Experiencing meaning in life (MiL) is a primary motivation for human beings and a central topic in theories about the good life and well-being (Aftab et al., 2019). Viktor Emil Frankl, the founder of logotherapy, argued that MiL is related to the experience of freedom and responsibility, a positive conception of one’s life, significant purposes and goals, and self-realization (Frankl, 2014). Suppose a person experiences a lack of MiL. In that case, he/she develops a negative cognitive, emotional, and motivational state associated with hopelessness, perception of a lack of control over his or her life, a lack of goals and purposes, as well as a negative and pessimistic attitude toward life in general.
Empirical research supports these ideas. A high level of MiL has significant relationships with psychological well-being and health, happiness, satisfaction with life, and positive cognitive-emotional functioning (e.g., García-Alandete, 2015). By contrast, a low level of MiL is related to a negative and pessimistic attitude about life in general, hopelessness, depression, substance dependence, self-injury behaviors, and suicide, among others, and it hinders the activation of resources to face adversity (e.g., Marco et al., 2015).
Differences in MiL in clinical samples according to diagnosis
Several studies have analyzed the differences in MiL between people diagnosed with mental disorders and the differences in MiL according to diagnosis. Schulenberg et al. (2011) found that patients with different mental disorders (schizophrenia-spectrum, schizoaffective disorder, major depressive disorder, and bipolar disorder) reported lower levels of MiL than people without a diagnosis of mental disorder, and a non-significant interaction between the diagnosis and MiL one-year after diagnosis in people with schizophrenia-spectrum disorders, major depressive disorder, and bipolar disorder. Volkert et al. (2014) observed that people with depressive disorder showed a lower level of MiL than healthy controls and those with anxiety disorders, adjustment disorders, somatoform disorder, personality disorders, among others. Marco, Pérez, et al. (2017) found that patients with borderline personality disorder showed a lower MiL than people with mental disorders without borderline personality disorder, due to their greater sense of emptiness, identity disturbance, and confusion. The results of these studies indicate that people diagnosed with mental disorders score lower in MiL than those that do not suffer a mental disorder.
Interesting results were found by Roberts (1991) and Fervaha et al. (2016) with patients diagnosed with schizophrenia. Roberts (1991) examined MiL in a sample of actively psychotic patients with schizophrenia, nurses working at a psychiatric hospital, Anglican priests, and psychiatric patients in remission from active psychosis. This author found that the former scored higher in MiL than all the other subsamples and suggested an interesting hypothesis: the formation of delusions in patients with schizophrenia might provide them with a strong, although non-reality-based, sense of MiL. By their part, Fervaha et al. (2016) found that young people with schizophrenia endorsed significantly lower levels of subjective well-being and happiness than healthy controls, although there was substantial overlap in scores, and many participants with schizophrenia endorsed a high level of well-being; likewise, these authors found a marked overlap in individual scores in happiness between those with and without schizophrenia, demonstrating that many young people with schizophrenia do, in fact, endorse high levels of subjective well-being.
Role of MiL in people diagnosed with mental disorders
Several studies suggest that MiL might play a positive role in therapeutic interventions in people diagnosed with mental disorders or who suffer emotional dysregulation. For example, MiL buffers the association between risk factors for suicide and hopelessness among patients with mental disorders (Marco et al., 2016), and on the relationship between emotional dysregulation and hopelessness among adolescents (García-Alandete et al., 2019). Moreover, the pursuit and attainment of significant life goals (e.g., in goal-oriented treatment programs) are successful managing of mental disorders and positively influencing the therapeutic process (Sivaraman, 2003). Therefore, it is important to include MiL in assessment and interventions for people diagnosed with mental disorders.
The studies above suggest that: (1) only a few studies have analyzed the differences in MiL according to the diagnosis in people with mental disorders; (2) MiL is expressed at a different level in different mental disorders; (3) the symptomatology might provide people with schizophrenia-spectrum and eating disorders a source of MiL, although non-reality based and dysfunctional, by which they score higher in MiL than those diagnosed with depressive disorders. Taking this into account, better understanding the differences in MiL based on the diagnosis might improve the assessment, treatment, prognosis, and prevention of symptomatology and frequent negative behaviors among people with mental disorders (such as self-injuries, suicide, and hopelessness) (e.g., Marco et al., 2014; Marco, Guillen et al., 2017).
The present study
The present study aimed to analyze the differences between people diagnosed with schizophrenia-spectrum, eating, anxiety, and major depressive disorders according to the diagnosis. We hypothesized that (1) both the schizophrenia-spectrum disorder and eating disorder subsamples will show higher scores in MiL than both the anxiety and major depression disorders subsamples and that (2) the major depressive disorder subsample will show the lowest score in MiL.
The present study’s findings highlight the importance of considering MiL in people with mental disorders, and they can stimulate further research on this issue for better understanding the way MiL is experienced and how it can be improved in patients with mental disorders.
Method
Participants
Participants were 157 Spanish out-patients (28 men, 17.83%, and 129 women, 82.17%) age-ranged from 13 to 68 years old (M = 32.58, SD = 13.34), diagnosed with different mental disorders and with an illness evolution ranged from 1 to 35 years, recruited from 6 public mental health services. Clinical participants satisfied the DSM-5 (American Psychiatric Association [APA], 2013) diagnostic criteria for schizophrenia-spectrum, eating, anxiety, and major depressive disorder subsamples. The exclusion criterion was moderate to severe intellectual disability. Table 1 shows the size of the subsample, age range, mean and standard deviation, and the distribution of the subsamples in the variable gender.
Table 1
Age range, mean, standard deviation, and gender of the clinical groups
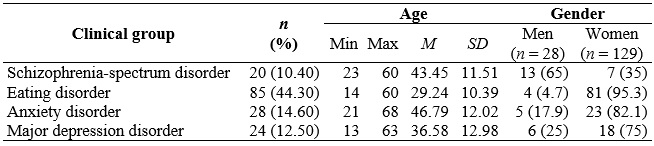
Note. N = 157.
Instruments
Structured Clinical Interview for DSM-5 Axis I Disorders (SCID-I; First et al., 1997). This is an interview used to make the major DSM-5 (APA, 2013) Axis I diagnoses, and it offers good psychometric properties, Kappa 0.66, demonstrating reliability (Altman, 1991). Clinicians confirmed the participants’ diagnoses by using the SCID-I.
Purpose in Life-10 Items (PIL-10; García-Alandete et al., 2013). This instrument is a 10-item Likert-type scale with seven response categories (both categories 1 and 7 have specific anchoring phrases, and category 4 indicates neutrality) that assess different aspects of MiL: (1) enthusiasm/boredom, (2) excitement in living, (3) presence of clear life goals, (4) newness of each day, (5) wishing for more lives, (6) activity after retirement, (7) good things in life, (8) having a reason to be alive, (9) capacity to find meaning, and (10) presence of goals/life purpose. The higher the score in the PIL-10, the higher the MiL. In the present study, the PIL-10 showed an excellent internal consistency, McDonald’s v = 0.91.
Procedure
The sampling was carried out in three individual sessions. In the first session, the patients’ informed consent and their families (if the case required it) were obtained, and the patients filled out the assessment scales. During the subsequent two sessions, the therapists, who were informed about the nature and purpose of the current research, supervised the scales’ completion and established the diagnosis. Participation was voluntary, and participants did not receive any compensation for their collaboration. Authors received ethics approval from their institutions to gather data for their project.
Statistical analyses
The SPSS 25.0 software for Windows (IBM, 2017) was used to analyze the descriptive statistics and internal consistency of the PIL-10, as well as for carrying out an analysis of covariance (ANCOVA), using the diagnosis as factor and gender, age, and length of diagnosis as covariables to test the differences in MiL according to the diagnosis, followed by the Bonferroni post hoc test.
Results
The schizophrenia-spectrum disorder subsample showed the highest score in MiL, M = 48.35, SD = 15.28, followed by the eating disorder subsample, M = 46.08, SD = 9.63, the anxiety disorder subsample, M = 36.64, SD = 12.19, and the major depressive disorder subsample, M = 31.17, SD = 13.66. There was a significant effect of diagnosis in MiL, F(4, 192) = 27.08, p = 0.000, h2 = 0.371, after controlling for the effects of gender, F(1, 192) = 2.34, p = 0.128, age, F(1, 192) = 0.58, p = 0.447, and length of evolution, F(1, 192) = 0.29, p = 0.589.
The Bonferroni test showed significant differences (1) between the schizophrenia-spectrum disorder subsample and both the major depressive and anxiety disorders subsamples, and (2) between the eating disorder subsample and both the major depressive and anxiety disorders subsamples (Table 2).
Table 2
Multiple comparisons for differences in MiL according to diagnosis
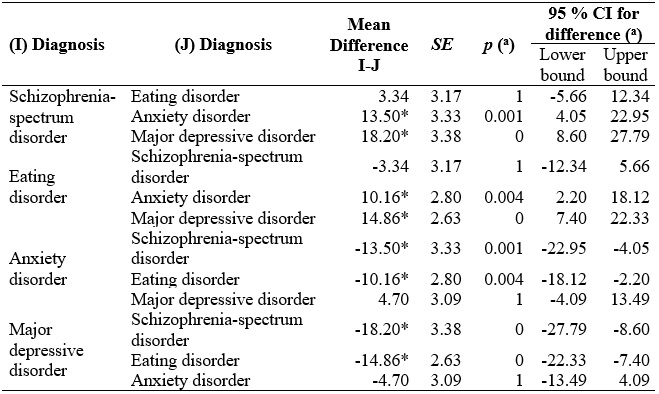
Note. Based on the estimated marginal means.
aAdjustment for multiple comparisons: Bonferroni.
*p < 0.05
Discussion
The purpose of the present study was to analyze the differences in MiL between people without a diagnosis of mental disorder and patients diagnosed with schizophrenia-spectrum, eating, anxiety, and major depressive disorders. We hypothesized that: (1) both the schizophrenia-spectrum and eating disorders subsamples would show higher scores in MiL than both the anxiety and major depressive disorders subsamples; (2) the major depressive disorder subsample would show the lowest scores in MiL.
Hypothesis 1: Both the schizophrenia-spectrum and eating disorders subsamples would show higher scores in MiL than both the anxiety and major depressive disorders subsamples
Both the schizophrenic-spectrum disorder and eating disorder subsamples scored significantly higher in MiL than the other subsamples. The means difference between the schizophrenic-spectrum disorder and the eating disorder subsamples was not significant. The means differences between both the schizophrenic-spectrum disorder subsample and eating disorder subsample and both the anxiety disorder and major depressive disorder subsamples were significant. In contrast, the means difference between the anxiety and major depressive disorder subsamples was not significant.
Regarding the differences between the schizophrenic-spectrum disorder subsample and both the anxiety disorder and major depressive disorder subsamples, previous studies found higher scores in MiL in schizophrenic patients than those with anxiety and depressive disorders, as well as higher scores on quality of life (Saarni et al., 2006) and positive life satisfaction, even though their educational, psychosocial, functioning conditions, social life, and work were more deteriorated than patients with depression, lack of social support, and low economic status (Koivumaa-Honkanen et al., 1996). It is worth noting that both quality of life and life satisfaction are positively related to MiL (Martela & Steger, 2016). The relationship between schizophrenia-spectrum disorder and MiL might be mediated by other variables, such as social support (care of family and friendships) (e.g., Lan & Su, 2007), affective (positive emotional experiences) (e.g., Koivumaa-Honkanen et al., 1999), or even spiritual (e.g., Rosmarin & Koenig, 2020), among others, that might offer resources for coping with the mental disorder. On the other hand, as noted above, the formation of delusions might provide a strong, although non-reality-based, sense of MiL in patients with schizophrenia, especially in psychotic phases (Roberts, 1991). Likewise, it must be noted that the schizophrenia-spectrum disorder subsample in the present study was composed of long-term patients in an outpatient social-rehabilitation unit, where they participated in subsample-therapy, social skills, and daily-skills subsamples, which were a strong resource to help them in their lives. This very close level of support may make them feel that their lives, despite their diagnosis, are worth living. In this regard, Stolovy et al. (2009) concluded that the caring that inpatients with schizophrenia received within the hospital provided them with a kind of community where they felt they belonged and found MiL.
Regarding the eating disorder subsample, D’Abundo and Chally (2004) found in a qualitative study that women with eating disorders experienced a false sense of control by not eating, and Fox and Leung (2009) suggested that eating disorder symptoms function as a source of MiL in anorexic patients, providing the patient with a sense of control and a sense of uniqueness with which to address negative states. Sense of control and uniqueness, although dysfunctional, might prevent people with eating disorders from being aware of their disorder, thus allowing them to feel optimistic about their daily lives, which might explain the higher score in MiL in the eating disorder subsample than in both the major depressive and anxiety disorder subsamples.
Hypothesis 2: The major depressive disorder subsample would show the lowest score in MiL
The major depressive disorder subsample scored lower in MiL than all the other subsamples, although the difference with the anxiety disorder subsample was not significant. The sense of lack of control and self-determination, lack of vital interests and goals, hopelessness, a negative and pessimistic attitude toward life, and emotional suffering, which are stronger among people with major depressive disorder than among people with other mental disorders, might explain the lower scores of the former in MiL (e.g., Sacco & Beck, 1995).
As noted above, the differences were significant with both the schizophrenic-spectrum disorder and eating disorder subsamples. It is widely accepted that mood disorders, such as depression, are common psychiatric comorbidities in people with anxiety disorder. Likewise, most cases of mood disorders-not otherwise specified represent hybrids between mood and anxiety disorders, such as mixed anxiety-depressive disorder (e.g., Williams et al., 2007). The common comorbidity between depression and anxiety (e.g., Kelftaras & Katsogianni, 2012) might explain the non-significant differences between the major depressive disorder subsample and the anxiety disorder subsample in the present study. This result suggests some reflections considering previous studies whose results contradicted those obtained in the present study. For example, Volkert et al. (2014) found that patients with depression scored lower in MiL than patients with anxiety disorders, among others, stating that this result seems meaningful, considering that loss of interest and hopelessness are part of the diagnostic criteria for depression. In another vein, Seow et al. (2016) found non-significant differences between patients with depression and patients with anxiety disorders in general coping, spirituality, interpersonal skills, personal growth, and autonomy (which are domains of positive mental health related to MiL), but significant differences in emotional support, as patients with anxiety disorders scored higher than those with depression. These results and those obtained in the present study suggest that differences in levels of hopelessness might explain why people with anxiety disorders score higher in MiL than people with major depressive disorder: hopelessness might mediate the relationship between MiL and both anxiety and major depressive disorder.
On the other hand, in the present study, other variables such as social support, spirituality, and treatment, among other variables that could influence participants’ MiL, were not included. These issues should be taken into account in future research in people diagnosed with mental disorders.
Clinical implications
MiL is not only significantly related to positive mental health, but it can even be a strong resource for coping with mental disorders. Several studies suggest that having significant life goals might influence the motivation to be actively involved in the therapeutic process (Sivaraman, 2003) and be crucial in understanding the etiology and recovery from mental disorders (e.g., Fulford et al., 2020). MiL might buffer the relationship between risk factors for suicide and hopelessness in mental disorders (Marco et al., 2016); the dysfunctional sense of control in people with mental disorders might be redirected within a “circle of acceptance” toward an authentic sense of MiL that leads to recovery (D’Abundo & Chally, 2004). Therefore, MiL should be included in both assessment and psychotherapeutic intervention for people with mental disorders by considering how MiL is expressed in each. Empowering patients to discover a personal source of MiL and involve them in setting their own life purposes and goals should be an important goal in mental disorder treatment and recovery. On the other hand, MiL might increase during interventions with people with mental disorders (e.g., Kelftaras & Katsogianni, 2012). Therefore, there could be an effect of reciprocal feedback between MiL and psychotherapy in people with mental disorders.
In this regard, Meaning-Centered Therapy in combination with Cognitive-Behavioral Therapy (Ameli, 2016), Dialectic-Behavioral Therapy (Lungu & Linehan, 2017), and Acceptance and Commitment Therapy (Moghbel & Haghayegh, 2019), among others, might be a helpful resource. This type of therapy can introduce issues related to life satisfaction and setting significant life goals to improve the intervention, thus contributing to managing symptoms and behaviors caused by the mental disorder, facing life challenges (e.g., stressful life events), and having a fulfilling life, even when one has a mental disorder (Volkert et al., 2014).
Limitations and suggestions for future research
An important limitation of the present study was the small subsamples size and their unbalanced composition in age and gender. Although it is common to use small and unbalanced sample sizes in studies with clinical samples (e.g., Schulenberg et al., 2011; Volkert et al., 2014), future research should use subsamples with sufficiently large and more balanced sample sizes to carry out comparative analyses in better conditions. In the same way, future research should include patients with different mental disorders from those used in the present study to better understand how MiL is expressed.
Because MiL might mediate the relationship between mental disorders and clinically relevant behaviors, such as substance abuse, self-injurious behaviors, and suicide (e.g., Marco et al., 2019), and it might predict treatment outcome (e.g., Glaw et al., 2017), it would be relevant to assess its role in the relationships among mental disorders, relevant behaviors, and therapeutic intervention (e.g. Marco et al., 2020).
In addition, it would be interesting to analyze the role played by psychosocial (such as gender, religiosity/spirituality, social support, marital status, and quality of life, among others) and clinical (such as symptomatologic phenomenology of the different mental disorders, the severity of symptoms, use of psychiatric medication, and attending social-rehabilitation units, among others) variables in the relationship between mental disorders and MiL. Likewise, future studies should explore whether people with mental disorders attending different types of medical or psychosocial resources differ in their levels of MiL.
References
Aftab, A., Lee, E. E., Klaus, F., Daly, R., Wu, T. C., Tu, X., Huege, S., & Jeste, D. V. (2019). Meaning in life and its relationship with physical, mental, and cognitive functioning: A study of 1,042 community-dwelling adults across the lifespan. Journal of Clinical Psychiatry, 81(1), 19m13064. https://doi.org/10.4088/JCP.19m13064
Altman, D. G. (1991). Practical statistics for medical research. Chapman and Hall.
Ameli, M. (2016). Integrating logotherapy with cognitive behavior therapy: A worthy challenge. In A. Batthyány (Eds.), Logotherapy and existential analysis: Proceedings of the Viktor Frankl Institute Vienna (Vol. 1, pp. 197-217). Springer. https://doi.org/10.1007/978-3-319-29424-7_18
American Psychiatric Association (APA). (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.). Author.
D’Abundo, M., & Chally, P. (2004). Struggling with recovery: Participant perspectives on battling an eating disorder. Qualitative Health Research, 14(8), 1094-1106. https://doi.org/10.1177/1049732304267753
Fervaha, G., Agid, O., Takeuchi, H., Foussias, G., & Remington, G. (2016). Life satisfaction and happiness among young adults with schizophrenia. Psychiatry Research, 242, 174-179. https://doi.org/10.1016/j.psychres.2016.05.046
First, M. B., Spitzer, R. L., Gibbon, M., & Williams, J. B. W. (1997). User’s guide for the structured clinical interview for DSM-IV Axis I Disorders: Clinician version (1st ed.). American Psychiatric Press.
Fox, A. P., & Leung, N. (2009). Existential well-being in younger and older people with anorexia nervosa: A preliminary investigation. European Eating Disorders Review, 17(1), 24-30. https://doi.org/10.1002/erv.895
Frankl, V. E. (2014). Theory and therapy of the mental disorders. Routledge.
Fulford, D., Meyer-Kalos, P. S., & Mueser, K. T. (2020). Focusing on recovery goals improves motivation in first-episode psychosis. Social Psychiatry and Psychiatric Epidemiology, 55(1), 1629-1637. https://doi.org/10.1007/s00127-020-01877-x
García-Alandete, J. (2015). Does meaning in life predict psychological well-being? An analysis using the Spanish versions of the Purpose-In-Life Test and the Ryff’s Scales. Euroean Journal of Counselling Psychology, 3(2), 89-98. https://doi.org/10.5964/ejcop.v3i2.27
García-Alandete, J., Gallego, B., Pérez, S., & Marco, J. H. (2019). Meaning in life among adolescents: Factorial invariance of the Purpose in Life Test and buffering effect on the relation between emotional dysregulation and hopelessness. Clinical Psychology and Psychotherapy, 26(1), 24-34. https://doi.org/10.1002/cpp.2327
García-Alandete, J., Rosa, E., & Sellés, P. (2013). Factorial structure and internal consistency of a Spanish version of the Purpose-In-Life Test. Universitas Psychologica, 12(2), 517-530. https://doi.org/10.11144/Javeriana.UPSY12-2.efci
Glaw, X., Kable, A., Hazelton, M., & Inder, K. (2017). Meaning in life and meaning of life in mental health care: An integrative literature review. Issues in Mental Health Nursing, 38(3), 243-252. https://doi.org/10.1080/01612840.2016.1253804
IBM. (2017). IBM SPSS Statistics for Windows, Version 25.0. IBM Corp.
Kelftaras, G., & Katsogianni, I. (2012). Spirituality, meaning in life, and depressive symptomatology in individuals with alcohol dependence. Journal of Spirituality and Mental Health, 14(4), 268-288. https://doi.org/10.1080/19349637.2012.730469
Koivumaa-Honkanen, H. T., Honkanen, R., Antikainen, R., Hintikka, J., & Viinimäki, H. (1999). Self-reported life satisfaction and treatment factors in patients with schizophrenia, major depression and anxiety disorder. Acta Psychiatrica Scandinavica, 99(5), 377-384. https://doi.org/10.1111/j.1600-0447.1999.tb07244.x
Koivumaa-Honkanen, H. T., Viinamäki, H., Honkanen, R., Tanskanen, A., Antikainen, R., Niskanen, L., Jääskeläinen, J., & Lehtonen, J. (1996). Correlates of life satisfaction among psychiatric patients. Acta Psychiatrica Scandinavica, 94(5), 372-378. https://doi.org/10.1111/j.1600-0447.1996.tb09875.x
Lan, C. M., & Su, T. M. (2007). Life meaning of patients with schizophrenia. Chang Gung Nursing, 18(4), 385-475.
Lungu, A., & Linehan, M. M. (2017). Dialectical behavior therapy: overview, characteristics, and future directions. In S. G. Hofmann & G. J. G. Asmundsonr, (Eds.), The Science of Cognitive Behavioral Therapy (pp. 429-459). Academic Press.
Marco, J. H., Cañabate, M., Llorca, G., & Pérez, S. (2019). Meaning in life moderates hopelessness, suicide ideation, and borderline psychopathology in participants with eating disorders: A longitudinal study. Clinical Psychology & Psychotherapy, 27(2), 146-158. https://doi.org/10.1002/cpp.2414
Marco, J. H., García-Alandete, J., & Pérez, S. (2020). Meaning in life in eating disorders patients with non-suicidal self injuries. Revista Argentina de Clínica Psicológica, 29(5), 468-477. https://doi.org/10.24205/03276716.2020.1044
Marco, J. H., García-Alandete, J., Pérez, S., & Botella, C. (2014). Meaning in life as a mediator variable between depression and hopelessness in patients with borderline personality disorder. Behavioral Psychology, 22(2), 291-303.
Marco, J. H., García-Alandete, J., Pérez, S., Guillén, V., Jorquera, M., Espallargas, P., & Botella, C. (2015). Meaning in life and non-suicidal self-injury: A follow-up study with participants with borderline personality disorder. Psychiatry Research, 230(2), 561-566. https://doi.org/j.psychres.2015.10.004
Marco, J. H., Guillen, V., & Botella, C. (2017). The buffer role of meaning in life in hopelessness in women with borderline personality disorders. Psychiatry Research, 247, 120-124. https://doi.org/10.1016/j.psychres.2016.11.011
Marco, J. H., Pérez, S., & García-Alandete, J. (2016). Meaning in life buffers the association between risk factors for suicide and hopelessness in participants with mental disorders. Journal of Clinical Psychology, 72(7), 689-700. https://doi.org/10.1002/jclp.22285
Marco, J. H., Pérez, S., García‐Alandete, J., & Moliner, R. (2017). Meaning in life in people with borderline personality disorder. Clinical Psychology and Psychotherapy, 24(1), 162-170. https://doi.org/10.1002/cpp.1991
Martela, F., & Steger, M. (2016). The three meanings of meaning in life: Distinguishing coherence, purpose, and significance. Journal of Positive Psychology, 11(5), 531-545. https://doi.org/17439760.2015.1137623
Moghbel, S., & Haghayegh, S. A. (2019). The effectiveness of acceptance and commitment therapy on resilience, meaning in life, and family function in family caregivers of patients with schizophrenia. The Horizon of Medical Sciences, 25(4), 298-311. https://doi.org/10.32598/hms.25.4.298
Roberts, G. (1991). Delusional belief systems and meaning in life: A preferred reality? British Journal of Psychiatry, 159(Suppl. 14), 19-28. https://doi.org/10.1192/S0007125000296438
Rosmarin, D. H., & Koenig, H. G. (Eds.) (2020). Handbook of spirituality, religion, and mental healt. Academic Press. https://doi.org/10.1016/C2017-0-04790-0
Saarni, S. I., Härkänen, T., Sintonen, H., Suvisaari, J., Koskinen, S., Aromaa, A., & Lönnqvist, J. (2006). The impact of 29 chronic conditions on health-related quality of life: A general population survey in Finland using 15D and EQ-5D. Quality of Life Research, 15(8), 1403-1414. https://doi.org/10.1007/s11136-006-0020-1
Sacco, W. P., & Beck, A. T. (1995). Cognitive theory and therapy. In E. E. Beckham & W. R. Leber, (Eds.), Handbook of Depression: Treatment, Assessment and Research (2nd ed., pp. 329-351). Guilford Press.
Schulenberg, S. E., Strack, K. M., & Buchanan, E. M. (2011). The meaning in life questionnaire: Psychometric properties with individuals with serious mental illness in an inpatient setting. Journal of Clinical Psychology, 67(12), 1210-1219. https://doi.org/10.1002/jclp.20841
Seow, L. S. E., Vaingankar, J. A., Abdin, E., Sambasivam, R., Jeyagurunathan, A., Pang, S., Chong, S. A., & Subramaniam, M. (2016). Positive mental health in outpatients with affective disorders: Associations with life satisfaction and general functioning. Journal of Affective Disorders, 190, 499-507. https://doi.org/10.1016/j.jad.2015.10.021
Sivaraman, K. P. (2003). Life goals: The concept and its relevance to rehabilitation. Clinical Rehabilitation, 17(2), 192-202. https://doi.org/10.1191/0269215503cr599oa
Stolovy, T., Lev-Wiesel, R., Doron, A., & Gelkopf, M. (2009). The meaning in life for hospitalized patients with schizophrenia. The Journal of Nervous and Mental Disease, 197(5), 133-135. https://doi.org/10.1097/NMD.0b013e3181963ede
Volkert, J., Schulz, H., Brütt, A. L., & Andreas, S. (2014). Meaning in life: Relationship to clinical diagnosis and psychotherapy outcome. Journal of Clinical Psychology, 70(6), 528-535. https://doi.org/10.1002/jclp.22053
Williams, D. T., Hirsch, S., & Coffey, B. (2007). Mood and anxiety symptoms in an adolescent with pervasive developmental disorder not otherwise specified and moderate mental retardation. Journal of Child and Adolescence Psychopharmacology, 17(5), 721-726. https://doi.org/10.1089/cap.2007.17503
Notes
*
Research article.
Author notes
a Correspondence author. Email: joaquin.garcia-alandete@uv.es
Additional information
How to cite: García-Alandete, J., Pérez, S., & Marco, J. H. (2021). Differences in the meaning in of life in patients diagnosed with mental disorders. Universitas Psychologica, 20, 1-10. https://doi.org/10.11144/Javeriana.upsy20.dmlp