, but also changes their lifestyle and that of their families (21). Oral affections expand their negative impact to other functions, which hinders interpersonal relationships and the patient's emotions (22). Therefore, it is important to create comprehensive interventions for this population, considering their psychosocial needs beyond the disease, especially since it is a chronic degenerative disease. Therefore, it would be worth delving into other aspects that improve their quality of life in general.
The only oral conditions and injuries that showed a negative impact on the total GOHAI scores were sub-prosthetic stomatitis in the physical function and pain domains, and low salivary flow in the psychosocial function and pain domains. The negative impact of sub-prosthetic stomatitis on OHRQoL in patients with DM2 is related to discomfort with the use of prostheses, which may be maladapted and with poor hygiene (23). Removable dentures are a reservoir of microorganisms that favor the proliferation of fungal cells, causing greater inflammation of the oral mucosa (24). This accentuates discomfort, dissatisfaction and, mainly, the perception of pain that reaches moderate to severe levels, and negatively impacts quality of life (25). It is recommended for future studies to evaluate the satisfaction and acceptance of the prosthesis as it can behave as a confounding variable. Likewise, it is suggested to inquire the interest of this type of population in replacing teeth with this type of removable alternative that, although it solves a functional problem, deserves much more care so as not to further complicate the situation of the disease. This would make us think of other types of treatments that can be offered to patients with chronic diseases that can meet all the patient's needs, considering the feasibility of treatments based on the severity and complexity of the disease suffered.
Regarding low salivary flow and its negative impact on OHRQoL, hyposalivation can compromise the chewing function individually and collectively, for example, during social gatherings, making the chewing of dry and hard foods an unpleasant activity, which can generate feelings of fear and trepidation in such meetings (26,27). It would be valuable to know what types of foods are limited or stopped consuming and that can compromise the psychosocial domain of quality of life in patients with DM2. The disease per se generates a modification in the diet to improve its prognosis and course and, if this were added to another modification due to the state of oral health among these patients, there would be a double impact on OHRQoL.
High salivary pH was a variable that negatively impacted only the psychosocial domain. High pH values, in combination with low salivary flow, could contribute to tartar formation (28) and these, in turn, the feeling of hygiene and cleanliness of patients, as well as the clinical presentation of the mouth, which limits some functions such as speech and smiling. The presence or absence of dental tartar was not evaluated, but it is known that gingival inflammation and acidic taste typical of oral alterations, which can be generated by DM2 would modify the enjoyment of food, cause halitosis, and would negatively impact quality of life ( 27).
Other variables showed a positive impact on the total GOHAI score, such as being ≥ 45 years old, low level of schooling (< 10 years of study), changes in the mouth, having < 19 teeth in the mouth (WHO parameter), suffering from periodontitis, and having sialosis and geographic tongue.
A patient over 45 years of age could more maturely accept the emergence of diseases such as diabetes, since many times patients perceive that this also occurs with age changes (29). In the psychosocial domain, having diabetes positively impacts daily activities that would protect the patient, such as exercising and eating a healthy diet (30). Probably in the same sense, having less than 10 years of schooling would generate greater commitment to one's own health by knowing the challenges related to socioeconomic status and, perhaps, people with DM2 would have better attitudes towards self-care (30).
Oral changes, when investigated in a general way, without specifying the type of changes, showed a positive impact on the OHRQoL. It is likely that the patient does not distinguish what kind of changes appear in their mouth due to the disease, but rather appreciates them in a general way and considers them changes related to the disease (30). In this sense, they do not perceive a negative impact; A variable such as the duration of the disease should be studied for a better understanding of diabetes and its management in future studies (29).
Periodontitis had a positive impact on OHRQoL. This may indicate that patients with DM2 are less concerned about their periodontal condition than about other health problems as part of their treatment (30), or they may be aware of the changes related to said disease and do not see it negatively. There are few studies that analyze the knowledge that a patient with DM2 has about their own disease and how they would face these changes, which would shed light, both for the patient themself and for health professionals, regarding the best treatment of the disease.
Regarding other conditions such as sialosis and geographic tongue, there are studies that report how patients with DM2 pay more attention to general health than to oral health (31). The need to solve various problems of the disease can lead to better coping with the impacts of oral health problems or, in fact, to a lower expectation of general health (32).
The missing teeth component, according to the DMF index, had a negative impact on quality of life. However, when the number of teeth was analyzed according to the WHO criteria, having fewer than 19 teeth in the mouth had a positive impact on the total GOHAI score and physical function, which explains that, regardless of the number of missing teeth , this can affect people. Dentists are always attentive to restoring the oral health of their patients, but to what extent do patients perceive such a need? The OHRQoL studies offer valid information when offering restorative treatments based on the patient's own perceptions.
Thus, Schmalz, et al. (33), in their study conducted on adults, indicated that having at least 10 teeth in the mouth is a protective factor for oral health. However, these results and those found in this study do not discriminate with respect to the position of the missing teeth, which would allow knowing if the impact is related to the position of the missing tooth and that it generates different perceptions of the impact of oral health on quality of life. Some studies show that the loss of teeth in the frontal area has a negative impact on quality of life, by compromising physical appearance and social relationships. For this reason, it is recommended to include this variable for future studies (34).
The alcohol consumption variable had a negative impact on the pain domain. Bijlsma-Rutte, et al. (35), establish that the harmful effects that alcohol generates for good glycemic control and the person's feeling of guilt, after consuming it, may be influenced by other variables. Carvalho, et al. (37), speak of the existence of cultural components that favor high alcohol consumption in people who live in hot places, as is the case of the patients in this study who lived in the city of Cartagena, Colombia. In this city with a hot climate, alcohol consumption is a pattern of behavior to face high temperatures, it is part of social events and it is consumed with high frequency, even on certain days of the week, due to cultural traditions, such as Sundays, which can complicate the prognosis of DM2.
Worldwide, specifically in Colombia, approximately 48 % of the population over 15 years of age consume alcohol (36,37), a situation that from the perspective of public health represents a risk, not only for the emergence of diseases but also for their treatment and control. It would be worth investigating the cultural practices that could complicate the prognosis of some diseases such as DM2, the perception and importance that patients have of self-care in health and whether, in certain cases, greater importance is given to enjoyment and pleasure than to health as a possible antonym of enjoyment.
This study has several limitations that should be carefully considered when interpreting the results. The cross-sectional design does not allow inferences to be made regarding the direction of the observed associations or the selection of patients belonging to the same private institution (MEDICUS Foundation). This could represent a bias regarding the positive perceptions reported in relation to some variables, probably due to the education and prevention activities received.
CONCLUSIONS AND RECOMMENDATIONS
Sub-prosthetic stomatitis and low salivary flow showed a negative impact on OHRQoL in patients with DM2 from the city of Cartagena de Indias, Colombia, while other conditions such as periodontitis, geographic tongue, sialosis and having <19 teeth in mouth presented a positive impact.
These results can guide health professionals, specifically those of the MEDICUS Foundation, towards interventions that seek not only the patients’ physical care, but also biopsychosocial well-being in relation to their oral health status. This will make it possible to optimize resources and seek health care from the perceptions of the patients and not of the treating professionals.
It is recommended to include other professionals, such as psychologists and social workers, as well as social activities that allow inquiring about social and family situations experienced by patients. These are activities that can complement the treatment conducted in these populations and include the family as a protective nucleus against the disease.
This type of studies promotes the joint, transdisciplinary, and articulated work of the medical professional with other health professionals such as the general dentist and the specialist (e.g., oral rehabilitator, periodontist, and endodontist) in search of the best solution for oral problems that a patient with DM2 may present and have an impact on their quality of life.
REFERENCES
1. Carrillo-Larco RM, Pearson-Stuttard J, Bernabe-Ortiz A, Gregg EW. The Andean Latin-American burden of diabetes attributable to high body mass index: A comparative risk assessment. Diabetes Res Clin Pract. 2020 Feb; 160: 107978. https://doi.org/10.1016/j.diabres.2019.107978
2. Guariguata L, Whiting DR, Hambleton I, Beagley J, Linnenkamp U, Shaw JE. Estimaciones mundiales de la prevalencia de diabetes para 2013 y proyecciones para 2035. Inv Práctica Clín Diabetes. 2014 fe; 103(2): 137-149. https://doi.org/10.1016/j.diabres.2013.11.002137-49.
3. Avilés-Santa ML, Monroig-Rivera A, Soto-Soto A, Lindberg NM. Current state of diabetes mellitus prevalence, awareness, treatment, and control in Latin America: challenges and innovative solutions to improve health outcomes across the continent. Curr Diab Rep. 2020 Oct; 20(11):62. https://doi.org/10.1007/s11892-020-01341-9
4. Camacho PA, Gomez-Arbelaez D, Otero J, González-Gómez S, Molina DI, Sanchez G, Arcos E, Narvaez C, García H, Pérez M, Hernandez-Triana E, Duran M, Cure C, Sotomayor A, Rico A, Cotes F, Rangarajan S, Yusuf S, López-Jaramillo P. Self-reported prevalence of chronic non-communicable diseases in relation to socioeconomic and educational factors in Colombia: a community-based study in 11 departments. Glob Heart. 2020 Apr 21; 15(1): 35. https://doi.org/10.5334/gh.792
5. Simpson TC, Weldon JC, Worthington HV, Needleman I, Wild SH, Moles DR, Stevenson B, Furness S, Iheozor-Ejiofor Z. Treatment of periodontal disease for glycaemic control in people with diabetes mellitus. Cochrane Database Syst Rev. 2015 Nov 6; (11): CD004714. https://doi.org/10.1002/14651858
6. Porto I, Díaz S. Repercusiones de la salud bucal sobre calidad de vida por ciclo vital individual. Acta Odontol Col. 2017 Jul; 7(2): 49-64. http://www.revistas.unal.edu.co/index.php/actaodontocoll
7. Khalifa N, Rahman B, Gaintantzopoulou MD, Al-Amad S, Awad MM. Oral health status and oral health-related quality of life among patients with type 2 diabetes mellitus in the United Arab Emirates: a matched case-control study. Health Qual Life Outcomes. 2020 Jun 15; 18(1): 182. https://doi.org/10.1186/s12955-020-01418-9
8. Atchison KA, Dolan TA. Development of the Geriatric Oral Health Assessment Index. J Dent Educ. 1990 Nov; 54(11): 680-687.
9. Cerón-Bastidas XA. Relación de calidad de vida y salud oral en la población adolescente. Rev CES Odontol. Jun 2018; 31(1): 38-46. http://dx.doi.org/10.21615/cesodon.31.1.4
10. Valladales-Restrepo LF, Machado-Alba JE. Potentially inappropriate anticholinergic drug prescriptions for patients with Sjögren's syndrome. J Transl Autoimmun. 2019 Jun 27; 2: 100007. http://dx.doi.org/10.1016/j.jtauto.2019.100007
11. Botero JE, Rodríguez C, Agudelo-Suarez AA. Periodontal treatment and glycaemic control in patients with diabetes and periodontitis: an umbrella review. Aust Dent J. 2016 Jun; 61(2): 134-48. http://dx.doi.org/10.1111/adj.12413
12. Vázquez Machado A, Mukamutara J. Depresión en pacientes con diabetes mellitus y su relación con el control glucémico. MEDISAN. 2020; 24(5): 847-860.
13. Concha-Sanchez SC. Relación de la salud oral con las enfermedades crónicas en las personas mayores: una revisión. Rev USTASalud Odontol. 2006 May; 5: 49–63 https://doi.org/10.15332/us.v5i1.1822
14. de Miguel-Infante A, Martinez-Huedo MA, Mora-Zamorano E, Hernández-Barrera V, Jiménez-Trujillo I, de Burgos-Lunar C, Cardenas Valladolid J, Jiménez-García R, Lopez-de-Andrés A. Periodontal disease in adults with diabetes, prevalence and risk factors. Results of an observational study. Int J Clin Pract. 2018 Nov 16: e13294. https://doi.org/10.1111/ijcp.13294
15. Walker RJ, Smalls BL, Campbell JA, Strom Williams JL, Egede LE. Impact of social determinants of health on outcomes for type 2 diabetes: a systematic review. Endocrine. 2014 Sep; 47(1): 29-48. https://doi.org/10.1007/s12020-014-0195-0
16. Castaño J, Ortega A, Ortega J, Palacios JM, Contreras A. Diabetes mellitus tipo 1 y condición periodontal. Rev Nal Odontol. 2014; 10(18): 7-14. https://doi.org/10.16925/od.v10i18.716
17. Rodríguez-Medina C, Agudelo-Suárez AA, Botero JE. Weak evidence hinders the understanding of the benefits of periodontal therapy on glycemic control in patients with diabetes and periodontitis. J Evid Based Dent Pract. 2016 Dec; 16(4): 236-238. https://doi.org/10.1016/j.jebdp.2016.11.005
18. Aguirre-Bustamante J, Barón-López FJ, Carmona-González FJ, Pérez-Farinós N, Wärnberg J. Validation of a modified version of the Spanish Geriatric Oral Health Assessment Index (GOHAI-SP) for adults and elder people. BMC Oral Health. 2020 Feb 19; 20(1): 61. https://doi.org/10.1186/s12903-020-1047-3
19. Gutiérrez Quiceno B, Calzada Gutiérrez MT, Fandiño-Losada A. Cultural adaptation and validation of the Geriatric Oral Health Assessment Index - GOHAI - Colombian version. Colomb Med (Cali). 2019 Jun 30; 50(2): 102-114. https://doi.org/10.25100/cm.v50i2.3999
20. Fuentes-García A, Lera L, Sánchez H, Albala C. Oral health-related quality of life of older people from three South American cities. Gerodontol. 2013 Mar; 30(1): 67-75. https://doi.org/10.1111/j.1741-2358.2012.00649.x
21. Organización Mundial de la Salud (OMS). Ficha de datos de salud bucal 2018. Ginebra: OMS; 2018.
22. Petersen PE, Baez RJ, Ogawa H. Global application of oral disease prevention and health promotion as measured 10 years after the 2007 World Health Assembly statement on oral health. Community Dent Oral Epidemiol. 2020 Aug; 48(4): 338-348. https://doi.org/10.1111/cdoe.12538
23. Ferreira RC, Kawachi I, Souza JGS, Campos FL, Chalub LLFH, Antunes JLF. ¿La dentición reducida con y sin prótesis dental está asociada con la calidad de vida relacionada con la salud oral? Un estudio transversal. Resultados de calidad de vida en salud. Health Quality Life Outcomes. 2019; 17(1): 79 https://doi.org/10.1186/s12955-019-1149-2
24. Montero J, Castillo-Oyagüe R, Lynch CD, Albaladejo A, Castaño A. Self-perceived changes in oral health-related quality of life after receiving different types of conventional prosthetic treatments: a cohort follow-up study. J Dent. 2013 Jun; 41(6): 493-503. https://doi.org/10.1016/j.jdent.2013.01.006
25. Yen YY, Lee HE, Wu YM, Lan SJ, Wang WC, Du JK, Huang ST, Hsu KJ. Impact of removable dentures on oral health-related quality of life among elderly adults in Taiwan. BMC Oral Health. 2015 Jan 5; 15: 1. https://doi.org/10.1186/1472-6831-15-1
26. Hahnel S, Schwarz S, Zeman F, Schäfer L, Behr M. Prevalence of xerostomia and hyposalivation and their association with quality of life in elderly patients in dependence on dental status and prosthetic rehabilitation: a pilot study. J Dent. 2014 Jun; 42(6): 664-70. https://doi.org/10.1016/j.jdent.2014.03.003
27. Atchison KA, Der-Martirosian C, Gift HC. Components of self-reported oral health and general health in racial and ethnic groups. J Public Health Dent. 1998 Fall; 58(4): 301-308. https://doi.org/10.1111/j.1752-7325.1998.tb03013.x
28. Lima DLF, Carneiro SDRM, Barbosa FTS, Saintrain MVL, Moizan JAH, Doucet J. Salivary flow and xerostomia in older patients with type 2 diabetes mellitus. PLoS One. 2017 Aug 2; 12(8): e0180891. https://doi.org/10.1371/journal.pone.0180891
29. Cervino G, Terranova A, Briguglio F, De Stefano R, Famà F, D'Amico C, Amoroso G, Marino S, Gorassini F, Mastroieni R, Scoglio C, Catalano F, Lauritano F, Matarese M, Lo Giudice R, Nastro Siniscalchi E, Fiorillo L. Diabetes: Oral health related quality of life and oral alterations. Biomed Res Int. 2019 Mar 18; 2019: 5907195. https://doi.org/10.1155/2019/5907195
30. Brown AF, Ettner SL, Piette J, Weinberger M, Gregg E, Shapiro MF, Karter AJ, Safford M, Waitzfelder B, Prata PA, Beckles GL. Socioeconomic position and health among persons with diabetes mellitus: a conceptual framework and review of the literature. Epidemiol Rev. 2004; 26: 63-77. https://doi.org/10.1093/epirev/mxh002
31. Irani FC, Wassall RR, Preshaw PM. Impact of periodontal status on oral health-related quality of life in patients with and without type 2 diabetes. J Dent. 2015 May; (5): 506-11. https://doi.org/10.1016/j.jdent.2015.03.001
32. Niesten D, van Mourik K, van der Sanden W. The impact of frailty on oral care behavior of older people: a qualitative study. BMC Oral Health. 2013 Nov 1; 13: 61. https://doi.org/10.1186/1472-6831-13-61
33. Schmalz G, Schiffers N, Schwabe S, Vasko R, Müller GA, Haak R, Mausberg RF, Ziebolz D. Dental and periodontal health, and microbiological and salivary conditions in patients with or without diabetes undergoing haemodialysis. Int Dent J. 2017 Jun; 67(3): 186-193. https://doi.org/10.1111/idj.12282
34. Schmalz G, Noack S, Patschan S, Patschan D, Müller GA, Rupprecht A, Schmickler J, Haak R, Ziebolz D. Disease activity, morning stiffness and missing teeth are associated with oral health-related quality of life in individuals with rheumatoid arthritis. Clin Oral Investig. 2020 Oct; 24(10): 3559-3566. https://doi.org/10.1007/s00784-020-03226-3
35. Bijlsma-Rutte A, Rutters F, Elders PJM, Bot SDM, Nijpels G. Socio-economic status and HbA1c in type 2 diabetes: A systematic review and meta-analysis. Diabetes Metab Res Rev. 2018 Sep; 34(6): e3008. https://doi.org/10.1002/dmrr.3008
36. Whiteford HA, Degenhardt L, Rehm J, Baxter AJ, Ferrari AJ, Erskine HE, Charlson FJ, Norman RE, Flaxman AD, Johns N, Burstein R, Murray CJ, Vos T. Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010. Lancet. 2013 Nov 9; 382(9904): 1575-1586. https://doi.org/10.1016/S0140-6736(13)61611-6
37. Carvalho AF, Heilig M, Perez A, Probst C, Rehm J. Alcohol use disorders. Lancet. 2019 Aug 31; 394(10200): 781-792. https://doi.org/10.1016/S0140-6736(19)31775-1
Notes
*
Original research.
Author notes
Authors’ Note:aCorrespondence: sdiazc@unicartagena.edu.co; cvergarah@unicartagena.edu.co; jabruges@gmail.com; mespitaleta08@gmail.com
Additional information
How to cite this article: Díaz Cárdenas S, Vergara Hernández CI, Brugés Ruiz JA, Espitatela Mejía MC. Quality of Life and Oral Health in Colombian Patients with Type 2 Diabetes Mellitus. Univ Odontol. 2021; 40. https://doi.org/10.11144/Javeriana.uo40.qloh