INTRODUCTION
The term “special patient” or patient with a disability has several definitions, but the one that best identifies these patients in the field of Dentistry es, “Patients who have some biopsychosocial impairment, in which dental care requires greater complexity” (1). Epidermolysis bullosa (EB) is a rare disease of genetic origin that mainly affects the skin and mucous membranes in areas of friction and pressure that form blisters and ulcers. Recessive dystrophic (RDEB) is the type of EB that has the most severe oral involvement, including microstomia, ankyloglossia, and reduced depth of the buccal vestibule due to repeated healing cycles (2).
EB is a pathology determined by the fragility of the skin with the formation of blisters, which develop after minimal trauma. EB can be classified as acquired or of genetic origin (3). EB comprises a group of hereditary bullous disorders of rare incidence in the world population that present extreme friability of the cutaneous and mucous tissues. Individuals with the RDEB subtype have more severe symptoms due to the constant ulceration and healing process, with excessive scarring, which results in pain, microstomia, ankyloglossia, tongue depapilation, high rate of caries, and gingivitis. In addition to anatomical limitations, behavioral, social, and psychological factors generally make outpatient dental treatment unfeasible (4). This literature review supported by a clinical case aims to contribute to a better understanding of the clinical picture and diagnosis of patients with EB and its genetic variant since this pathology is rare and will provide material for clinical dental practice.
LITERATURE REVIEW
EB comprises a heterogeneous group of inherited disorders that have epithelial fragility in common. The skin, and in some cases the mucosa, develop blisters and/or erosions after minimal friction or trauma. Hereditary EB should be suspected in children who have a history of recurrent blisters and erosions, or neonates who have blisters and erosions in the absence of another plausible explanation (1).
EB is a clinically and genetically heterogeneous group of diseases characterized by skin fragility and the formation of skin blisters induced by mechanical actions. Depending on the morphological alteration, EB can be classified according to its aggressiveness, with the less aggressive forms being linked to dominant inheritance and the most severe to recessive inheritance (4). The prevalence of EB varies worldwide around 1:50,000 and can affect any sex and ethnicity, in the genetic or acquired forms. In Brazil, there is no official report on the number of patients with EB, whereas the incidence in the United States is 50:1,000,000 of live births (4).
EB is a chronic condition with varying degrees of intensity, which requires an interdisciplinary approach so that patients and their families can be provided with effective care. An understanding of the disease and its care are necessary so that they can be maintained at home. In addition, patients with EB requires interventions aimed at preventing the appearance of sequelae, which can even hinder the process of social integration (5).
In front of a suspected newborn with EB, it is immediately necessary to identify the lesion, performing a schematization of the affected areas and then a photographic documentation. The continuity of patient follow-up should be performed with evaluation of the whole body, looking for new lesions. The oral manifestations in this disease are a challenge for the dental surgeon due to the friction of the oral mucosa by manipulation (6).
Blisters are voluminous intra and subepidermal cavities, containing fluid inside. The pathophysiological mechanism of its formation is attributed to a fragility of the epidermal basal cells. When ruptured, blisters allow the space produced in the epidermis to be filled with extracellular fluid and consequent blister formation. Histologically, blisters are characterized by the complete detachment of the epidermis or one of its layers, which are formed by keratinocytes and dendritic cells (7).
Squamous cell carcinoma, which may appear early in these patients, must be treated by a wide-margin excision. This, in addition to maintaining patient's follow-up to avoid recurrences (6,8).
The oral involvement of EB affects all oral surfaces, including the tongue, buccal mucosa, palate, floor of the mouth, and gingiva. However, with the progression of the disease, some complications can arise as a result of the severity and increase of blisters. There is often a difficulty in moving the tongue, as a consequence of scarification. Moreover, the mucosa may become attached to the gingiva in edentulous areas or to the neck of the tooth in dentate areas. Such adhesion is the result of scar contractions or blister formations in the region (7).
In teeth, changes have been described as deformities, congenital defects, and abnormal enamel formation. Impacted and supernumerary teeth are also very common. Extensive caries, scarification of periodontal tissues, and abscesses have been reported (8). There are several limitations that the dental surgeon has when dealing with a patient with EB. The very fact that there is no specific treatment for the disease is quite concerning. Palliative therapy is the only management that may promote a temporary improvement (9).
DESCRIPTION OF A CLINICAL CASE
We inform that the patient's caregiver gave free and informed consent to the propaedeutics applied. Patient T.S, 10 years old, female, white, who was referred to the oral and maxillofacial surgeon for removal of teeth 36 (first left lower permanent molar, under 2-digit nomenclature) due to marked dental destruction and odontogenic infection. The patient had a diagnosis of RDEB, which was confirmed through histopathological analysis, and underwent clinical follow-up with a dermatologist (Figures 1,2,3).
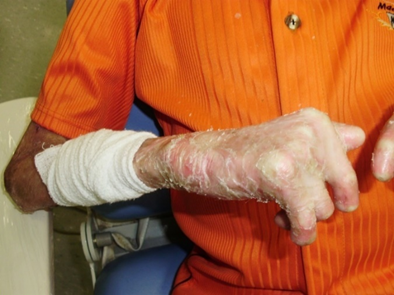 FIGURE 1
Bullous lesions in the upper limb with arachnoid-shaped hands and motor difficulties
FIGURE 1
Bullous lesions in the upper limb with arachnoid-shaped hands and motor difficulties
Source: the author.
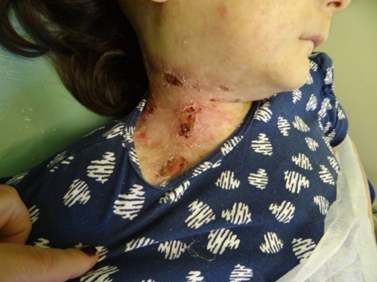 FIGURE 2
Bullous lesions with areas of necrosis in the neck
FIGURE 2
Bullous lesions with areas of necrosis in the neck
Source: the author.
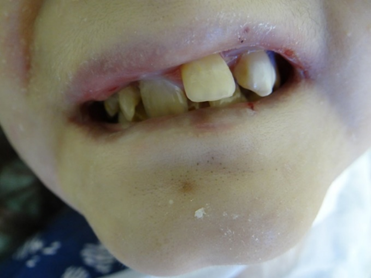 FIGURE 3
Oral appearance with desquamation and bullous lesions, muscle contracture, limited mouth opening
FIGURE 3
Oral appearance with desquamation and bullous lesions, muscle contracture, limited mouth opening
Source: the author.
Regarding family history, one sister had already died as a result of complications associated with EB. In the system review, ulcerations and blister flaps were observed in the upper and lower limbs, synechiae of the fingers and toes, in addition to the presence of pyogenic granuloma on the scalp. The patient reported the constant emergence of intraoral blisters and ulcers, mainly in the region of the buccal mucosa and tongue. According to the pain scale (0 to 10), the patient scored the pain of intraoral origin as 8. Oral lesions were observed in the gingiva and buccal mucosa and nasal obstruction. Regarding the teeth element, the prognosis was dismal, and the extraction of tooth 36 was indicated.
After planning, treatment under general anesthesia was chosen. Treatment in patients with EB is challenging, especially in cases in which there will be significant trauma. The treatment modality under general anesthesia (dental treatment under general anesthesia or sedation is indicated in cases with disorders of medical, mental or psychological origin, including intellectual disability, physical limitations, behavioral changes, and chronic diseases) (10,11,12), corroborating the choice to perform in the operating room environment, has the monitoring of the multidisciplinary team that administers drugs and anesthetics, control anxiety, and monitor the patient’s vital signs. Furthermore, the hospital has the adequate structure to deal with complications and provides a safe environment for the dentist to perform all dental treatment in a single session.
Anesthetic induction was performed through intravenous access, the multidisciplinary team opted for orotracheal intubation with a pediatric cannula, and special non-adherent dressings were used to protect the face, neck, and eyes. During the surgery, carefully handled topical petroleum ointment was applied on the lip region for protection of the tissues. Tooth 36 weas extracted followed by the patient referral to the intensive care unit, where the postoperative protocols were performed and occurred without abnormalities. The patient was discharged 48 hours later. The instructions to family members were reassessed five days after the procedure and the clinical evolution was satisfactory.
DISCUSSION
Ankyloglossia and reduced buccal vestibule depth are considered important indicators of severe impairment of the oral cavity soft tissues. Furthermore, some authors (5,8) have indicated that palatal wrinkles and lingual papillae tend to disfigure with advancing age (1,4). In the clinical case portrayed, the patient had stomatological manifestations associated with EB, which made it difficult to perform dental procedures and caused painful symptoms during brushing. Consequently, it was necessary for the dentist to guide the child and the parents regarding the performance of intraoral hygiene methods in an adapted and adequate way; increasing the frequency of brushing; implementing mouthwash with an alcohol-free antiseptic solution containing fluoride; reinforcing the use of fluoride toothpaste; and use of dental floss (10).
The authors report the incidence of squamous cell carcinomas in these patients, as well as the limitation of mouth opening, promoting cleft lip and fissured tongue in the attempt (6,8,14).
The treatment and, consequently, the clinical planning of patients with EB generate an important challenge; the clarification during the anamnesis and the contact with the doctor responsible for the clinical care are fundamental for the dental workup (2,5). Sedation in children protects safety and well-being; minimizes physical discomfort and pain during procedures; controls anxiety; reduces psychological trauma; maximizes the potential for amnesia; and modifies behavior and/or movement to allow completion of treatment (10,12).
CONCLUSION
Hereditary EB is a very rare dermatological disorder; however, it has a great impact on the life of the patient and their families. The most severe forms of the disease cause great physical and emotional suffering to the child. These forms are most often related to the extracutaneous involvement of the disease, which may affect the eyes, nose, oral mucosa, teeth, gastrointestinal and genitourinary tracts, musculoskeletal system, in addition to metabolic disorders such as malnutrition and anemia.
EB is difficult to diagnose since it has a high morbidity and mortality together with a great functional impairment to the patient. Thus, its discovery and treatment are extremely important in clinical practice, aiming at an improvement in the quality of life of those affected, providing an improvement in techniques and protocols in dental care.
The oral cavity was difficult to manipulate, either in the examination or the clinical procedures, due to the bullous lesions in the region, often preventing conventional treatment. These special patients should be treated by professionals familiar with the pathology and who have a systemic knowledge of rare diseases.