Introduction
Currently, the demand for cosmetic procedures has grown exponentially. Dental procedures, as well as medical ones, besides working to obtain the principle of health promotion, seek smile esthetics, as the smile is a form of communication and socialization that expresses many feelings (1,2,3).
Facial esthetic harmony correlates directly with the smile and this, in turn, is formed by the union of three components: teeth, gum and lips (1,2,3,4). The smile becomes esthetically pleasing when these elements are disposed in suitable proportion, and exposure of the gingival tissue is limited to 3 mm. When the gingival exposure is greater than 3 mm, it is characterized the non-esthetic condition called gummy smile, which affects some patients psychologically (1,2,5,6,7,8).
Several therapeutic modalities have been proposed for the correction of gummy smile, among them: gingivectomy or gingivoplasty (2,3,5,6,7), myectomy (6,8) and orthognathic surgery (6,8,9); and the last two procedures are more invasive and associated with high morbidity (6). In contrast, the use of botulinum toxin can be considered as a therapeutic option to surgery, because it is a more conservative method, more effective, faster and safer, as compared to surgical procedures (1,5,10).
Botulinum toxin is synthesized by Gram-positive anaerobic bacterium Clostridium botulinum (6,8,9), and inhibits the release of acetylcholine at the neuromuscular junction, preventing muscle contraction. There are seven distinct serotypes of toxins (A, B, C1, D, E, F, and G). However, the subtype A is the most frequently used clinically and the most powerful (6).
Currently, botulinum toxin has been shown effective in the treatment of gummy smile in patients with hyperfunction of the muscles involved in smiling, as well as in patients with other disorders such as temporomandibular disorders (hypertrophy of the masseter muscle, bruxism, clench) and myofascial pain (1,6,9). The purpose of this study was to report a case of a patient who presented gingival overgrowth and gummy smile and was treated by application of botulinum toxin type A complementing the gingivoplasty.
Description of the case
A Caucasian female, 28 years old, attended the particular clinic complaining gummy smile. Clinically, the patient presented severe anatomic discrepancy between the length of the maxillary teeth (Figure 1), and prominent gingival display, with more than 4mm, featuring gummy smile.
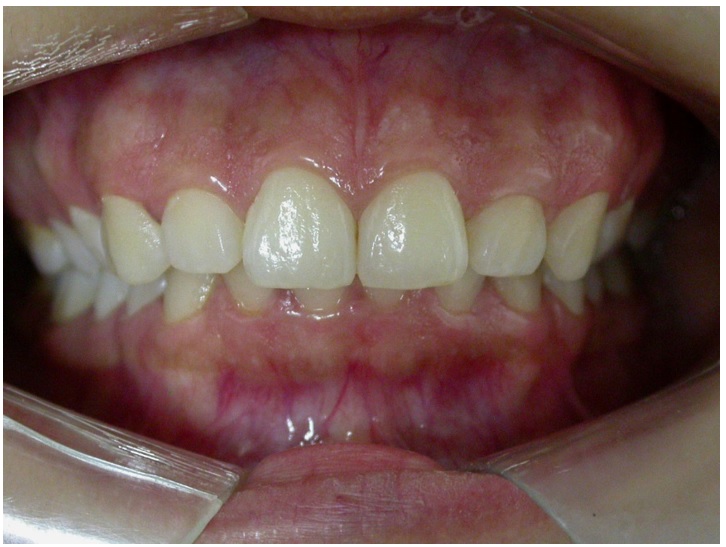 Figure 1
Initial clinic aspects presenting mild
anatomical discrepancy between the length of teeth 11, 12, 12, 21, 22 and 23
Figure 1
Initial clinic aspects presenting mild
anatomical discrepancy between the length of teeth 11, 12, 12, 21, 22 and 23
Source: own
elaboration.
The gingivoplasty was proposed. Before the surgical procedure, the patient was oriented about oral hygiene, in order to reduce gingival inflammation and prevent the possibility of recurrence of gingival overgrowth.
Under local infiltrative anesthesia, gingivoplasty was performed by determination of the bleeding points with the aid of a millimeter probe and the union of these points was made with the electric scalpel (2). The length of the teeth was increased, characterizing the new dental zenith. Posteriorly, the scraping was performed, resembling the technique of external bevel, with the purpose of enhancing tissue repair (Figure 2). There was no need for the use of surgical cement, given that the process of the wound occurs by secondary intention. The patient was counseled, and analgesics were administered postoperatively.
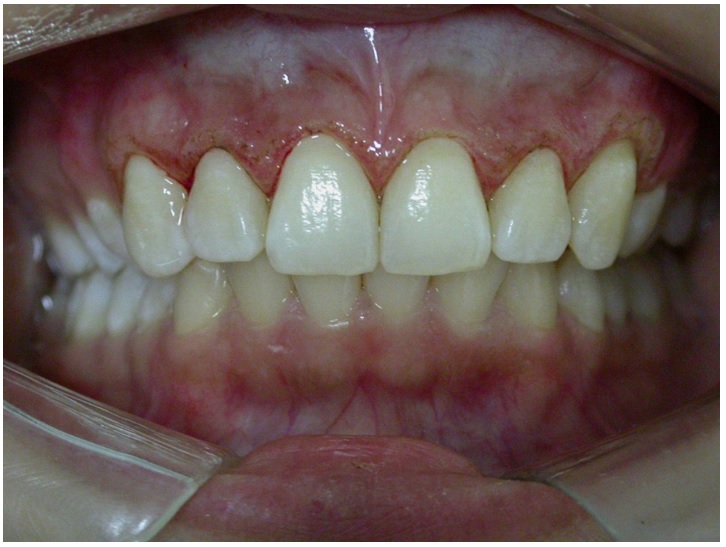 Figure 2
Immediate postoperative
Figure 2
Immediate postoperative
Source: own
elaboration.
After 30 days, satisfactory tissue repair was observed (Figure 3) and the patient reported no changes or complaints. However, the patient yet reported the complaint of gummy smile (Figure 4). The application of botulinum toxin was suggested, and the patient was counseled about the recurrence of the gummy smile after 6 months of application.
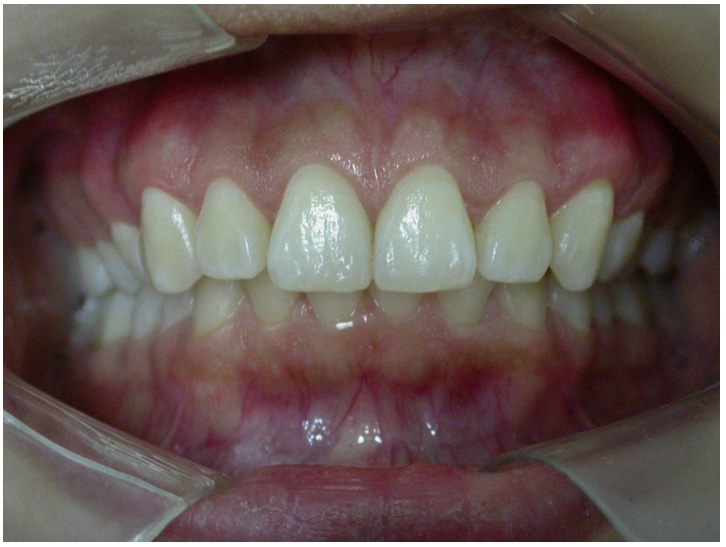 Figure 3
Post-surgical (30 days): satisfactory
tissue reparation observed
Figure 3
Post-surgical (30 days): satisfactory
tissue reparation observed
Source: own
elaboration.
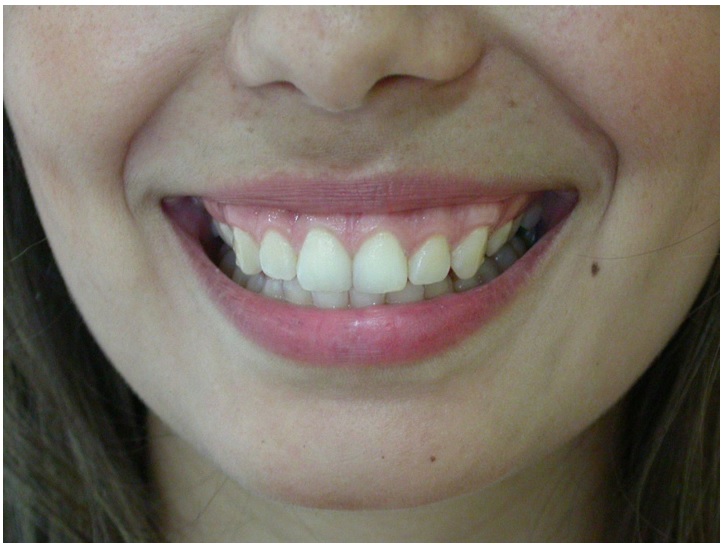 Figure 4
Persistence of gummy smile after gingivoplasty (30 days)
Figure 4
Persistence of gummy smile after gingivoplasty (30 days)
Source: own
elaboration.
Prior to application of botulinum toxin, the surface of the skin was disinfected with ethanol, to avoid local infection and remove the oils from the skin. Posteriorly, local anesthetic (Emla®, Astra, Sao Paulo, Brazil) was applied, with the purpose to promote comfort during the procedure. The botulinum toxin type A (Dysport®, Ipsen Biopharm Ltd, Wrexham, UK) was diluted in 1.7 ml of saline, according to the manufacturer’s instructions, and injected 2 units at the recommended site, laterally to each nostril. After application, the patient was advised do not lower her head and not engage in physical activity during the first 4 hours after the procedure.
After 10 days, the patient was evaluated presenting uniform dehiscence of the upper lip (Figure 5). Were no reported side effects or complaints. The patient was advised about the need for applications, on average, 6 months after the first, according to their needs.
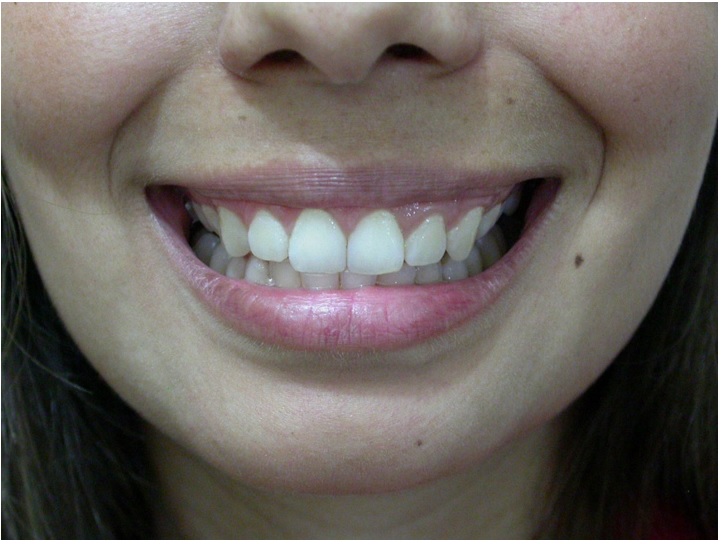 Figure 5
Aesthetic result after 10 days of botulinum toxin application
Figure 5
Aesthetic result after 10 days of botulinum toxin application
Source: own
elaboration.
Discussion
Botulinum toxin has become an excellent auxiliary mean in the treatment of several dental disorders. Despite being known for cosmetic use in the reduction of hyperkinetic facial lines, it can also be used for therapeutic purposes in cases of bruxism, temporomandibular joint dysfunction, masseter hypertrophy and severe gingival exposure (1,4,5,6,7,8,9,10,11).
The gummy smile is conceptualized by the exposure of more than 3 mm of gingival tissue during smiling (1,5,7), and it is often found in women (10). The predominance of females can be explained by the fact that male patients present lower smile line (4,5).
Several etiologies have been suggested to gummy smile, as vertical maxillary excess (1,4,5,6,8,9), delayed passive eruption (1,4,6,7,9), hyperfunction of the muscles involved in smiling (1,6,7,9) and reduced length of the clinical crown of the teeth (1,2,3,7), which can occur separately or together, and determine the type of treatment to be used.
In gummy smile caused by overactive muscle, botulinum toxin was indicated. It is the treatment of first choice for the ease and security of applications, quick effect, besides being a more conservative approach when compared to surgical procedures (myectomy or Le Fort I osteotomy) (1,4,5,6,7,8,9,10,11).
The activity of the smile is determined by several facial muscles, like the elevator of the upper lip and wing of the nose, the zygomatic major and minor, the angle of the mouth, orbicularis oris and risorius (4,5,6,8,9,10). Among them, the first three ones play higher function and determine the amount of lip elevation and, therefore, should be the muscles affected by the injection of the toxin. The fibers of these muscles converge to the same area, and they form a triangle, what suggests that the point of adequate election comprehend the three muscles in a single injection. The toxin, when injected, can spread in an area of 10 to 30 mm, what allows the effective extent (4,5). The proposed site of injection was laterally to the wing of the nose (4,8,9,10). After being injected into predetermined locations, the toxin decreases the contraction of the muscles responsible for the elevation of the upper lip, and this reduces gum exposure (4,5,6,7,8,9,10,11).
Each muscle involved in the elevation of the upper lip has a function during the activity of smile. The points of the injections are determined by the contraction of specific muscle groups, that results in different areas of gingival display. Several classifications have been proposed to gummy smile: anterior, posterior, mixed and asymmetric, involving different muscle groups (4,10). The anterior gummy smile should be treated with the conventional technique, with the applications laterally to the wing of the nose. In patients with posterior gummy smile, the application of the toxin must involve the zygomatic major and minor muscles, with the injection of the toxin in two different points: the point of greatest contraction of nasolabial during the activity of smile, and the second point 2 cm laterally to the first, at the level of the tragus line. In the case of patients who have mixed gummy smile, the application of the toxin should be performed on all the points mentioned above. However, the dose should be reduced to 50 % in the lateral to the wing of the nose point (5). In cases of labial asymmetry, that occurs due to differences in muscle activity (4), the patients receive injections of different doses on either side of the face (5,10).
Botulinum toxin type A is a hydrophilic powder, stored under vacuum, sterile and stable (1,6,8). The reconstitution occurs from the smooth injection of the diluent (sodium chloride 0.9 %) inside the bottle. The solution should be stored at 2 to 8 °C and used within 4 to 8 hours, in order to ensure its effectiveness (1,9).
At the beginning of the treatment, extraoral photographs, including the close-up of the smile, were performed. Some authors mentioned the importance of taking the picture of the smile before and after the application of the toxin (1,6,10,11). It has been suggested that the picture of the smile should be performed stimulating individually the muscles with electrical current, in order to ensure that muscle contraction be controlled, precise and repeatable, as the spontaneous smile is extremely difficult to be replicated. Patients understand that the treatment is carried out to produce a different smile, and, from this perspective, unconsciously, there is a tendency to smile differently in photographs after the treatment (11).
The clinical effects show up in 2-10 days after the injection, and the most visible effect occurs 14 days after the injection (1,4,6). This first effect, scheduled to be progressive, is also reversible, lasting about 3 to 6 months (1,5,6,9). Patients should be advised of the need for applications, according to their tastes and needs, as was quoted in this report.
The injection of botulinum toxin, despite being a simple and safe procedure, may be associated with some adverse events such as: Pain at the injection site, bruising, infection, edema, dysphonia, dysphagia, ptosis or lengthening of the upper lip and asymmetry of the smile. The dentist should be attentive in relation to dosage, precision of technique and location of the puncture (1,5,6,9,11). In this report, claims or changes arising from the application were not reported.
Contraindications to the use of botulinum toxin are: pregnancy; lactation; hypersensitivity (allergy) to botulinum toxin itself; lactose and albumin; muscle and neurodegenerative diseases (myasthenia gravis and Charcot’s disease); and concurrent use of aminoglycoside antibiotic that enhances the action of the toxin (1,9).
In this report, the result was satisfactory to the harmony of the smile of the patient by association of treatments - gingivoplasty and application of botulinum toxin type A. The institution of isolated treatments could not culminate in the excellence of the earned results. Initially, the creation of the new dental zenith during the course of resective gingival surgery promoted the new dental architecture, favoring harmony gingival-dental-facial for the patient. Subsequently, the application of botulinum toxin type A softened the gummy smile, by the uniform dehiscence itself of the upper lip, still promoting smoothness to facial lines of the smile, as can be seen in the nasolabial folds, adjacent to the nostrils, comparing figures 4 and 5.
Conclusions
The application of botulinum toxin is an alternative
less invasive, faster, safer, more effective and it produces harmonics and pleasing
results when applied in target muscles, respecting the appropriate dose and type
of smile, and, therefore, it is a useful adjunct in the esthetic improvement of
the smile and provides better results when combined with resective
gingival surgery.
Recommendations
Based in this case report, future researches become important for the clinical evidence of this therapeutic association.