INTRODUCTION
Enamel is a highly mineralized dental tissue, organized, and structured in hydroxyapatite crystals. It is secreted by ameloblasts in a protein-containing organic matrix. Because it is an acellular tissue, enamel does not have the capacity to repair itself when it is altered extrinsically or intrinsically (1). Alterations of enamel development can cause amelogenesis imperfecta (AI), a widespread hereditary condition that affects the structure of dental enamel of deciduous and permanent dentitions in quantity and quality (2).
The color of the teeth in people with AI varies according to the phenotype and occurs in different shades from light yellow to brown. Patients experience high sensitivity to thermal changes during the intake of beverages and food, which does not allow them to have adequate oral hygiene habits, causing a greater predisposition to cavities, dental fractures, and tooth loss (3). AI patients, due to aesthetic alterations, may suffer from low self-esteem (2). AI is caused by mutations in genes such as AMEL (amelogenin), ENAM (enamelin), MMP20 (matrix metalloproteinase-20), and KLK4 (kallikrein-4), which code for proteins involved in the formation of tooth enamel (4,5,6,7,8 ), and FAM83H, a gene that codes for a protein apparently involved in the organization of ameloblast desmosomes (9). AI has also been associated with other clinical alterations such as dental agenesis, taurodontism, and anterior open bite, and systemic alterations such as nephrocalcinosis, tricho-dento-osseous syndrome and Jalili syndrome (10,11,12,13).
AI is classified according to its phenotype and mode of inheritance into 14 subtypes. Based on the phenotype, it is classified as hypoplastic, hypocalcified, hypomadurative, and hypomadurative-hypoplastic with taurodontism. According to its inheritance pattern, AI is classified as autosomal dominant, autosomal recessive, and linked to the X chromosome (14). Radiographic examination of some phenotypes may show lack of contrast between enamel and dentin. It is also possible to observe some associated anomalies that are not clinically visible, such as pulp calcifications, dental agenesis, and apical dilacerations (15).
Research on the prevalence of AI is limited. In the international context, studies carried out in Switzerland by Backman and Holm (1986) stand out. They found 1:700 individuals affected with AI (16). The proportion of impacts was 1:14,000-1:16,000 in the United States (14), 1:8,000 in Israel (Jerusalem) (17) and 1:10,000 in Pakistan (18).
In Colombia, clinical and molecular studies of AI in families have been carried out. Different phenotypic, dental, and skeletal characteristics have been found, as well as genes involved with this anomaly (19,20,21,22,23). However, to date, prevalence studies have been limited to describing developmental enamel defects, such as hypoplasia, hypomineralization, and opacities (24,25,26,27). Even in the 4th National Oral Health Study (ENSAB IV, 2013-2014) (28), AI was not specifically reported. For this reason, it is relevant to know the frequency, magnitude, and distribution of this pathology and its behavior in the different regions of the country. The research question of this study was: What is the prevalence of AI in Colombian patients who attended the dental clinics of the Pontificia Universidad Javeriana from Bogotá, between January 2015 and December 2017? This prevalence study is the first one carried out in Colombia on AI. The findings provide initial evidence to plan preventive actions for caries, periodontal disease, and associated complications, and corrective actions to improve functionality and aesthetics (16). They also represent the basis to carry out similar studies in other Colombian regions.
MATERIALS AND METHODS
This is a descriptive study with retrospective cross-sectional observational design. The study was approved by the Ethics and Research Committee of the Pontificia Universidad Javeriana’s Dental School, through Resolution OD-0218 of 28 July 2017, minute 010B. It adheres to the standards of Resolution 008430 of 1993 and Resolution 2378 of 2008, according to which it was classified as a risk-free study.
Population and Sample
The reference population was taken from the medical records of patients treated at the undergraduate and graduate clinics of the Pontificia Universidad Javeriana’s Dental School, between January 2015 and December 2017. The sample size was determined with a confidence of the 95 % and 80 % power. It started by assuming an unknown prevalence (50%), since the reported prevalence of the event of 1:14,000 comes from an Anglo-Saxon population (14). In accordance with this, a sample of 1,394 medical records was taken.
Clinical records of patients 5 years of age and older were included, taking into account that AI occurs in both dentitions. Likewise, criteria such as completion of the clinical records, their approval by the instructor in charge, informed consents filled out and signed, and radiographic examinations were included. The medical records of patients with syndromes and those of patients diagnosed with total absence of teeth (anodontia) were excluded.
AI-related variables analyzed as dependent variables, in terms of presence and absence, followed Witkop (1988) (14) classification criteria (Table 1). Sociodemographic factors such as age, sex, and origin were considered as independent variables. Similarly, radiographic findings related to taurodontism, enamel-dentin contrast, dental agenesis, presence of microdontia, macrodontia and pulp calcifications were included. The presence or absence of a family history of AI and other alterations of tooth structure such as hypoplasias were evaluated as independent variables. The genetic factor and the consumption of any antibiotic during childhood were taken into account as confounding variables.
Table 1
AI Classification according to Witkop & Sauk, 1988*
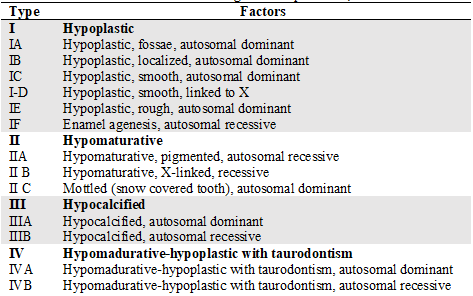
*This classification system is the most widely accepted to date, which considers the inheritance pattern of the disorder, as well as its specific phenotypic characteristics.
Training Process for Diagnostic Unification
With prior authorization of access to reviewing clinical records and respecting the confidentiality of diagnoses and paraclinical examinations, medical records were randomly selected, using the Microsoft Excel 2016® selection program. The examiner (graduate students) training process in identifying the diagnosis of AI was carried out in three stages: homogenization of the theoretical criteria; observation; and discussion of them. This process was carried out using digital photographs and panoramic radiographs of children and adolescents with AI, on which each phenotype and mode of inheritance of this alteration was analyzed and described based on the Witkop 1988 classification (14) (Table 1). Subsequently, the homogeneity of the observation was determined by means of files selected by the main researcher (training, Universidad de Chile, 2010), in which 50 panoramic images and radiographs of patients with AI were analyzed, thus evaluating the similarity and variability from what was observed among the researchers in this study. Of the 1,394 records reviewed for this study, 5 patients with a previous diagnosis of AI were reevaluated.
Data Collection from Medical Records
Data collected from the medical records were based on both the odontogram and the final diagnosis and was recorded in tailored formats designed for this study (Figures 1 and 2). Afterwards, the data obtained were digitized into a database designed in Excel 2016. The data analysis was performed through the IBM® SPSS Statistics® V22 program. To determine the prevalence of AI, as well as to estimate the percentage of occurrence of other dental alterations, a descriptive analysis was carried out. An inferential analysis according to sex, age by decade, and origin in relation to the presence of other dental anomalies was carried out, using the Chi-square test / Fisher's exact test (p <0.05).
 Figure 1
Clinical Record Format for AI designed for this Study
Figure 1
Clinical Record Format for AI designed for this Study
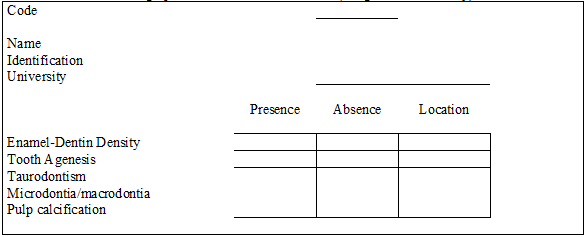 Figure 2
Radiographic Assessment Form for AI (designed for this study)
Figure 2
Radiographic Assessment Form for AI (designed for this study)
RESULTS
Clinical Record Data Analysis
Prevalence. The prevalence of AI in patients who attended the dental clinics of Pontificia Universidad Javeriana from Bogotá was assessed between January 2015 and December 2017. Of the total medical records (n = 1,394), 8 were found with a diagnosis of AI (0.6 %) (Table 2). Of the 8 people diagnosed with AI, 7 had a hypoplastic phenotype and 1 had a hypocalcified one.
Table 2
Prevalence of AI and Associated Dental Anomalies in the Population Studied (Guide Chart)
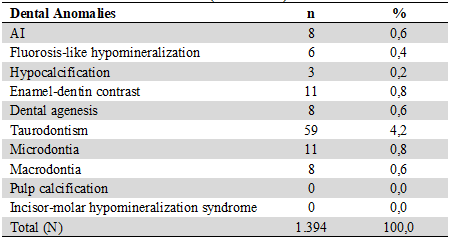
Source: the authors.
Sociodemographic Characteristics
Among the sociodemographic characteristics of the analyzed population, 55.31 % were female (n = 771) and 44.69% (n = 623) male. Regarding patients diagnosed with AI, based on the Witkop classification (1988) (14) (table 1), no statistically significant differences or trends were observed with respect to sex (1:1 ratio) (Table 3).
Table 3
Distribution by Sex of Dental Anomalies associated with AI
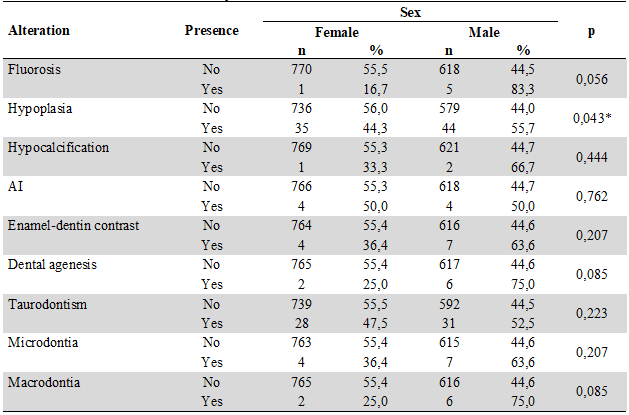
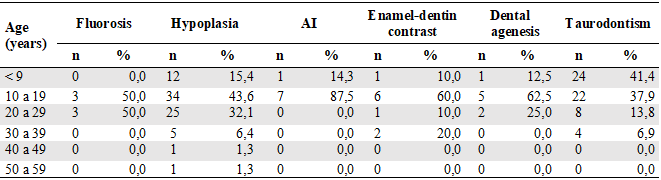
Regarding the origin, 7 patients (87.50 %) who presented AI came from the urban area and one from the dispersed rural area. Regarding the age distribution, the subjects affected by AI were in the age range of 10-19 years (87.5 %; n = 7) (Table 4).
Table 4
Distribution of Dental Pathologies analyzed by Age
Dental Anomalies
In the population analyzed, the 8 patients with a diagnosis of AI (0.6 %) had a higher frequency of dental anomalies related to enamel hypoplasia (n = 7; 87.50 %), according to which a lack of contrast between enamel and dentin in 6 (75 %) and taurodontism in all (100 %). Alterations such as dental agenesis, microdontia, macrodontia, or pulp calcifications were not described (Table 5). On the other side, the population had a higher frequency of dental anomalies related to enamel hypoplasia in 5.7 % and taurodontism in 4.2 %.
Table 5
Distribution of Dental Conditions in Presence of AI
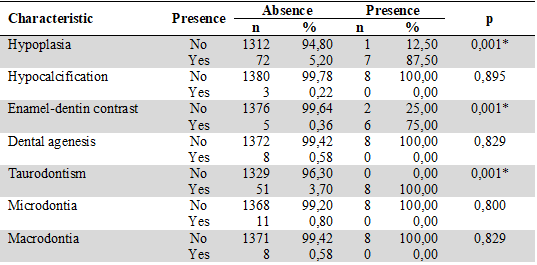
*Statistically significant differences.
Source: the authors. Importar tabla
Radiographic Characteristics
The analysis of radiographic characteristics in patients with AI showed lack of contrast between enamel and dentin in 6 patients (75 %) and taurodontism in 8 (100 %). No dental agenesis or alterations in tooth size (microdontia or macrodontia) were observed (Table 6). In the population of study, taurodontism was the most frequent anomaly (3.7%), although it was not statistically significant.
Table 6
Distribution of Radiographic Characteristics Assessed Regarding Presence of AI
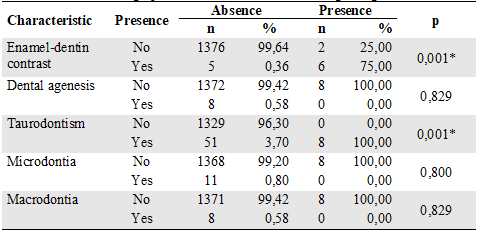
*Statistically significant differences
Source: the authors.
Other findings observed among people diagnosed with AI included one (12.5 %) with a history of antibiotic intake in their first year of life. Likewise, 62.5 % reported having a family history of AI (Table 7).
Table 7
History of Antibiotic Intake and AI in the Family Regarding Present Pathologies (Percentages)
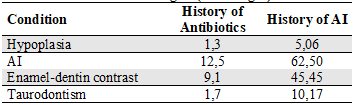
Source: the authors
DISCUSSION
This study aimed to determine the prevalence of AI in patients who attended the clinics of the Pontificia Universidad Javeriana’ Dental School from Bogotá, between January 2015 and December 2017. 1,394 medical records were analyzed. To date, few studies describe the prevalence of AI in some populations (14,16,17,18). Shokri et al. (2014) (18) evaluated the prevalence of all types of dental anomalies in 1,640 Iranians, including AI, aged between 7 and 35 years, by means of panoramic radiographs. They found a prevalence of AI of 0.24 %, that is, 4 individuals.
Gupta et al. (2011) (29) reported a prevalence of 0.27 % in 3 people in the Indian population. More recently, Harini & Don (2019) (30), in the same population, reported a prevalence of 0.6 %. In the present study, the prevalence of AI in the Colombian population was also 0.6 %. Such data coincide with those found by Witkop et al. (1988), Shokri et al. (2014), and Gupta et al. (2014) (14,18,29). However, the prevalence is lower than that described in studies from Switzerland (16) and Jerusalem (17).
Regarding age, it was found that AI was diagnosed in the group aged 10 to 19 years, n = 8 (Table 4). This finding coincides with that described in studies of populations from Switzerland (16), Michigan (14), and Jerusalem (17). This could suggest that, at these ages, since permanent teeth are erupting or already erupted, the AI is more visible since this pathology is more serious in permanent teeth than in temporary ones. This aspect could suggest that AI in primary teeth sometimes goes unnoticed and may be underdiagnosed. On the other hand, it is also possible that a differential diagnosis has not been made with other enamel defects such as incisor-molar hypomineralization and fluorosis.
In this study, 7 patients presented hypoplastic phenotype (87.50 %) and one hypocalcified (Table 2). This suggests that the hypoplastic phenotype could influence its mainly autosomal dominant segregation, in which the enamel formation process (amelogenesis) is interrupted in the first stage (secretory). Likewise, the presence of a family history of AI was understood as an important sociodemographic factor since it is a hereditary disorder (2).
On the other hand, the 8 individuals affected by AI came from the lower-middle socioeconomic background and their origin was mainly urban. This could suggest that environmental aspects could be part of the etiology of AI. For example, taking antibiotics was found in 12.5 % of cases (Table 7). More specific studies must be carried out to clarify whether antibiotics play a role in the etiology of AI.
The Colombian population analyzed in this study was represented in its majority (55.31 %) by the female sex (n = 771), although the reported cases of AI showed a 1:1 relationship in both sexes (Table 3). The same was observed in clinical and molecular studies carried out in Colombians (19,22), in which AI has presented indistinctly in men and women, especially the hypoplastic phenotype, which was one of the most frequent in these studies. These findings also coincide with those of Gupta et al. (2011) (29) in Indian population, who evaluated 1,123 patients, 572 men and 551 women. They found that two men and one woman were affected by AI. Similarly, Shokri et al. (2014) (18) and Harini & Don (2019) (19), in Indian population, found a total of 4 people (2 men and 2 women) affected by AI.
Regarding the contrast between enamel and dentin, in the present study an absence of said contrast was evidenced in patients with hypoplastic AI (75 %), a characteristic that is more marked in the hypocalcified phenotype that was identified in 1 of the 8 individuals who presented AI. Another relevant radiographic characteristic was taurodontism, which was observed in all patients affected by AI. However, despite taurodontism being described more frequently than other abnormalities studied (3.7 %), the differences were not statistically significant (Table 6). These results coincide with those of Collins et al. (1999) (10), who analyzed dental anomalies associated with AI in panoramic radiographs. They found that in people with AI, taurodontism was present in 9 of 23 (39 %), a proportion that is similar to that of individuals without AI (10 of 24 cases, 42%).
Similarly, it was observed that in patients affected by AI with a hypoplastic phenotype, the enamel density was quantitatively lower than in those with a hypocalcified phenotype. This was also reported by Witkop in 1988 (14), who showed that the density in the hypoplastic phenotype is highly variable in its mineral content, while in the hypocalcified one this decrease is more constant.
Finally, this study is the first approximation to determine the prevalence of AI and, in turn, of dental anomalies in a Colombian population of patients from the dental clinics of the Pontificia Universidad Javeriana from Bogotá in a period of two years. The data collected allow us to see a trend in the distribution of AI and provide the basis for further studies with a larger population to implement preventive actions and establish therapeutic programs involving different disciplines.
CONCLUSIONS
A prevalence of 0.6 % (n = 8) of AI was found in Colombian patients who attended the dental clinics of the Pontificia Universidad Javeriana from Bogotá, attended between January 2015 and December 2017. This prevalence is similar to that described in other populations.
This is the first study of the prevalence of AI carried out in Colombia and shows a trend in magnitude, frequency, and distribution, as well as associated characteristics of this pathology. Taurodontism was the most frequent associated characteristic (100 %).
No predilection for AI was identified with respect to the sex variable.
Family history was important as AI presented more frequently in an autosomal dominant form, closely related to the hypoplastic phenotype.
RECOMMENDATIONS
Continue conducting AI prevalence studies with a larger population that includes different regions of Colombia.
Include this pathology in the National Oral Health Studies of Colombia.
Perform updates in the unification of diagnostic criteria for AI with respect to phenotype and associated dental and skeletal abnormalities bearing in mind this pathology can often be underdiagnosed.
Conduct trainings on differential diagnosis criteria with other enamel defects (hypomineralization, hypoplasia, incisor-molar syndrome and fluorosis).
Acknowledgments
To the Pontificia Universidad Javeriana, the Dental School, and the Center for Dental Research (Centro de Investigaciones Odontológicas—CIO), for the logistical support and funding of this project.
This study was approved by the ethics and research committee of the Pontificia Universidad Javeriana’s Dental School, through resolution OD-0218 of July 28, 2017, minute 010B, within the framework of the line of research in amelogenesis imperfecta.
REFERENCES
1. Wright J. The molecular etiologies and associated phenotypes of amelogenesis imperfecta. Am J Med Genet A. 2006 Dec 1; 140(23): 2547-2555.
2. Wright JT, Torain M, Long K, Seow K, Crawford P, Aldred MJ, Hart PS, Hart TC. Amelogenesis imperfecta: genotype-phenotype studies in 71 families. Cells Tissues Organs. 2011; 194(2-4): 279-83. https://doi.org/10.1159/000324339
3. Gadhia K, McDonald S, Arkutu N, Malik K. Amelogenesis imperfecta: an introduction. Br Dent J. 2012 Apr 27; 212(8): 377-379. https://doi.org/10.1038/sj.bdj.2012.314.
4. Wright JT, Hart PS, Aldred MJ, Seow K, Crawford PJ, Hong SP, Gibson CW, Hart TC. Relationship of phenotype and genotype in X-linked amelogenesis imperfecta. Connect Tissue Res. 2003; 44(Suppl 1): 72-78.
5. Hu JC, Yamakoshi Y. Enamelin and autosomal-dominant amelogenesis imperfecta. Crit Rev Oral Biol Med. 2003; 14(6): 387-398. https://doi.org/10.1177/154411130301400602
6. Rajpar MH, Harley K, Laing C, Davies RM, Dixon MJ. Mutation of the gene encoding the enamel-specific protein, enamelin, causes autosomal-dominant amelogenesis imperfecta. Hum Mol Genet. 2001 Aug 1; 10(16): 1673-1677. https://doi.org/10.1093/hmg/10.16.1673
7. Kim JW, Simmer JP, Hart TC, Hart PS, Ramaswami MD, Bartlett JD, Hu JC. MMP-20 mutation in autosomal recessive pigmented hypomaturation amelogenesis imperfecta. J Med Genet. 2005 Mar; 42(3): 271-5. https://doi.org/10.1136/jmg.2004.024505
8. Hart PS, Hart TC, Michalec MD, Ryu OH, Simmons D, Hong S, Wright JT. Mutation in kallikrein 4 causes autosomal recessive hypomaturation amelogenesis imperfecta. J Med Genet. 2004 Jul; 41(7): 545-549. https://doi.org/10.1136/jmg.2003.017657
9. Wang SK, Zhang H, Hu CY, Liu JF, Chadha S, Kim JW, Simmer JP, Hu JCC. FAM83H and autosomal dominant hypocalcified amelogenesis imperfecta. J Dent Res. 2021 Mar; 100(3): 293-301. https://doi.org/10.1177/0022034520962731.
10. Collins MA, Mauriello SM, Tyndall DA, Wright JT. Dental anomalies associated with amelogenesis imperfecta: a radiographic assessment. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999 Sep; 88(3): 358-364. https://doi.org/10.1016/s1079-2104(99)70043
11. Ravassipour DB, Powell CM, Phillips CL, Hart PS, Hart TC, Boyd C, Wright JT. Variation in dental and skeletal open bite malocclusion in humans with amelogenesis imperfecta. Arch Oral Biol. 2005 Jul; 50(7): 611-623. https://doi.org/10.1016/j.archoralbio.2004.12.003.
12. Seow WK. Taurodontism of the mandibular first permanent molar distinguishes between the tricho-dento-osseous (TDO) syndrome and amelogenesis imperfecta. Clin Genet. 1993 May; 43(5): 240-246. https://doi.org/10.1111/j.1399-0004.1993.tb03810.x
13. Zhang H, Koruyucu M, Seymen F, Kasimoglu Y, Kim JW, Tinawi S, Zhang C, Jacquemont ML, Vieira AR, Simmer JP, Hu JCC. WDR72 Mutations Associated with Amelogenesis Imperfecta and Acidosis. J Dent Res. 2019 May; 98(5): 541-548. https://doi.org/10.1177/0022034518824571
14. Witkop CJ Jr. Amelogenesis imperfecta, dentinogenesis imperfecta and dentin dysplasia revisited: problems in classification. J Oral Pathol. 1988 Nov; 17(9-10): 547-553. https://doi.org/10.1111/j.1600-0714.1988.tb01332.x
15. Sabandal MM, Schäfer E. Amelogenesis imperfecta: review of diagnostic findings and treatment concepts. Odontology. 2016 Sep; 104(3): 245-256. https://doi.org/10.1007/s10266-016-0266-1. Epub 2016 Aug 22.
16. Bäckman B. Amelogenesis imperfecta--clinical manifestations in 51 families in a northern Swedish county. Scand J Dent Res. 1988 Dec; 96(6): 505-516. https://doi.org/10.1111/j.1600-0722.1988.tb01590.x.
17. Chosack A, Eidelman E, Wisotski I, Cohen T. Amelogenesis imperfecta among Israeli Jews and the description of a new type of local hypoplastic autosomal recessive amelogenesis imperfecta. Oral Surg Oral Med Oral Pathol. 1979 Feb; 47(2): 148-156. https://doi.org/10.1016/0030-4220(79)90170-1.
18. Shokri A, Poorolajal J, Khajeh S, Faramarzi F, Kahnamoui HM. Prevalence of dental anomalies among 7- to 35-year-old people in Hamadan, Iran in 2012-2013 as observed using panoramic radiographs. Imaging Sci Dent. 2014 Mar; 44(1): 7-13. https://doi.org/10.5624/isd.2014.44.1.7.
19. Gutierrez SJ, Chaves M, Torres DM, Briceño I. Identification of a novel mutation in the enamalin gene in a family with autosomal-dominant amelogenesis imperfecta. Arch Oral Biol. 2007 May; 52(5): 503-506. https://doi.org/10.1016/j.archoralbio.2006.09.014
20. Calero J, Soto L. Amelogénesis imperfecta. Informe de tres casos en una familia en Cali, Colombia. Colomb Med. 2005 dec 1; 36(3): 47-50.
21. Simancas-Escorcia V, Berdal A, Diaz-Caballero A. Caracterización fenotípica del síndrome amelogénesis imperfecta–nefrocalcinosis: una revisión. Duazary 2019; 16(1): 129-143.
22. Gutiérrez S, Torres D, Briceño I, Gómez AM, Baquero E. Clinical and molecular analysis of the enamelin gene ENAM in Colombian families with autosomal dominant amelogenesis imperfecta. Genet Mol Biol. 2012 Jul; 35(3): 557-566. https://doi.org/10.1590/S1415-47572012000400003.
23. Gutiérrez SJ. Características clínicas de la caries en individuos con diferentes fenotipos de amelogénesis imperfecta. Univ Odontol. 2013 ene-jun; 32(68): 51-61
24. Duque Borrero AM, Rodríguez Manjarrez C, Soto Llanos OL, Triana Escobar FE. Prevalencia de anomalías dentales en pacientes de 4 a 14 años de edad, atendidos en las clínicas de odontopediatría de la Universidad del Valle en el período de enero de 2013 a junio de 2016. Gastrohnup. 2016 ene-abr 18; (1): 4-11.
25. Arias Acero NE, Fonseca Almánzar AM , Mora Oróstegui ML, Moreno Acuña DL, Pico Prada AR. Prevalencia de los defectos de desarrollo del esmalte en estudiantes de 7 a 9 años de dos instituciones educativas de Girón Santander 2014. Bucaramanga, Colombia: Repositorio Universidad Santo Tomas; 2015. https://repository.usta.edu.co/handle/11634/18755
26. Mafla AC, Córdoba DL, Rojas MN, Vallejos MA, Erazo MF, Rodríguez J. Prevalencia de defectos del esmalte dental en niños y adolescentes colombianos. Rev Fac Odontol Univ Antioq. 2014; 26(1): 106-125.
27. Rozo Gómez ER, .ánchez Castillo DZ, Silva Quevedo JD, Wong Arenas L. Prevalencia de hipoplasia e hipomineralización en niños de 7-13 años que asisten a la Clínica Odontopediátrica de la Universidad Cooperativa de Colombia. Bogotá, Colombia: Repositorio Universidad Cooperativa de Colombia; 2015. https://repository.ucc.edu.co/bitstream/20.500.12494/6489/1/2015-RozoySanchez-Prevalencia-Hipoplasia-Hipomineralizacion.pdf
28. Tovar S, Ziga E, Franco A, Jácome S, Ruiz III J. Estudio Nacional en Salud Bucal (ENSAB IV). Bogotá, Colombia: Ministerio de Salud; 2014.
29. Gupta SK, Saxena P, Jain S, Jain D. Prevalence and distribution of selected developmental dental anomalies in an Indian population. J Oral Sci. 2011 Jun; 53(2): 231-238. https://doi.org/10.2334/josnusd.53.231
30. Harini N, Don KR. Prevalence pattern of developmental anomalies of oral cavity in South Indian population-A hospital-based study. Drug Invention Today. 2019; 11(2).
Notes
*
Original research.
Author notes
Authors’ Note:a Correspondence: lizethnaranjo@javeriana.edu.co; Myriam.muñoz@javeriana.edu.co; angelasuarez@javeriana.edu.co; clamby@javeriana.edu.co; s.gutierrez@javeriana.edu.co.
Additional information
How to cite: Naranjo Jiménez LP, Muñoz Briceño MA, Suárez Castillo A, Lamby Tovar CP, Gutiérrez Prieto SJ. Amelogenesis Imperfecta Prevalence in a Colombian Population: A Retrospective Study. Univ Odontol. 2021; 40. https://doi.org/10.11144/Javeriana.uo40.aipc