Introduction
Today's medicine has succeeded in prolonging life and changing the course of many previously fatal diseases. This has increased the recovery of health in many patients and clinical situations. However, some circumstances lead to the final stage of life, where death is inevitable for the patient. In these situations, the objective of care must change from an unattainable goal, such as a cure, to that of care and symptom relief (therapeutic adaptation or reorientation), trying to maintain the best possible quality of life in a holistic sense, both physical, emotional, mental, and spiritual, which is generally desired by the patient, their family members, and the health care team (1-4).
The end of life can be predictable in many situations, especially when patients have chronic, debilitating, and incurable diseases. Unfortunately, despite this, all therapeutic efforts are often maintained to try to cure the patient, performing disproportionate diagnostic and therapeutic interventions that bring no real benefit, and, many times, what is achieved is to prolong the agony, deteriorate the quality of life in the time before death, and increase health care costs (5-7).
Taking into account the above and personal experience in daily clinical practice, a group of clinical experts led by the Clinical Ethics Service of the Hospital Universitario San Ignacio, which included physicians specialized in internal medicine, palliative care, geriatrics, and psychiatry, among others, and with the approval of the Hospital Ethics Committee, developed and implemented in 2016 the Care Plan for the Patient in End-of-Life Condition—PFV, by its Spanish acronym for "Paciente en Condición Fin de Vida" (Patient in End-of-Life Condition), based on available scientific information and integrating humane, individualized, and compassionate management.
The PFV aims to support groups and treating physicians within the hospital for the adequate planning of end-of-life care. The PFV was based on the previous experience of numerous institutions worldwide, especially the United Kingdom strategy known as The Liverpool Care Pathway (8,9). The PFV structures an approach based on five priorities of care:
-
Recognition by treating physicians when a patient is at the end of life and activation of the PFV.
-
Establish appropriate communication between the medical team, the patient, and the patient's family.
-
Involve the patient and family members in treatment decisions, if they wish.
-
To explore and meet the needs of the family members to the extent possible.
-
Establish an individual care plan, including comfort measures, hydration, nutrition, symptom control, and psychological and spiritual support.
Based on these care priorities, special care was established (Table 1), some of which are called anti-orders, which consist of the suspension of certain routine activities that do not change the patient's prognosis for the clinical situation and, on the contrary, may cause discomfort, for example, taking vital signs or paraclinical tests, among others. Special care seeks to alleviate symptoms, provide comfort, and guarantee dignified treatment at the end of life for each patient, which is why it is vital to have adequate communication to recognize what the patient's preferences and wishes are and thus provide an individualized and humanized care plan.
Table 1
Special care

The socialization of the PFV consisted of multiple participatory lectures by all health personnel, including physicians, nurses, therapists, nursing assistants, and stretcher-bearers, among others.
After four years of dissemination and implementation, the general perception, according to uncontrolled observations of physicians and nurses, is that patients who have entered such a care plan have received adequate management at the end of life without disproportionate interventions and have maintained adequate symptomatic management. However, the specific management provided upon admission to PFV (what is discontinued and what is added to the management?) and the common and individual clinical characteristics of these patients are not well known. Therefore, it was decided to conduct a retrospective observation of the management of adult patients admitted to the PFV to learn about and describe the clinical management of patients admitted to this plan and, if necessary, improve the management of patients at the end of life.
Materials and methodology
This was an observational, descriptive, retrospective study based on the investigators' review of the medical records of patients admitted to the PFV at Hospital Universitario San Ignacio between 2016 and 2019, according to the Clinical Ethics Service database. We only went as far as 2019, as the pandemic significantly changed the clinical management of end-of-life patients. All adult patients over 18 years of age were included.
The study was approved by the Institutional Ethics Committee, complying with all patient data confidentiality and security standards. The clinical management received by the patients at the end of life was analyzed, taking into account the care plan already described.
Results
-
We analyzed 339 medical records of patients admitted to the PFV from January 1, 2016, to December 31, 2019, who at the time of death had a mean age of 66.3 years (range 19-100 years; standard deviation 17.51). Of these, 51.9% (176 patients) were male, and 48% (163 patients) were female. The established approach was followed in all patients who entered the PFV:
-
Adequate communication was established between the medical team, the patient, and the patient's family.
-
The patient and family members were involved in treatment decisions if they wished.
-
Family members' needs were explored and, to the extent possible,
-
Visits were freed up, allowing the presence of the family members 24 hours a day.
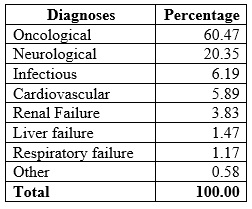
The time elapsed between admission to the PFV and the deaths of the patients was 4.05 days on average (range between 0 and 40 days; standard deviation of 4.5). Table 2 shows the main diagnoses of the 339 deceased patients. The most prevalent diagnosis was oncological, with 60.47% (205 patients), followed by neurological pathologies (cerebrovascular events, hypoxic encephalopathy after cardiopulmonary resuscitation, neurodegenerative encephalopathy) and infectious pathologies such as HIV.
Table 2
Definitive diagnoses of patients admitted to the PFV
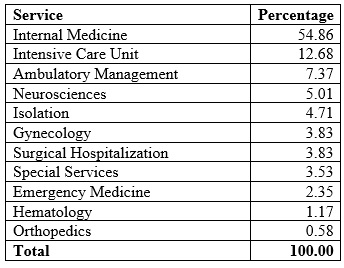
It was observed that at the time of death, more than half of the patients, that is, 54.86% (186 patients), were hospitalized in the Internal Medicine Department, followed by the Intensive Care Unit, with 12.68% (43 patients). See Table 3.
Table 3
Services in which the patients admitted to the VFP died
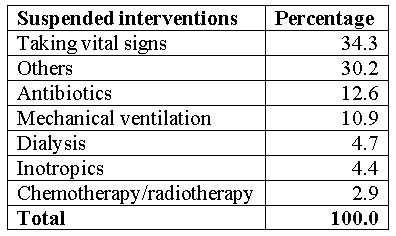
The PFV establishes the suspension of medications and interventions that are futile for the patient's clinical situation to direct care toward the greatest possible well-being. It was found that the taking of vital signs was suspended in 34.3% (116 patients), as well as other therapeutic measures, in 24.4% (83 patients), which included the withdrawal of oral medications, heparins, insulins, nutrition, suspension of surgical procedures, etc. Likewise, mechanical ventilation was suspended in 10% of the patients, as were dialysis and inotropic drugs, as shown in Table 4.
Table 4
Suspended medical procedures and interventions in patients admitted to the PFV
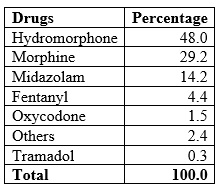
All patients admitted to the PFV were managed jointly with the Palliative Care Service to ensure that their symptoms were adequately controlled. Where warranted, symptom-specific medications were used (Table 5).
Table 5
Sedation/analgesia received by patients admitted to the PFV
Likewise, all patients admitted to the PFV received spiritual support according to their wishes, as well as permanent and specific attention from the nursing staff, such as skin care, changes of position, and moisturizing of the oral mucosa, among others.
Discussion
To improve the care of patients in the final phase of life, guidelines and management protocols have been developed for comprehensive care that includes a palliative care approach and aims to provide dignified treatment at the end of life. This care focuses on controlling symptoms, reducing suffering, and promoting comfort, seeking to improve the quality of life for the patient and his or her family (10,11).
Because of the highly individualized nature of the dying experience, a multidisciplinary approach to care must be ensured, with an assessment that includes physical, psychological, social, and spiritual aspects. This analysis should guide physicians in the formulation of goals to ensure a good dying experience (12-14).
Worldwide, about 20 million people receive palliative care at the end of life. Steinhauser et al. (2) reported, based on the perspectives of patients, physicians, and other caregivers, that a good death includes not only physical but also psychosocial and spiritual factors. Therefore, it depends on each person according to his or her life experience, so no universal definition of a good death can be adopted (15).
Likewise, Zhang et al. (7) and Sagha Zadeh et al. (3) documented that quality of life in the final stage is better when hospitalization is avoided and futile or disproportionate medical interventions are decreased or eliminated, reorienting therapeutic efforts towards symptom management. Additionally, they emphasize understanding the concerns of each individual; therefore, spiritual and psychological support should be offered to the sick person and their loved ones, taking into account and understanding the social, cultural, and religious contexts.
The present study showed that thanks to the institutional PFV, an individual approach was made to each patient according to their needs and preferences, to ensure a good death, such as palliative care, spiritual support, and special nursing care, among others. Most of the patients died in an adequate and comfortable place, and more than half of the patients were transferred to the Internal Medicine Department in a single room. They were also located in the different hospitalization services, which have a suitable location so that the patient and his family could have privacy.
It is important to highlight that 7.37% of the patients continued the PFV at home due to the desire of the patient or their relatives to return home and spend their last days in the company of their loved ones. Therefore, physicians established a home management plan with therapeutic indications that would guarantee optimal symptom control and necessary care.
Gempeler et al. (5) published a study carried out in the same hospital before the implementation of the PFV, with a retrospective analysis of the management of patients at the end of life, focused on detecting disproportionate medical interventions in that final stage. The study found that more than half of the patients underwent interventions considered futile. With the results of the present study, we can see that the implementation of the PFV allowed us to reduce some of the futile interventions, such as mechanical ventilation, dialysis, use of inotropic drugs, artificial nutrition, suspension of surgical procedures, insertion of catheters, as well as chemotherapy and radiotherapy at the end of life.
Within the specific care of the PFV are the anti-orders, which include suspending or not initiating disproportionate interventions, such as taking vital signs, since such care is considered to be uncomfortable for the patient and has no clinical relevance in the final stage of life, except for taking the temperature, since if fever is present, it is a symptom to palliate. Surprisingly, in only 34.3% of the patients, the vital signs were not taken. Analyzing this result and socializing it with the nursing group, not taking vital signs can be erroneously interpreted as carelessness or a deficit in patient care. For this reason, the nursing group, on many occasions, continued with this care.
Nursing work is fundamental for patients at the end of life because the essence of this profession is care. Initially, the nursing team must perform an individualized analysis of the different needs of the patient and then establish specific and special care. Nursing actions are aimed at helping, relieving, comforting, and providing greater well-being, whether physical, psychological, or psychosocial. In addition, this action is accompanied by values such as empathy, compassion, recognition, and love, among others, which are essential to alleviating suffering and promoting a dignified death (13,16-22).
Conclusions
The results of the present study show that the PFV offered a comprehensive approach, that the needs of the patients were met, and that some of the invasive and disproportionate interventions were reduced, promoting the execution of an individualized analysis to promote the necessary care for a dignified death according to the wishes of each patient.
Additionally, the present study exposes the importance of a multidisciplinary approach, always including palliative care, to achieve adequate symptom control.
Despite the positive achievements of this strategy, the education of healthcare personnel on the importance of building care plans focused on guaranteeing a dignified death must be strengthened.
Conflict of interests
None.